Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.103 no.1 Madrid ene. 2011
LETTERS TO THE EDITOR
Upper gastrointestinal bleeding as an initial manifestation of metastasis, secondary to a choriocarcinoma in a patient suffering from testicular mixed germ cell tumour
Hemorragia de tubo digestivo alto como manifestación inicial de metástais, secundario a coriocarcinoma en un paciente con tumor germinal mixto de testículo
Key words: Upper gastrointestinal bleeding. Choriocarcinoma.
Palabras clave: Hemorragia de tubo digestivo alto. Coriocarcinoma.
Dear Editor,
Testicular tumor in germinal cells is the most common neoplasia in men between 15 and 35 years old. Choriocarcinoma represents less than 1% of testicular tumors. The main characteristic of these tumors is that they metastasize to retroperitoneal lymph nodes, less frequently, to lungs, liver and brain in 80% of the cases. Metastasis to gastrointestinal tract is extremely rare, around 5%. 95% of the cases are presented in the small bowel, the duodenum being the most usual site followed by the esophagus, stomach and colon.
Clinical case
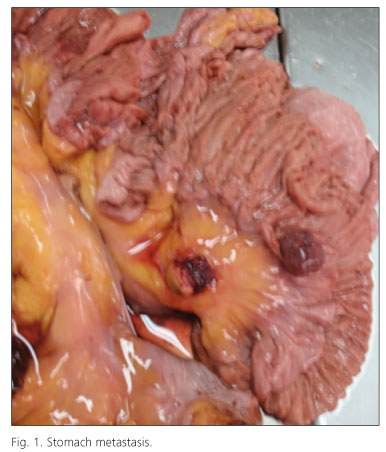
We present a clinical case where a 25-year-old male with no significant medical background was admitted showing asthenia, adinamy, general discomfort, hiporexy, dizziness, palpitations, dyspnea, melenic stool and a six kilo weight loss within one month. Physical Exploration: pale, rhythmic cardiac noises increased in intensity and frequency, plurifocal holosystolic murmur. Abdomen: no pain during palpation, without visceromegalies or palpable masses. Genitals: right testicle showed a volume increase of 5 x 5 cm, petrous, painless, without color changes on skin. Lab Studies: Hemoglobin 5.5 mg/dl, hematocrit 15%, lactate dehydrogenase 1237 UI/L, alpha-fetoprotein 11.1 ng/ml, human chorionic gonadotrophin beta fraction higher than 1,000 ng/ml. Panendoscopy: reported a 2 mm diameter purplish polypoidal injury with minor curvature. The chest radiography showed cannonball pulmonary injuries related to metastasis. The chest-abdominal-pelvic tomography showed: multiple, different sizes rounded images distributed all around the pulmonary parenquime and right scrotal sac occupied by an isodense image with hyperdense pointed-shaped images in its periphery. During his stay in the hospital, he developed multiple skin lesions with nodular appearance, erythematous-purplish with friable surface, some of them ulcerated, with active bleeding, aside from intermittent and profuse bleeding events on the high digestive tube, he developed a serious respiratory insufficiency resulting in death. The autopsy showed an increase, in weight and size, of the right testicle, with a hard consistency and normal residual tissue only at the periphery, the rest of the testicle has a necrohemorragic appearance with peripheral bleeding and central necrosis predominance. The microscopic analysis showed neoplastic cells, some of them with eosinophilic cytoplasm, unique central nucleus with pleomorphism in chords, which corresponds to cytotrophoblastic cells; the other cell type consists in pleomorphic cells, multi-nucleus, with limited cytoplasm, eosinophilic and vacuolar, which belong to the syncytiotrophoblastic type. Neoplastic cells, with syncytiotrophoblast and cytotrophoblast characteristics were also found in the stomach, skin, tongue, thyroid gland, brain, lung, right suprarenal, kidneys, bladder, prostate, duodenum, jejunum, colon, and liver (Fig. 1).
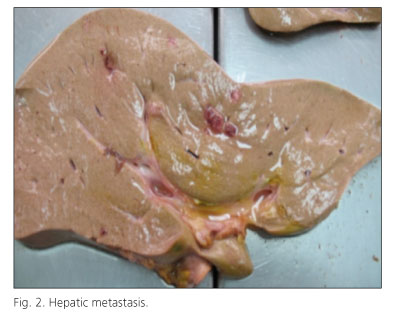
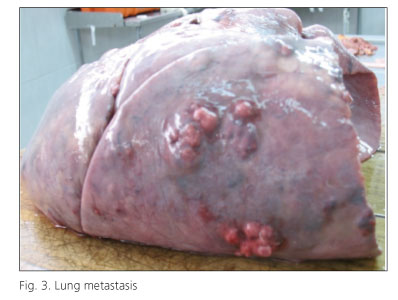
Discussion
The aggressive evolution of this tumour in such a short time caused the patient to develop skin damage, from which biopsies were taken. They showed metastatic choriocarcinoma and confirmed the testicular tumour diagnosis. Approximately 20 cases of skin metastasis have been reported around the world (1,2). There are specific tumor markers to make the diagnosis easier. The serum levels of human chorionic beta-gonadotrophin (B-hCG) are high in the 100% of the choriocarcinomas, while it might be a raise of alpha-fetoprotein in mixed histology choriocarcinomas. Unfortunately for the patient the fast installation of metastatic lung injuries led to his death before he could receive the proper treatment, which is combined chemotherapy with a high dose of cisplatinum, etoposide and bleomicine, aside from the surgical treatment. In the intended search for metastatic injuries to the stomach in these kind of tumors we found only 8 cases worldwide, which confirms that it is an extraordinarily rare injury, more frequently being skin metastasis (3-6).
M. Fosado Gayosso1, J. L. Pérez Hernández1, F. Bernal Sahagún1, C. Acevedo García2, E. L. Aguilar Ayala3 y J. Pérez Espinosa3
1Servicio de Gastroenterología.
2Servicio de Urología.
3Servicio de Anatomía Patológica. Hospital General de México, O.D. México, DF.
References
1. Saito J, Miyagawa Y, Kamoto A, et al. Testicular cancer metastatic to multiple organs including the stomach, kidneys, and skin: a case report. Urology Hinyokika Kiyo 2006; 52 (4): 297-301. [ Links ]
2. Hapa AA, Erkin G, Boztepe G, Baydar DE, Ustun H. Testicular mixed germ cell tumor metastasizing to skin as choriocarcinoma. Int J Dermatol 2008; 47(10): 1090-2. [ Links ]
3. Harikumar R, et al. Testicular choriocarcinoma with gastric metastasis presenting as hematemesis. Indian J Gastroenterol 2004; 23(6): 223-4. [ Links ]
4. Zerbib P, Prieur E, Khoury-Helou A, Catala P, Pruvot FR, Chambon JP. Hemorrhagic digestive metastases from testicular choriocarcinoma. Ann Chirurgie 2002; 127(4): 300-1. [ Links ]
5. Stokes EW, Perkins C. Testicular choriocarcinoma. An unusual presentation as occult gastrointestinal blood loss. J Adolesc Health Care 1989; 10(2): 146-50. [ Links ]











 texto en
texto en