Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO  Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.97 no.1 Madrid ene. 2005
| ORIGINAL PAPERS |
Rubber-band ligation for hemorrhoids in a colorectal unit. A prospective study
J. C. Bernal, M. Enguix, J. López García, J. García Romero and R. Trullenque Peris
Service of General Surgery. Hospital General Universitario. Valencia, Spain
ABSTRACT
Introduction: nowadays the rubber band ligation technique is one of the most worldwide used and effective treatment of the hemorrhoidal disease.
Objectives: our study has as a goal to analyze the success or failure of the rubber band ligation in hemorrhoids grade 1,2 and 3, to analyze their complications and to see if all symptomatic hemorrhoids should be treated with ligation at the first visit.
Patients and method: a prospective and descriptive study was designed for patients who came to the Colorectal Unit with hemorrhoidal disease from September 1997 to December 2001. First, second and third degree patients were treated according to the classification of hemorrhoids of St. Mark's Hospital. The technique of ligation after Barron was applied.
Results: from 261 patients with a mean age of 48.3 (range: 16-86), 181 (99 M/82 W) have been treated with Barron's method and 80 with rich fiber diet and water.
Rectal bleeding was the most common symptom (91.16%). Anuscopy showed hemorrhoidal disease in all the cases.
From 181 patients, 19.33% were hemorrhoids degree I, 51.93% degree II and 29.83% degree III. Two hundred and eighty-seven ligation sessions were done and the balance of ligations per patient was 2.45 and 1.5 rubber band per session. The 32% of the patients referred pain after ligation. A 13.81% of cases were operated due to persistent rectal bleeding or hemorrhoidal prolapse.
Conclusions: symptomatic hemorrhoids degree I and II with a short clinical history should be treated initially with a rich fiber and water diet.
The technique of Barron is an effective therapy to treat the hemorrhoids degree 1, 2 and in 74% of success in cases with degree 3.
Key words: Ligation. Hemorrhoidal disease. Rectal bleeding. Rubber band.
Bernal JC, Enguix M, López García J, García Romero J, Trullenque. R. Rubber-band ligation for hemorrhoids in a colorectal unit. A prospective study. Rev Esp Enferm Dig 2003; 96: 38-45.
Recibido: 14-01-03.
Aceptado: 24-02-04.
Correspondencia: Juan-Carlos Bernal Sprekelsen. Servicio de Cirugía General y Digestiva. Hospital General Universitario. Valencia. Avda. Tres Cruces, s/n. 46015 Valencia.
INTRODUCTION
Hemorrhoids are considered one of the most frequent diseases of the anal region with a high prevalence (nearly 50% of proctological visits in a colorectal unit). Its incidence peak is between 45 and 65 years of age, and is more common in males (1). It is the most frequent anorectal pathology with rectal bleeding in primary care (2).
There are a large number of treatments: medical support, instrumental techniques (rubber-band ligation, sclerosis, infrared photocoagulation), and a variety of surgical techniques (Milligan-Morgan, Longo, and other) that have to be used in about 10% of cases (3).
Nowadays, rubber-band ligation is the most widely used procedure, and it offers the possibility to resolve hemorrhoidal disease without the need for hospitalization or anesthesia, and with a lower incidence of complications when compared to conventional surgery (4). Prior experience with this method in our unit has been reported elsewhere (5), but in the present study we changed our focus and evaluate not only the importance of the diagnosis and treatment of hemorrhoids at present, but also the response to treatment in long-term follow-up. Our study goals include: a) to determine the usefulness to follow a protocol in the management of the hemorrhoid bleeding in a proctologic unit; b) to evaluate of the success/failure of the rubber-band ligation in grade-I, II, and III hemorrhoids; and c) to analysis of complications due to ligatures. We wanted also to answer the following questions: a) should all hemorrhoids be treated by rubber-band ligation at presentation (mainly grades I and II)?; and b) should grade III hemorrhoids be treated by ligation?
PATIENTS AND METHODS
A prospective and descriptive study was designed. The Colorectal Unit at Consorcio Hospital General Universitario de Valencia covers Health Care Area 8 with 326,667 inhabitants. All successive patients visiting our Unit because of hemorrhoidal disease between September 1997 and December 2001 were included. Exclusion criteria included: patients with hemorrhoidal disease grade IV not suitable for rubber-band ligation, and immunosuppressed patients, particularly patients with anti-HIV antibody positive.
An "ad hoc" database was set up, which included: age, gender, dates related to past anorectal history or operations, bowel habit, and use of laxatives. Clinical data included: past and present rectal bleeding symptoms, a short history of rectal bleeding (less than 6 months), isolated rectal bleeding episodes, proctalgia, mucus discharge, tenesmus, pruritus/itching, hemorrhoids grades (I-II-III), and complications following ligations. Physical examination included: visual inspection, digital rectal exploration, and anuscopy in all patients. Colonoscopy was done in patients older than 40 years. In patients younger than 40 year, colonoscopy was performed if there was a family history of colorectal neoplasia. Rectoscopy with contrast-enhanced enema was performed in patients refusing colonoscopy.
All patients received a short rectal washout 1-2 hours prior to treatment, with the goal of avoiding bowel movements in the first 24 hours so that ligatures would not be expelled, as was the case in a previous series of 51 patients treated in our hospital (unpublished data).
No antibiotics were administered, except to patients with valvular heart disease or chronic liver disease.
Rubber-band ligation was done with a Heine 20 mm gauge proctoscope. The ligator used was a McGivney device. Piles were held with McGivney forceps, and the patient was placed in a left lateral position. Ligatures were placed about 1 cm above the linea dentata after Barron's technique. Two black rubber bands were placed for every pile. Postligation treatment consisted of standard analgesia with pyrazolones (2 g/8 hours during the first 48 hours or acetaminophen 500 mg in case of pyrazolone allergy. Patients with severe pain received also nonsteroideal anti-inflammatory drugs with gastric protection.
Follow-up was made at one month, six months, 1 year, and then yearly via a telephone questionnaire. Subsequent ligations were performed at one month after the prior one, if the patient still had symptoms.
We followed the hemorrhoid classification criteria developed at St. Mark's Hospital.
Subject descriptions and group comparisons were performed with a descriptive analysis of the sample by adapting frequency distribution to qualitative variables; quantitative variables were analyzed with both centralization (mean) and dispersion (range) measures. Data analysis was done using the computer program SPSS for Windows (SPSS Iberica, Madrid, Spain).
RESULTS
A total of 261 patients with hemorrhoidal disease were included in this study. The mean age was 48.3 years (range, 16-86 years). One hundred eighty one patients (99 man/82 women) underwent to rubber-band ligature following the procedure described by Barron. Eighty patients were treated with watery and fiber-rich diet.
Of 181 cases treated by Barron's method, 153 had an anorectal history of several years' standing (84.53%), and 20 cases had undergone previous anorectal operations. Rectal bleeding was the most common symptom (91.16%) followed by anal pain (39.2%) and itching (53.59 %); other symptoms are listed in table I.
Associated conditions included two cases of previously unknown ulcerative colitis, seven cases with anal fissure, two cases with condyloma acuminata, one case with anal fistula, another with an anal polyp.
A colonoscopy was performed in 72 cases - 67 patients older than 40 years, and five patients younger than 40 (range: 32 and 78 years). Eighteen patients had colonic polyps, 1 case had colon cancer, 2 had ulcerative colitis, and two had chronic nonspecific colitis (Tables II and III).
A barium enema was performed in 29 patients, and was normal in all of them; rectoscopy was carried out in 26 patients, and pathologic findings were detected in 9 of them. Anuscopy evidenced hemorrhoidal disease in all cases (Table II). Of the 181 patients, 32 had grade-I (19.33%), 95 grade-II (51.93%), and 54 grade-III (29.83%) hemorrhoids. A total of 445 ligations in 287 sessions were carried out, with a mean of 2.45 ligations per patient and 1.5 ligations per session; 32% of patients had pain or tenesmus following ligation, whereas 5% had rectal bleeding and 1% had vesical tenesmus (Table IV).
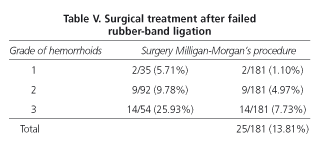
Twenty-five of 181 patients (13.81%) underwent surgery due to persistence of rectal bleeding and hemorrhoidal prolapse. In 2 of 35 patients with grade I hemorrhoids, surgery was indicated because of rectal bleeding, in 9 of 92 cases with grade II hemorrhoids due to rectal bleeding and prolapse and in the remaining 14 cases because of grade III hemorrhoids (Table V).
Patients with a recent history of rectal bleeding (less than six months) [80/261 (30,65%): 44 with grade I, 36 with grade II hemorrhoids] received treatment with a high-fiber and water diet, and remained asymptomatic.
All patients were followed up for one year (100%). From the second year on, follow-up covered not more than 6% (patients lost to follow-up), a fact that led to the administration of a questionnaire by telephone. This allowed to monitor 85% of patients the second year, and up to 67% at year five. The remaining patients could not be contacted.
DISCUSSION
Causes of hemorrhoidal disease are unknown. Constipation and bowel habit distress have usually been involved, but there is no clear evidence of it. The present study, in fact, has found constipation in only 27.62% of patients.
Hemorrhoidal stage is useful for therapeutic assessment, but the fact that prolapse grade may change over time should not be overlooked. We think that the major difficulty is to differentiate grade II from grade III hemorrhoids, with inter-observer agreement being impossible for patients with the same grading in different times of their natural evolution. This may somewhat explain therapeutic failure in patients with grade II hemorrhoids (prolapse reduces spontaneously) that become grade III hemorrhoids (prolapse is reduced manually), and some grade III cases progress to grade IV (irreducible prolapse).
Perhaps we should use the classification by Nicholls and Glass (6). This classification states that prolapse itself would be a clear indication for hemorrhoid therapy using rubber-band ligation, whereas grade I and II hemorrhoids would be managed with medical treatment.
The diagnosis of hemorrhoidal disease is made by anuscopy, which allows 100% of cases to be confirmed. It is important the use of anuscopy and recto-sigmoidoscopy becomes widespread for the etiological diagnosis of rectal bleeding. Colonoscopy may be warranted for patients older than 40 years in view of our findings regarding polyps and other diseases in 32.65% of cases. Therefore, all rectal symptoms should be studied in a protocolized manner, and anuscopy should complete the patient's study in the following cases: a) patients older than 40 years; b) when hemorrhoids do not seem to be the source of rectal bleeding; and c) when bleeding persists after ligation of hemorrhoids.
Anuscopy allows complementary information to be obtained in middle-aged adults with rectal bleeding (7), which is important to have in mind since this is the most important symptom in anal tumors (8). Hemorrhoids -grade I and II- with a short history of rectal bleeding should initially be treated with a high-fiber and water diet (9,10).
In this way, the first step for symptomatic low-grade hemorrhoids is medical treatment: adequate local hygiene, a correct diet, and a stable bowel habit (11,12). Otherwise, if medical treatment fails for grade I and II hemorrhoids, treatment with ligation or other alternatives should be offered (1). Ligation treatment at presentation should be a patient's decision, following informed consent (13).
Barron's method is an efficacious therapy for grade III hemorrhoids, with a success rate of 74.07% in the present study. Rubber-band ligation is an easy and safe technique in treating symptomatic grade II and III hemorrhoids. Our results are similar to those reported in the literature, where success rates for rubber-band ligation range between 70 and 80% (14). A meta-analysis comparing different treatments for hemorrhoids showed that band ligation is the first line of non-surgical treatment for grade I to III hemorrhoids, ahead of sclerotherapy and infrareds (14). Band ligation is a safe technique even in patients with cirrhosis and portal hypertension (15), as well as in patients undergoing anticoagulation therapy. Failed band ligation of grade III hemorrhoids makes surgery necessary in a small percentage of cases, mainly in those with persistent prolapse and bleeding.
Nearly 10% of patients have symptom recurrence after some years (16), and this percentage increases to 40% at one year in patients with grade III hemorrhoids (17). Most frequent complications after ligation include rectal pain/tenesmus and mild bleeding. Severe complications are rare and include severe bleeding (requiring blood transfusion), perineal sepsis, and urinary retention (18). After ligation, pain/tenesmus develops in 32% of patients treated with this method, a finding similar to those by other Spanish authors (1). Foreign authors report higher percentages: 84% of patients have pain on the first day after ligation (18% with moderate to severe pain), and 60% within the first 48 hours (14% with moderate to severe pain) (13). Bleeding is a complication that most usually develops between the 5th and 10th day after ligation. Bupivacaine injections can be useful to relieve pain after ligation (19), as can premedication with dextrometorphane, which also reduces pain after ligation (20); however, we did not use the latter. It is important that a safe margin is provided by applying the ligation at about one centimeter above the dentate line; this relieves pain, but increases therapy failures in grade III hemorrhoids.
In conclusion, we would like to highlight the following: a) rubber-band ligation is an effective treatment for grade I and -II hemorrhoids; b) it is effective in 74% of cases with grade III hemorrhoids, and should therefore be considered as a first-line treatment; c) rectal pain/tenesmus develops in 32% of cases treated with ligation, but is minimized when only one ligation per session is performed; and d) patients with a short history of rectal bleeding should be initially treated with a high-fiber and water diet.
ACKNOWLEDGMENT
We would like to thank Dra. Inocencia Martínez Mir for the review of this article and her statistical approach. Técnico Superior de Investigaciones del Consorcio Hospital General Universitario de Valencia.
REFERENCES
1. Linares Santiago E, Gómez Parra M, Mendoza FJ, Pellicer FJ. Eficacia del tratamiento hemorroidal mediante ligadura con banda elástica y la fotocoagulación infrarroja. Rev Esp Enferm Dig 2001; 93: 238-42. [ Links ]
2. Hussain JN. Hemorrhoids. Prim Care 1999; 26: 25-51. [ Links ]
3. Enciclopedia Médico-Quirúrgica 1987; 2: 40-685. [ Links ]
4. Pezzullo A, Palladino E. Rubber Band Ligation of hemorrhoids. Five years follow-up. Min Chir 2000; 21: 253-6. [ Links ]
5. Trullenque Peris R, García Moncó P, Fernández Tena JM, Bolufer Cano JM, García Vilanova A, Cano Ivorra J. Tratamiento de las hemorroides con ligadura elástica. Rev Quir Esp 1988; 1: 38-41. [ Links ]
6. Nicholls RJ, Glass RE. In: Coloproctology: diagnosis and outpatient management. Berlin: Spring Verlag, 1985. p. 84. [ Links ]
7. Korkis AM, Mc Dougall CJ. Rectal bleeding in patients less than 50 years of age. Dig Dis Sci 1995; 40: 1520-3. [ Links ]
8. Janicke DM, Pundt MR. Anal disorders. Emerg Med Clin North Am 1996; 14: 757-88. [ Links ]
9. Moessgaard F, Nielson Ml, Hansen JB, et al. High fiber diet reduces bleeding and pain in patients with hemorrhoids. Dis Colon Rectum 1982; 25: 454-6. [ Links ]
10. Pérez Miranda M, Gómez Cedenilla A, Loen Colombo T, Pajares J, Male-Jiménez J. Effects of fiber supplements on internal bleeding haemorrhoids. Hepatogastroenterology 1996; 43: 1504-7. [ Links ]
11. Gricar JA, Goodwin SA, Care DG. Hemorrhoids. Manag Care Interface 1998; 11: 50-2. [ Links ]
12. Battochio F, Giacchetto F. Conservative therapy of hemorrhoids. Ann Ital Chir 1995; 66: 761-7. [ Links ]
13. Hardwick RH, Durdey P. Should rubber band ligation hemorrhoids be performed at the initial outpatient visit? Surg Clin North Am 1992; 72: 665-79. [ Links ]
14. Mac Rae HM, McLeod RS. Comparison of hemorrhoidal treatments: a meta-analysis. Can J Surg 1997; 40: 14-7. [ Links ]
15. Pissiotis CA, Komborozos VA, Skrekas GJ. Rubber band ligation of symptomatic internal haemorrhoids: results of 500 cases Dig Surg 2000; 17: 71-6. [ Links ]
16. Konings M, Debets JM, Beaten CG. Rubber band ligation of hemorrhoids. Symptoms almost gone after 6 weeks. Ned Tijdschr Geneeskd 1999; 143: 1841-2. [ Links ]
17. Yárnoz C, Ortiz H. Estado actual del tratamiento de las hemorroides. Cirugía Andaluza 1997; 4: 342-4. [ Links ]
18. Spallanzani A, Richi E, Carriero A, Fundaro S. Rubber band ligation. Our experience. Minerva Chir 1997; 52: 1017-51. [ Links ]
19. Hooker GD, Plewes EA, Rajgopal C, Taylor BM. Local injection of bupivacaine after rubber band ligation of hemorrhoids: prospective and randomised study. Dis Colon Rectum 1999; 42: 174-9. [ Links ]
20. Liu St, Wu CT, Yeh Cc, Ho St. Premedication with dextrometorfan provides posthemorrhoidectomy pain. Dis Colon Rectum 2000; 43: 507-10. [ Links ]











 texto en
texto en