Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.102 no.5 Madrid may. 2010
LETTERS TO THE EDITOR
Glycogenic acanthosis of the esophagus: an unusually endoscopic appearance
Acantosis glucogénica del esófago: un hallazgo endoscópico inusual
Key words: Glycogenic acanthosis. Endoscopic appearance.
Dear Editor,
Glycogenic acanthosis of the esophagus is a common benign entity characterized by multifocal plaques of hyperplastic squamous epithelium with abundant intracellular glycogen deposits (1). At esophagoscopy these lesions appear as slightly raised grey-white plaques which are usually 2-10 mm in diameter and may be confluent. Although they may involve any segment, the literature suggests that are most common in the distal third (2).
Case report
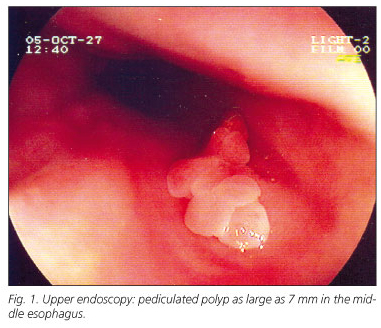
A 78-year-old white male admitted to the Medicine Department with microcytic anaemia [haemoglobin: 8.8 g/dl (13-15); mean corpuscular volume: 66 fl] and for a suspicion of lead poisoning. He had a diffuse abdominal pain, nausea, anorexia, asthenia and constipation. There were no symptoms of esophageal reflux or dysphagia. He drank heavily (100 g of wine per day) and smoked three packs of cigarettes a day for 30 years. Current medications included furosemide, perindopril and metformin for hypertension and diabetes mellitus. On examination, he presented cutaneomucosal pallor, tenderness in the lower quadrants and peripheral edema. An upper endoscopy revealed a pale-pink, lobulated and pediculated polyp as large as 7 mm in diameter in the middle esophagus (Fig. 1). A polypectomy was performed and histology demonstrated glycogenic acanthosis (Figs. 2 and 3). A grade B esophagitis in the distal third and a linear area of red mucosa, 2 cm above the esophago-gastric transition were also visualized. Biopsy of that area revealed Barrett's epithelium with no dysplasia. Acid-reducing drug was instituted. A total colonoscopy was performed and revealed no changes. Abdominal ultrasonography showed only hepatic steatosis. The blood lead level was 3,848 μg/L (40-290) which confirmed the lead poisoning's diagnosis. Chelation therapy was started with symptomatic and laboratory improvement.
Discussion
Glycogenic acanthosis is a benign entity of unknown pathogenesis and etiology, perhaps representing a degenerative or reactive phenomenon involving the squamous esophageal epithelium, apparently age-related and progressive (1). Despite the name, there is no association with abnormalities of glucose metabolism or with skin disorders, such as acanthosis nigricans. There isn't a clear relationship to smoking, alcohol, hot liquids or acid reflux (3,4). In fact, despite the antireflux therapy seems to improve symptoms, it failed to eradicate the lesions of glycogenic acanthosis (4). Unless there is a coexisting disease, patients with glycogenic acanthosis are asymptomatic (2). The present case, endoscopy was performed in the workup of microcytic anaemia.
The overall incidence in the general population is difficult to determine (endoscopic series have ranged from 5-15%). Endoscopy shows whitish mucosal elevations usually less than 0.5 cm surrounding by normal mucosa. A few or multiple lesions may be found assuming sometimes a confluent conglomeration with a cobblestone mucosal pattern. Exceptionally, nodularity is focal or there is diffuse fold thickening, such cases endoscopy may be necessary to exclude some other possibilities, particularly superficial carcinoma (2). In contrast with literature, the endoscopic appearance of the current case has never been reported. Morphology and the underlying disease have led to a resection because it's important to recognize the nature of the lesion. Pathologically, the squamous epithelium is focally thickened by groups of enlarged and clear cells located in the upper layers of the epithelium which contain abundant cytoplasmic glycogen and appear clear because of routine histological processing removal (1,3).
In summary, glycogenic acanthosis seems to have no clinical significance and endoscopy should be used only when the appearance is atypical and/or the clinical suspicion of esophageal disease is high. Furthermore, this condition must be differentiated from lesions of similar appearance and more important prognostic significance.
S. Lopes, P. Figueiredo, P. Amaro, P. Freire, S. Alves, M. A. Cipriano, H. Gouveia, C. Sofia and M. Correia-Leitão
Department of Gastroenterology. Coimbra University Hospital. Coimbra, Portugal
References
1. Ghahremani GG, Rushovich M. Glycogenic acanthosis of the esophagus: radiographic and pathologic features. Gastrointest Radiol 1984; 9: 93-8. [ Links ]
2. Glick SN, Teplick SK, Goldstein J, Stead JA, Zitomer N. Glycogenic acanthosis of the esophagus. Am J Roentgenol 1982; 139(4): 683-8. [ Links ]
3. Bender MD, Allison J, Cuartas F, Montgomery C. Glycogenic acanthosis of the esophagus: a form of benign epithelial hyperplasia. Gastroenterology 1973; 65(3): 373-80. [ Links ]
4. Vadva MD, Triadafilopoulos G. Glycogenic acanthosis of the esophagus and gastroesophageal reflux. J Clin Gastroenterol 1993; 17(1): 79-83. [ Links ]