Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.101 no.1 Madrid ene. 2009
PICTURES IN DIGESTIVE PATHOLOGY
Duodenal leishmaniasis in a HIV patient
Leishmaniasis duodenal en paciente VIH positivo
J. Egea Valenzuela, R. Baños Madrid, J. L. Rodrigo Agudo, C. Galera Peñaranda1, A. Torroba2, J. Molina Martínez and F. Carballo Álvarez
Services of Digestive Disease, 1Internal Medicine. HIV Unit, and 2Pathology. University Hospital Virgen de la Arrixaca. Murcia, Spain
Clinical case
We report the case of a 31-year-old male who was diagnosed with HIV infection eleven years ago. At this moment his disease is in stage C3. He consulted because of watery diarrhea with no pathologic products for the last 5 months. He also reported continual abdominal pain unrelated to food ingestion. Over those months he lost about 7-8 kg of body weight, and some skin nodes developed in different parts of his body.
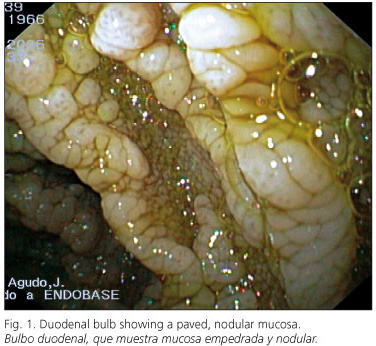
Laboratory parameters were nonspecific in the first study. Antibodies against Leishmania, CMV, syphilis, HBV, and HCV were all negative. Blood and stool cultures and parasite tests were all negative, too. A biopsy was obtained from skin nodes, which was positive for Leishmania, and a digestive endoscopy was carried out, which showed a paved, nodular mucosa all over the duodenum, from which we took several biopsies (Figs. 1 and 2). A histological study revealed a clear, severe infiltration of duodenal villi by macrophages filled with Leishmania bodies (Fig. 3).
Diagnosis: malabsorption due to visceral leishmaniasis with skin and small-bowel infiltration in a HIV patient.
Discussion
Leishmaniasis is a parasitic disease transmitted by the biting of Phlebotomus, a kind of mosquito, and caused by different species of Leishmania. There are three forms of presentation: skin nodes (caused by Leishmania tropica), mucocutaneous involvement (caused by Leishmania braziliensis) and visceral leishmaniasis (caused by Leishmania donovani and Leishmania infantum). It is especially frequent in areas by the Mediterranean sea.
Visceral leishmaniasis, an opportunistic disease, usually develops in HIV patients with a previous diagnosis of AIDS, and is less frequent in other types of immunodepression. The disease usually manifests with fever, general discomfort, and hepatosplenomegaly. Digestive involvement is rare (only 5 to 10% of all visceral leishmaniasis cases), and presentation is also different, with predominant watery diarrhea, nausea, weight loss, and abdominal pain.
Diagnosis requires Leishmania bodies to be found in the histological study of various tissues.
Recommended references
1. Boukthir S, Mejri A, M'rad S, Barsaoui S. Visceral Leishmaniasis diagnosed on duodenal biopsy in a child. Acta gastroenter Belg 2003; 66: 258-9. [ Links ]
2. Pasquau F, Ena J, Sanchez R, Cuadrado JM, Amador C, Flores J, et al.; Leishmania HIV Mediterreanean Co-operative Group. Leishmaniasis as an opportunistic infection in HIV-infected patients: determinants of relapse and mortality in a collaborative study of 228 episodes in a Mediterreanean region. Eur J Clin Microbiol Infect Dis 2005; 24: 411-8 [ Links ]
3. Ferreira MS, Borges AS. Some aspects of protozoan infections in inmunocompromised patients. Mem Inst Oswaldo Cruz. 2002; 97: 443-57. [ Links ]
4. Berenguer J, Moreno S, Cercenado E, Bernaldo de Quirós JC, García de la Fuente A, Bouza E. Visceral Leishmaniasis in patients infected with human immunodeficiency virus. Ann Intern Med 1989; 111: 129-31. [ Links ]











 texto en
texto en