Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
The European Journal of Psychiatry
versión impresa ISSN 0213-6163
Eur. J. Psychiat. vol.30 no.1 Zaragoza ene./mar. 2016
Major depression: does gender influence the risk of recurrence? A systematic review
Gilles Bertschya,b,c; Michel Veltend,b and Sébastien Weibela,c
a Department of Psychiatry and Mental Health, Strasbourg University Hospital, 1 place de l'Hôpital, 67091 Strasbourg. France
b Translational Medicine Federation, Medical School, Strasbourg University, Strasbourg. France
c INSERM Unit 1114, Strasbourg. France
d Department of Epidemiology and Public Health, University of Strasbourg, EA3430 1 place de l'Hôpital, 67091 Strasbourg. France
ABSTRACT
Background and Objectives: A woman's lifetime risk of major depression is almost twice as high as that of a man. Major depression is associated with a high risk of recurrence, but the question of a differential risk of recurrence between genders is unclear. Based on a systematic review of the literature, this paper attempts to answer the following question: "Following a major depressive episode, do women and men have the same risk of recurrence?".
Methods: We prospectively collected all studies from the period 2005-2014 where the variable gender was considered a potential predictor of recurrence. The database has also been expanded with articles cited in the bibliography of the prospectively collected articles and with a PubMed Database search covering the period January 2005-August 2014.
Results: Of the prospective studies (n = 98), most found no influence of gender on recurrence risk, but a minority, mostly large sample studies, found that female gender is a statistically significant risk factor for recurrence. Results suggest a probable female-to-male relative risk of recurrence between 1.0 and 1.2. Given the heterogeneity of the studies (length of follow-up, populations, nature of the studies, choice of dependant variables, statistical methods, and available data) no meta-analyses were performed. There are many interfering variables (age of onset, subchronic evolution, treatments, etc.) that can influence the results of prospective studies.
Conclusions: Women probably have a slightly higher risk of recurrence after a major depressive episode than men. This increased risk is much smaller than women's much higher lifetime risk of depression.
Key words: Depression; Recurrence; Relapse; Gender.
Introduction
Major depression is a highly prevalent disorder with a lifetime risk of 10 to 20%. For women this risk is almost twice as high as for men1. Major depression is associated with a high risk of recurrence. The lifetime risk of a further episode of major depression after an initial episode is probably around 50% or more2. The studies also evidenced that the longer the follow-up, the higher the recurrence rate3. Since a publication by the Mac Arthur Foundation Network on the Psychobiology of Depression4, recurrence has been usually defined in relation to remission, recovery and relapse, with "full remission" defined as a brief period during which the individual is symptom-free, "recovery" as a period without symptoms lasting at least eight weeks, and "relapse" as a return to symptoms matching the full syndrome criteria for a depressive episode occurring during remission but before recovery. "Recurrence" is defined as a new episode following a period of recovery. This is now almost a standard definition; although recurrence studies may use slightly different definitions, for instance as regards the threshold for the symptoms of recurrence.
Burcusa and Iacono2 stated that "despite women being at increased risk for developing depression and for depression relapse, female gender does not appear to be a significant risk factor for recurrence". This statement about a greater risk of relapse but not recurrence was based on another review of depression and gender issues stating that "despite women being at increased risk for developing depression and for depression relapse, female gender does not appear to be a significant risk factor for recurrence". This statement about a greater risk of relapse but not recurrence was based on another review of depression and gender issues1. A few years previously another review concluded that the findings were controversial5. More recently, a review of the predictors of recurrence6 mentioned two studies that showed a higher risk in women. The issue of gender and the risk of recurrence were not central to any of these four reviews, and the number of cited references was very limited. To the best of our knowledge, a specific and systematic review of this issue, based on a large number of studies, has never been published. That is why we propose to conduct such a review ourselves, with a view to answering the following question: "Following a major depressive episode, do women and men have the same risk of recurrence?"
Methods
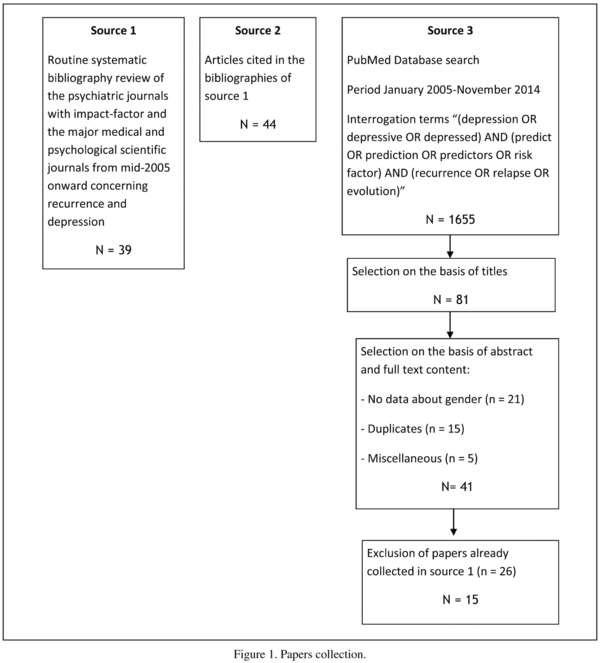
Most of the articles came from a personal database built by the first author on the recurrence of depression. The database received prospective input from a routine systematic bibliography review of psychiatric journals with impact-factor and the major medical and psychological scientific journals from mid-2005 onwards. It was also enriched with articles cited in the bibliographies of the other articles. For the purpose of our review, we selected all the articles in our personal database that provided information about an association between gender and the recurrence of unipolar major depression in the context of a prospective study. In addition, a systematic PubMed Database search was made covering the period January 2005 to November 2014 for the terms "(depression OR depressive OR depressed) AND (predict OR prediction OR predictors OR risk factor) AND (recurrence OR relapse OR evolution)". The papers to be included in our review were then selected using the following selection process: exclusion of papers whose title revealed that their content was not related to our review, then exclusion of papers whose abstract or full content failed to meet our inclusion criteria (prospective studies, unipolar major depression), overlapped with another paper (when the same sample of probands were used in different studies) or were already included in our prospectively collected database. A summary of the data collection process is presented in Figure 1.
Few studies examined the gender and recurrence status directly. To maximise the number of studies, we included prospective studies that did not explore gender in the context of depression specifically, but in which gender was one of the specifically addressed variables or covariates. We included epidemiological cohort studies, studies relating to clinical trials involving pharmacotherapy or psychotherapy, and studies about biological markers. Thus, we expected a high degree of heterogeneity from the studies. Besides the aforementioned criteria concerning the dependent variable and length of studies, many other variables could affect the risk of recurrence (2) and contribute to the heterogeneity of the studies. We include information about these variables and examine their possible influence in the Results section. A first variable concerned the diagnostic criteria (most of the time DSM III, III-R or IV were used, but some studies relied on other diagnostic systems, and in a few cases proxies such as admission to hospital for depression or prescription of antidepressants were used for the depression diagnosis). Other variables were the age of the sample, where patients were recruited (general population, primary, secondary or tertiary care, or health insurance database), the context of the study (epidemiological cohort studies, studies relating to clinical trials involving pharmacotherapy or psychotherapy, or studies about biological markers). Studies could also include probands regardless of the number of previous episodes, or could specifically target the recurrence risk after an initial episode. Given the many variables that could contribute to the heterogeneity of the studies we did not consider using meta-analytical methods.
To structure our presentation of so many papers we used three criteria. First, we divided the papers into different tables according to the dependant variable for recurrence (recurrence versus no recurrence as a qualitative dependant variable versus time to recurrence as a quantitative dependant variables) and according to the quality of the statistics (univariate versus multivariate analyses). Kuehner1 concluded from her review that women had a higher risk of relapse but not recurrence. Therefore, to take account of the duration of follow-up that can distinguish between relapse and recurrence, we presented the studies by decreasing length of follow-up.
Results
Overview of selected studies
We collected 98 papers, most of them from the prospectively collected database (n = 39), or from the papers cited by these articles (n = 44). The systematic PubMed Database research for the period January 2005-November 2014 provided a few additional papers (n = 15). The initial search produced a list of 1655 references, 81 of which were selected based on the title. Forty of them were excluded (21 included no data about gender, 15 were duplicates of other studies, 2 concerned minor depression, 2 included bipolar depression cases without control of the polarity, 1 was about persistence of depression) and of the 41 remaining papers, 26 were already in our own personal database.
The results are presented in three tables. Tables 1 and 2 concern studies that use recurrence as a qualitative variable. Table 1 presents studies that used only univariate statistics (n = 24), whereas Table 2 presents studies (n = 51) using multivariate statistics (among them, gender was sometimes not included in the multivariate model because it was not significant in univariate analyses). Table 3 concerns studies that used time to recurrence as the dependant variable, and all of them used multivariate statistics (n = 24). Two studies presented shorter- and longer-term data in two different papers. We included both papers for each. One long-term study also provided short-term results in the same paper with the same methodology. It is listed once in Table 27. One study8 included short-term and long-term data in the same paper with different statistical methodology and is therefore mentioned in two different tables (Tables 1 and 3), which is why there are 99 citations in our tables although we collected 98 papers.
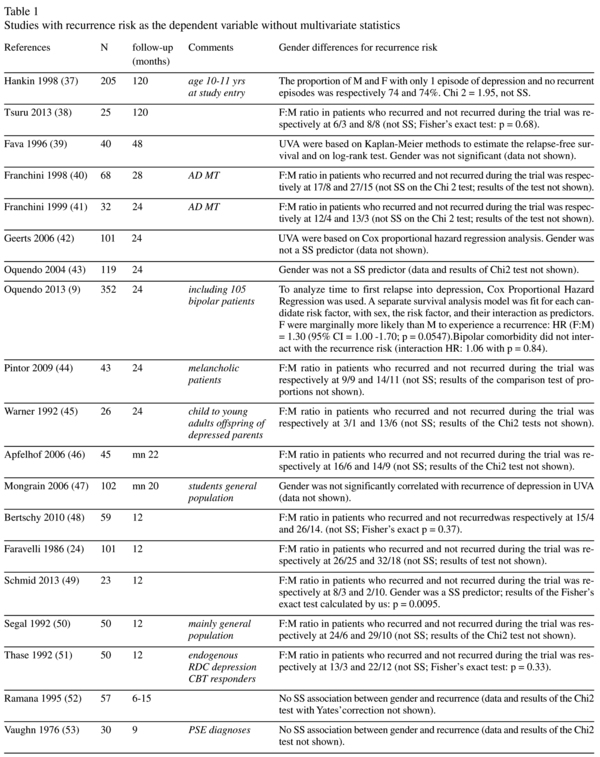
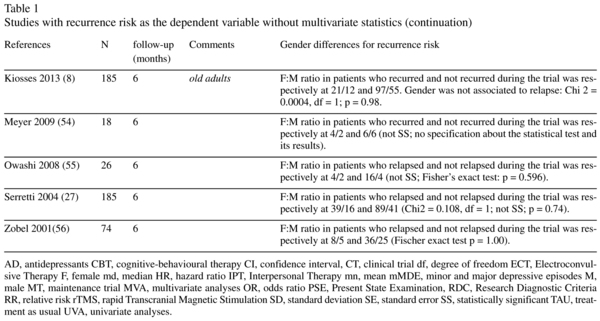
Risk of recurrence and gender: univariate statistics studies (Table 1)
Twenty-four studies presented data about the association between gender and recurrence during the follow-up period using only univariate statistics. All of the studies found a lack of association, although one study found there was a nearly significant (p < 0.06) higher risk of recurrence in women9.
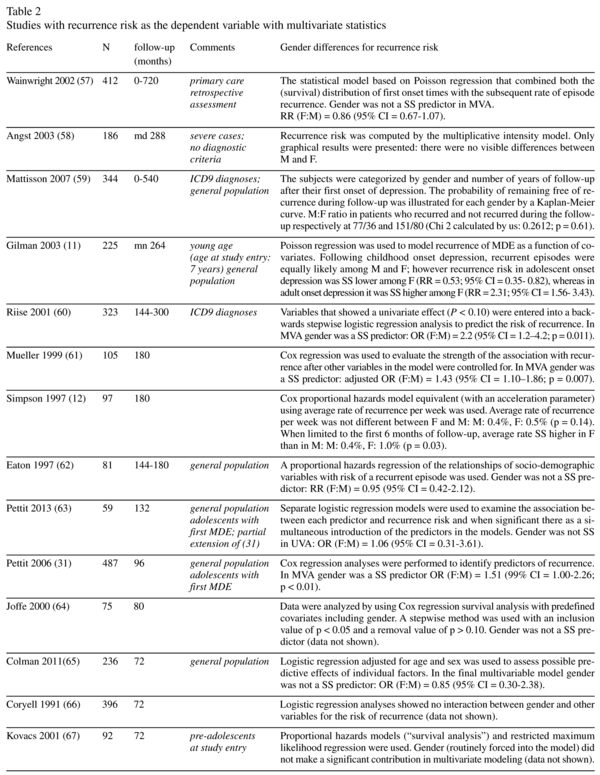
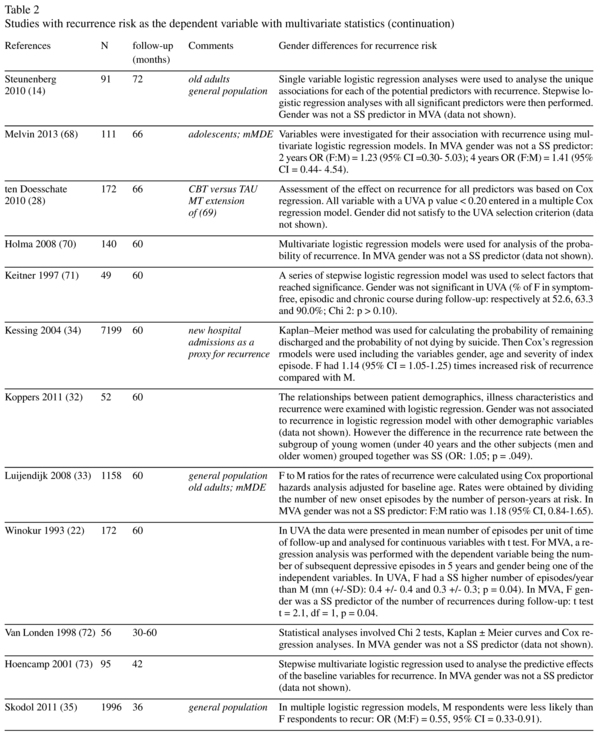
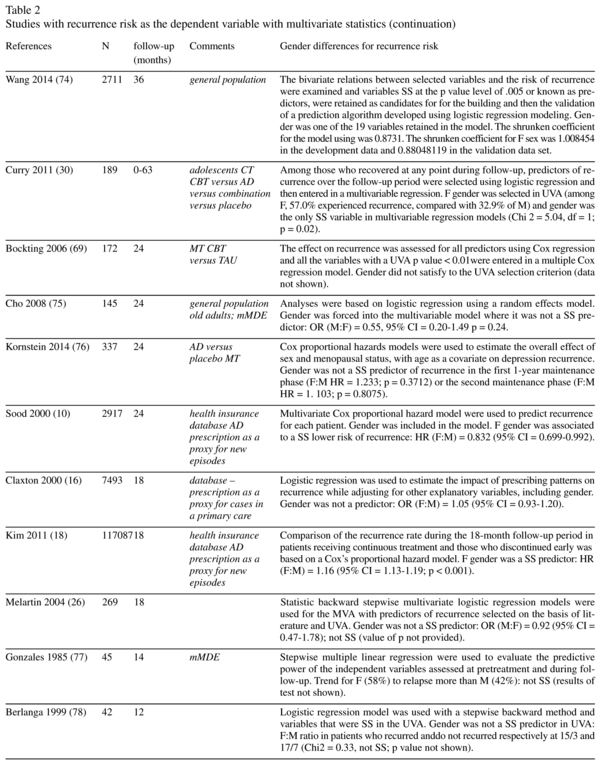
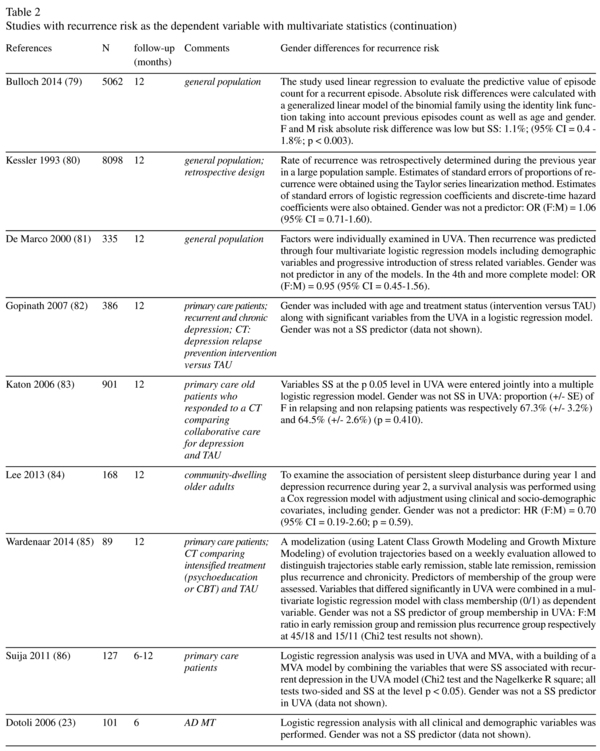
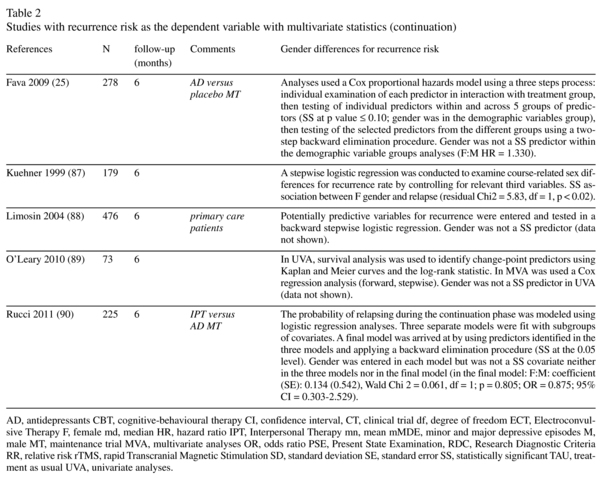
Risk of recurrence and gender: multivariate statistics studies (Table 2)
Fifty-one studies provided data about the association between gender and recurrence during the follow-up period using multivariate statistics (table 2). Thirteen studies (25.5%) found a statistically significant higher rate of recurrence among women, compared with only two studies that found a statistically significant higher rate of recurrence in men. Of these two studies showing a higher risk of male recurrence, one used data extracted from a health insurance database10 whereas the other 11 contributed to both sides of the gender-related risk insofar as it showed a significantly higher risk of recurrence for men in adolescent-onset depression and a significantly higher risk of recurrence for women in adult-onset depression. Another study12 found a significant higher risk of relapse for women in the first 6 months but not long-term (15-year follow-up period). There was also one study that found a non-significant trend towards a higher proportion of recurrence in women and two studies that showed a higher risk of recurrence for women in univariate but not multivariate analyses. Of the 13 significant studies, 9 provided values for ratios (odds-ratio, hazard ratio or relative risk). In the majority of cases, the ratios were below 2 and sometimes very close to 1. Of the studies which found no gender influence and which provided values for the odds-ratio, hazard ratio or relative risk, the majority (11 out of 16) found that the ratio tended towards a higher risk in women.
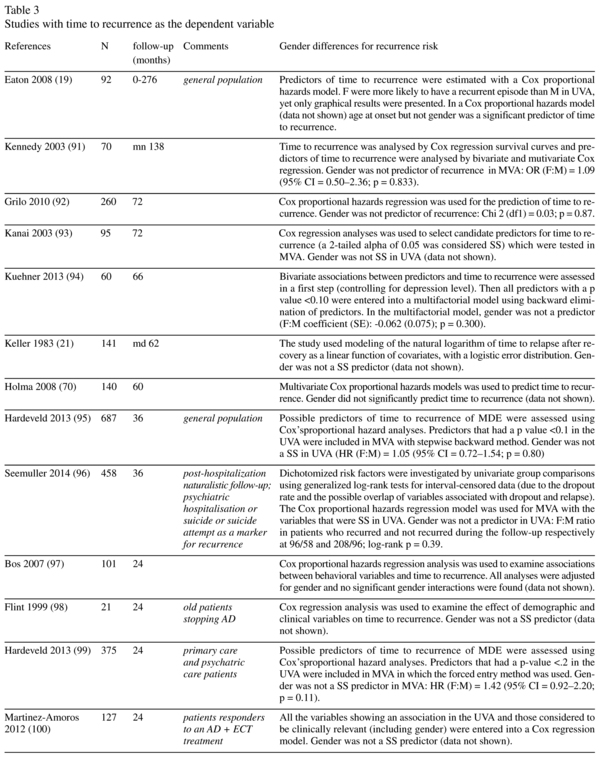
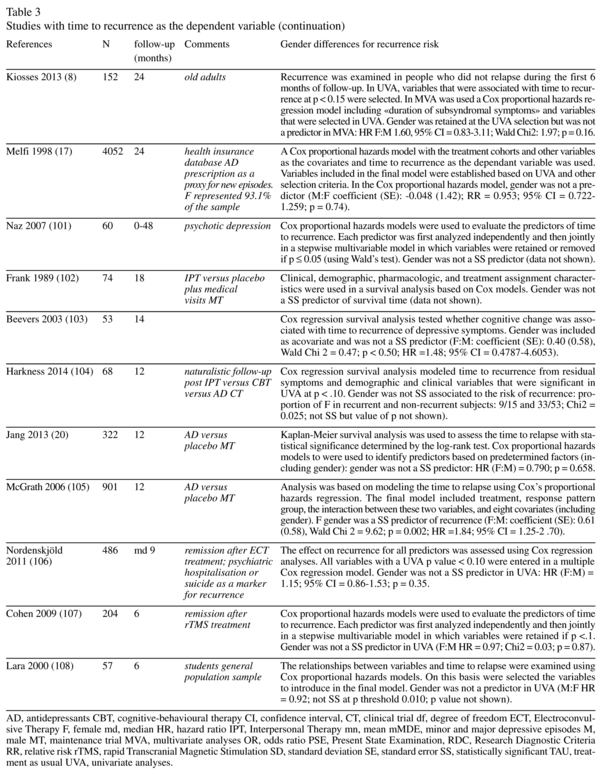
Time before recurrence and gender (Table 3)
Twenty-four studies provided data about the association between gender and the time before recurrence in the follow-up period with multivariate statistics (Table 3). One study found a statistically significant higher rate of recurrence among women13. In 3 of the studies which found no gender influence and which provided values for the odds-ratio, hazard ratio or relative risk (n = 5), the ratio denoted a higher risk in women. There were also three studies which showed a higher risk of recurrence for women in univariate but not multivariate analyses.
Influence of length of follow-up period
The follow-up period ranged from 6 months for some studies to several decades for some of the subjects in the longer-term studies. A higher short-term recurrence risk (in the 6 months after remission) in women has been suggested by Kuehner1. No obvious links between follow-up duration and the significance of the results emerged from the data we collected. However, some of the individual results are noteworthy. One result goes against Kuhnert's hypothesis, insofar as during a 6-year follow-up study of older adults, recurrence among women was significantly more frequent after three years of follow-up than before three years of follow-up14. Two studies lent some support to the Kuehner hypothesis. In the first study12 there was no effect of gender on the long-term recurrence risk, but during the first 6 months the risk was significantly higher in women (weekly recurrence rates for men and women were 0.4 and 0.5% respectively on long term and 0.4 and 1.0 % respectively in the first 6 months). The second study15, which is the one upon which Kuehner1 based her opinion, used new hospital admission as a proxy for recurrence. In this long-term (22-year) case register study of hospital admissions for unipolar depression, female patients had a slightly higher rate of recurrence (new admission) than male patients after all episodes, but the rate decreased after the first three episodes. The female-to-male hazard ratio was in the range of 1.09-1.13 for the first three new admission episodes but dropped to 1.04 beyond three episodes (a value no longer significant). Overall, the support for the hypothesis of a higher recurrence risk in women in the short-term but not long-term is very limited.
Influence of sample size
The only almost significant recurrence study to use univariate statistics (Table 1) was the largest study in its category, and the only significant time-to-recurrence study (Table 3) was the second largest study in its category. With respect to the recurrence studies that used multivariate statistics (Table 2), we see an association between the rate of significant studies and sample size, insofar as a significant higher recurrence risk for women was found in 7%, 25% and 56% of studies with sample sizes below 100 (n = 14), in the 100-1,000 range (n = 28) and above 1,000 (n = 9) respectively. With respect to Table 2, it should be noted that one study which found a higher risk of recurrence for men was a large-sample study (n = 2,917) based on data extracted from a health insurance database10. Overall, the influence of female gender on the risk of recurrence is preferentially found in studies involving a large sample which is in agreement with a low intensity influence.
Influence of the population studied
Most studies concern patients assessed and treated in psychiatric settings, but some dealt with primary care patients or general population probands or used data from health insurance databases. The latter were based on very large samples, and in these studies, prescriptions of antidepressants help to identify the index episode and are used as a proxy for identifying recurrences. Thus, case determination in these studies is more approximate than in studies where the probands are assessed directly. Of the four health insurance database studies, one found a significantly higher risk of recurrence in men (10). Of the other three studies, two16,17 found no predictive effect of gender and one18, which used a very large sample (n = 117,087), found that female gender was a significant recurrence predictor. It might be the case that gender influences the probability of receiving antidepressants when depressed. Concerning primary care patient studies, none of them (n = 6) found any gender influence whereas regarding the general population studies there were 3 positive studies for 11 negative ones. Finally, there is no obvious influence of population profile on the relationship between gender and the depression recurrence risk.
Influence of age
Studies involving pre-adolescents, adolescents or very young adults concentrate on early-onset subjects, and early onset is a predictor of depression recurrence in some19-22 but not all studies23-28. At the other end of lifespan, studies involving only old patients include a mixture of cases of adult-onset recurrent depression with cases of late-onset depression (either first or recurrent episodes) which have specific etiological factors linked to neurological disorders29. Of the 73 papers reviewed in Tables 2 and 3, 7 concerned pre-adolescents, adolescents or very young adults, and three found a significant higher female risk of recurrence11,30,31. In the 3 studies that found no significant influence of gender and provided odds-ratio values, the hazard ratio or relative risk tended towards a higher risk in women. Owing to the small number of studies, it is not possible to conclude that there is an interaction between female gender and early onset that increases the recurrence risk. Maybe it is even more complex, as evidenced in a cohort study covering childhood to adulthood with a long follow-up period (mean 22 years)11. In this particular study, gender did not influence the risk of recurrence of childhood onset depression (14 years or less), which is the subgroup with the highest risk of recurrence, but the recurrence risk with adolescent onset depression (15 to 20 years) was significantly lower among women, whereas with adult onset depression (21 years or more) it was significantly higher among women. In another adult study32 the higher recurrence risk was particularly acute for women under 40. Thus, it may be that the differential risk for women is high in young adult women. As regards old age, our panel of studies included 7 studies of older patients. None of them showed a significant influence of female gender, and of the 5 studies that found no gender influence but provided values for the odds-ratio, hazard ratio or relative risk, in 4 out of the 5 studies the ratio tended towards a higher risk for women. There is nothing to support speculation about a different gender-recurrence risk interaction in older patients compared with other adult patients. In one study33, the gender recurrence risk differential showed no difference between young, old and old-oldest adults.
Discussion
Female gender predicts a higher risk of recurrence of major depression in a minority of studies. Only one study that used a health insurance database found a result that supported a higher risk for men. A majority of non-significant studies tended towards a higher risk for women, and in a few studies female gender was a significant predictor of recurrence risk in univariate analyses but not multivariate analyses. The best explanation we found for the discrepancy between studies is sample size. Studies involving large samples are more frequently statistically significant for a higher recurrence risk in women. All these aspects favour a small excess of recurrence risk in women, much lower than the women-to-men relative lifetime depression risk which is around 2. In respect of the relative risk, odds ratio, or hazard ratio presented in the Results section, the mean relative risk is probably in the 1.0 to 1.2 range. For instance, of the 9 studies that had a sample size of more than 1000, 7 found a relative risk, odds ratio, or hazard ratio in this 1.0-1.2 range, one35 was in a higher range (1.82), and the last one found a higher risk in men10. This risk seems to be independent of the study population (psychiatric or primary care or general population. There is no clear evidence that the excess of recurrence risk could be limited to the short term, as suggested by Kuehner1.
This review has its limitations. At the outset, the authors chose to seek out and collect a wide range of informative studies (and, indeed, we found a large number of informative studies). Consequently, the studies are very heterogeneous. Some of the heterogeneous aspects, namely choice of the dependent variable (recurrence or time to recurrence), duration of follow-up, sample sizes, types of population, have been incorporated in the presentation and the discussion of the results. This heterogeneity also explains the lack of meta-analysis, the main reason being the broad differences in the length of follow-up. When we grouped together studies with the same length of follow-up and available data, the sets of studies were very small, and very heterogeneous in terms of their population. How we collected our studies may be open to debate. There are other issues that also need to be addressed. First, any approach that regards depression as a purely episodic disorder is an approximate one. Second with long-term follow-up, there could be a change of diagnosis, specifically from unipolar to bipolar mood disorders. Third, treatment may influence the risk of recurrence, and this is a variable that could be different in a clinical population or the general population. Fourth, the length of the interval between remission of the last episode and the start of follow-up could vary among studies or among patients within the same study. Fifth, as pointed out by Monroe and Harkness36, most studies about recurrence compared patients with recurrence with patients without recurrence, but some of the patients in the second group may already have had one or more prior episodes whereas others may never have had any recurrence in the past nor ever will have in the future. Lastly, our review covered mainly North American and European studies.
Conclusion
In conclusion, this review, which was based on a large number of studies, suggests women have a much higher risk of lifetime depression than men (overrisk around 2), but that their risk of recurrence is only slightly higher than that of men. As regards people with a history of depression, the risk of a new episode is only slightly higher in women than in men (overrisk probably between 1.0 and 1.2).
Conflicts of interest
None.
References
1. Kuehner C. Gender differences in unipolar depression: an update of epidemiological findings and possible explanations. Acta Psychiatr Scand. 2003; 108(3): 163-74. [ Links ]
2. Burcusa SL, Iacono WG. Risk for recurrence in depression. Clin Psychol Rev. 2007; 27(8): 959-85. [ Links ]
3. Steinert C, Hofmann M, Kruse J, Leichsenring F. The prospective long-term course of adult depression in general practice and the community. A systematic literature review. J Affect Disord. 2014; 152-154: 65-75. [ Links ]
4. Frank E, Prien RF, Jarrett RB, Keller MB, Kupfer DJ, Lavori PW, et al. Conceptualization and rationale for consensus definitions of terms in major depressive disorder. Remission, recovery, relapse, and recurrence. Arch Gen Psychiatry. 1991; 48(9): 851-5. [ Links ]
5. Piccinelli M, Wilkinson G. Gender differences in depression. Critical review. Br J Psychiatry. 2000; 177: 486-92. [ Links ]
6. Hardeveld F, Spijker J, De Graaf R, Nolen W, Beekman A. Prevalence and predictors of recurrence of major depressive disorder in the adult population. Acta Psychiatr Scand. 2010; 122(3): 184-91. [ Links ]
7. Alfaro CL, Lam YW, Simpson J, Ereshefsky L. CYP2D6 inhibition by fluoxetine, paroxetine, sertraline, and venlafaxine in a crossover study: intraindividual variability and plasma concentration correlations. J Clin Pharmacol. 2000; 40(1): 58-66. [ Links ]
8. Kiosses DN, Alexopoulos GS. The prognostic significance of subsyndromal symptoms emerging after remission of late-life depression. Psychol Med. 2013; 43(2): 341-50. [ Links ]
9. Oquendo MA, Turret J, Grunebaum MF, Burke AK, Poh E, Stevenson E, et al. Sex differences in clinical predictors of depression: a prospective study. J Affect Disord. 2013; 150(3): 1179-83. [ Links ]
10. Sood N, Treglia M, Obenchain RL, Dulisse B, Melfi CA, Croghan TW. Determinants of antidepressant treatment outcome. Am J Manag Care. 2000; 6(12): 1327-36. [ Links ]
11. Gilman SE, Kawachi I, Fitzmaurice GM, Buka L. Socio-economic status, family disruption and residential stability in childhood: relation to onset, recurrence and remission of major depression. Psychol Med. 2003; 33(8): 1341-55. [ Links ]
12. Simpson HB, Nee JC, Endicott J. First-episode major depression. Few sex differences in course. Arch Gen Psychiatry. 1997; 54(7): 633-9. [ Links ]
13. McGrath PJ, Stewart JW, Quitkin FM, Chen Y, Alpert JE, Nierenberg AA, et al. Predictors of relapse in a prospective study of fluoxetine treatment of major depression. Am J Psychiatry. 2006; 163(9): 1542-8. [ Links ]
14. Steunenberg B, Beekman ATF, Deeg DJH, Kerkhof AJFM. Personality predicts recurrence of late-life depression. Journal of Affective Disorders. 2010; 123(1-3): 164-72. [ Links ]
15. Kessing LV. Recurrence in affective disorder. II. Effect of age and gender. Br J Psychiatry. 1998; 172: 29-34. [ Links ]
16. Claxton AJ, Li Z, McKendrick J. Selective serotonin reuptake inhibitor treatment in the UK: risk of relapse or recurrence of depression. Br J Psychiatry. 2000; 177: 163-8. [ Links ]
17. Melfi CA, Chawla AJ, Croghan TW, Hanna MP, Kennedy S, Sredl K. The effects of adherence to antidepressant treatment guidelines on relapse and recurrence of depression. Arch Gen Psychiatry. 1998; 55(12): 1128-32. [ Links ]
18. Kim KH, Lee SM, Paik JW, Kim NS. The effects of continuous antidepressant treatment during the first 6 months on relapse or recurrence of depression. J Affect Disord. 2011; 132(1-2): 121-9. [ Links ]
19. Eaton WW, Shao H, Nestadt G, Lee HB, Bienvenu OJ, Zandi P. Population-based study of first onset and chronicity in major depressive disorder. Arch Gen Psychiatry. 2008; 65(5): 513-20. [ Links ]
20. Jang S, Jung S, Pae C, Kimberly BP, Craig Nelson J, Patkar AA. Predictors of relapse in patients with major depressive disorder in a 52-week, fixed dose, double blind, randomized trial of selegiline transdermal system (STS). J Affect Disord. 2013; 151(3): 854-9. [ Links ]
21. Keller MB, Lavori PW, Lewis CE, Klerman GL. Predictors of relapse in major depressive disorder. Jama. 1983; 250(24): 3299-304. [ Links ]
22. Winokur G, Coryell W, Keller M, Endicott J, Akiskal H. A prospective follow-up of patients with bipolar and primary unipolar affective disorder. Arch Gen Psychiatry. 1993; 50(6): 457-65. [ Links ]
23. Dotoli D, Spagnolo C, Bongiorno F, Zanardi R, Serretti A, Smeraldi E, et al. Relapse during a 6-month continuation treatment with fluvoxamine in an Italian population: the role of clinical, psychosocial and genetic variables. Prog Neuropsychopharmacol Biol Psychiatry. 2006; 30(3): 442-8. [ Links ]
24. Faravelli C, Ambonetti A, Pallanti S, Pazzagli A. Depressive relapses and incomplete recovery from index episode. Am J Psychiatry. 1986; 143(7): 888-91. [ Links ]
25. Fava M, Wiltse C, Walker D, Brecht S, Chen A, Perahia D. Predictors of relapse in a study of duloxetine treatment in patients with major depressive disorder. J Affect Disord. 2009; 113(3): 263-71. [ Links ]
26. Melartin TK, Rytsala HJ, Leskela US, Lestela-Mielonen PS, Sokero TP, Isometsa ET. Severity and comorbidity predict episode duration and recurrence of DSM-IV major depressive disorder. J Clin Psychiatry. 2004; 65(6): 810-9. [ Links ]
27. Serretti A, Zanardi R, Franchini L, Artioli P, Dotoli D, Pirovano A, et al. Pharmacogenetics of selective serotonin reuptake inhibitor response: a 6-month follow-up. Pharmacogenetics. 2004; 14(9): 607-13. [ Links ]
28. ten Doesschate M, Bockting C, Koeter M, Schene A, Group DS. Prediction of recurrence in recurrent depression: a 5.5-year prospective study. J Clin Psychiatry. 2010; 71(8): 984-91. [ Links ]
29. Alexopoulos GS. Depression in the elderly. Lancet. 2005; 365(9475): 1961-70. [ Links ]
30. Curry J, Silva S, Rohde P, Ginsburg G, Kratochvil C, Simons A, et al. Recovery and recurrence following treatment for adolescent major depression. Arch Gen Psychiatry. 2011; 68(3): 263-9. [ Links ]
31. Pettit JW, Lewinsohn PM, Joiner TE, Jr. Propagation of major depressive disorder: relationship between first episode symptoms and recurrence. Psychiatry Res. 2006; 141(3): 271-8. [ Links ]
32. Koppers D, Peen J, Niekerken S, Van R, Dekker J. Prevalence and risk factors for recurrence of depression five years after short term psychodynamic therapy. J Affect Disord. 2011; 134(1-3): 468-72. [ Links ]
33. Luijendijk HJ, van den Berg JF, Dekker MJ, van Tuijl HR, Otte W, Smit F, et al. Incidence and recurrence of late-life depression. Arch Gen Psychiatry. 2008; 65(12): 1394-401. [ Links ]
34. Kessing LV. Severity of depressive episodes according to ICD-10: prediction of risk of relapse and suicide. Br J Psychiatry. 2004; 184: 53-6. [ Links ]
35. Skodol AE, Grilo CM, Keyes KM, Geier T, Grant BF, Hasin DS. Relationship of personality disorders to the course of major depressive disorder in a nationally representative sample. Am J Psychiatry. 2011; 168(3): 257-64. [ Links ]
36. Monroe SM, Harkness KL. Recurrence in major depression: a conceptual analysis. Psychol Rev. 2011; 118(4): 655-74. [ Links ]
37. Hankin BL, Abramson LY, Moffitt TE, Silva PA, McGee R, Angell KE. Development of depression from preadolescence to young adulthood: emerging gender differences in a 10-year longitudinal study. J Abnorm Psychol. 1998; 107(1): 128-40. [ Links ]
38. Tsuru J, Ishitobi Y, Ninomiya T, Kanehisa M, Imanaga J, Inoue A, et al. The thyrotropin-releasing hormone test may predict recurrence of clinical depression within ten years after discharge. Neuro Endocrinol Lett. 2013; 34(5): 409-17. [ Links ]
39. Fava GA, Grandi S, Zielezny M, Rafanelli C, Canestrari R. Four-year outcome for cognitive behavioral treatment of residual symptoms in major depression. Am J Psychiatry. 1996; 153(7): 945-7. [ Links ]
40. Franchini L, Gasperini M, Perez J, Smeraldi E, Zanardi R. Dose-response efficacy of paroxetine in preventing depressive recurrences: a randomized, double-blind study. J Clin Psychiatry. 1998; 59(5): 229-32. [ Links ]
41. Franchini L, Zanardi R, Gasperini M, Smeraldi E. Two-year maintenance treatment with citalopram, 20 mg, in unipolar subjects with high recurrence rate. J Clin Psychiatry. 1999; 60(12): 861-5. [ Links ]
42. Geerts E, van Os T, Ormel J, Bouhuys N. Nonverbal behavioral similarity between patients with depression in remission and interviewers in relation to satisfaction and recurrence of depression. Depress Anxiety. 2006; 23(4): 200-9. [ Links ]
43. Oquendo MA, Barrera A, Ellis SP, Li S, Burke AK, Grunebaum M, et al. Instability of symptoms in recurrent major depression: a prospective study. Am J Psychiatry. 2004; 161(2): 255-61. [ Links ]
44. Pintor L, Torres X, Navarro V, Martinez de Osaba MA, Matrai S, Gastó C. Prediction of relapse in melancholic depressive patients in a 2-year follow-up study with corticotropin releasing factor test. Prog Neuropsychopharmacol Biol Psychiatry. 2009; 33(3): 463-9. [ Links ]
45. Warner V, Weissman MM, Fendrich M, Wickramaratne P, Moreau D. The course of major depression in the offspring of depressed parents. Incidence, recurrence, and recovery. Arch Gen Psychiatry. 1992; 49(10): 795-801. [ Links ]
46. Appelhof BC, Huyser J, Verweij M, Brouwer JP, van Dyck R, Fliers E, et al. Glucocorticoids and relapse of major depression (dexamethasone/corticotropin-releasing hormone test in relation to relapse of major depression). Biol Psychiatry. 2006; 59(8): 696-701. [ Links ]
47. Mongrain M, Leather F. Immature dependence and self-criticism predict the recurrence of major depression. J Clin Psychol. 2006; 62(6): 705-13. [ Links ]
48. Bertschy G, Haffen E, Gervasoni N, Gex-Fabry M, Osiek C, Marra D, et al. Self-rated residual symptoms do not predict 1-year recurrence of depression. Eur Psychiatry. 2010; 25(1): 52-7. [ Links ]
49. Schmid M, Hammar A. A follow-up study of first episode major depressive disorder. Impairment in inhibition and semantic fluency-potential predictors for relapse? Front Psychol. 2013; 4: 633. [ Links ]
50. Segal ZV, Shaw BF, Vella DD, Katz R. Cognitive and life stress predictors of relapse in remitted unipolar depressed patients: test of the congruency hypothesis. J Abnorm Psychol. 1992; 101(1): 26-36. [ Links ]
51. Thase ME, Simons AD, McGeary J, Cahalane JF, Hughes C, Harden T, et al. Relapse after cognitive behavior therapy of depression: potential implications for longer courses of treatment. Am J Psychiatry. 1992; 149(8): 1046-52. [ Links ]
52. Ramana R, Paykel ES, Cooper Z, Hayhurst H, Saxty M, Surtees PG. Remission and relapse in major depression: a two-year prospective follow-up study. Psychol Med. 1995; 25(6): 1161-70. [ Links ]
53. Vaughn CE, Leff JP. The influence of family and social factors on the course of psychiatric illness. A comparison of schizophrenic and depressed neurotic patients. Br J Psychiatry. 1976; 129: 125-37. [ Links ]
54. Meyer J, Wilson A, Sagrati S, Miler L, Rusjan P, Bloomfield P, et al. Brain monoamine oxidase A binding in major depressive disorder: relationship to selective serotonin reuptake inhibitor treatment, recovery, and recurrence. Arch Gen Psychiatry. 2009; 66(12): 1304-12. [ Links ]
55. Owashi T, Otsubo T, Oshima A, Nakagome K, Higuchi T, Kamijima K. Relationships of DEX/CRH and GHRH test results to the outcome of depression-preliminary results suggest the GHRH test may predict relapse after discharge. J Psychiatr Res. 2008; 42(5): 356-64. [ Links ]
56. Zobel AW, Nickel T, Sonntag A, Uhr M, Holsboer F, Ising M. Cortisol response in the combined dexamethasone/CRH test as predictor of relapse in patients with remitted depression: a prospective study. J Psychiatr Res. 2001; 35: 83-94. [ Links ]
57. Wainwright NW, Surtees PG. Childhood adversity, gender and depression over the life-course. J Affect Disord. 2002; 72(1): 33-44. [ Links ]
58. Angst J, Gamma A, Sellaro R, Lavori PW, Zhang H. Recurrence of bipolar disorders and major depression. A life-long perspective. Eur Arch Psychiatry Clin Neurosci. 2003; 253(5): 236-40. [ Links ]
59. Mattisson C, Bogren M, Horstmann V, Munk-Jorgensen P, Nettelbladt P. The long-term course of depressive disorders in the Lundby Study. Psychol Med. 2007; 37(6): 883-91. [ Links ]
60. Riise T, Lund A. Prognostic factors in major depression: a long-term follow-up study of 323 patients. J Affect Disord. 2001; 65(3): 297-306. [ Links ]
61. Mueller TI, Leon AC, Keller MB, Solomon DA, Endicott J, Coryell W, et al. Recurrence after recovery from major depressive disorder during 15 years of observational follow-up. Am J Psychiatry. 1999; 156(7): 1000-6. [ Links ]
62. Eaton WW, Anthony JC, Gallo J, Cai G, Tien A, Romanoski A, et al. Natural history of Diagnostic Interview Schedule/DSM-IV major depression. The Baltimore Epidemiologic Catchment Area follow-up. Arch Gen Psychiatry. 1997; 54(11): 993-9. [ Links ]
63. Pettit JW, Hartley C, Lewinsohn PM, Seeley JR, Klein DN. Is liability to recurrent major depressive disorder present before first episode onset in adolescence or acquired after the initial episode? J Abnorm Psychol. 2013; 122(2): 353-8. [ Links ]
64. Joffe RT, Marriott M. Thyroid hormone levels and recurrence of major depression. Am J Psychiatry. 2000; 157(10): 1689-91. [ Links ]
65. Colman I, Naicker K, Zeng Y, Ataullahjan A, Senthilselvan A, Patten SB. Predictors of long-term prognosis of depression. CMAJ. 2011; 183(17): 1969-76. [ Links ]
66. Coryell W, Endicott J, Keller MB. Predictors of relapse into major depressive disorder in a nonclinical population. Am J Psychiatry. 1991; 148(10): 1353-8. [ Links ]
67. Kovacs M. Gender and the course of major depressive disorder through adolescence in clinically referred youngsters. J Am Acad Child Adolesc Psychiatry. 2001; 40(9): 1079-85. [ Links ]
68. Melvin GA, Dudley AL, Gordon MS, Ford S, Taffe J, Tonge BJ. What happens to depressed adolescents? A follow-up study into early adulthood. J Affect Disord. 2013; 151(1): 298-305. [ Links ]
69. Bockting CL, Spinhoven P, Koeter MW, Wouters LF, Schene AH. Prediction of recurrence in recurrent depression and the influence of consecutive episodes on vulnerability for depression: a 2-year prospective study. J Clin Psychiatry. 2006; 67(5): 747-55. [ Links ]
70. Holma KM, Holma IA, Melartin TK, Rytsala HJ, Isometsa ET. Long-term outcome of major depressive disorder in psychiatric patients is variable. J Clin Psychiatry. 2008; 69(2): 196-205. [ Links ]
71. Keitner GI, Ryan CE, Miller IW, Zlotnick C. Psychosocial factors and the long-term course of major depression. J Affect Disord. 1997; 44(1): 57-67. [ Links ]
72. Van Londen L, Molenaar RP, Goekoop JG, Zwinderman AH, Rooijmans HG. Three- to 5-year prospective follow-up of outcome in major depression. Psychol Med. 1998; 28(3): 731-5. [ Links ]
73. Hoencamp E, Haffmans PM, Griens AM, Huijbrechts IP, Heycop ten Ham BF. A 3.5-year naturalistic follow-up study of depressed out-patients. J Affect Disord. 2001; 66(2-3): 267-71. [ Links ]
74. Wang JL, Patten S, Sareen J, Bolton J, Schmitz N, MacQueen G. Development and validation of a prediction algorithm for use by health professionals in prediction of recurrence of major depression. Depress Anxiety. 2014; 31(5): 451-7. [ Links ]
75. Cho HJ, Lavretsky H, Olmstead R, Levin MJ, Oxman MN, Irwin MR. Sleep disturbance and depression recurrence in community-dwelling older adults: a prospective study. Am J Psychiatry. 2008; 165(12): 1543-50. [ Links ]
76. Kornstein SG, Pedersen RD, Holland PJ, Nemeroff CB, Rothschild AJ, Thase ME, et al. Influence of sex and menopausal status on response, remission, and recurrence in patients with recurrent major depressive disorder treated with venlafaxine extended release or fluoxetine: analysis of data from the PREVENT study. J Clin Psychiatry. 2014; 75(1): 62-8. [ Links ]
77. Gonzales LR, Lewinsohn PM, Clarke GN. Longitudinal follow-up of unipolar depressives: an investigation of predictors of relapse. J Consult Clin Psychol. 1985; 53(4): 461-9. [ Links ]
78. Berlanga C, Heinze G, Torres M, Apiquian R, Caballero A. Personality and clinical predictors of recurrence of depression. Psychiatr Serv. 1999; 50(3): 376-80. [ Links ]
79. Bulloch A, Williams J, Lavorato D, Patten S. Recurrence of major depressive episodes is strongly dependent on the number of previous episodes. Depress Anxiety. 2014; 31(1): 72-6. [ Links ]
80. Kessler RC, McGonagle KA, Swartz M, Blazer DG, Nelson CB. Sex and depression in the National Comorbidity Survey. I: Lifetime prevalence, chronicity and recurrence. J Affect Disord. 1993; 29(2-3): 85-96. [ Links ]
81. De Marco RR. The epidemiology of major depression: implications of occurrence, recurrence, and stress in a Canadian community sample. Can J Psychiatry. 2000; 45(1): 67-74. [ Links ]
82. Gopinath S, Katon WJ, Russo JE, Ludman EJ. Clinical factors associated with relapse in primary care patients with chronic or recurrent depression. J Affect Disord. 2007; 101(1-3): 57-63. [ Links ]
83. Katon WJ, Fan MY, Lin EH, Unutzer J. Depressive symptom deterioration in a large primary care-based elderly cohort. Am J Geriatr Psychiatry. 2006; 14(3): 246-54. [ Links ]
84. Lee E, Cho HJ, Olmstead R, Levin MJ, Oxman MN, Irwin MR. Persistent sleep disturbance: a risk factor for recurrent depression in community-dwelling older adults. Sleep. 2013; 36(11): 1685-91. [ Links ]
85. Wardenaar KJ, Conradi HJ, de Jonge P. Data-driven course trajectories in primary care patients with major depressive disorder. Depress Anxiety. 2014; 31(9): 778-86. [ Links ]
86. Suija K, Aluoja A, Kalda R, Maaroos HI. Factors associated with recurrent depression: a prospective study in family practice. Fam Pract. 2011; 28(1): 22-8. [ Links ]
87. Kuehner C. Gender differences in the short-term course of unipolar depression in a follow-up sample of depressed inpatients. J Affect Disord. 1999; 56(2-3): 127-39. [ Links ]
88. Cuijpers P, Weitz E, Twisk J, Kuehner C, Cristea I, David D, et al. Gender as predictor and moderator of outcome in cognitive behavior therapy and pharmacotherapy for adult depression: an "individual patient data" meta-analysis. Depress Anxiety. 2014; 31(11): 941-51. [ Links ]
89. O'Leary D, Hickey T, Lagendijk M, Webb M. Onset of remission and relapse in depression: Testing operational criteria through course description in a second Dublin cohort of first-admission participants. Journal of Affective Disorders. 2010; 125(1-3): 221-6. [ Links ]
90. Rucci P, Frank E, Calugi S, Miniati M, Benvenuti A, Wallace M, et al. Incidence and predictors of relapse during continuation treatment of major depression with SSRI, interpersonal psychotherapy, or their combination. Depress Anxiety. 2011; 28(11): 955-62. [ Links ]
91. Kennedy N, Abbott R, Paykel ES. Remission and recurrence of depression in the maintenance era: long-term outcome in a Cambridge cohort. Psychol Med. 2003; 33(5): 827-38. [ Links ]
92. Grilo CM, Stout RL, Markowitz JC, Sanislow CA, Ansell EB, Skodol AE, et al. Personality disorders predict relapse after remission from an episode of major depressive disorder: a 6-year prospective study. J Clin Psychiatry. 2010; 71(12): 1629-35. [ Links ]
93. Kanai T, Takeuchi H, Furukawa TA, Yoshimura R, Imaizumi T, Kitamura T, et al. Time to recurrence after recovery from major depressive episodes and its predictors. Psychol Med. 2003; 33(5): 839-45. [ Links ]
94. Kuehner C, Huffziger S. Factors predicting the long-term illness course in a cohort of depressed inpatients. Eur Arch Psychiatry Clin Neurosci. 2013; 263(5): 413-23. [ Links ]
95. Hardeveld F, Spijker J, De Graaf R, Nolen WA, Beekman AT. Recurrence of major depressive disorder and its predictors in the general population: results from The Netherlands Mental Health Survey and Incidence Study (NEMESIS). Psychol Med. 2013; 43(1): 39-48. [ Links ]
96. Seemüller F, Meier S, Obermeier M, Musil R, Bauer M, Adli M, et al. Three-Year long-term outcome of 458 naturalistically treated inpatients with major depressive episode: severe relapse rates and risk factors. Eur Arch Psychiatry Clin Neurosci. 2014; 264(7): 567-75. [ Links ]
97. Bos EH, Bouhuys AL, Geerts E, Van Os TW, Van der Spoel ID, Brouwer WH, et al. Cognitive, physiological, and personality correlates of recurrence of depression. J Affect Disord. 2005; 87(2-3): 221-9. [ Links ]
98. Flint AJ, Rifat SL. Recurrence of first-episode geriatric depression after discontinuation of maintenance antidepressants. Am J Psychiatry. 1999; 156(6): 943-5. [ Links ]
99. Hardeveld F, Spijker J, De Graaf R, Hendriks SM, Licht CM, Nolen WA, et al. Recurrence of major depressive disorder across different treatment settings: Results from the NESDA study. J Affect Disord. 2013; 147(1-3): 225-31. [ Links ]
100. Martínez-Amorós E, Cardoner N, Soria V, Gálvez V, Menchón JM, Urretavizcaya M. Long-term treatment strategies in major depression: a 2-year prospective naturalistic follow-up after successful electroconvulsive therapy. J ECT. 2012; 28(2): 92-7. [ Links ]
101. Naz B, Craig TJ, Bromet EJ, Finch SJ, Fochtmann LJ, Carlson GA. Remission and relapse after the first hospital admission in psychotic depression: a 4-year naturalistic follow-up. Psychol Med. 2007; 37(8): 1173-81. [ Links ]
102. Frank E, Kupfer DJ, Perel JM. Early recurrence in unipolar depression. Arch Gen Psychiatry. 1989; 46(5): 397-400. [ Links ]
103. Beevers CG, Keitner GI, Ryan CE, Miller IW. Cognitive predictors of symptom return following depression treatment. J Abnorm Psychol. 2003; 112(3): 488-96. [ Links ]
104. Harkness KL, Theriault JE, Stewart JG, Bagby RM. Acute and chronic stress exposure predicts 1-year recurrence in adult outpatients with residual depression symptoms following response to treatment. Depress Anxiety. 2014; 31(1): 1-8. [ Links ]
105. Jang KL, Lam RW, Livesley WJ, Vernon PA. The relationship between seasonal mood change and personality: more apparent than real? Acta Psychiatr Scand. 1997; 95(6): 539-43. [ Links ]
106. Nordenskjöld A, von Knorring L, Engström I. Predictors of time to relapse/recurrence after electroconvulsive therapy in patients with major depressive disorder: a population-based cohort study. Depress Res Treat. 2011; 2011: 470985. [ Links ]
107. Cohen RB, Boggio PS, Fregni F. Risk factors for relapse after remission with repetitive transcranial magnetic stimulation for the treatment of depression. Depress Anxiety. 2009; 26(7): 682-8. [ Links ]
108. Lara ME, Klein DN, Kasch KL. Psychosocial predictors of the short-term course and outcome of major depression: a longitudinal study of a nonclinical sample with recent-onset episodes. J Abnorm Psychol. 2000; 109(4): 644-50. [ Links ]
![]() Correspondence:
Correspondence:
Gilles Bertschy
Département de psychiatrie et santé mentale
Hôpitaux Universitaires de Strasbourg
1 place de l'Hôpital, 67091 Strasbourg, France
Tel: + 33 388 11 65 48
E-mail: gilles.bertschy@chru-strasbourg.fr
Received: 4 July 2015
Revised: 20 November 2015
Accepted: 10 December 2015