INTRODUCTION
According to the World Health Organization, 40 million people die from noncommunicable diseases (NCDs) each year, which is equivalent to 70% of all deaths globally (1). Cancer is the second leading cause of death after cardiovascular disease. In 2018, the International Agency for Research on Cancer (IARC) estimated 18.1 million new cancer cases and 9.6 million deaths (2). Cancer incidence varies according to gender and different geographic locations, among other factors. In women, the most commonly diagnosed type worldwide is breast cancer (BC), both in developed and developing countries. In 2018, approximately 2.0 million new cases were diagnosed (24.2% of all cancer cases were diagnosed in women). The same year in Spain, the incidence of female BC was 24.7% (2).
The World Cancer Research Fund (WCRF) has concluded that healthy lifestyles may help to prevent up to 70% of cancer cases. These include healthy diet eating, regular physical activity, a healthy weight, and avoiding smoking and alcohol drinking (3). There is growing and consistent epidemiological evidence, with robust confirmation for mechanisms operating in humans, that greater body fatness is a cause of postmenopausal breast cancer (3).
At the same time, malnutrition is very common in these cancer patients after the disease has been diagnosed. The prevalence of disease-related malnutrition ranges from 20% to 80% in patients with cancer, and increases the risk of adverse outcomes, including poor prognosis, treatment response, and quality of life (4,5).
Early identification of malnutrition and an appropriate nutritional intervention are essential in this population to avoid the potential pathological effects of deficient nutrition, and to reduce the cytotoxic effects and other associated complications (6).
In Spain, although a preliminary assessment of the nutritional status is recommended at the time of diagnosis with any cancer (6), the clinical care of cancer patients focuses mainly on the medical treatment. A dietitian assesses only patients with severe malnutrition, but not those who are newly diagnosed, thus limiting the benefits of an earlier nutritional intervention. To date, few Spanish studies have addressed this assessment of nutritional status in newly diagnosed cancer patients, before a therapy is established (7,8). There is some information during periods of treatment such as chemotherapy, or concerning malnutrition in terminal stages. But current studies deal only with diet, or physical activity, or lifestyle, and not enough studies are performed to provide an integral evaluation of all these environmental factors (7,8). Furthermore, there are no previous nutritional assessment studies in women with breast cancer in the northern Spanish region of Asturias, which exhibits the highest cancer-related mortality rate among all Spanish regions (9).
Therefore, the aim of the present study was to assess the nutritional status of newly diagnosed female patients with breast cancer in the north-western coast of Spain (Asturias), as well as specific information on their physical activity and body composition.
METHODS
STUDY DESIGN AND PARTICIPANTS
A cross sectional study was conducted in newly diagnosed female patients with breast cancer attending the Oncology Unit at Centro Médico de Asturias and the Surgery Unit at Hospital Universitario Central de Asturias. The Spanish region of Asturias has the highest obesity rates for adults in the country (25.7%, aged between 24-65 years) (10). The population sample of female cancer patients was recruited on their first hospital visit after cancer diagnosis, between February 2016 and July 2017. Therefore, the recruitment took place prior to any type of therapeutic intervention. The inclusion criteria considered women aged 18 years or older with an initial diagnosis and a confirmed result of breast cancer. Patients with nutritional support, supplementation, or psychiatric illness were excluded. The Ethics Committee of Universidad CEU San Pablo approved the study. Informed consent was obtained from all participants before enrolment. A single dietitian performed all measurements and administered all questionnaires, thus variability between observers was avoided.
PHYSICAL ACTIVITY AND ANTHROPOMETRIC DATA
The validated International Physical Activity Questionnaire (IPAQ, short version) was used to obtain information about each patient’s physical activity before their diagnosis during a face-to-face interview (11).
Anthropometric measures such as height, weight, waist, hip and arm circumferences, and triceps skin fold thickness were obtained according to the methodology described by the International Society for the Advancement of Kinanthropometry (ISAK) (12). A trained dietitian performed these measurements. Patients were weighed in light clothing without shoes on an In Body 230 (Microcaya) weighing scale with a graduation of 0.1 kg. Patient height was determined with a mechanical height rod stadiometer (Wunder HRi) using a graduation of 1.0 mm. All measurements were obtained in duplicate. The measurements of waist, hip, and arm circumferences were made in triplicate by using a Cescorf flexible steel tape measure with a graduation of 1.0 mm. The triceps skinfold thickness was measured by using a Holtain skinfold caliper (0.2 mm). Arm strength was determined with the Takei 5401 Hand Grip Dynamometer (graduation of 0.1 kg). The mean arm circumference and triceps skinfold thickness were used to calculate the mid-arm muscle circumference and the corrected arm muscle area using standard equations. The corrected arm muscle area ≤ 21.6 cm for females was used to determine the risk of malnutrition (13). Fat and lean mass were determined using an InBody 230 multi-frequency (20 kHz, 100 kHz, Microcaya) measurement, according to the recommendations issued by the European Society for Parenteral and Enteral Nutrition (ESPEN) for the assessment of patients conforming to the bioelectrical impedance test (14). The participants were classified according to their BMI and waist/hip index as described in the Spanish Society for the Study of Obesity (SEEDO) classification (15).
NUTRIENT INTAKE ASSESSMENT AND CLINICAL DATA
A trained dietitian collected and processed the dietary data using standardized questionnaires of 24-hour recall for three different days – two week days and one weekend day (16). The 24-hour dietary recall was carried out prior to the initiation of the prescribed treatment. Participants were asked for detailed descriptions of the foods and beverages they had consumed, as well as their portions, cooking methods, and recipes. The 24-hour recall interviewer used visual aids, food models, food portions and probing questions to overcome the memory lapses of the respondents (17). The food weights obtained were converted to nutrient intake estimates per day by using the DIAL programme, based on the Spanish food composition database (version 3.0.0.5) (18).
Diet quality and intake adequacy were assessed according to the recommended food portions and the nutritional targets authorized by the Spanish Society for Community Nutrition (19). Dietary energy and nutrients were compared to the recommended intakes for the Spanish population (20). Patients were also administered the Patient Generated Subjective Global Assessment (PG-SGA), a validated tool for nutritional diagnosis, simple and effective, that is currently considered the standard reference for the assessment of nutritional status in cancer patients (21). In addition, medical records were collected in the PG-SGA too (e.g., type of tumor and stage data) in order to complete their clinical status assessment.
STATISTICAL ANALYSIS
The size of the sample was determined according to the incidence of BC amongst women in Asturias (9). A sample of 72 subjects was calculated, with a 95% confidence interval, α error of 5%, β error of 20%, and a power of 80%, by using the McNemar test. With a prediction of percentage loss of 20%, an initial sample consisting of 76 subjects was proposed. All statistical tests were performed using the IBM SPSS Statistics for Windows, Version 22.0 software (IBM Corp., Armonk, NY, USA). Descriptive statistics (mean, standard deviation, proportions, and absolute number and percentage) were computed for each investigated variable.
RESULTS
GENERAL CHARACTERISTICS
A total of 76 female participants finally joined the study. All participants completed the study (100% response rate) and none of them suffered from pre-existing comorbidities. All had a diagnosis of breast cancer. Their baseline characteristics (Table I) showed that most patients were > 50 years old (average age: 56.9 years). The patients were diagnosed with stage I (n = 57; 75%), stage II (n = 18; 24%) or stage III (n = 1; 3%) malignancies. Most of the cancers had hormone receptors and were of the luminal A/B type (n = 60, 79%). Twenty-four percent of these BC patients were smokers (n = 18) or ex-smokers (n = 26; 34%), and more than half of the sample (n = 49) drank alcohol regularly. The physical activity level was low, and the patients were currently sedentary (59%, n = 45). According to the PG-SGA criteria, 98% of patients were well-nourished at the time of diagnosis.
Table I. Selected baseline characteristics of newly diagnosed breast cancer female patients in Asturias

Number of patients (percentage), n (%).
*Tumor grade: I = well differentiated, II = moderately differentiated, III = poorly differentiated, IV = undifferentiated.
†HER2: human epidermal growth factor receptor 2.
‡Physical activity levels (11).
ANTHROPOMETRIC MEASURES
According to their body mass index, nearly one-third (31.6%) of the participants were considered obese at diagnosis. Anthropometric measures are summarized in table II. The body fat percentage was higher than recommended (38.3%). Waist circumference and waist/hip ratio data were also higher than the reference values in all participants (17). The average mid-arm muscle circumference was 29.4 cm. Our BC patients aged 60-69 years showed greater strength in their right arm (p = 0.02) when compared to references (22).
Table II. Anthropometric measures of newly diagnosed breast cancer female patients in Asturias
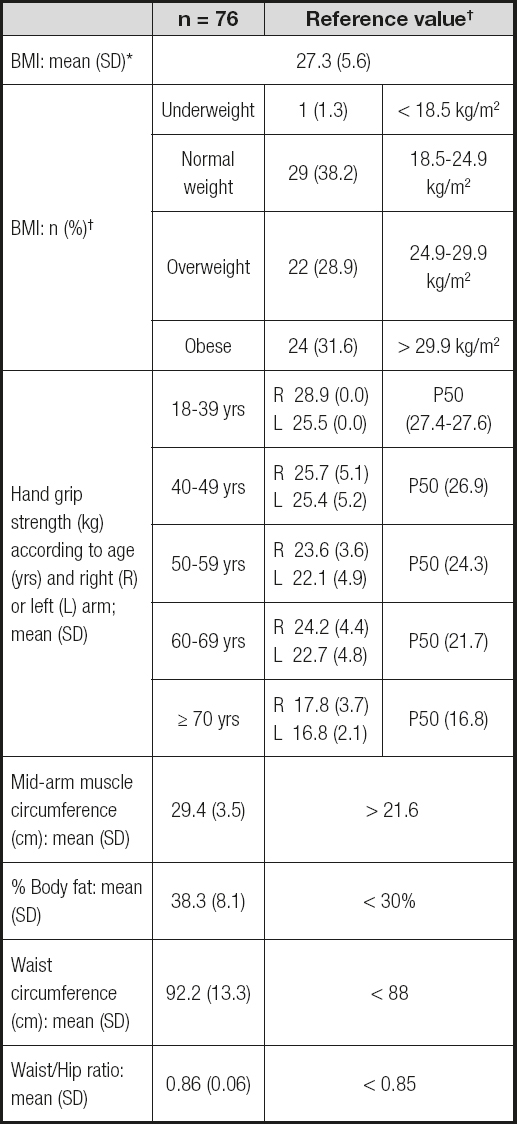
Number of patients; mean values (standard deviation).
*BMI (body mass index): weight (kg)/height2 (m2).
†Consensus SEEDO 2007 (15).
BIOCHEMICAL PARAMETERS
At diagnosis, the values of the measured biochemical parameters (Table III) were considered clinically normal for hemoglobin, hematocrit, glucose, triglycerides, albumin, and iron in all participants (23). Total cholesterol levels (212.6 mg/dL) were higher than the reference values (200.0 mg/dL).
Table III. Biochemical markers of newly diagnosed breast cancer female patients in Asturias

Mean values (standard deviation).
*Reference values (23).
NUTRIENT INTAKE ASSESSMENT AND ADEQUACY OF THE REPORTED INTAKE
The results obtained for the intake frequency of food groups among these newly diagnosed BC female patients in Asturias are presented in table IV. All participants had an insufficient intake of plant-based foods (fruits, vegetables, cereals and potatoes, legumes, and nuts). In contrast, they had adequate intakes for lean meats, and for olive and sunflower oils.
Table IV. Daily frequency of food groups consumption in newly diagnosed breast cancer female patients in Asturias
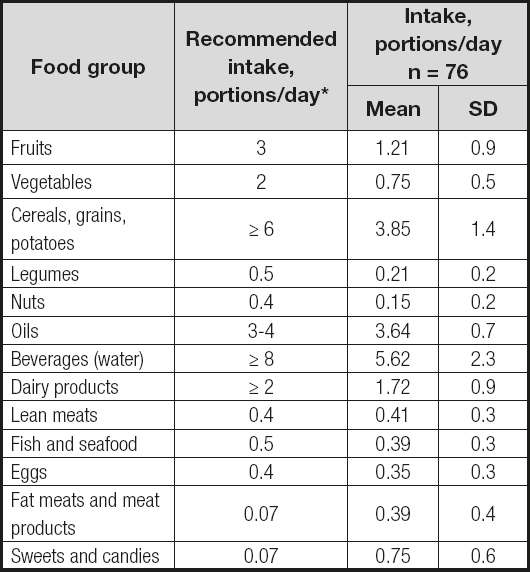
Mean values (standard deviation).
*Daily consumption recommended by Spanish nutritionists (19).
The intakes of macronutrients and selected micronutrients are summarized in table V. The dietary assessment showed an unbalanced energy and macronutrient distribution in the patients. Energy and carbohydrate intakes were lower than recommended (p < 0.05) (20). The average carbohydrate intake was particularly low (39.6%).
Table V. Total energy intake and the contributions of macronutrients and lipids (%) in newly diagnosed breast cancer female patients in Asturias

SFA:saturated fatty acids;
MUFA:monounsaturated fatty acids;
PUFA:polyunsaturated fatty acids. Mean values (standard deviation).
*Nutritional objetives for the Spanish population (19).
The reported intakes of minerals and vitamins (Table VI) were compared to Spanish recommendations (20). The daily intake of vitamins and minerals did not meet the recommendations for folate (62.3% of recommended intake), vitamin D (13.1%), vitamin E (36.6%), calcium (66.6%), and zinc (54.8%).
Table VI. Reported intake of vitamins and minerals in newly diagnosed breast cancer female patients in Asturias, and its adequacy with regards to the daily intakes recommended for the Spanish population

*Spanish reference intake (20).
DISCUSSION
The present study provides the first data available on the baseline characteristics and lifestyle factors (physical activity, tobacco use, and alcohol intake), anthropometry, biochemical parameters, and nutrient intake of women newly diagnosed with breast cancer (BC) in Asturias, northern Spain, prior to any therapeutic intervention. Actually, very few studies in Spain have evaluated the nutritional status of oncologic female patients at diagnosis (7,8). Some studies have analyzed the nutritional status of cancer patients in a terminal stage, or during chemotherapy and radiotherapy interventions. Other studies have considered only some parameters separately, like quality of life, or diet, or physical activity (7,8).
In the present study, sedentarism rates were high among our patients. The evidence suggests an inverse relationship between physical exercise, aerobic and strength, and the risk for relapse in cancer survivors (24). Travier et al., in 2015, studied the effect of an 18-week exercise programme during BC treatment. They reported positive effects on physical fatigue, submaximal cardiorespiratory fitness, and muscle strength (24).
A high percentage of newly diagnosed female patients with cancer were smokers and regular alcohol drinkers. The World Cancer Research Fund (WCRF)/American Institute of Cancer Research (AICR) report from 2018 showed that alcohol intake is strongly linked to the risk of developing BC in postmenopausal women (25). Furthermore, high alcohol intakes reduce folate absorption (26). This could explain why BC risk is higher in women with a regular alcohol intake and a folate-deficient dietary intake (26). Interestingly, the present study showed deficient folate intakes at diagnosis (Table VI). This result follows the same trend than that found by the ANIBES study for the general female population in Spain (27).
According to the PG-SGA method used to assess the nutritional status of participants in this study, 97.8% of participants were well-nourished at diagnosis. The prevalence of malnutrition in the current study was lower than that reported in other studies. Bering T et al. found that 80.8% of BC female patients were well nourished before starting chemotherapy or radiotherapy (28).
Despite this result, in the present study it is important to note that there is a high prevalence of overweight and obesity, with high body fat percentages and high waist circumference values in the study patients. This result follows the same pattern shown by the ENPE study for the Spanish population, which recently reported a prevalence of overweight and obesity of 25.7% among healthy adults aged 24-65 years living in Asturias (10). Also, our results are similar to those obtained for the general population of Spain according to the ANIBES study, which revealed a high prevalence of overweight and obesity in women (31.5% and 17.2%, respectively) (29).
Overweight and obesity could increase the risk of several types of cancers, such as BC. Ewertz M et al. have established that the higher the BMI value (≥ 30 kg/m2) of BC patients at diagnosis, the higher the cancer risk (30). In addition, a study on obesity and BC risk indicated that general and central obesity were positively associated with BC risk in pre- and post-menopausal BC women (31). Along the same lines of our BMI results, 61.8% of the patients had abdominal obesity as based on waist circumference. A high percentage of overweight and obesity (66.5%) was also reported in a study among Malaysian BC patients after 1 year post-diagnosis (32). Excessive abdominal fat and large waist circumference values are associated with an increased risk of postmenopausal BC (33).
The assessment of muscle strength using the handgrip strength test has been widely utilized in BC survivors. In the present study, BC patients (60-69 years) showed greater strength in their right arm when compared to references (22). A good status for this indicator could be considered particularly interesting, primarily considering that previous studies have showed a markedly impaired muscle strength after treatment in BC patients (34). To our knowledge, no studies have thus far reported handgrip strength in cancer patients at diagnosis.
Regarding biochemical markers, BC patients showed increased total cholesterol (TC) levels when compared to references values. Several studies have investigated the relationship between TC and HDL-C and the risk for BC. A meta-analysis (35) confirmed the evidence of a modest but statistically significant inverse association between HDL-C and BC. Ni et al. (35)suggested that serum HDL-C protects against breast carcinogenesis only among postmenopausal women.
Recent research has reported a protective role against cancer of some dietary patterns, specifically those including a high intake of vegetables, fruits, whole grains, fish, olive oil, and nuts (36). The Mediterranean diet is an example of this. However, in the current study, we found that BC female patients evaluated in the northwestern region of Spain did not follow the classical, recommended Mediterranean dietary pattern. The patients’ dietary intake was poor in plant-based foods such as fruits, vegetables, cereals, grains, legumes, and nuts, and was instead rich in red meats and meat derivatives, as well as sweet foodstuffs. These findings are consistent with those of other studies in cancer female patients on treatment, which reported a low consumption of fruits, vegetables, and wholegrain cereals (36). Consistently with this pattern, the energy and macronutrient distribution of these patients was unbalanced when compared to the Spanish Nutritional Objectives (19), with an excessive intake of lipids and a low proportion of energy provided by carbohydrates. The contribution of lipids to total energy intake was higher than the values stated in the Spanish Nutritional Objectives because of a higher intake of MUFAs. Our data follow the current typical western dietary patterns, actually quite similar to those reported by the ANIBES study for the general Spanish population (37).
Regarding micronutrients, as a consequence of the low intake of fruits and vegetables, folate dietary intake was markedly lower when compared to the Spanish reference intakes (20). Other authors (38) have also reported similar results in BC patients undergoing treatment. Vitamin E and vitamin D intakes were also definitely low in these patients’ diets. Several studies in cancer patients also reported an inadequate intake of these vitamins (13). Vitamin D dietary intake results were dramatically low, indeed. As a matter of fact, reported calcium intakes were low, underscoring another weakness in their diet. These results are of particular concern and could lead to many potential implications, since folate, calcium, and vitamin D are critical nutrients specifically involved in the nutritional status and health of women. Zinc and potassium dietary intakes were also suboptimal. A diet poor in vegetables also led these patients to have a reduced intake of fiber. Several studies have demonstrated the protective effect of fiber against BC, among other types of cancer (39). A strong evidence suggests that dietary intervention could reduce nutritional status failure during intensive treatment (5,40).
CONCLUSIONS
In summary, this study provides for the first time specific knowledge on the nutritional status at diagnosis of breast cancer (BC) female patients in a northern region of Spain (Asturias), a region where breast cancer rates are particularly high when compared to the rest of Spain. Most of these participants showed overweight and high sedentarism levels, and reported unbalanced dietary patterns, quite far from the Mediterranean model. All of them reported a low intake of vegetables and a high intake of red meat. Patients also showed an alarming low intake of folate, vitamin D, and calcium. These results are particularly concerning, since folate, calcium, and vitamin D are critical nutrients involved in the nutritional status and health of women.
An early identification of malnutrition risk, and a timely nutritional intervention, are critical for cancer patients at diagnosis. Such an intervention – before, during, and after cancer therapy – might well be critical not only to cover the nutritional requirements of cancer patients, but also to reduce the cytotoxic effects and complications associated with cancer treatment, whose effects have an impact on nutritional status. Longitudinal studies evaluating the evolution of the nutritional status of patients are also needed.














