Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO  Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.96 no.2 Madrid feb. 2004
| PICTURES IN DIGESTIVE PATHOLOGY |
Clindamycin-induced esophageal ulcer
P. A. Rivera Vaquerizo, Y. Santisteban López1, M. Blasco Colmenarejo, M. Vicente Gutiérrez,
V. García García and R. Pérez-Flores
Departments of Digestive Diseases and 1Internal Medicine. Hospital General Universitario. Albacete, Spain
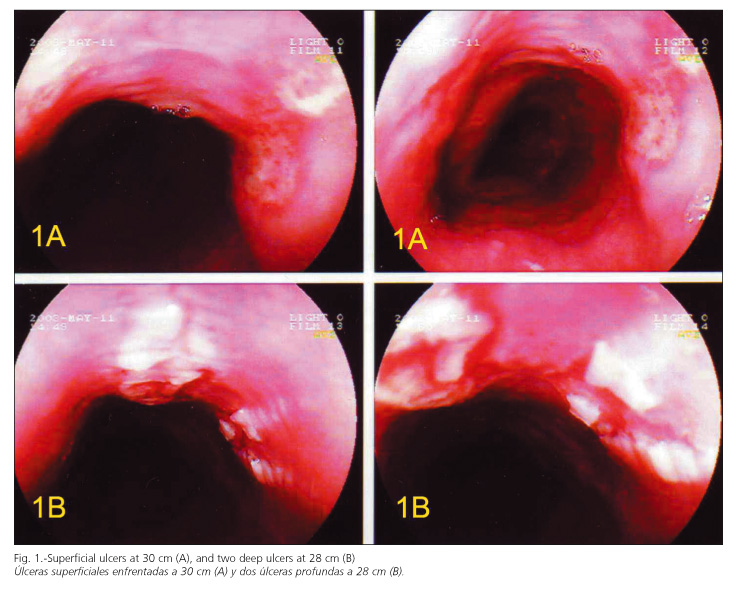
A 27-year-old man with an uneventful record was examined because of ongoing odynophagia and dysphagia at mid esophageal level for a few hours. Five days before he had been operated on for a pilonidal cyst, having henceforth been treated with clindamycin in capsules, which were ingested with very small amounts of liquid. He had been feeling some pain ever since. An upper endoscopy revealed the presence of two superficial ulcers at 30 cm (Fig. 1A) and another two deep, friable-upon-friction ulcers at 28 cm (Fig. 1B). Following a diagnosis of possible esophageal ulcers induced by clindamycin, this drug was discontinued and pantoprazole and sucralfate was administered instead; the patient remains asymptomatic and an upper endoscopy performed 45 days later did not revealed any lesion.
The first known drug-induced esophageal injury was reported by Pemberton in 1970 in a patient taking oral potassium. To date, over 70 drugs have been reported to cause esophageal injury, though the incidence of drug-induced esophageal ulcers is underestimated (2).
The harmful effect of the drug seems to be produced by a direct action on the wall of the esophagus after extended contact. Two mechanisms (3) are involved as far as injuries of this kind are concerned, namely drug-related factors and patient-related factors. Supine position after drug ingestion is present in more than 75% of cases, and drug ingestion with too small amounts of liquid is another triggering factor. Risk increases when both these factors are combined.
Patients with drug-induced esophageal damage very often experience mid-chest pain (61-72%) (4). Pain may increase when further doses of the offending drug, food or fluid are taken. Odynophagia is the next most common symptom (50-74%). These symptoms may develop within hours and up to 10 days after medication onset. Dysphagia, which is less common than chest pain or odynophagia, is reported in 20 to 40% of cases and usually indicates severe inflammatory stenosis or stricture formation.
Upper endoscopy is the technique of choice for the detection of esophageal mucosal injuries, and also allows for direct inspection, biopsy-taking, cytology-sampling and microbiological tests. Findings may vary, and injuries are most frequently located at the junction between the upper and middle parts of the esophagus. This was the location of ulcers seen in our patient, the same as in a similar clindamycin-induced case reported in 1977 (5).
The best treatment is discontinuation of the offending drug and supportive care. There is no evidence that any therapy, other than suppressing the offending drug, may play an active role in the healing process, though antacid, sucralfate and proton pump inhibitors have been used.
REFERENCES
1. Kikendall JW. Pill-induced esophageal injury. Gastroenterol Clin North Am 1991; 20: 835-46.
2. Georges MD, Uri MD, Delpre G, Kadish U, Stahl B. Induction of esophageal injures by doxycycline and others pills. A frequent but preventable occurrence. Dig Dis Sci 1989; 34: 797-800.
3. Del Valle García M, Gómez F, Poyato A, Vignote ML, Miño G. Úlcera esofágica por doxiciclina. Gastroenterol Hepatol 2001; 24: 390-1.
4. Worth H. Drug-induced esophageal damage: diseases of medical progress. Gastrointest Endoscopy 1998; 47 (6): 547-50.
5. Sutton DR, Gosnold JK. Oesophageal ulceration due to clindamycin. Br Med J 1977; 1 (6076): 1598.











 texto en
texto en