Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
The European Journal of Psychiatry
versión impresa ISSN 0213-6163
Eur. J. Psychiat. vol.30 no.3 Zaragoza jul./sep. 2016
Prevalence of psychotropic medication use and associated factors in the elderly
Juan Téllez-Lapeiraa; Jesús López-Torres Hidalgob; Nuria García-Agua Solerc; Luis Gálvez-Alcarazd; Francisco Escobar-Rabadánb y Antonio García-Ruizc
a Albacete Area VB Health Centre. Health Care Service of Castilla-La Mancha. Albacete Spain
b Albacete Area IV Health Centre. Health Care Service of Castilla-La Mancha. Albacete Spain
c Department of Pharmacology. Faculty of Medicine. University of Málaga. Málaga Spain
d Málaga El Palo Health Center. Health Care Service of Andalucia. Málaga Spain
This study was financed by the Instituto de Salud Carlos III (Biomedical and Health Science Research Promotion Programme, Ministry of Health and Consumer Affairs (Dossier P1031562) and the Health Ministry of the Castilla-La Mancha Autonomous Community (Directive 50903).
Part of the study was presented as scientific poster at the 19th WONCA Europe Conference, held at the Lisbon Congress Center, July 2-5, 2014.
ABSTRACT
Background and Objectives: The object of our study was to estimate the prevalence of psychotropic drug use among non-institutionalised elderly people 65 years or older and identify possible conditioning factors.
Methods: A cross-sectional, observational study was carried out of 1161 subjects aged 65 years and older. Participants were randomly selected from health care registry listings. The main outcomes of interest were based on self-reporting and included consumption of psychotropic and other drugs (filed by the ATC Classification System), mood (based on the GDS-VE), cognitive status (Pfeiffer Questionnaire), physical-functional assessment based on Katz score, health problems (ICPC-2 classification WONCA) and socio-demographic variables.
Results: The prevalence of self-reported psychotropic drug consumption was 20.5% (95% CI: 18.2 to 22.8). Anxiolytics and hypnotics were consumed by 16.6% of the elderly, antidepressants by 7.0% and antipsychotics by only 2.1%. In multivariate logistical analyses, the use of psychotropics was independently associated with other drug consumption (non-psychotropics), (OR: 4.0, 95% CI: 1.7 to 9.5), presence of established depression (OR: 3.2, 95% CI: 1.3 to 7.6), presence of 4 or more comorbidities (OR: 2.7, 95% CI: 1.9 to 3.8), being female (OR: 2.1, 95% CI: 1.5 to 3.0) and being dependent for basic activities of daily living (OR: 1.7, 95% CI: 1.0 to 2.6).
Conclusions: The prevalence of psychotropic drug use among the elderly from Albacete is high. Several factors were identified as potential determinants of psychotropic drug use. It will be important to evaluate the misuse of these drugs in order to inform effective, efficient and safe prescription strategies.
Keywords: Drug use; Elderly; Epidemiological factors; Prevalence; Psychotropic drugs.
Introduction
In Spain, the elderly account for 70% of pharmaceutical spending even though they represent slightly less than one-fourth of the population1. In this context, over the last 20 years there has been an important increase in the psychotropic drugs prescribed to adults, and particularly the elderly. The prevalence of psychotropic drugs use in community-dwelling elderly (generally defined as people 65 years or older) varies from 10% to 40%2-7. This variability is determined, among other factors, by methodological differences in the studies, whether data are obtained from surveys, population studies or from people attended in Primary Care centers.
The importance of the use of medications in general and psychotropic drugs in particular among the elderly is associated with the consequences. Aging increases the probability of drug build-up and intoxication which means that the elderly are particularly vulnerable to the effects of these drugs. These effects include cognitive impairment, sedation, confusional syndrome, falls and increased risk of fractures, which are frequent reasons for hospitalization6,8-10.
While mental health problems are likely a factor in the use of these drugs, they may not be the only factor or even the decisive one, which means that there are other predisposing factors that must also be considered3,6. Some of the specific factors involved, although they have not been sufficiently analysed, include: physiological alterations of sleep patterns, demographic and socio-economic factors, the functional situation of the elderly person, the presence and simultaneity of chronic diseases, anxiety and depressionas well as other factors associated with the prescribers, all of which appear to have converted the elderly into a risk group for the misuse of these drugs2,6. In a study based on the National Health Survey on Spanish population non-institutionalized, the authors observed a higher consumption of psychotropic drugs in women over 65 years (26.4%) than in men (10.6%)11. Another study carried outin US community populationwith a similar methodology, identified as predictors of the use of psychotropic medication, in addition to the gender, race, regional differences and the educational level3. The limitations in the functional abilities of non-institutionalized elderly have been linked to the use of sedatives, hypnotics and antianxiety drugs. It has also been associated dependency for mobility and the difficulties to perform instrumental activities with the use of antipsychotics12-14. The characteristics of prescribers such as medical specialty, number of years of practice, number of visits and type of consultations, or the number of prescribers also seem to influence the inappropriate use of these drugs1,15-17.
If we want to minimise the problems caused by the misuse of these kinds of drugs and improve the quality of care provided to the elderly, it is essential to have a real understanding of how these drugs are used among the elderly population. In this regard, the goal of our study was to estimate the prevalence of psychotropic drug use in non-institutionalised persons aged 65 or older and to evaluate, in relation to the use of such drugs, the possible conditioning factors in terms of morbidity, physical function, emotional and cognitive status and socio-demographic characteristics.
Methods
Study design
This is a community-level transversal observational study conducted in the city of Albacete (south-eastern Spain) that has 8 basic health zones and a total population of 165,664.
Participants
The sample was selected from a list of people aged 65 or older residing in the city of Albacete, whose information was on file in the Castilla-La Mancha Health Service database. We use a simple random sampling, to ensure that all the subjects would have the same probability to be part of the sample.
The sample size was 1,387 subjects which correspond to an expected proportion of elderly consumers of psychotropics of 25%, a level of confidence of 95% and a precision rate of ± 2.4%, which was increased by 15% as a means of offsetting the anticipated lack of responses. Subjects who were institutionalised, unable to travel to the interview site or unable to take part in the interview (severe cognitive impairment, sensorial deficit or altered mental state) were excluded.
The information was gathered on a questionnaire designed for the study that was administered in the form of a semi-structured interview in person conducted by previously trained primary care nurses.
Ethical Questions
The study was approved by the Albacete Area's Clinical Research Ethics Committee. The following ethical principles were respected: consent to participate in the study once informed of the purpose and use of the data provided by the participants restricted to the proposed investigation.
Variable Studies. Measurements
The main study variable was the use of psychotropic drugs. Their prevalence among people aged 65 and older was calculated as a percentage of the participants that referred to the use of the psychotropics included in the groups of the Anatomical Therapeutic Chemical Classification System. More specifically, the active ingredients included in the following pharmacological subgroups were defined as psychotropics: antipsychotics (N05A), anxiolytics (N05B), hypnotic-sedatives (N05C), antidepressants (N06A) and psycholeptics and psychoanaleptics in combination (N06C). To correct gaps, limitations and errors in the drug consumption information provided by the subjects, they were asked to show the bottles of the medicines they consumed on a regular basis at the time of the interview.
Other variables that can be factors associated with drug use were also evaluated: socio-demographics (age, gender, marital status, education status, social class); use of other drugs (according to The Anatomical Therapeutic Chemical Classification System); polymedication (5 or more medications); chronic morbidity, arranged according to the International Classification of Primary Care (ICPC-2) of the World Organization of National Colleges, Academies and Academic Associations of General Practitioners/Family; emotional status, measured using the Spanish version of the Yesavage abbreviated Geriatric Depression Scale18; cognitive condition, evaluated using the abbreviated Pfeiffer Questionnaire19; physical-functional status determined using the Katz Index of Independence in Activities of Daily Living20. In all cases, the evaluation instruments were used with versions validated in our environment.
Statistical Analysis
The data were analysed using the SPSS 15.0 statistical program for Windows. First, a descriptive analysis was performed using ratios, measures of central tendency and dispersion measures. The response rate and the prevalence of each of the parameters studied together were calculated, along with the corresponding confidence interval of 95%.
The techniques used to compare observed proportions between two qualitative variables were the chi-square test with Yates correction when necessary, and Fisher's exact test. In the case of a binary variable and one with more than two ordered categories, the Mantel-Haenszel linear trend test was applied. Others like the Student T test or the Mann-Whitney U test were used to measure explanatory variables on the quantitative scale. Analysis of Variance and the "H" Kruskal Wallis test were used to compare means in more than two independent groups. The association between variables was considered significant when p < 0.05.
Finally, multivariate analysis (logistic regression) was used to verify the association of the use of psychotropic medication, and in each subgroup, with their conditioning factors, performing a statistical adjustment and checking for confounding factors and interaction variables. The predictor variables were included with p values < 0.05 and were excluded when p > 0.10. Being a cross-sectional study, the estimated coefficients were interpreted as prevalence odds ratios.
Results
Of 1387 elderly people selected, a total of 1161 subjects were ultimately enrolled in the study, which corresponds to a response rate of 83.7%. The average age of respondents was 73.4 years ± 5.9 SD and a higher proportion of women (55.9%) was observed. Table 1 shows the characteristics of the study participants.
Prevalence of referred use of psychotropics
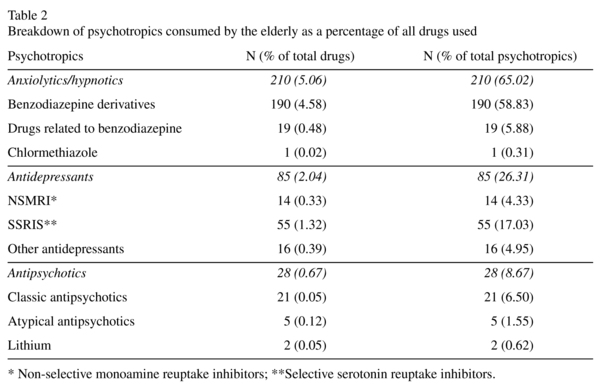
The prevalence of self-reported psychotropic drug consumption (anxiolytics, hypnotics, antidepressants and/or antipsychotics) was 20.5% (95% CI: 18.2 to 22.8). Anxiolytics and hypnotics were the most consumed drug subgroups (16.6% of the elderly), primarily benzodiazepines. Antidepressants were consumed by 7.0%, primarily in the form of SSRIs. Antipsychotics were the least used psychotropics (only 2.1% of the study participants). Moreover, the proportion of therapeutic subgroups of psychotropics consumed by the elderly compared to all drugs used and all psychotropics is shown on Table 2.
Factors associated with the use of psychotropic drugs
The consumption of psychotropic drugs by the elderly subjects in our study was significantly higher in women, widows and divorcees, subjects with established depression, cognitive deterioration and dependence for some basic activities of daily living as observed on Table 3.
The average number of health problems was significantly higher in the elderly who reported consuming psychoactive drugs (2.69 ± 2.08 DE versus 1.69 ± 1.68 DE health problems in nonusers) (p <0.001). In addition, we observed a statistically significant linear trend among this number and proportion of subjects who were consumers (p <0.001) (Figure 1).
Multivariate Analysis
A logistic regression model was constructed to determine the variables related to the consumption of psychotropic drugs, the dependent variable being the consumption of psychotropic drugs.
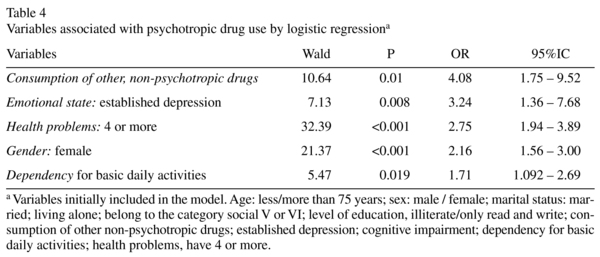
We noted that the variables associated independently as the most important predictors were consumption of other non-psychotropic drugs and established depression. Having four or more health problems, being a woman and/or being dependent for basic activities of daily living also appear to be related to the use of psychotropic drugs, but to a lesser extent (Table 4).
Discussion
Prevalence of psychotropic drug use in non-institutionalised elderly
The prevalence of psychotropic drug consumption by the elderly participants in our study was 20.5%. This result is consistent with findings from studies published in our area. In the Spanish National Health Survey, the prevalence of psychotropic drug consumption (anxiolytics, hypnotics and antidepressants) in people over the age of 65 residing in the community was 4.6% in 1993 and ten years later, in 2003, it was 20.5%, identical to the results of our study11. Likewise, the ESEMeD study (a Europe-wide study conducted by home interview) points to a consumption rate of psychotropic drugs by this age group in our country of 25.9%21.
International research of non-institutionalised elderly populations published in the last decade show a clear trend toward high consumption rates that are higher than those obtained in our study. Consumption rates were 35%, 37% and 38%, respectively, among subjects in New Zealand22, France23 and Finland24,25, although in this case the subjects were over the age of 75. The variability in the prevalence of psychotropic drug use reflected in the studies may be due to significant methodological differences3,26,27.
The use of psychotropic drugs reported by non-institutionalised elderly refers primarily to anxiolytics and hypnotics, followed by antidepressants and, to a much lesser extent, antipsychotics7,25,28-30. However, the prevalence of anxiety disorders among the elderly is relatively low31, which suggests that excessive use may also be due to inappropriate use2,30,32.
Factors associated with psychotropic drug use
In our study, taking other medication was an independent variable associated with the overall use of psychotropic drugs. It is known that the use of psychotropics in the elderly, especially benzodiazepines, has been associated with the presence of psychological alterations, but also with comorbidity, negative perception of health condition, complaints and symptoms without clearly defined diagnoses and more frequent doctor visits, all leading to increased drug use24,33,34.
The mood (established depression) resulted in our study, as it was predictable, a variable associated independently to the use of psychoactive drugs (OR 3.24, 95% CI: 1.36 to 7.68), especially antidepressants (OR 5.69, 95% CI: 2.28 to 14.18) but also to the consumption of anxiolytic and hypnotic drugs (OR 2.53; 96% CI: 1.07 to 5.95). Therefore, we observe a significant use of benzodiazepines in subjects with established depression, as other authors have pointed out. Several studies have highlighted the frequent use of benzodiazepines in these patients12,23,30,35, which may raise doubts about the proper use of anxiolytics and the need to tackle depression in the elderly population. However, depression in older people often manifests in atypical ways, with symptoms of anxiety and insomnia that may explain the tendency of internists and family physicians to start the elderly patient on benzodiazepines.
Our results show higher consumption rates of psychotropic drugs associated with an increased number of health problems in the elderly. Some authors suggest that comorbidity is a stressful event in the elderly that can affect mental health and create a perceived need on the part of the patient or the clinician for the use of psychotropics36.
Our data show a significant relationship between the consumption of psychotropic drugs and female sex. Although there are several hypotheses about possible causes of this relationship, we have not found studies that allow us to explain it consistently. Some research have suggested that women present higher prevalence of mental disorders or they are more prone to reveal their emotional problems to their doctor, to request prescriptions explicitly or to hold more positive views of psychotropic drugs3,6,37-39. Also, women visit physicians more often, increasing their chance of receiving a prescription39 and physicians might be more willing to prescribe a psychotropic drug to a woman rather than to a man (prescription bias described in the literature)3,38,39. It is possible that, when these differences in health status between older men and women are not controlled, the relationship between gender and use of psychoactive drugs is more likely obtained40,41. However, other studies, such as ours, adjusting for the presence of chronic comorbidity, functional physical, mental or cognitive status and other factors such as medical visits, still detect an independent association of the female gender with the consumption of psychotropic drugs39,42,43.This relationship persists when the statistical adjustment also includes the mental health status44."
Reliance on others to perform basic activities of daily living was associated with the overall use of psychotropic drugs. Although this relationship is independent, it may be influenced by other factors such as physical and mental comorbidity and poor self-perception of health3,6,23,45.
The results of our study refer to the non-institutionalised elderly population. People aged 65 or older who live in nursing homes are the minority but their physical and mental deterioration is much more exacerbated than that of the elderly who live in the community. If the institutionalised population were considered, the results of the prevalence of drug use, especially psychotropics, would be higher all around.
In conclusion, our findings show a high prevalence of psychotropic drug use in the elderly population residing in the community, particularly if we consider the vulnerability of this population group to the significant adverse effects of these drugs. Different factors appear to be associated with a greater or lesser prevalence of this excessive and probably inadequate drug use among the non-institutionalised elderly population. In this sense, we need a better understanding of the determining factors for the use of these drugs and evaluate effective and efficient strategies to enhance the safety of this population.
Competing interests
The authors declare no conflict of interest.
References
1. Blasco Patiño F, Martínez López J, Villares P, Jiménez AI. El paciente anciano polimedicado: efectos sobre su salud y sobre el sistema sanitario. Inf Ter Sist Nac Salud. 2005, 29(6): 152-162. [ Links ]
2. Linjakumpu T, Hartikainen S, Klaukka T, Koponen H, Kivelä SL, Isoaho R. Psychotropics among the home-dwelling elderly-increasing trends. Int J Geriatr Psychiatry. 2002; 17(9): 874-83. [ Links ]
3. Aparasu RR, Mort JR, Brandt H. Psychotropic prescription use by community-dwelling elderly in the United States. J Am Geriatr Soc. 2003; 51(5): 671-7. [ Links ]
4. Gili M, García Campayo J, Roca M. Crisis económica y salud mental. Informe SESPAS 2014. Gac Sanit. 2014, 28(S1): 104-108. [ Links ]
5. Carrasco P, Astasio P, Ortega P, Jiménez R, Gil A. Factores asociados al consumo de fármacos psicotropos en la población adulta española. Datos obtenidos a partir de las Encuestas Nacionales de Salud de España de los años 1993, 1995 y 1997. Med Clin (Barc). 2001, 116(9): 324-329. [ Links ]
6. Voyer P, Cohen D, Lauzon S, Collin J. Factors associated with psychotropic drug use among community-dwelling older persons: A review of empirical studies. BMC Nurs. 2004; 3(1): 3. [ Links ]
7. Carrasco-Garrido P, López de Andrés A, Hernández Barrera V, Jiménez-Trujillo I, Jiménez-García R. National trends (2003-2009) and factors related to psychotropic medication use in community-dwelling elderly population. Int Psychogeriatr. 2013; 25(2): 328-38. [ Links ]
8. Higashi T, Shekelle PG, Solomon DH, Knight EL, Roth C, Chang JT, et al. The quality of pharmacological care for vulnerable older patients. Ann Intern Med. 2004, 140: 714-20. [ Links ]
9. Bloch F, Thibaud M, Dugué B, Brèque C, Rigaud AS, Kemoun G. Psychotropic drugs and falls in the elderly people: updated literature review and meta-analysis. J Aging Health. 2011; 23(2): 329-46. [ Links ]
10. Montastruc F, Sommet A, Bondon-Guitton E, Durrieu G, Bui E, Bagheri H, et al. The importance of drug-drug interactions as a cause of adverse drug reactions: a pharmacovigilance study of serotoninergic reuptake inhibitors in France. Eur J Clin Pharmacol. 2012; 68(5): 767-75. [ Links ]
11. Carrasco-Garrido P, Jiménez-García R, Astasio-Arbiza P, Ortega-Molina P, de Miguel AG. Psychotropics use in the Spanish elderly: predictors and evolution between years 1993 and 2003. Pharmacoepidemiol Drug Saf. 2007; 16(4): 449-57. [ Links ]
12. Blazer D, Hybels C, Simonsick E, Hanlon JT. Sedative, hypnotic, and antianxiety medication use in an aging cohort over ten years: a racial comparison. J Am Geriatr Soc. 2000; 48(9): 1073-9. [ Links ]
13. Gray SL, LaCroix AZ, Blough D, Wagner EH, Koepsell TD, Buchner D. Is the use of benzodiazepines associated with incident disability? J Am Geriatr Soc. 2002; 50(6): 1012-8. [ Links ]
14. Ahto M, Isoaho R, Puolijoki H, Laippala P, Romo M, Kivelä SL. Functional abilities of elderly coronary heart disease patients. Aging (Milano). 1998; 10(2): 127-36. [ Links ]
15. Linden M, Lecrubier Y, Bellantuono C, Benkert O, Kisely S, Simon G. The prescribing of psychotropic drugs by primary care physicians: an international collaborative study. J Clin Psychopharmacol. 1999; 19(2): 132-40. [ Links ]
16. Kjosavik SR, Hunskaar S, Aarsland D, Ruths S. Initial prescription of antipsychotics and antidepressants in general practice and specialist care in Norway. Acta Psychiatr Scand. 2011; 123(6): 459-65. [ Links ]
17. Mercier A, Benichou J, Auger-Aubin I, Lebeau JP, Houivet E, Van Royen P, et al. How do GP practices and patient characteristics influence the prescription of antidepressants? A cross-sectional study. Ann Gen Psychiatry. 2015; 14(1): 3. [ Links ]
18. Martínez-Iglesia J, Onís MC, Dueñas R, Albert C, Aguado C, Luque R. Versión española del cuestionario de Yesavage abreviado (GDS) para el despistaje de depresión en mayores de 65 años: adaptación y validación. Medifam. 2002, 12(10): 620-30. [ Links ]
19. Martínez-Iglesia J, Dueñas R, Onis MC, Aguado C, Albert C, Luque R. Adaptación y validación al castellano del cuestionario Pfeiffer (SPMSQ) para detectar la existencia de deterioro cognitivo en personas mayores de 65 años. Med Clin (Barc). 2001, 117: 129-34. [ Links ]
20. Álvarez M, Alaiz AT, Brun E, Cabañeros JJ, Calzón M. Capacidad funcional de pacientes mayores de 65 años, según el índice de Katz. Fiabilidad del método. Aten Primaria. 1992, 10: 812-5. [ Links ]
21. Codony M, Alonso J, Almansa J, Vilagut G, Domingo A, Pinto-Meza A, et al. Psychotropic medications use in Spain. Results of the ESEMeD-Spain study. Actas Esp Psiquiatr. 2007 Sep; 35 Suppl 2: 29-36. [ Links ]
22. Norris P, Horsburgh S, Lovelock K, Becket G, Keown S, Arroll B, et al. Medicalisation or under-treatment? Psychotropic medicines use by elderly people in New Zealand. Health Sociol. Rev 2011, 20(2): 202-218. [ Links ]
23. Fourrier A, Letenneur L, Dartigues JF, Moore N, Bégaud B. Benzodiazepine use in an elderly community-dwelling population. Characteristics of users and factors associated with subsequent use. Eur J Clin Pharmacol. 2001; 57(5): 419-25. [ Links ]
24. Hartikainen S, Rahkonen T, Kautiainen H, Sulkava R. Kuopio 75+ study: does advanced age predict more common use of psychotropics among the elderly? Int Clin Psychopharmacol. 2003; 18(3): 163-7. [ Links ]
25. Desplenter F, Caenen C, Meelberghs J, Hartikainen S, Sulkava R, Bell JS.Change in psychotropic drug use among community-dwelling people aged 75 years and older in Finland: repeated cross-sectional population studies. Int Psychogeriatr. 2011; 23(8): 1278-84. [ Links ]
26. Nielsen MW, Hansen EH, Rasmussen NK. Patterns of psychotropic medicine use and related diseases across educational groups: national cross sectional survey. Eur J Clin Pharmacol. 2004; 60(3): 199-204. [ Links ]
27. Schäfers A, Martini N, Moyes S, Hayman K, Zolezzi M, McLean C, Kerse N. Medication use in community-dwelling older people: pharmacoepidemiology of psychotropic utilisation. J Prim Health Care. 2014; 6(4): 269-78. [ Links ]
28. Lasserre A, Younès N, Blanchon T, Cantegreil-Kallen I, Passerieux C, Thomas G, et al. Psychotropic drug use among older people in general practice: discrepancies between opinion and practice. Br J Gen Pract. 2010; 60(573): e156-62. [ Links ]
29. Martinsson G, Fagerberg I, Wiklund-Gustin L, Lindholm C. Specialist prescribing of psychotropic drugs to older persons in Sweden-a register-based study of 188,024 older persons. BMC Psychiatry. 2012; 12: 197. [ Links ]
30. Blumstein T, Benyamini Y, Chetrit A, Mizrahi EH, Lerner-Geva L. Prevalence and correlates of psychotropic medication use among older adults in Israel: cross-sectional and longitudinal findings from two cohorts a decade apart. Aging Ment Health. 2012; 16(5): 636-47. [ Links ]
31. Saz P, Copeland JR, de la Cámara C, Lobo A, Dewey ME. Cross-national comparison of prevalence of symptoms of neurotic disorders in older people in two community samples. Acta Psychiatr Scand. 1995; 91(1): 18-22. [ Links ]
32. Demyttenaere K, Bonnewyn A, Bruffaerts R, De Girolamo G, Gasquet I, Kovess V, et al. J. Clinical factors influencing the prescription of antidepressants and benzodiazepines: results from the European study of the epidemiology of mental disorders (ESEMeD). J Affect Disord. 2008; 110(1-2): 84-93. [ Links ]
33. Veehof LJG, Jong MB, Haaijer-Ruskamp FM. Polypharmacy in the elderly: a literature review. Eur J Gen Pract. 2000, 6: 98-106. [ Links ]
34. Lechevallier-Michel N, Berr C, Fourrier-Réglat A. Incidence and characteristics of benzodiazepine use in an elderly cohort: the EVA study. Therapie. 2005; 60(6): 561-6. [ Links ]
35. Dealberto MJ, Mcavay GJ, Seeman T, Berkman L. Psychotropic drug use and cognitive decline among older men and women. Int J Geriatr Psychiatry. 1997; 12(5): 567-74. [ Links ]
36. Gustafsson TM, Isacson DGL, Thorslund M, Sörbom D. Factors associated with psychotropic drug use among the elderly living at home. J Appl Gerontol. 1996, 15: 238-54. [ Links ]
37. Zunzunegui MV, Béland F, Recalde JM. La utilización de medicamentos en las personas mayores que residen en su comunidad. Rev Esp Geriatr Gerontol. 1997, 32: 109-15. [ Links ]
38. Mamdani M, Herrmann N, Austin P. Prevalence of antidepressant use among older people: population-based observations. J Am Geriatr Soc. 1999, 47(11): 1350-3. [ Links ]
39. Jorm AF, Grayson D, Creasey H, Waite L, Broe GA. Long-term benzodiazepine use by elderly people living in the community. Aust N Z J Public Health. 2000; 24(1) :7-10. [ Links ]
40. Swartz M, Landerman R, George LK, Melville ML, Blazer D, Smith K. Benzodiazepine anti-anxiety agents: prevalence and correlates of use in a southern community. Am J Public Health. 1991; 81(5): 592-6. [ Links ]
41. Mayer-Oakes SA, Kelman G, Beers MH, De Jong F, Matthias R, Atchison KA, et al. Benzodiazepine use in older, community-dwelling southern Californians: prevalence and clinical correlates. Ann Pharmacother. 1993; 27(4): 416-21. [ Links ]
42. Weyerer S, Dilling H. Psychiatric and physical illness, sociodemographic characteristics, and the use of psychotropic drugs in the community: results from the Upper Bavarian Field Study. J Clin Epidemiol. 1991; 44(3): 303-11. [ Links ]
43. Brown SL, Salive ME, Guralnik JM, Pahor M, Chapman DP, Blazer D. Antidepressant use in the elderly: association with demographic characteristics, health-related factors, and healthcare utilization. J Clin Epidemiol. 1995, 48: 445-53. [ Links ]
44. Kirby M, Denihan A, Bruce I, Radic A, Coakley D, Lawlor BA. Benzodiazepine use among the elderly in the community. Int J Geriatr Psychiatry. 1999, 14: 280-4. [ Links ]
45. Peron EP, Gray SL, Hanlon JT. Medication use and functional status decline in older adults: a narrative review. Am J Geriatr Pharmacother. 2011, 9(6): 378-391. [ Links ]
![]() Correspondence:
Correspondence:
Juan Téllez-Lapeira
Albacete Area VB Health Centre Health
C/ Profesor Macedonio Jiménez s/n
02006 Albacete Spain
E-mail: juanmtellez@gmail.com
Received: 5 December 2015
Revised: 3 April 2016
Accepted: 5 May 2016