Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
The European Journal of Psychiatry
versión impresa ISSN 0213-6163
Eur. J. Psychiat. vol.23 no.3 Zaragoza jul./sep. 2009
Motor speed predicts stability of cognitive deficits in both schizophrenic and bipolar I patients at one-year follow-up
J. Salazar-Fraile*,**,***, V. Balanzá-Martínez*,**, G. Selva-Vera*,**, A. Martínez-Aran**,****, J. Sánchez-Moreno**,****, C. Rubio*,**, E. Vieta**,****, M. Gómez-Beneyto*,**, R. Tabarés-Seisdedos*,**
* The Teaching Unit of Psychiatry and Psychological Medicine, Department of Medicine, University of Valencia, Valencia
** Centro de Investigación Biomédica en Red de Salud Mental (CIBERSAM), Ministry of Science and Innovation
*** Neurophysiology and Psychopathology Unit, Hospital Arnau de Vilanova, Consellería de Sanitat, Valencia
**** The Bipolar Disorders Program, Clinical Institute of Neuroscience, Hospital Clinic of Barcelona, IDIBAPS, University of Barcelona, Barcelona. Spain
ABSTRACT
Background: We examined whether motor speed assessed by the finger tapping test predicts generalized and specific stable deficits because of a common pathogenic process in bipolar and schizophrenic patients.
Methods: One hundred and two patients underwent a battery of neuropsychological tests. Patients with a score of less than one standard deviation from their siblings', sample in two assessments with an interval of one year were defined as suffering from stable deficits because of a common pathogenic process. In addition to univariate analyses, factor analyses, ordinal logistic regression, and multiple linear regressions were used. A general score was also calculated.
Results: No differences were found between schizophrenic and bipolar patients in the deficits of verbal fluency, shift reasoning ability and executive attention. Schizophrenic patients had greater persistent cognitive deficit because of a common pathogenic factor in the verbal memory dimension than bipolar patients. Motor speed predicted the specific deficits of verbal fluency, shift reasoning, executive attention and the general deficit of both bipolar I and schizophrenic patients. Bipolar patients suffered a lesser specific deficit in the verbal memory dimension than schizophrenic patients did, this domain not being predicted by motor speed. Motor speed predicted the generalized deficit and the specific dimensions in which schizophrenic and bipolar patients showed no differences.
Conclusions: These results suggest the presence of general and specific stable cognitive deficits because of a common pathogenic factor related to psychomotor slowness. Motor speed seems to be suitable endophenocognitype for schizophrenia and bipolar disorder.
Key words: Motor speed; Cognitive deficit; Schizophrenia; Bipolar I; Psychomotor slowness; Endophenotype
Introduction
Recent studies on cognitive functioning confirm consistently that schizophrenic and bipolar patients suffer from cognitive deficits1-7. It has been shown that schizophrenia is characterized by a broadly based cognitive impairment, present since the onset of the disease regardless of schizophrenic patients' baseline characteristics and clinical state8-10. However, a subgroup of schizophrenic patients with preserved intellectual functions and normal cognitive performances although with subtle executive and attentional deficits has also been identified11,12. Similar cognitive deficits have also been shown in bipolar patients, although to a lesser degree2,4,13, but at present, there is no agreement whether these two groups of patients with generalized or specific cognitive deficits can be identified in bipolar disorders. Cognitive deficits in schizophrenia are relatively stable in patients even when in remission, e.g., state independent14,15, whereas in bipolar patients, although a stable deficit has been shown2,4, test performances are more sensitive to symptomatology and clinical state of remission after an acute episode16,17. Furthermore, some studies carried out on healthy relatives of schizophrenic and bipolar patients have also described impairment in cognitive performances, although to a lesser degree than the patients, when compared with normal control subjects18-21. It has been suggested that schizophrenic patients suffer neurodevelopmental impairment in contrast to bipolar patients and that both groups of patients have similar poor cognitive performances because of a common pathogenic process that operates once illness has begun22. Thus, both pathogenic versus premorbid deficits and generalized versus specific deficits have been described.
Clinical studies consider psychomotor poverty as a core symptom of schizophrenia23 shown through negative symptoms (poverty of speech, movement, expressivity and emotion). In accordance with these studies, slower cognitive processing speed and slower motor performances have been described as a phenotype of the generalized cognitive deficit in schizophrenic patients both in cross-sectional24-28 and prospective studies29. In contrast to this evidence in schizophrenic patients, psychomotor poverty is not a core symptom in bipolar disorders. Whether psychomotor speed could be a phenotype marker of specific or generalized cognitive deficits in bipolar patients has not been clarified. Similarly, whether psychomotor speed could be a marker in pathogenic deficits in patients with schizophrenia or bipolar disorder has not been reported either.
Although a number of cognitive deficits have been reported, methodological issues must be considered in order to support a conclusion of pathogenic versus premorbid deficit. Deficits are usually established by comparing patients' cognitive performances with those of normal controls, and in the case of family studies, the comparison is often established with first-degree nonsibling relatives. Potential confounding factors, such as age, cohort effects, and level of education, can influence the overall analysis15. Moreover, as many previous studies have been carried out on small samples, clustering of tests into cognitive domains is usually done on a theoretical basis, varying among studies the number and type of tests used for each domain.
Taking into account these concerns, to assess pathogenic deficits the present study compares cognitive performances of bipolar and schizophrenic patients with those of a sample of patients' healthy siblings and defines the cognitive domains on an empirical basis by means of a factor analysis performed on the whole sample. The objectives of this study were 1) to determine whether in a large sample of schizophrenic and bipolar I patients, empirically determined deficits because of a common pathogenic process are different in each group, and 2) whether motor speed performances predicts stability of (general or specific) cognitive deficits.
Methods
Subjects
One hundred and two outpatients who consecutively attended any of the three mental health centers in the metropolitan area of Valencia that participated in patient recruitment over a nine-month period were recruited if they fulfilled the criteria of the Diagnostic and Statistical Manual of Mental Disorders-Fourth Edition30 for either schizophrenia (n = 53) or bipolar disorder type I (n = 49). A written consent form was obtained from all participants following an explanation of study procedures. The ethics committee of the University Clinic Hospital of Valencia (Spain) approved the research protocol. All subjects were aged between 18 and 60 years. Diagnoses were established with the Spanish version of the Schedules for Clinical Assessment in Neuropsychiatry31 after a minimum of one year's evolution of the illness. The exclusion criteria used were: current drug dependence or abuse, electroconvulsive therapy during the previous six months, and epilepsy, medical illness or a known organic cause that may account for either psychosis or cognitive abnormalities. Patients were interviewed using the Spanish adaptation of the Family History Research Diagnostic Criteria Interview (FH-RDC)32,33 and with the psychotic screening questionnaire of Bebbington and Nayani34 to confirm the absence of any family or personal history of psychiatric disorders respectively. They were assessed two times within a mean interval of 12.5 months. Twelve patients (five schizophrenic and seven with bipolar disorder) discontinued collaboration after inclusion in the study. The final sample consisted of 48 patients with schizophrenia and 42 with bipolar disorder. As control subjects, 35 patients' healthy siblings who lived in the same home were recruited, and four refused to participate. 21 (6 male and 15 female) were siblings of schizophrenic patients and 14 (4 male and 10 female) were siblings of bipolar patients.
Neuropsychological assessment
The assessment was performed according to Balanzá-Martínez et al.2 and Tabarés-Seisdedos et al.35. Briefly, all patients and control subjects completed a battery of nine tests measuring cognitive domains with the following sequence: executive functions-abstraction (Wisconsin Card Sorting Test (WCST) with three separate scores: categories, perseverative errors, and nonperseverative errors), categorical and phonological verbal fluency (Category Instant Generation Test (CIG); FAS Test of the Controlled Oral Word Association Test), immediate and working memory (the forward and backward parts of the Digit Span Test from the Wechsler Adult Intelligence Scale-Revised or WAIS-R), verbal memory (VM, the Babcock Story Recall Test-Immediate and Delayed Free Recall), visual-motor processing attention (the Stroop Color and Word Test with the Color-Word Interference trial), sustained attention from the Asarnow Continuous Performance Test (CPT) (the total number of hits and the total number of false alarms were calculated), and motor speed (finger tapping test FT). The last sequence was consistent for all subjects and was administered on the same day that the subject's clinical state was assessed.
Clinical assessment and sociodemographic and evolutive variables
On the same day, patients were rated according to the Positive and Negative Syndrome Scale36,37, for depressive symptoms with the Hamilton Rating Scale for Depression38,39 and for manic symptoms with the Clinician-Administered Rating Scale for Mania40,41. Classification of longitudinal course for schizophrenia was done by means of DSM-IV specifiers. As sociodemographic variables, gender and age were used. The evolutive variables used were years of illness duration, number of hospitalizations, and number of episodes of illness. As premorbid variables, we used age at onset, premorbid social adjustment, and years of education. Finally, the equivalent doses of antipsychotic, benzodiazepine, and anticholinergic medication, and daily doses of lithium and number of cigarettes smoked per day were used.
Statistical analysis
Clustering of the cognitive variables
We applied principal components analysis to test for clustering of the cognitive variables. The adoption of a four-factor structure was based on the rule of eigenvalues greater than 1 for each interpretable factor. Four cognitive domains were then extracted using a varimax (orthogonal) rotation: executive attention (Stroop test, Digit Span Forward, Digit Span Backward, and Asarnow CPT), shift reasoning (categories, perseverative errors, and nonperseverative errors of the WCST), verbal memory (Immediate and Delayed Recall of the Babcock Memory Test), and verbal fluency (FAS and CIG). Each test score was Z-transformed based on the sibling control group's mean and standard deviation. Persistent deficit was defined as having a score below 1SD of the control group mean in both cognitive assessments. Then a test-deficit binary variable (deficit vs no deficit) was obtained for each neuropsychological test. A domain deficit score for each cognitive domain was obtained by computing the proportion of test-deficit variables that each domain had (range 0-1); thus, a patient scoring 0.5 in one domain would have been classified as deficit in half of the neuropsychological tests of that domain, 0.25 would not have been classified as deficit in a quarter of the neuropsychological tests of that domain, a score of 1 would not have been classified as deficit in any of the neuropsychological tests of that domain etc. A global deficit score was obtained by adding the scores of each domain.
Analytical strategy
First, we studied the association between the clinical, evolutive, and premorbid variables with the binary deficit variables of each neuropsychological test, the specific domain deficits, and the general deficit variables. The X2 test, t test, Mann-Whitney U test, and Pearson and Spearman correlation tests were used for this univariate analysis. Second, those variables yielding significant results were analyzed by ordinal logistic regression for the deficit dimension variables, and multiple regression analysis was used for the global deficit variable as this variable had a normal distribution. In order to control multiple comparison variable bias, we repeated the analyses using Bonferroni's correction employing only those variables that reached a significance level < 0.02 in the univariate analyses. In both cases, the results were similar.
Results
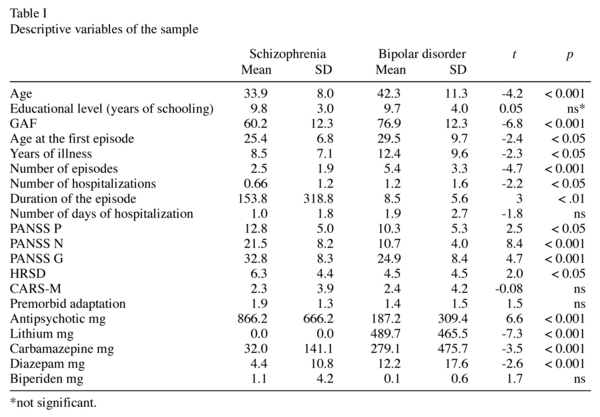
Patients and siblings did not show statistical differences for age (mean for patients = 38 years, mean for siblings = 34, t = 1.6, p = ns) or years of education (mean for patients = 9.8, mean for siblings = 11, t = -1.4, p = ns). Women accounted for a higher proportion in the control group (74%) than in the patient group (39%) (X2 = 12.8, p < 0.001). Clinical, evolutive and sociodemographic characteristics of the patients are reported in Table I.
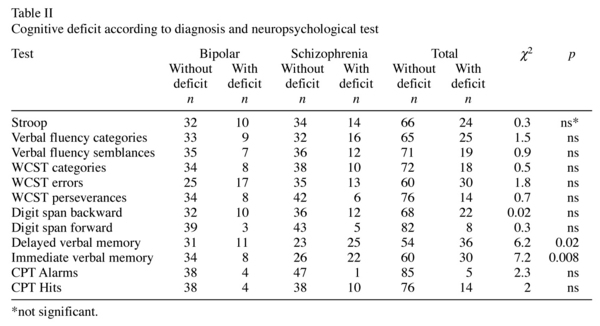
With respect to the neuropsychological variables, schizophrenic patients had a greater risk of deficit than bipolar patients did in the immediate (OR = 1.6, IC 95% = 1.1-2.4) and delayed (OR = 1.6, IC 95% = 1.1-2.4) free recall of the Babcock verbal memory test. No risk of deficit in any other neuropsychological test was significant (Table II).
Considering the cognitive dimensions, schizophrenic patients scored higher in verbal memory deficit than bipolar patients did (Mann-Whitney U = 946, p < 0.01), and no differences were found in executive attention, shift reasoning, or verbal fluency deficits. Correlations between cognitive dimensions and evolutive and clinical variables are shown in Table III. Neither dimension deficit nor the general deficit showed differences in the history of psychoses. The doses of antipsychotic medication correlated with the verbal memory deficit (r = 0.27, p < 0.01). The remaining deficit variables did not correlate with antipsychotic, benzodiazepine, or anticholinergic doses.
In schizophrenic patients, the course of the illness was associated with global deficit (Kruskal-Wallis = 7.9, p < 0.05). Specifically, those who had an evolutive type without interepisodic residual symptoms had lower global deficit than those who had interepisodic residual symptoms (Mann-Whitney U = 72.5, p < 0.05) or continuous symptoms (U = 34.5, p < 0.05). Functional outcome (GAF) was related with executive attention (r = 0.27, p < 0.01), verbal memory (r = 0.38, p < 0.001), verbal fluency (r = -0.25, p < 0.01) and general (r = 0.28, p < 0.01) deficits. GAF was not correlated with shift reasoning ability deficit. The number of cigarettes smoked per day was associated with a lower deficit in verbal fluency (r = 0.23, p < 0.05), shift reasoning ability (r = 0.37, p < 0.001), and verbal memory (r = 0.25, p < 0.01) deficits.
Motor speed
Males had a higher motor speed (FT) than women did (men mean = -0.9, women mean = -1.5, t = 3.5, p < 0.001), and siblings had a higher motor speed than patients did (-1.2 for patients vs 0.6 for siblings, t = 3.1, p < 0.01). Motor performances were correlated with doses of benzodiazepines (r = -0.28, p < 0.01) and the number of cigarettes smoked per day (r = 0.24, p = 0.05). FT correlated with Stroop (r = -0.46, p < 0.001), WCST categories (r = 0.41, p < 0.001), WCST errors (r = 0.43, p < 0.001), WCST perseverative errors (r = -0.35, p < 0.001), premorbid educational level (r = 0.34, p < 0.001), Asarnow CPT total (number of) hits (r = 0.5, p < 0.001), Babcok Story Recall immediate verbal memory (r = 0.27, p < 0.01), and Babcok Story Recall delayed verbal memory (r = 0.25, p < 0.05). CPT alarms did not correlate with FT. No differences were found by diagnostic group (bipolar vs schizophrenic) or type of antipsychotic (typical vs atypical).
FT correlated with every deficit dimension: executive attention (r = 0.44, p < 0.001), shift reasoning (r = 0.38, p < 0.001), verbal memory (r = 0.26, p < 0.001), verbal fluency (r = 0.38, p < 0.001), and general deficit (r = 0.45, p < 0.001) (Table III).
Multivariate analysis
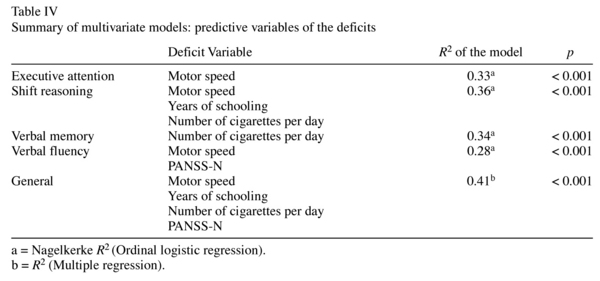
Ordinal Logistic Regression showed that only FT (coeff. = 0.85, Wald c2 = 6.5, p < 0.01) predicted executive attention deficit. Educational level, age, PANSS-P, PANSS-N and PANSS-G did not reach a significant level (Model c2 = 32.8, p < 0.001, Nagelkerke R2 = 0.33). shift reasoning deficit was predicted by educational level (coeff. = 0.2, Wald c2 = 6.1, p < 0.05), number of cigarettes smoked per day (coeff. = 0.05, Wald c2 = 6.6, p < 0.05) and FT (coeff. = 0.72, Wald c2 = 6.1, p < 0.01). Age and illness duration did not reach a significant level (Model c2 = 34.6, p < 0.001, Nagelkerke R2 = 0.36). Verbal memory deficit was predicted by number of cigarettes smoked per day (coeff. = 0.044, Wald c2 = 4.7, p < 0.05). Educational level, premorbid adjustment, FT, PANSS-P, PANSS-N, PANSS-G, doses of antipsychotic and diagnosis did not reach a significant level (Model c2 = 34.9, p < 0.001, Nagelkerke R2 = 0.38). Verbal fluency deficit was predicted by FT (coeff. = 0.78, Wald c2 = 6.0, p < 0.05) and PANSS-N (coeff. = -0.05, Wald c2 = 3.7, p < 0.05). Educational level and number of cigarettes smoked per day did not reach a significant level (Model c2 = 23.9, p < 0.001, Nagelkerke R2 = 0.28). Gender did not reach a significant level in any of the four models.
Multiple regression showed that general deficit was predicted by FT (b = 0.3, p < 0.001), educational level (b = 0.26, p < 0.01), PANSS-N (b = -0.26, p = 0.01) and number of cigarettes smoked per day (b = 0.2, p < 0.05, R2 = 0.41, Model f = 10.98, p = 0.001). Age and PANSS-G were not included in the model.A summary of the multivariate models is shown in Table IV.
Discussion
The current study has shown the existence of persistent cognitive deficits (specific and generalized) in a large sample of bipolar and schizophrenic outpatients. Both types of patients showed similar deficits, except for the verbal memory domain in which schizophrenic patients suffer from more severe deficits. Motor speed predicted persistence of deficits of executive attention, shift reasoning, verbal fluency and a general deficit, which are the dimensions that affect schizophrenic and bipolar patients to the same degree, in contrast to verbal memory deficit, which was not predicted by motor speed.
Executive attention, shift reasoning, and verbal fluency deficits are attributable to a common pathogenic process as their assessment has been done in comparison with a sample of siblings with the same characteristics of age and educational level, therefore controlling potential confounding factors such as socioeconomic level or cohort effects that are usually related to performance in neuropsychological tests. The higher proportion of females in the sibling sample is accounted for by the proportion of male siblings that had daytime work commitments and were therefore less likely to collaborate in the study. Nevertheless, multivariate analyses allowed us to control this confounding factor . The dimensions used had a good ecological validity as they are factors extracted from the sample studied and are therefore representative of the consecutive sample of patients attending three mental health centers. Our results confirm a common attention deficit factor shared by schizophrenic and bipolar patients related to motor speed. Factor analysis compiled the attention tests (Stroop, Digit Symbol, and Trail Making) into one dimension related with speed processing42-46. The relationship between speed processing deficits and attention deficits has been shown in schizophrenic patients suggesting common deficits in temporal perception processes8,9,28. The specific mechanism of poor performances in speed tasks and speed processing in patients with schizophrenia is not clear, although some studies have explained it by a deficit in the translation of stimulus-response47 or by instable attention reaction times that are affected when attention demands are increased26,48.
WCST is orthogonal with other executive tests and requires a set of tasks, some of them frontal, which involve mainly numeric complex visomotor processing and the ability to identify a relevant stimuli, working memory, mental set shifting, and speed processing46,49,50. In accordance with these results, our study has classified the WCST as a whole dimension of shift reasoning related to speed processing. Speed processing and executive function impairments seem to persist over time51.
Factor analysis compiled the immediate and delayed memory tasks of the Babcock memory test, which do not take into account time control, into one single memory dimension. In our study, schizophrenic patients showed greater deficit than bipolar patients did in these specific tests and in the memory dimension. Memory disorders have been shown in schizophrenic and, to a lesser degree, in bipolar patients13. Our results coincide with Daban et al.13, who have shown that verbal memory, and specifically immediate memory, seems to distinguish between both diagnostic groups, although these deficits are not specific to any diagnostic group. In contrast with our study, the association between memory deficit and speed processing has also been reported52; therefore, the verbal memory deficit could have been predicted by motor speed in our study. This difference can be accounted for if we consider that the tests used for memory measurements in other studies resemble those of verbal fluency and executive attention that we have used. Psychomotor functions have been reported to be significantly reduced in remitted bipolar patients as compared with healthy controls53. Schizophrenic and bipolar patients were neurocognitively impaired, with the schizophrenic group performing significantly worse on conceptual ability, verbal leaning, visuospatial processing, and motor speed54. Moreover, Seidman et al.55 also reported that bipolar patients showed moderate-to-large effect size decrements on perceptual-motor speed. Cognitive-motor disturbances may help to explain impairments in daily functioning in remitted bipolar patients56.
Factor analysis grouped phonemic fluency (words) and semantic fluency (animals) into the verbal fluency dimension. This result is consistent with Henry and Crawford57, who consider semantic and phonemic deficits as shortfalls associated with general intelligence and psychomotor speed. The verbal fluency tests tap somewhat different abilities compared with other executive measures (e.g., WCST) and although the mechanisms underlying verbal fluency remain to be worked out, word knowledge, episodic memory, working memory and speed of processing information appear to be integral components. In our study, verbal fluency deficits attributable to a common pathogenic factor are predicted by motor speed in both schizophrenic and bipolar disorders, and according to Henry and Crawford58, this deficit would show a generalized intellectual deficit instead of specific impairments in executive control.
Cigarette consumption has been reported to be higher among psychiatric patients than in the general population59. This behavior has been attributed to either a risk factor for some illnesses like schizophrenia or the search for remedies to alleviate and improve cognitive symptoms60. In our sample, cigarette consumption predicts a lesser deficit associated with verbal memory and shift reasoning. These results coincide with other studies that have shown an important role of nicotinic receptors on attention, learning and memory functions61, and by improvements in the performances of these functions after nicotine administration in schizophrenic patients62,63 or as a result of cigarette smoking64. A relationship between tobacco consumption and motor speed in schizophrenic patients regardless of other clinical, evolutive or medication variables has been shown65, confirming its stimulant effect by improving speed processing in medicated schizophrenic patients. Our results suggest that these effects could also be experienced by bipolar disorder patients with cognitive deficits and that the effect is not only short term but also long term.
Our finding that motor speed predicts cognitive deficits because of a pathogenic process presumably common to bipolar and schizophrenic disorders follows recent studies on the relationship between D2 dopamine receptor density and finger tapping tasks66,67. These authors have shown that striatal dopamine D2 receptor density is associated with an impaired performance in motor processing and time tasks in both schizophrenic and healthy subjects, with correlations between striatum D2 receptor density and finger tapping tasks that range between 0.5 for healthy subjects and 0.7 for schizophrenic patients. Furthermore, D2 receptor density correlated mainly with neuropsychological tests in which time measuring was involved (attentional tests), and a decrease in striatal dopamine D2 receptor density seemed to be associated with impaired performance in optimal timing tasks and motor speed processing. According to these results, the sensitivity of FT to age and to side effects of antipsychotic medication could also be explained in part by a decline of D2 receptor density. Although antipsychotic treatment is associated with a reduction in striatal D2 densities and performance on cognitive tasks is also known to be influenced by neuroleptics, in our study, neither the type of antipsychotic nor the doses have been associated with any deficit dimension.
One strength of this study is the definition of deficit by comparing a patient's cognitive performance with that of a sample of siblings living in the same home, avoiding confounding sociodemographic and rearing factors. The control group had a higher proportion of women, probably because of gender roles in Spain associated with care of relatives and a limitation of this study is that the small number of siblings not living in the patient's home, mainly males, would limit the external validity of the definition of deficit not being generalizable to this subgroup of siblings. Nevertheless, although the extent that the cognitive performances of these groups of siblings differ is not known, it is probable that they would not be influenced by gender roles. Eighty-eight percent of the sample finished the follow-up, and there were no significant differences between bipolar and schizophrenic patients. Potential loss of validity because of attrition would be small and would not affect diagnoses. Although the participants in this study were enrolled from three different psychiatric outpatient units and their symptom severity was similar to the subjects included in some studies' large samples, the extent to which we can generalize those findings is unknown.
Compared with their healthy siblings, a subgroup of schizophrenic and bipolar patients showed persistent cognitive deficits. Bipolar patients suffered a lesser deficit in the verbal memory dimension than schizophrenic patients did, this domain not being predicted by motor speed. On the other hand, motor speed predicted the generalized deficit and the specific domains in which schizophrenic and bipolar patients showed no differences. These results suggest the presence of general and specific persistent cognitive deficits because of a common pathogenic factor of both disorders that is related to psychomotor slowness. Thus, motor speed seems to be suitable endophenocognitype for schizophrenia and bipolar disorder68-71.
References
1. Addington J, Brooks B, Addington D. Cognitive functioning in first episode psychosis: initial presentation. Schizophr Res 2003; 62: 59-64. [ Links ]
2. Balanzá-Martínez V, Tabarés-Seisdedos R, Selva-Vera G, Matínez-Arán A, Torrent C, Salazar-Fraile J, et al. Persistent cognitive dysfunctions in bipolar I disorder and schizophrenic patients. A 3-year follow-up study. Psychother Psychosom 2005; 74: 113-119. [ Links ]
3. Bilder R, Goldman R, Robinson D, Reiter G, Bell L, Bates J, et al. Neuropsychology of first-episode schizophrenia: initial characterization and clinical correlates. Am J Psychiatry 2000; 157: 549-559. [ Links ]
4. Martínez-Arán A, Vieta E, Reinares M, Colom F, Sánchez-Moreno J, Benabarre A, et al. Cognitive function across manic or hypomanic, depressed, and euthymic states in bipolar disorder. Am J Psychiatry 2004; 161: 262-270. [ Links ]
5. Mohamed S, Paulsen JS, O'Leary D, Arndt S, Andreasen N. Generalized cognitive deficits in schizophrenia: a study of first episode patients. Arch Gen Psychiatry 1999; 56: 749-754. [ Links ]
6. Mur M, Portella M, Martínez-Arán A, Pifarré J, Vieta E. Persistent neuropsychological deficit in euthymic bipolar patients: executive function as a core deficit. J Clin Psychiatry 2007; 68: 1078-1086. [ Links ]
7. Townsend L, Malla A, Norman R. Cognitive function in stabilized first-episode psychosis patients. Psychiatry Res 2001; 104: 119-131. [ Links ]
8. Dickinson D, Iannone V, Wilk C, Gold J. General and specific cognitive deficits in schizophrenia. Biol Psychiatry 2004; 55: 826-33. [ Links ]
9. Heaton R, Gladsjo J, Palmer B, Kuck J, Marcotte T, Jeste D. Stability and course of neuropsychological deficits in schizophrenia. Arch Gen Psychiatry 2001; 58: 24-32. [ Links ]
10. Heinrichs R, Zakzanis K. Neurocognitive deficit in schizophrenia: a quantitative review of the evidence. Neuropsychology 1998; 12: 426-445. [ Links ]
11. Allen D, Goldstein G, Warnick E. A consideration of neuropsychologically normal schizophrenia. J Int Neuropsychol Soc 2003; 9: 56-63. [ Links ]
12. Kremen W, Seidman L, Faraone S, Toomey R, Tsuang M. The paradox of normal neuropsychological function in schizophrenia. J Abnorm Psychol 2000; 109: 743-752. [ Links ]
13. Daban C, Martínez-Aran A, Torrent C, Tabarés-Seisdedos R, Balanza-Martínez V, Salazar-Fraile J, et al. Specificity of cognitive deficits in bipolar disorder versus schizophrenia. A systematic review. Psychother Psychosom 2006; 75: 72-84. [ Links ]
14. Albus M, Hubmann W, Mohr F, Hechts S, Hinterberg-Weber P, Seitz N, et al. Neurocognitive functioning in patients with first-episode schizophrenia. Results of a prospective 5 year follow-up study. Eur Arch Psychiatry Clin Neurosci 2006; 256: 442-451. [ Links ]
15. Heydebrand G. Cognitive deficits in the families of patients with schizophrenia. Curr Opin Psychiatry 2006; 19: 277-281. [ Links ]
16. Liu S, Chiu C, Chang C, Hwang T, Hwu H, Chen W. Deficits in sustained attention in schizophrenia and affective disorders: stable versus state-dependent markers. Am J Psychiatry 2002; 159: 975-982. [ Links ]
17. Malhi GS, Ivanovski B, Hadzi-Pavlovic D, Mitchell PB, Vieta E, Sachdev P. Neuropsychological deficits and functional impairment in bipolar depression, hypomania and euthymia. Bipolar Disord 2007; 9: 14-25. [ Links ]
18. Glahn D, Bearden C, Niendam T, Escamilla M. The feasibility of neuropsychological endophenotypes in the search for genes associated with bipolar affective disorder. Bipolar Disord 2004; 6: 171-182. [ Links ]
19. Robinson L, Ferrier I. Evolution of cognitive impairment in bipolar disorder: a systematic review of cross-sectional evidence. Bipolar Disord 2006; 8: 103-116. [ Links ]
20. Sitskoorn M, Aleman A, Ebisch S, Appels M, Kahn R. Cognitive deficits in relatives of patients with schizophrenia: a meta-analysis. Schizophr Res 2004; 71: 285-295. [ Links ]
21. Snitz B, MacDonald A, Carter C. Cognitive deficits in unaffected first-degree relatives of schizophrenia patients: a meta-analytic review of putative endophenotypes. Schizophr Bul 2006; 32: 179-194. [ Links ]
22. Toulopoulou T, Quraishi S, McDonald C, Murray R. The Maudlsey Family Study: premorbid and current general intellectual function levels in familial bipolar I disorder and schizophrenia. J Clin Exp Neuropsychol 2006; 28: 243-259. [ Links ]
23. Liddle P. Schizophrenic syndromes, cognitive performance and neurological dysfunction. Psychol Med 1987; 22: 27-35. [ Links ]
24. Badcock J, Williams R, Anderson M, Jablensky A. Speed of processing and individual differences in IQ in schizophrenia: General or specific cognitive deficits? Cognit Neuropsychiatry 2004; 9: 233-247. [ Links ]
25. Flashman L, Flaum M, Gupta S, Andreasen N. Soft signs and neuropsychological performance in schizophrenia. Am J Psychiatry 1996; 153: 526-532. [ Links ]
26. Fuller R, Jahanshahi M. Concurrent performance of motor tasks and processing capacity in patients with schizophrenia. J Neurol Neurosurg Psychiatry 1999; 66: 668-671. [ Links ]
27. Gschwandtner U, Pflüger M, Aston J, Borgwardt S, Drewe M, Stieglitz R, et al. Fine motor function and neuropsychological deficits in individuals at risk for schizophrenia. Eur Arch Psychiatry Clin Neurosci 2006; 256: 201-206. [ Links ]
28. Silver H, Shlomo N. Perception of facial emotions in chronic schizophrenia does not correlate with negative symptoms but correlates with cognitive and motor dysfunction. Schizophr Res 2001; 52: 265-273. [ Links ]
29. Niendam T, Bearden C, Rosso I, Sanchez L, Hadley T, Nuechterlein K, et al. A prospective study of childhood neurocognitive functioning in schizophrenic patients and their siblings. Am J Psychiatry 2003; 160: 2060-2062. [ Links ]
30. American Psychiatric Association. Diagnostic and statistical manual of mental disorders (DSM-IV). Washington, DC: American Psychiatric Association; 1994. [ Links ]
31. Vázquez-Varquero J. SCAN: Cuestionarios para la Evaluación Clínica en neuropsiquiatría (adaptación al español). Santander: Unidad de Investigación en Psiquiatría Social de Cantabria, Servicio de Psiquiatría Hospital Universitario Marques de Valdecilla; 1993. [ Links ]
32. Endicott J, Andreasen N, Spitzer R. Family history RDC. 3rd ed. New York: New York State Psychiatric Institute. Biometrics Research; 1976. [ Links ]
33. Leal C, Gómez-Beneyto M, De Vicente T, Sanjuán J, Tabarés R. Adaptación de la historia familiar RDC para la investigación de la morbilidad psiquiátrica en familiares de pacientes psiquiátricos. Madrid: Actas del II Congreso de la Sociedad Española de Psiquiatría Biológica; 1988. [ Links ]
34. Bebbington P, Nayani T. The psychosis screening questionnaire. Int J Methods Psychiatr Res 1995; 5: 11-19. [ Links ]
35. Tabarés-Seisdedos R, Balanza-Martínez V, Salazar-Fraile J, Selva-Vera G, Leal Cercós C, Gómez-Beneyto M. Specific executive attentional déficits in patients with schizophrenia or bipolar disorder who have a positive family history of psychosis. J Psychiatry Res 2003; 37: 479-486. [ Links ]
36. Kay S, Opler L, Lindenmayer J. The positive and Negative Syndrome Scale (PANSS): rationale and standardisation. Br J Psychiatry (Suppl.) 1988; 155: 59-65. [ Links ]
37. Peralta V, Cuesta M. Síntomas esquizofrénicos positivos y negativos: un análisis del modelo dicotómico de la esquizofrenia. Actas Esp Psiquiatria 1990; 18: 266-273. [ Links ]
38. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatr 1960; 23: 56-62. [ Links ]
39. Ramos-Brieva J, Cordero-Villafáfila A. Validación de la versión castellana de la Escala de Hamilton para la Depresión. Actas Esp Psiquiatr 1986; 14: 324-334. [ Links ]
40. Altman E, Hedeker D, Peterson J, Davis J. The Altman Self-Rating Mania Scale. Biol Psychiatry 1997; 42: 948-955. [ Links ]
41. Livianos L, Rojo L, Guillem J, Villavicencio D, Pino A, Mora R, et al. Adaptación de la escala para la valoración de la manía por clínicos (EVMAC). Actas Esp Psiquiatr 2000; 28: 169-177. [ Links ]
42. Bondi M, Serody A, Chan A, Eberson-Schumate S, Delis D, Hansen L, et al. Cognitive and neuropathologic correlates of Stroop Color-Word Test performance in Alzheimer's disease. Neuropsychology 2002; 16: 335-343. [ Links ]
43. Boone K, Pontón M, Gorsuch R, González J, Miller B. Factor analysis of four measures of pre-frontal lobe functioning. Arc Clin Neuropsychol 1998; 13: 585-595. [ Links ]
44. Erlanger D, Feldman D, Kutner K, Kroger H, Festa J, Barth J, et al. Development and validation of a web-based neuropsychological test protocol for sports-related return-to-play decision making. Arch Clin Neuropsychol 2003; 18: 293-316. [ Links ]
45. Nigg J, Glass J, Wong M, Poon E, Jester J, Fitzgerald H, et al. Neuropsychological executive functioning in children at elevated risk for alcoholism: findings in early adolescence. J Abnorm Psychol 2001; 113: 302-314. [ Links ]
46. Strauss E, Sherman E, Spreen O. A compendium of Neuropsychological Tests: Administration, Norms, and Commentary, third ed. Oxford: Oxford University Press; 2006. [ Links ]
47. Manschreck T, Maher B, Candela S, Redmond D, Yurgelun-Todd, Tsuang M. Impaired verbal memory is associated with impaired motor performance in schizophrenia: relationship to brain structure. Schizophr Res 2000; 43: 21-32. [ Links ]
48. Fuller R, Jahanshahi M. Impairment of willed actions and use of advance information for movement preparation in schizophrenia. J Neurol Neurosurg Psychiatry 1999; 66: 502-509. [ Links ]
49. Greve K, Ingram F, Bianchini K. Latent structure of the Wisconsin Card Sorting Test in a clinical sample. Arch Clin Neuropsychol 1998; 13: 597-609. [ Links ]
50. Pukrop R, Matuschek E, Ruhrmann S, Brockhaus-Dumke A, Tendolkar I, Bertsch A, et al. Dimensions of working memory dysfunction in schizophrenia. Schizophr Res 1993; 62: 259-268. [ Links ]
51. Mur M, Portella M, Martínez-Arán A, Pifarré J, Vieta E. The long-term stability of cognitive impairment in bipolar disorder: a two-year follow-up study of lithium-treated euthymic bipolar patients. J Clin Psychiatry 2008; 69: 712-719. [ Links ]
52. Brébion G, David A, Bressan R, Pilowsky L. Processing speed: a strong predictor of verbal memory performance in schizophrenia. J Clin Exp Neuropsychol 2006; 28: 370-382. [ Links ]
53. Varga M, Magnusson A, Flekkøy K, Rønneberg U, Opjordsmoen S. Insight, symptoms and neurocognition in bipolar I patients. J Affect Disord 2006; 9: 1-9. [ Links ]
54. Varga M, Magnusson A, Flekkøy K, David A, Opjordsmoen S. Clinical and neuropsychological correlates of insight in schizophrenia and bipolar I disorder: does diagnosis matter? Compr Psychiatry 2007; 48: 583-591. [ Links ]
55. Seidman L, Kremen W, Koren D, Faraone S, Goldstein J, Tsuang M. A comparative profile analysis of neuropsychological functioning in patients with schizophrenia and bipolar psychoses. Schizophr Res 2002; 53: 31-44. [ Links ]
56. Martino D, Igoa A, Marengo E, Scápola M, Ais E, Strejilevich S. Cognitive and motor features in elderly people with bipolar disorder. J Affect Disord 2008; 105: 291-295. [ Links ]
57. Henry J, Crawford J. A meta-analytic review of verbal fluency performance in patients with traumatic brain injury. Neuropsychology 2004; 18: 621-628. [ Links ]
58. Henry J, Crawford J. A meta-analytic review of verbal fluency deficits in schizophrenia relative to other neurocognitive deficits. Cognit Neuropsychiatry 2005; 10: 1-33. [ Links ]
59. Berk M, Ng F, Wang WV, Tohen M, Lubman DI, Vieta E, et al. Going up in smoke: Tobacco smoking is associated with worse treatment outcomes in mania. Journal of Affective Disorders 2008; 110: 126-134. [ Links ]
60. Zammit S, Allebeck P, Dalman C, Hemmingsson T, Lewis G. Investigating the association between cigarette smoking in a cohort study. Am J Psychiatry 2003; 160: 2216-2221. [ Links ]
61. Levin E, McClernon F, Rezvani A. Nicotine effects on cognitive function: behavioral characterization, pharmacological specification, and anatomic localization. 2006; Psychopharmacology (Berl.) 2006; 184: 523-539. [ Links ]
62. Smith R, Warner-Cohen J, Matute M, Butler E, Kelly E, Vaidhyanathaswamy S. Effects of nicotine nasal spray on cognitive function in schizophrenia. Neuropsychopharmacology 2006; 31: 637-643. [ Links ]
63. Dépatie L, O'Driscoll G, Holahan A, Atkinson V, Thavundayil J, Ying Kin . Nicotine and behavioral markers of risks for schizophrenia: a double-blind, placebo-controlled, cross-over study. Neuropsychopharmachology 2002; 27: 1056-1070. [ Links ]
64. Sacco K, Termine A, Seyal A, Dudas M, Vessicchio J, Krishnan-Sarin S, et al. Effects of cigarette smoking on spatial working memory and attentional deficits in schizophrenia: involvement of nicotinic receptor mechanisms. Arch Gen Psychiatry 2005; 62: 649-659. [ Links ]
65. Silver H, Shlomo N, Hiemke C, Rao M, Ritsne M, Modai I. Schizophrenic patients who smoke have a faster finger tapping rate than non-smokers. Eur Neuropsychopharmacol 2002; 12: 141-144. [ Links ]
66. Yang Y, Chiu N, Chen C, Chen M, Yeh T, Lee I. Correlation between fine motor activity and striatal dopamine D2 receptor density in patients with schizophrenia and healthy controls. Psychiatry Res 2003; 123: 191-197. [ Links ]
67. Yang Y, Yeh T, Chiu N, Lee I, Chen P, Lee L, et al. Association between cognitive performance and striatal dopamine binding is higher in timing and motor tasks in patients with schizophrenia. Psychiatry Res 2004; 131: 209-216. [ Links ]
68. Seisdedos RT, Arias JS, Gómez-Beneyto M, Cercós CL. Early age of onset, brain morphological changes and non-consistent motor asymmetry in schizophrenic patients. Schizophr Res 1999; 37: 225-31. [ Links ]
69. Tabarés-Seisdedos R, Balanzá-Martínez V, Pallardó Y, Salazar-Fraile J, Selva G, Vilela C, et al. Similar effect of family history of psychosis on Sylvian fissure size and auditory P200 amplitude in schizophrenic and bipolar subjects. Psychiatry Res 2001; 108: 29-38. [ Links ]
70. Balanzá-Martínez V, Rubio C, Selva-Vera G, Martinez-Aran A, Sánchez-Moreno J, Salazar-Fraile J, et al. Neurocognitive endophenotypes (endophenocognitypes) from studies of relatives of bipolar disorder subjects: a systematic review. Neurosci Biobehav Rev 2008; 32: 1426-1438. [ Links ]
71. Tabarés-Seisdedos R, Balanzá-Martínez V, Sánchez-Moreno J, Martinez-Aran A, Salazar-Fraile J, Selva-Vera G, et al. Neurocognitive and clinical predictors of functional outcome in patients with schizophrenia and bipolar I disorder at one-year follow-up. J Affect Disord 2008; 109: 286-299. [ Links ]
![]() Correspondence:
Correspondence:
Prof. Dr. Rafael Tabarés-Seisdedos
Teaching Unit of Psychiatry and Psychological Medicine
Department of Medicine, University of Valencia
Blasco Ibáñez, 17
46010 Valencia. Spain
E-mail: Rafael.Tabares@uv.es
Received 31 December 2008
Revised 14 April 2009
Accepted 4 May 2009