Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.102 no.4 Madrid abr. 2010
Intraabdominal hemophilic pseudotumor: case report
Pseudotumor hemofílico intraabdominal. A propósito de un caso
R. García-Pérez, G. Torres-Salmerón, F. Sánchez-Bueno, A. García-López and P. Parrilla-Paricio
Department of Surgery. Virgen de la Arrixaca Hospital. El Palmar, Murcia. Spain
Introduction
Hemophilia A is a congenital clot pathology transmitted by the X chromosome with recessive character that is characterized by the deficient production of the VIII factor (1). About one third of the cases are produced by novo mutations, without any previous family medical history of hemophilia. It has an estimated incidence from 10 to 20 cases for 100,000 males (2). Clinically it manifests itself by a hemorrhagic syndrome that may appear on any location. A rare complication is the hemophilic pseudotumor, also called hemophilic cyst. The first description of a hemophilic pseudotumor was, in 1918, by Starker (3) in a 14 year old male that presented a massive hematoma along extensive bone femur destruction. After the first description around a 100 cases have been published affecting mainly the musculoskeletal system. In the bibliography revision there are none described in the intraabdominal cavity, on pelvic level. The aim of this study is to describe a patient with a hemophilic intraabdominal pseudotumor and make a review of the literature on this subject.
Clinical case
Thirty four year old male diagnosed with severe hemophilia A in Cuba 25 years ago (Cuba is his native country and he has been a resident in Spain for the last 6 years). He did not refer any medical family history. During these years presented two episodes of hemarthros in the right knee, treated conventionally, and requiring cryoprecipitations. Previous to the actual episode, he was asymptomatic and had none medical home treatment.
The patient arrived to the emergency room of another hospital for abdominal pain located on the hypogastrio with a 3 hours development associated to hematuria.
After the analytics and radiologies he was diagnosed with nephritic colic, being discharged with analgesic treatment.
Five hours later, during micturition, he suffered syncope with loss of knowledge that lasted few seconds, reason for which he came to emergency room of our hospital.
On the physical exploration the patient was conscious and oriented, with a regular general condition and intense mucocutaneous paleness. The systolic blood pressure was 70 mmHg and the diastolic was 37 mmHg with a heart rate of 61 beats/min. On the abdominal exploration the abdomen was distended, painful to diffuse palpation, with defense and general peritoneal irritation signs. The analytics presented a hematocrit of 20%, with an hemoglobuline of 6.7 g/dl. Leukocytes 12,270/uL (84% neutrophils) and platelets 358,000/uL. Prothrombin activity 100%, APTT 46%.
The ultrasound scan performed on the patient revealed plenty left subdiaphragmatic loose liquid, subhepatic and on both paracolic gutters. In the rectovesical pouch an oval image could be visualized with liquid in its interior. A CT was ordered, showing the same retro and supravesical cyst image with a 5 cm diameter mass that seemed to depend on an arterial blood vessel but without detecting its origin (Fig. 1).
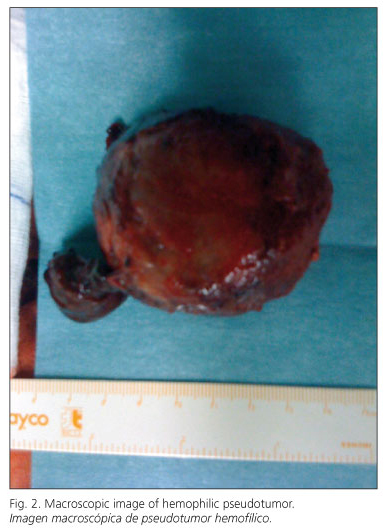
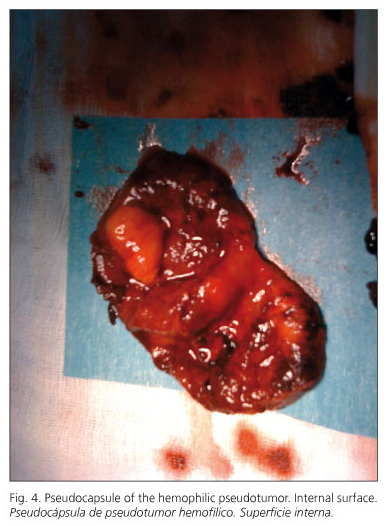
In view of the suspicion of bleeding in a hemophilic patient it was decided to perform an immediate transfusion of 2 packs of red blood and 3 vials of VIII factor besides another one of recombining VII factor. The administration of VIII factor required the analytic evaluation of the VII antifactor Ab that came back positive, reason for which previous to its administration, it required the application of inhibitors of the anti-factor VIII Ab (4). After the improvement on the analytics and the persistent bad general condition of the patient, the decision was to operate by medium supra-infraumbilical laparothomy discovering haemoperitoneum of approximately 3 liters of clots and red blood. A tumorous retrovesical cyst with a 6 cm mass was found. It had an elastic consistence and even surface, intimately attached to vesical posterior face. Blunt dissection and excision of the tumor was performed. Later on the abdominal cavity was checked without identifying a bleeding active point (Figs. 2, 3 and 4).
The patient progressed satisfactorily in the hospital, showing no fever with a sustained hematocrit and decreasing volumes because of the draining, reason for which he was discharged on the tenth postoperating day.
The patient required hematology controls after the administration of the VIII factor every 12 hours during the first four days.
The pathologic anatomy informed a dome shaped formation with a 6.5 cm diameter mass. The external surface was even and the internal one presented multiple hematic hard clots. The fibrous dome contained moderated inflammatory infiltration of chronic unspecified predominance with some pulmonary haemosiderinladen macrophages. In the internal surface presented, besides the hematic attached surface, mature fatty tissue, everything compatible to a hemophilic pseudo-tumor.
Discussion
In accordance with the level of deficiency of the antihemophilic factor (AHF), the hemophilia is classified as mild (> 5% of AHF), moderate (1-5% de HAF) and severe (< 1% HAF). The symptoms depend on the deficiency degree of the coagulation factor. In the severe hemophilia, hemorrhagic spontaneous phenomena´s occur mainly in the osteoarticular system, soft tissues or natural cavities. In the moderate hemophilia spontaneous bleeding may exist occasionally, being specially serious in patients subjected to traumatisms and surgery (5).
In the mild form, bleedings are not frequent if there is no severe traumatism or major surgery as a trigger.
The hemophilic pseudotumor (6) is a rare and serious complication of the typical hematomas of this condition. It manifests as an unpainful cystic mass of slow and irregular growth that may compress vital organs or open to the exterior. It is an infrequent complication that shows up in 1-2% of the patients affected by the severe types and is usually related to a traumatic precedent.
In our case, there was neither traumatic precedent nor previous surgery. Generally it is located in soft tissues like the muscle, in other occasions in bones (7), but can occasionally affect the lung (8) and even intraabdominal organs.
Probably the most affected muscle is the iliopsoas. Other described locations with less frequency are the orbit, the jaw and the jawbone. There are none descriptions of intraabdominal location (9) as presented in our case.
A pseudotumor consists on blood products in different evolution stages surrounded by a fibrous capsule that contains macrophages charged with hemosiderin. The progressive growth of these benign masses compresses the adjacent structures and causes bone destruction besides muscle and skin necrosis. Regularly it involves unpainful masses that remain asymptomatic for long periods of time. If complications show up, they may reinfect, form fistulas or break spontaneously producing hemorrhagic phenomena.
As to the diagnostic handle, the CT (10) is particularly useful in the osseous evaluation, while the MRI is superior to determine if soft tissues are affected.
Handling these patients is complex and must be done by multidisciplinary teams on specialized centers. The most important fact for its treatment and the decrease on the incidence is the early diagnosis and preventing the formation of hematomas. There are multiple therapeutic alternatives for this entity: conservative handle, surgical extirpation, arterial embolization and radiotherapy. In our case the urgent surgical intervention was decided in the light of the hemodynamic deterioration of the patient. The conservative treatment consists on the infusion of the factor VIII and the immobilization of the patient. In these cases there might be regression, though in never heals. This kind of treatment is recommended only in patients with high levels of factor inhibitor when surgery is not possible. The surgical removal (11,12) is the treatment of choice established by most publications.
It should be performed on specialized centers due to the fact that it is not free of complications and presents a death rate of 20%. Besides, meticulous determinations of the factor should be performed during the surgery and the postoperatory right away. The arterial embolization (13,14) is a therapeutical weapon that allows to reduce the vascularization of the tumor, reduce its size and therefore, the risk of bleeding during the surgery. The radiotherapy (15) with 10-20 g doses has been used in cases where surgery is out of question and the patient does not respond to conservative treatment (16).
Without treatment, the natural evolution of this tumors leads to the compression of nearby visceral as well as neural and even vascular structures, with the chance of evolving into tissue adjacent destruction even with osseal erosion.
Concluding, the hemophilic pseudotumor is a rarely frequent complication, but requires multidisciplinary teams for its correct treatment.
References
1. Mathew M, Goel G, Kurien A. Digital pseudotumor associated with Von Willebrand disease. The Internet Journal of Hematology 2009; 5(2). [ Links ]
2. Van der Bom JG, ter Avest P, Van den Berg HM, Psaty BM, Weiss NS. Assessment of incidence of inhibitors in patients with haemophilia. Haemophilia 2009; 15(3): 707-11. [ Links ]
3. Stafford JM, James TT, Allen AM, Dixon LR. Hemophilic pseudotumor: radiologic-pathologic correlation. Radiographics 2003; 23: 852-6. [ Links ]
4. Smejkal P, Brabec P, Matyskova M, Bulikova A, Slechtova M, Kissova J, et al. FEIBA in treatment of acute bleeding episodes in patients with haemophilia A and factor VIII inhibitors: a retrospective survey in regional haemophilia centre. Haemophilia 2009; 15(3): 743-51. [ Links ]
5. Huth-Kühne A, Baudo F, Collins P, Ingerslev J, Kessler CM, Lévesque H, et al. International recommendations on the diagnosis and treatment of patients with acquired hemophilia A. Haematologica 2009; 94(4): 566-75. [ Links ]
6. Rodriguez-Merchan EC. The haemophilic pseudotumour. Haemophilia 2002; 8(1): 12-6. [ Links ]
7. Castro-Boix S, Pradell-Teigell J, Boqué-Genovard R, Zanón-Navarro V, Nadal-Guinard A, Altisent-Roca C, et al. Hemophilic pelvic pseudotumor. Cir Esp 2007; 81(2): 102-4. [ Links ]
8. Bicknell S, Mason AJ. Hemophilic pseudotumor of the chest. Thorac Imaging 2001; 16(3): 188-90. [ Links ]
9. Preston A, Griscom N. Pediatric case of the day: hemophilic pseudotumor of the left ilium. Radiographics 1991; 11: 501-3. [ Links ]
10. Hermann G, Yeh HC, Gilbert MS. Computed tomography and ultrasonography of the hemophilic pseudotumor and their use in surgical planning. Skeletal Radiol 1986; 15(2): 123-8. [ Links ]
11. Ahuja SP, Sidonio R Jr, Raj AB, Bertolone SJ, Silverman C, Antekeier DP, et al. Successful combination therapy of a proximal haemophilic pseudotumour with surgery, radiation and embolization in a child with mild haemophilia A. Haemophilia 2007; 13(2): 209-12. [ Links ]
12. Iwata H, Oishi Y, Itoh A, Ishiguro N, Yamaga H, Miyamoto N, et al. Surgical excision of hemophilic pseudotumor of the ilium. Clin Orthop Relat Res 1992; (284): 234-8. [ Links ]
13. Rodriguez-Merchan EC, Jimenez-Yuste V. The role of selective angiographic embolization of the musculoskeletal system in haemophilia. Haemophilia 2009; 15(4): 864-8. [ Links ]
14. Pisco JM, Garcia VL, Martins JM, Mascarenhas AM. Hemophilic pseudotumor treated with transcatheter arterial embolization: case report. Angiology 1990; 41(12): 1070-4. [ Links ]
15. Espandar R, Heidari P, Rodriguez-Merchan EC. Management of haemophilic pseudotumours with special emphasis on radiotherapy and arterial embolization. Haemophilia 2009; 15(2): 448-57. [ Links ]
16. Subasi M, Dirier A, Kapukaya A, Uludag A, Karadayi B, Cebesoy O. Successful treatment of hemophilic hand pseudotumors by only radiotherapy. Ann Plast Surg 2007; 59(3): 338-40. [ Links ]
![]() Correspondence:
Correspondence:
Gloria Torres Salmerón.
Servicio de Cirugía, 3a planta.
Hospital Virgen de la Arrixaca.
Ctra. Madrid-Cartagena, s/n. 30120 El Palmar, Murcia.
e-mail: gtorres-salmeron@yahoo.es
Received: 18-01-10.
Accepted: 22-01-10.











 texto en
texto en