INTRODUCTION
The preferred method of artificial nutrition administration in patients who do not want to, cannot or should not use the oral route but have a functional bowel is called enteral nutrition (EN) (1-4). Patients with EN who are able to obtain ≥ 80 % of the total caloric requirement have well-documented beneficial effects, including a reduced risk of complications, short hospital stays, and decreased mortality (5,6). However, the majority of patients do not reach the optimal protein and energy requirements (OPER ≥ 80 %), achieving only an average that ranges between 50-95 % of their energy requirements and 38-82 % of their protein requirements (5).
Potential complications of nutritional interventions include refeeding syndrome (RS), which produces an anabolic reaction associated with alterations in serum electrolytes. These abnormalities include clinical manifestations, low concentrations of intracellular ions, such as phosphate, magnesium, and potassium, or both, resulting in metabolic changes and fluid imbalance (peripheral edema, heart or respiratory failure) (7,8). This disorder can occur despite risk identification, immediate treatment, and administration of low-calorie nutritional therapy; however, in many cases it can be prevented by performing an adequate and complete nutritional assessment, including identifying the risk of developing RS before starting nutritional support (9,10).
The use of EN algorithms in critically ill patients has shown beneficial effects by using a safe increase in caloric and protein administration in a shorter period of time compared to usual therapy (11-15). Ortíz-Reyes published the results of a randomized controlled trial that compared the algorithm for total enteral nutritional support (ASNET) versus usual therapy in noncritical patients. They found that a high percentage of patients started EN within 72 hours after prescription compared to usual practice (74 % vs. 50 %, p = 0.026). In addition, the use of ASNET allowed an increased number of patients to receive ≥ 80 % of the calories and protein prescribed within the first 4 days (15). However, patients at risk of developing RS require a different approach for prevention, and adherence to the recommendations may influence the results obtained.
We hypothesized that adherence to the ASNET protocol would allow more than 50 % of the patients to meet the optimal energy requirements. For these reasons, the present study aimed to evaluate the adherence to the ASNET, and the efficacy of achieving optimal energy requirements in non-critical patients at risk of RS.
MATERIALS AND METHODS
This was a cohort study that included patients admitted to a third-level hospital between April 2018 and September 2019. This study complied with the guidelines stipulated in the International Ethical Guidelines for Biomedical Research involving humans, as stipulated in the Declaration of Helsinki and the Nuremberg Code (16,17), and received approval by the Ethics and Institutional Research Committee (No. 1390). All patients provided written informed consent.
Patients of both sexes who were ≥ 18 years old, admitted to noncritical areas and expected to stay in the hospital for a period equal to or greater than 72 hours, with indication of EN and at risk of RS were included. Risk of RS was determined by using the criteria of the National Institute of Health and Clinical Excellence (NICE) (18,19):
- Very high risk: if one of the following factors were present: BMI < 14 kg/m2, unintended weight loss > 20 % or starvation greater than 15 days (20).
- High risk: patients presenting one risk factor A (BMI < 16 kg/m2; unintentional weight loss > 15 % in the last 3 to 6 months; little food intake or fasting for more than 10 days; or low levels of potassium, phosphate and magnesium) and two risk factors B (BMI < 18.5 kg/m2; unintended weight loss > 10 % in the last 3 to 6 months; little food intake or fasting for more than 5 days; history of alcohol, drugs, insulin, antacids or diuretics consumption).
- Low risk with a risk factor B.
Patients with established RS, with intestinal failure or chronic diarrhea were excluded. Patients who decided not to participate in the study, those who self-removed the tube 48 hours after the start of the EN, those with mixed nutrition (enteral plus oral or parenteral) during the first 72 hours of EN, and those whose condition deteriorated and were admitted to the intensive care unit were not included in the final analysis.
Prior to beginning the EN infusion, a nutritional screening was performed with the Nutritional Risk Screening (NRS) 2002 tool, and nutritional evaluation included anthropometric measurements, biochemistry, clinical and dietary data. Assessment of weight loss/gain, dietary intake prior to hospitalization and severity of current disease were used to identify possible alterations such as the risk of RS, and if present, the ASNET showed steps to prevent such a risk (15) (Fig. 1).
Adherence to ASNET was determined with a checklist that was created specifically for this study with the 10 items listed below. This checklist was completed by an independent researcher from the clinical nutrition team responsible for the EN prescription in all hospital an according to the average compliance of the items, which corresponds to the main aspects evaluated in the ASNET protocol, patients were divided into 2 different groups: adherence (≥ 80 % of the items) and nonadherence (< 80 % of the items). According to the algorithm, the evaluated items for compliance were as follows: 1) assessment of patient clinical stability; 2) assessment of RS risk; 3) review and correction of serum electrolytes before starting EN; 4) continuous strict monitoring; 5) thiamine indication prior to EN; 6) thiamine administration for 5 to 7 days; 7) caloric calculation (days 1-3 = 8-10 kcal/kg/24 h, days 4-7 = 12-15 kcal/kg/24 h; days 8-15 = 15-20 kcal/kg/24 h); 8) calculated caloric objective using 25-30 kcal/day/actual weight, 1.2-2 grams protein/day/actual weight; 9) EN administration route either gastric or postpyloric with their respective indications; 10) protocolized restart EN table usage.
Data were collected from electronic and physical records, including nursing progress notes and nutritional clinical history. Variables related to nutritional support were recorded, such as duration, initial rate of administration, amount of energy (kcal), grams of protein (g Pt) prescribed and administered per day of hospitalization. The above information was obtained by knowing the type of formula and the EN prescribed until the total and OPER ≥ 80 % was reached. Associated mechanical, gastrointestinal and metabolic complications were recorded during follow-up. Imminent RS was considered if the phosphate level decreased > 30 % during the first 72 hours after the start of nutritional therapy, with respect to the initial value (baseline); or to a total value < 1.85 mg/dL or if two other electrolytes decreased below the normal range (magnesium < 1.85 mg/dL, potassium < 3.50 mmol/L) (9). Follow-up ended when the patient changed the feeding routes or was discharged (alive or dead), recording the hospital length of stay.
STATISTICAL ANALYSIS
Descriptive statistics were used to determine frequencies and percentages for qualitative variables. Quantitative variables were expressed with measures of central tendency (mean and median) and dispersion (standard deviation or interquartile range [25th and 75th percentiles]), according to their type of distribution using the Kolmogorov-Smirnov test. To perform the intergroup comparison of qualitative variables we used the Chi2 test and for continuous quantitative variables Student's t-test for independent samples or the Mann-Whitney U-test. Student's t-test or Wilcoxon's test were used for paired samples. ANOVA or Friedman's test were used for multiple comparisons. A p-value < 0.05 was considered indicative of statistical significance, and the data were analyzed using the SPSS 21 statistical package. The sample size was calculated with the formula for two proportions (15): one proportion was the data of the ASNET study when it was implemented, where 61 % of patients achieved more than 80 % of caloric requirements. The second proportion was the investigations' hypothesis where more than 50 % of patients would accomplish the optimal requirement. Assuming a confidence level of 95 %, a power of 80 %, and a maximum loss value of 20 %, a total of 40 patients resulted.
RESULTS
During the study period, 87 patients were eligible, 73 patients met the inclusion criteria, and 14 were excluded because they did not have EN exclusively (Fig. 2). Infections were the main admission diagnosis, and all the patients had nutritional risk. The median NRS-2002 score was 5 points (IQR 4-5). Table I describes the demographic and clinical characteristics of the study population.
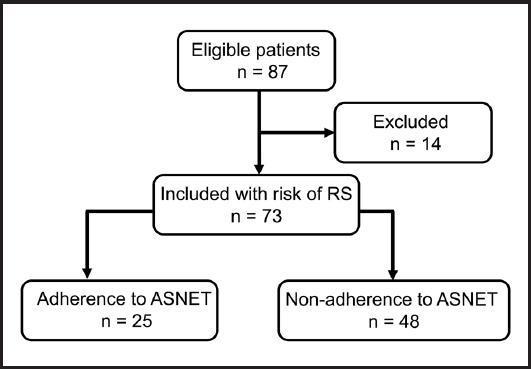
Figure 2. Flow diagram for the total of patients included in the study (ASNET: enteral nutrition algorithm; RS: refeeding syndrome).
Table I. General characteristics of patients according to adherence to the ASNET algorithm

Mean ± DE. *Median [P25-P75].
The median adherence to the ASNET was found to be 70 %, and 34 % of the patients had adequate adherence (≥ 80 % of the items). The items that had significant differences between the groups and that determined such adherence were the identification of RS risk (100 % vs 29 %, p < 0.0001), the indication of thiamine prior to EN (100 % vs 29 %, p < 0.0001), the administration of thiamine for 5 to 7 days (32 % vs 2 %, p < 0.0001), the calculation of calories according to recommendations (28 % vs 8 %, p = 0.026), and the indications of either gastric or postpyloric EN (82 % vs 52 %, p = 0.002), with or without adequate adherence, respectively.
There was a significant progression in the administration of EN on the days evaluated (p < 0.05); 33 % of the patients managed to cover the total caloric requirement between 4 to 6 days of EN, and 19 % did not reach it during follow-up. Mean OPER compliance according to adherence to ASNET was 4.7 ± 2.3 days for the adherence group compared to the group that did not adhere, with 4.0 ± 3.5 days (p = 0.054) corresponding to 27 kcal (24-31) and 25 kcal (22-30), respectively. Of the patients at risk of RS, 38 % covered the OPER on the fourth day of EN (p = 0.006), and those who adhered to ASNET had a greater chance of doing so compared to those who did not adhere (RR: 2.2, 95 % CI: 1.6-3.2, p < 0.0001) (Fig. 3).

Figure 3. Percentage of energy and protein achieved by patients during follow-up (A), and proportion of patients who reached the optimal requirement (80 %) according to adequate adherence to ASNET (B).
A total of 36 % of the included patients developed complications (16 patients had electrolyte alterations, with 8 who could be considered at risk of imminent RS without eventually developing it; 1 patient had a mechanical complication, and 1 had diarrhea), and of these, 96 % were observed in patients who did not adhere to ASNET. Interestingly, of all the patients who covered the OPER on the 4th day, 82 % did not have complications; however, 47 % of those who did not cover the OPER did present a complication (p = 0.03). Therefore, patients at risk of RS who did not present complications associated with EN are more likely to reach OPER on the fourth day of EN when compared to those who did (RR 0.4, 95 % CI, 0.2-0.6 p < 0.0001). Hospital length of stay was 18 days (11-25) with no significant differences between groups [19 days (12-25) in the adherence group vs 16 days in the nonadherence group (12-25); p = 0.27], and 75 % of the patients were discharged alive, with no differences in adherence to the algorithm (88 % of the group with adequate adherence vs 69 %; p = 0.07).
DISCUSSION
Protocols for EN support are effective in increasing the amount of nutrients provided to hospitalized patients in critical care units (20,22-26). For patients admitted outside critical areas, there is a lack of protocols, and EN prescriptions are based on studies designed for critical care patients. The ASNET was implemented in non-critical care areas and has been proven to be a well-tolerated and safe protocol with several beneficial effects, including early-start of nutritional support, an ability to meet caloric targets, and a reduced incidence of gastrointestinal and metabolic complications (15). Among these complications, RS is a life-threatening condition that occurs secondary to rapid and inadequate nutritional support in malnourished patients. In these scenarios, the ASNET is a practical option since it was design for hospitalized patients, including those who are at risk of RS. The ASNET assesses the risk of developing RS, allows the monitoring of patients, and helps to optimize and standardize the prevention of RS.
The present study focused on evaluating adherence to this protocol, specifically in patients at risk of RS with respect to OPER compliance, since this population is prone to receiving their diet more slowly and with a higher risk of undernourishment. When comparing the groups according to adherence to ASNET, significant differences were found in weight and consequently in BMI, these being larger in the group that did not adhere to the algorithm. This result may be secondary to the fact that only these parameters were considered when carrying out the initial RS risk screening and not the rest that include the recommendations established by the NICE guidelines. These guidelines include a low BMI and involuntary weight loss in a short time. But they also include little or no nutritional intake for approximately 5 to 10 days; or a history of alcohol and/or drug abuse, other medications (including insulin, chemotherapy, antacids or diuretics) or even low levels of potassium, phosphorus or magnesium prior to the start of feeding (18,19). Therefore, a complete evaluation is necessary considering all the criteria already established.
The percentage of patients who had adequate adherence to ASNET was low. This finding is similar to that by previous studies that found that compliance with evidence-based clinical guidelines is still a challenge (27). One reason could be that the prescribing staff are reluctant to adhere to new guidelines and prefer the convenience of continuing with regular therapy, or even that patient nutrition support does not receive the necessary attention by the medical or nursing staff, and that adherence is not usually recorded in the clinical record.
The NICE recommendations are the most frequently used guidelines in patients at risk of RS (28). Based on this and on the available evidence, the actual consensus proposed using a low caloric objective adjusted according to RS risk. In this consensus, the recommended initial energy intake was established on the risk categories (low, high and very high) with a gradual increment until the total caloric requirement is reached within 5 to 10 days (9). Considering the beneficial effects of nutrition in hospitalized patients, the risk of RS should not be a cause for suboptimal nutrition care (15,29).
The results in terms of the percentage of energy administered are consistent with those previously reported (15) and were found to be higher in patients who did adhered to ASNET, hence covering the optimal caloric requirement in the first days of hospitalization as recommended by international guidelines (5,24). Reaching the optimal nutritional requirements has various beneficial effects, including a reduction in complications as demonstrated by the EN protocols administered in the intensive care unit (11-13). This highlights that the highest proportion of patients who developed imminent RS (9) were those who did not cover their requirement by the fourth day. Previous studies emphasized that the gastrointestinal complications of EN can be significantly reduced after implementing an EN protocol (14). This was consistent with our findings in the present study. Therefore, this study demonstrates that the risk of RS and its associated complications can be managed with monitoring and an adequate EN protocol, as reported by other authors (20,29).
It should be remembered that RS is a complex complication of EN in which the biochemical alterations developed can trigger different issues that lead to prolonged hospitalizations, increased risk of infections and death, emphasizing that this last group was the one with the greatest complications of EN as a consequence of non-adherence to the established protocol. Our result agrees with the existing literature that reports that complications are reduced with the implementation of EN protocols (5,13,15).
Although it is suggested that lack of adherence to the algorithm is what causes the complications referred to as a consequence, it is possible that these were present and did not allow the planned nutritional increases. The foregoing is a limitation to the study and must be defined and evaluated in subsequent studies. Longer hospital stays and higher percentages of live discharges in the group that adhered to the protocol compared to the group that did not adhere could be due to other factors, such as underlying disease, severity, or higher incidence of complications.
Previous studies emphasize that caloric and protein adequacy through EN has been improved by the implementation of protocols (10,14,15). Similar data were found in the population analyzed in the present study, where patients at risk of RS who adhered to the ASNET obtained higher adequacy percentages than those who did not adhere. This finding can clarify that patients at risk of RS must improve adherence to a protocol to provide a gradual increase and achievement of the caloric requirement within 5 to 10 days, as recommended by Friedli (9,30). A high percentage (19 %) did not achieve the optimal caloric requirement in that period of time, although the majority of the population is at low risk of RS.
Currently, adherence to EN protocols is still far from ideal. Our study adds more evidence that the traditional practice continues despite the vast existing evidence and the proven efficacy and safety of the ASNET. One of the reasons is that EN is prescribed with slow infusion rates and increases; on the other hand, EN interruptions are always present, due to gastrointestinal intolerance, displacement or obstruction of the tube, and routine procedures, among others. This often causes underestimation of the restart table and, therefore, it is not used (25,31). It is essential to remember that to achieve tolerance, beneficial effects, and patient safety with EN, adequate guidelines should be followed for initiation and progression. Above all, teamwork and effective communication are essential in achieve this (23,24).
The positive results found in this study reveal that adherence to ASNET in patients at risk of RS allows optimization of EN support, similar to the results of other authors (14,15,26), which is necessary to continue implementing this algorithm and adjust it to the type of risk of RS that is present in each patient. Currently, there are no protocols developed for the introduction of EN in patients at risk of RS, representing the main strength of the present study and analyzed population, given that our institution is a center where patients with this condition are referred for this aspect of the algorithm.
There are limitations that must be recognized, and among them is that the recommendations were not reinforced by the nursing staff, as they are the responsible for manipulating interruptions in the administration and use of restart table. On the other hand, the ASNET does not include the caloric recommendation according to the current risk categories for RS (low, high and very high), since when it was first developed, there was no such categorization. It includes only a general recommendation that is currently used in patients with high and very high risk of RS, this being one of the items that was not fulfilled in its majority, since most of the study population was at low risk of SR, further limiting the proportion of patients with adherence to ASNET.
Despite its limitations, the present study has important implications that strongly support the efficacy of the ASNET in engaging patients hospitalized in non-critical areas, including those at risk of RS. Adherence to the ASNET in patients at risk of RS allows increasing the probability of achieving OPER safely in the recommended period of time, thus avoiding complications, and achieving the benefits of EN.















