Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.102 no.1 Madrid ene. 2010
LETTERS TO THE EDITOR
Groove pancreatitis with duodenal stenosis
"Groove pancreatitis" o pancreatitis del surco con estenosis duodenal
Key words: Pancreatoduoenal groove. Groove pancreatitis. Pancreatic cancer.
Palabras clave: Surco pancreaticoduodenal. Pancreatitis del surco. Cáncer de páncreas.
Dear Editor,
Groove pancreatitis (GP) is a rare subtype of chronic pancreatitis. It is a special form of segmental pancreatitis characterized by fibrous scars of the anatomic space between the dorsocranial part of the head of the pancreas, the duodenum and the common bile duct.
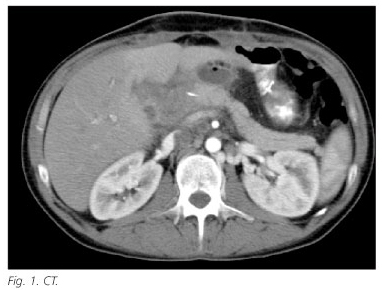
We report the case of a 40-year-old man, with a past history of chronic alcohol consumption and parenteral drugs addiction. He presented complaining of abdominal pain over three months with nocturnal exacerbations and incoercible vomiting. His blood tests upon admission were found to be normal except for a slight elevation of serum pancreatic enzymes. Computerised tomography (CT) (Fig. 1) scan of the abdomen revealed an enhanced mass in the head of head of pancreas and a cystic 7 mm lesion between the pancreatic head and the duodenum. The duodenum was involved by the inflammatory process showing thickening of the wall and partial stenosis of the second portion. Endoscopic evaluation of the upper gastrointestinal tract showed gastric stasis with retained fluids associated with stenosis of the second duodenal portion.
The patient was hospitalized for the one month and treated conservatively, consistent with the diagnosis of GP. However, after repetead episodes of abdominal pain and the development of oral intolerance, the patient was referred to the General Surgery Unit and finally a cephalic pancreatoduodenectomy was performed. The histological evaluation of the resected specimen confirmed the inflammatory nature of the changes involving the duodenal wall and pancreaticoduodenal interface, and the presence of inflamed, cystically dilated ducts of ectopic pancreatic tissue within the periampullary duodenal wall. The patient has had a favourable postoperative course. He has been followed at the out-patient clinic and has had an uneventful recovery.
Discussion
GP is an uncommon subtype of focal pancreatitis and only a few case reports have been published. The differential diagnosis of GP from pancreatic head carcinoma is difficult, since specific discriminating imaging features are lacking. The appearance of GP may resemble pancreatic, common bile duct or duodenal wall cancer, conditions which require prompt surgical intervention. Distinguishing between GP and pancreatic carcinoma may be difficult, particularly in those cases in which the carcinoma has a large fibrous component. Other differential diagnoses for GP include: a) pancreatic diseases, such as acute pancreatitis with inflammation of peripheral pancreatic zones; exophytic pancreatic ductal adenocarcinoma; or neoendocrine tumours such as gastrinoma; b) duodenal diseases such as periampullary diverticulum; c) bile ducts diseases such as cholangiocarcinoma and choledochal cysts; and d) diseases which involve adenopathies.
GP is an uncommon type of focal chronic pancreatitis affecting the groove between the head of the pancreas, the duodenum and the common bile duct. The clinical presentation is similar to more prevalent forms of chronic pancreatitis, but recurrent vomiting, attributable to marked duodenal stenosis and impaired motility, tends to be more pronounced in GP.
GP appearance may resemble head pancreatic carcinoma, so it is necessary to take notice of differential diagnosis of the pancreas head tissues and duodenal stenosis. In cases where the diagnosis is in doubt, or there are local complications, or when treatment is ineffective; a cephalic pancreatoduodenectomy with histological examination of the excised tissue should be performed.
C. Viñolo-Ubiña, J. Morales-Ruiz, C. Heredia-Carrasco, M. Ruiz-Cabello-Jiménez, M. T. Villegas-Herrera and D. Garrote-Lara
Services of Digestive Diseases and General Surgery. University Hospital Virgen de las Nieves. Granada, Spain
Recommended references
1. Stolte M, Weiss W, Volkholz H, Rosch W. A special form of segmental pancreatitis: ''groove pancreatitis''. Hepatogastroenterology 1982; 29: 198-208. [ Links ]
2. Becker V, Mischke U. Groove pancreatitis. Int J Pancreatol 1991; 10: 173-82. [ Links ]
3. Yamaguchi K, Tanaka M. Groove pancreatitis masquerading as pancreatic carcinoma. Am J Surg 1992; 163:312-6. [ Links ]
4. Shudo R, Yazaki Y, Sakurai S, Uenishi H, Yamada H, Sugawara K, et al. Groove pancreatitis: report of a case and review of the clinical and radiologic features of groove pancreatitis reported in Japan. Intern Med 2002; 41: 537-42. [ Links ]
5. Mohl W, Hero-Gross R, Feifel G, Kramann B, Puschel W, Menges M, et al. Groove pancreatitis: an important differential diagnosis to malignant stenosis of the duodenum. Dig Dis Sci 2001; 46: 1034-8. [ Links ]
6. Itoh S, Yamakawa K, Shimamoto K, Endo T, Ishigaki T. CT findings in groove pancreatitis: correlation with histopathological findings. J Comput Assist Tomogr 1994; 18: 911-5. [ Links ]
7. Gabata T, Kadoya M, Terayama N, Sanada J, Kobayashi S, Matsui O. Groove pancreatic carcinomas: radiological and pathological findings. Eur Radiol 2003; 13: 1679-84. [ Links ]











 texto en
texto en