Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.109 no.2 Madrid feb. 2017
https://dx.doi.org/10.17235/reed.2016.4620/2016
ORIGINAL PAPERS
What is the real-life maintenance mesalazine dose in ulcerative colitis?
Alicia Algaba1, Iván Guerra1, Ana García-García-de-Paredes2, María Hernández-Tejero1, Carlos Ferre2, Daniel Bonillo1, Lara Aguilera2, Antonio López-Sanromán2 and Fernando Bermejo1
1Department of Gastroenterology. Hospital Universitario de Fuenlabrada. Fuenlabrada, Madrid. Spain.
2Department of Gastroenterology. Hospital Universitario Ramón y Cajal. Madrid, Spain
ABSTRACT
Objective: To describe how mesalazine (MSZ) is used in our practice in ulcerative colitis (UC), at what dose, and the success rate (regarding adherence to therapy).
Methods: Observational, transversal study, including all patients with UC and with MSZ maintenance therapy seen from September 2014 to February 2015 at two IBD units in Spain. Treatment adherence was measured by the Morisky-Green scale.
Results: We included 203 patients (mean MSZ dose: 2.6 ± 1.0 g/d; median of treatment: 19.5 months [IQR: 8-48]). Doses < 2 g/d were used in 15.3% of cases, 2-2.9 g/d doses in 35.0%, 3-3.9 doses in 29.5%, and ≥ 4 g/d doses in the remaining 20.2%. A single daily dose was preferred in 51.2% of cases, two doses in 33.0% and three doses in 15.8%. A different MSZ brand had been previously used in 36.6% of patients. In 134 cases (66%), the maintenance dose had been increased during a flare-up, and in 49 (36.6% of cases) this higher dose had been kept for maintenance (dose ≥ 4 g/d in 36 patients). During the MSZ therapy, 14 patients (6.9%) suffered mild side effects (21.4% altered liver function tests). Therapy adherence was good in 81.8% of cases.
Conclusions: Half of our UC patients take high MSZ doses (≥ 3 g/d) as maintenance therapy, with acceptable safety and good adherence. Half of all patients take a single daily dose, and one third needed a different commercial brand during therapy. Opting for a higher MSZ maintenance dose is a possible strategy for a satisfactory maintenance therapy.
Key words: Mesalazine. Ulcerative colitis. Maintenance therapy. Dose schedule. Adherence.
Introduction
Ulcerative colitis (UC) is a chronic inflammatory condition of the colon characterized by diffuse mucosal inflammation, bloody diarrhea, and urgency (1). UC follows periods of inactivity and relapse, so that different types of treatments are necessary to induce or maintain remission (2). The extension and natural course of a disease determines the evolution and treatment used to control it (2).
Although new treatment options have emerged, mesalazine (MSZ) is frequently used as maintenance therapy for UC (3,4). In fact, 5-aminosalicylic acid (5-ASA) is considered as first-line therapy for inducing and maintaining remission of mildly to moderately active UC (5,6). 5-ASA preparations were created to avoid adverse effects of sulfasalazine. The mechanisms of action proposed for this drug have been numerous, including inhibition of the activity of the nuclear factor-kappa B pathway, inhibition of intestinal epithelial cell injury and apoptosis induced by oxidative stress, increase in the intestinal epithelial cell heat shock protein response, inhibition of colonic production of chemoattractant leukotrienes and modulation of prostaglandin metabolism (7). Currently, there is a wide range of formats, and the drug has been formulated as granules and tablets, with different dosing schedules (8-10). Although adherence to treatment is a complex and multifactorial issue, there is a need for improvement strategies aiming to optimize the efficacy of treatment. At present, there is no convincing evidence that there are any meaningful differences between the various delivery systems (10). Sometimes the decision to choose one or the other is based on the personal preferences of both the prescribing doctor and the patient, and the real-life dose used by clinicians is still unknown.
The aim of the present study was to describe how MSZ is used in our practice, at which dose, and the success rate (regarding adherence to therapy) in UC patients.
Methods
Patients
This was an observational, transversal study including all patients with UC undergoing treatment with MSZ maintenance therapy (at least for six months) seen in scheduled outpatient visits between September 2014 and February 2015 at two IBD units in Spain. The diagnosis of UC was according to the Lennard-Jones criteria (11). All participants were asked to sign an informed consent form prior to recruitment. The study was approved by the ethics committee of the steering center.
Epidemiological and clinical data were collected during the patient visit and by review of computerized clinical histories. Next, variables were analyzed from each patient: age, sex, smoking, type of IBD, extent of UC according to the Montreal classification (12), time since diagnosis of UC, comorbidities, MSZ dose and schedules, previous evolution before starting MSZ treatment, concomitant treatment, clinical activity at the time of data collection according to partial Mayo score (13) and treatment adherence measured by the Morisky-Green scale (14) (Fig. 1).
Patients receiving immunosuppressors or biologicals or patients without treatment were excluded. Altered liver function was defined as an increase in transaminases, alkaline phosphatase, gamma-glutamyl transferase or total bilirubin more than twice the upper limit of normal, with other causes ruled out by appropriate serological tests and abdominal ultrasound.
Statistical analysis
Frequencies and percentages with their corresponding 95% confidence intervals were calculated for categorical variables. Regarding quantitative variables, they were shown as mean ± standard deviation or median and interquartile range when the variable did not follow a normal distribution. The Kolmogorov-Smirnov test was used to assess the normality of continuous variables. The comparison between categorical variables was performed using the Chi-squared test. The comparison between quantitative variables and categorical variables of two groups was performed using Student's t test or the Mann-Whitney U test when the variable did not follow a normal distribution. Comparisons between quantitative and qualitative variables with three or more categories were made via the analysis of variance test (ANOVA) or by the nonparametric Kruskal-Wallis. A value of p < 0.05 was considered to be statistically significant.
Results
Baseline characteristics of patients and schedule of treatment with MSZ
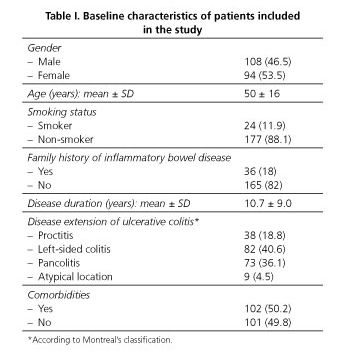
A total of 203 patients with UC were included in the study. Table I describes the baseline characteristics of the patients treated with MSZ included in the present study.
Mean MSZ dose was 2.6 ± 1.0 g/d. The median of time of treatment was 19.5 months (IQR: 8-48). The MSZ doses used were lower than 2 g/d in 15.3% (n = 31) of cases, in 35.0% (n = 71) the dose was from 2 to 2.9 g/d, from 3 to 3.9 in 29.5% (n = 60), and 4 g/d or more in the remaining 20.2% (n = 41). Regarding the dosing schedule, a single daily dose was preferred in 51.2% of cases (n = 104), two doses in 33.0% (n = 67) and three doses in 15.8% (n = 32) (Fig. 2). Patients with MSZ doses distributed several times a day had a longer time of UC evolution from the diagnosis than patients who took a single daily dose (12.7 ± 9.2 vs 8.9 ± 8.6 months; p = 0.003). Moreover, patients who took two or three doses per day had a longer treatment time with MSZ than patients who took MSZ once per day (43.2 ± 48.3 vs 27.9 ± 39.0 months; p = 0.01).
At the time of data collection, 68 (33.5%) patients were on combination with topical MSZ (15 with rectal suspension, 17 with foam and 36 with suppositories).
A different MSZ brand had been previously used in 36.6% of patients. Reasons for change were medical decision (n = 50, 69.4%), side effects (n = 12, 16.7%), patient's choice (n = 8, 11.1%) or poor treatment compliance (n = 2, 2.8%).
Regarding the different galenic formulations of MSZ, the pH-dependent formulation was the most frequently used in our patients (52.6%), followed by the formulations by hydration (34.6%) and the formulation with multi-matrix technology (12.8%). Significant differences in the mean of MSZ depending on the type of formulation used were found. So, patients on treatment with formulations by hydration had lower mean doses of MSZ than patients treated with other formulations (3.1 ± 1.1 g in patients with multi-matrix MSZ vs 2.9 ± 0.9 in patients with formulations pH-dependent vs 2.4 ± 0.9 in release by hydration; p = 0.001). Similarly, the kind of formulation influenced the dosing interval (p < 0.05), the administration of MSZ in a single dose being more frequent in patients with pH-dependent formulations (70%) or multi-matrix (74%) than in patients with hydration formulations (26%).
Evolution of patients on MSZ
Regarding the evolution of the disease and the severity of previous flare-ups, 55.7% of patients had had mild flare-ups (n = 113); 36.5%, moderate flare-ups (n = 74); and 7.9%, severe flare-ups (n = 16). During the year preceding the study, 135 patients were in remission (66.8%), whilst the remaining had suffered at least one flare-up (most of them, 63, had suffered one flare-up and only four patients, two flare-ups or more). In this group of patients, the mean dose of MSZ administered at the time of the flare-up was 2.4 ± 0.9 g/day. No significant differences were observed compared to the group of patients with no flare-ups in the previous year (2.4 ± 0.8 g). At the time of the data collection, the mean MSZ dose in patients who were in remission compared to those who had a flare-up in the previous year was 2.4 ± 0.8 vs 3.2 ± 1.0 g/day, respectively; p = 0.045. Almost half of patients (n = 31) who suffered a flare-up in the year preceding the study required oral corticosteroids to control the disease and 24 needed topical and oral MSZ on combination. The remaining cases were treated with topical (n = 3) or oral MSZ alone (n = 4) or with intravenous corticosteroids (n = 5).
In 134 cases (66%), the maintenance dose had been increased sometime during a flare-up, and in 49 this higher dose had been kept for maintenance (36.6% of cases). The maintenance dose was ≥ 4 g/d in 36 patients. On the other hand, in the remaining 85 patients, the dose was lowered after a period of time (to 2 g/d in 37 patients and to 3g/d in 25 patients). Patients with flare-ups in the previous year maintained more frequently the higher dose of MSZ compared with patients without recent flare-ups (51% vs 27% of patients that maintained higher dose, respectively; p = 0.003).
During the MSZ therapy, 20 patients were admitted (9.9%) and 29 took drug holidays, in the majority of cases (n = 26) due to patient's request after a prolonged remission (mean time without treatment 29.5 ± 40.0 months). Globally, 14 patients (6.9%) had suffered mild side effects with the current MSZ. The most frequent adverse events were altered liver function tests (21.4%) followed by dyspepsia (14.3%). Others observed adverse events are shown in table II. In any case the adverse event forced the withdrawal of the treatment with the current MSZ.
At the time of data collection, 26 patients (12.9%) had clinical activity according to partial Mayo score (22 patients with mild activity, three with moderate activity and one with severe activity) and additional determination (C-reactive protein or calprotectine). There was no difference in the mean of MSZ dose in patients with and without UC activity (2.9 ± 1.2 vs 2.7 ± 1.8 g per day, respectively; p = 0.47).
Adherence of MSZ treatment
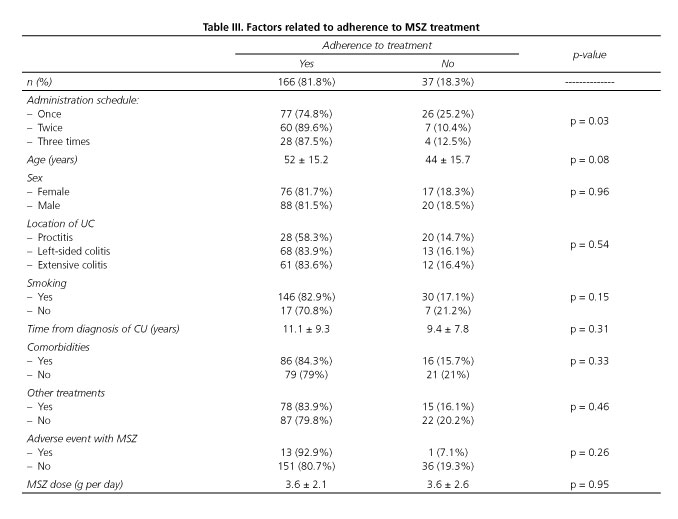
Globally, therapy adherence was good in 81.8% of cases. Only 11.4% of patients had forgotten to take their medicine ever, 10.9% had not been careful about taking their medicine, 6.5% had stopped taking their medicines when feeling better and 2%, when feeling worse. The schedule of MSZ intake influenced adherence to therapy significantly (Table III). Twice daily administration of MSZ improved the adherence to treatment (89.6% of adherence) compared to patients who took one (74.8%) or three daily doses (87.5%) of the medication with MSZ (p = 0.03). Also, age was related to adherence, in such a way that older patients had a tendency to better adhere than younger subjects (52 ± 15.2 years vs 44 ± 15.7 years; p = 0.08). On the other hand, differences according to sex (p = 0.96), UC location (p = 0.54), time of UC evolution (9.4 ± 7.8 years in patients with bad adherence vs 11.1 ± 9.3 years in patients with good adherence), smoking status (p = 0.15), presence of comorbidities (p = 0.33) or different treatments used for other diseases (p = 0.46) were not found (Table II). Differences in therapy adherence were found when an adverse event occurred (p = 0.26) or based on the different MSZ dosages (3.6 ± 2.6 g/d in patients with bad adherence vs 3.6 ± 2.1 g/d in patients with good adherence).
Adherence to treatment was not different according to the different types of galenic formulations. The highest rate of adherence was obtained in the group of patients with pH-dependent formulations (85.5% adherence), followed by formulations by hydration (81.9%) and multi-matrix technology (68.2%, p > 0.05).
Discussion
Following the most recent guidelines about the maintenance treatment in patients with UC, the minimum effective dose of oral 5-ASA is 1.2 g per day (10). In our study almost half of our UC patients take high MSZ doses (≥ 3 g/d) as maintenance therapy. In fact, the global mean of MSZ is close to 3 g per day, even in the group of patients without activity at the time of data collection. The meaning of these results is that the MSZ dose used in real life is clearly higher than the minimum effective dose recommended in guidelines. Previous studies have compared the efficacy of different doses of MSZ. Recently, Pica et al. observed that a daily dose of 4.8 g oral MSZ in UC patients younger than 40 years and/or with extensive disease increased rates and duration of remission compared to 2.4 g (15). Another study found a tendency of a better efficacy of 3 g/day compared with 1.5 g/day (p = 0.051) (16). Paoluzi et al. did not find differences in the relapse rate after one year on 1.2 g/day MSZ compared to 2.4 g/day (17). However, patients on the higher dose were in remission for longer than patients in the other group (175 days in remission vs 129 days, p < 0.001). They also found that the rate of remission was different according the previous disease evolution (17). So, in patients with frequent relapses (more than three relapses per year) 2.4 g/day was better than 1.2 g/day (17). In our study, almost 40% of patients had suffered one flare-up or more (the majority of them were mild flare-ups) the year preceding the study and almost the same percentage increased the MSZ dose sometime during a flare-up when under MSZ therapy, and kept this dose for maintenance. So, this fact could explain the high mean dose obtained, trying to avoid new flare-ups.
Regarding treatment schedule, the current guidelines suggest that once-daily administration of 5-ASA has been proven to be at least as effective as twice- or three-time-daily administration, with no increase of side effects (10). In a previous clinical trial developed by Lichtenstein et al., authors observed that the percentage of relapse-free patients at month 6/end of treatment was higher in patients taking MSZ compared to placebo (78.9% vs 58.3%, p < 0.001) (18). The authors concluded that once-daily MSZ was effective in maintaining remission of UC for six months. Other authors have also observed that once-daily dose of mesalamine is as effective and safe as multiple daily doses for the induction and maintenance treatment of mild to moderate UC (8,9,19). Taking into account that once-daily dosing with 5-ASA is as effective as multiple doses it would be advisable to instruct patients to take a single daily dose to ease the treatment better than several administrations per day. In our study, we observed that patients' features are different according to treatment schedule, in such a way that patients who take MSZ in a single dose have a shorter time of UC evolution and shorter time of treatment with MSZ than patients who took two or three doses per day. Despite this fact, more than half of our patients already take MSZ in one daily administration and it seems that this treatment regimen is taking hold in clinical practice; there is still a substantial number of patients who continue taking several doses following recommendations given in other sites or prescriptions given long time ago.
Current guidelines suggest that extensive UC of mild-moderate activity should initially be treated with oral 5-ASA > 2 g/day, which should be combined with topical MSZ to increase remission rates if tolerated (10). Systemic corticosteroids are appropriate if symptoms of active colitis do not respond to MSZ. In the present study, almost half of patients (46.3%) who suffered a flare-up in the year preceding the study required oral corticosteroids to control the disease, and 35.8% needed topical and oral MSZ in combination. Patients who suffered a flare-up did not have lower basal doses of MSZ. Regarding changes in MSZ dosage, in our study, 66% of patients increased the maintenance dose sometime during a flare-up, and in one third of them this higher dose (≥ 4 g/d in most of the cases) was kept for maintenance. This would explain why the mean dose of MSZ was significantly higher in patients who had had at least one flare-up in the previous year compared to patients who were in remission at the time of data collection. Results obtained in ASCEND I/II trials indicated that 4.8 g/day MSZ provides statistically significant higher rates of mucosal healing and sigmoidoscopic improvement within a 6-week period when compared with a 2.4 g/day dosing regimen in patients with moderately active UC (20-22). Takeshima et al. conducted a multicenter retrospective study to investigate the efficacy of continuous maintenance treatment with 4.0 g/day of MSZ (23). Patients receiving acute induction therapy with 4.0 g/day MSZ were enrolled and followed up. Those who improved clinically or achieved clinical remission were categorized into two sub-groups according to the median duration of treatment with 4.0 g/day of MSZ (a short-term treatment group (≤ 105 days, n = 58) and a long-term treatment group(> 105 days, n = 57). Long-term continuous treatment with high-dose MSZ (4.0 g/day) was more effective (relapse-free rate higher and mean time to relapse longer) than short-term treatment for maintenance of remission in UC patients (23). In a recent study (MOMENTUM Trial), patients achieving complete remission with a multimatrix MSZ 4.8 g/day once daily for eight weeks and then beginning dose reduction were more likely to remain in remission at month 12 than patients who began maintenance in partial remission (24). In our study, patients with flare-ups in the previous year more frequently maintained the higher dose of MSZ compared with patients without recent flare-ups (51% vs 27%, respectively). Increasing the dose of MSZ seems to be a good strategy before a therapeutic step-up to other medications, but the dose should be modified individually according to effectiveness and previous evolution of UC.
There are several formulations of oral MSZ available in our country primarily differentiated by the mechanism of MSZ delivery to the colon. There are formulations released by hydration, formulations with a pH-dependent mechanism of action and formulations with a multi-matrix basis. Regarding overall efficacy of the different formulations, it has been described in the literature that there are no significant differences, and the main differences are found in the dosage (3). In our study we evaluated how the MSZ is used in our clinical practice but we did not perform a prospective follow-up to assess the efficacy of such treatment. We found that patients on treatment with formulations by hydration have lower mean doses than patients with other formulations. We also found that the kind of formulation influenced the interval of administration, the administration in a single dose being more frequent in patients with pH-dependent formulations or multi-matrix than in patients with formulations by hydration.
MSZ intolerance is not very common; it has been described that it occurs in up to 15% of patients. In the clinical trial developed by Lichtenstein et al., the incidence of adverse events was similar between groups, MSZ and a placebo group. Diarrhea (3%), headache (2%), nausea (2%), rash (1%) and thrombocytopenia (1%) have been reported in different studies (25-27). In our study, adverse effects were infrequent (7% of patients developed an adverse event during treatment with the current MSZ), and they did not limit further treatments, even though in some cases it was necessary to change to other formulations of MSZ. The adverse events described in our study were heterogeneous, wherein alteration of liver function tests (three cases) and dyspepsia (two cases) were the most frequently observed. Recently, Suzuki et al., in a multicenter, double-blind, randomized study, found that the incidence of adverse drug reactions was 14.5% in the 3.6 g/day group, and 20.0% in the 4.8 g/day group. They also described two cases (3.6%) of abnormal liver function test in the 4.8 g/d group (28). Previous meta-analyses have reported gastrointestinal symptoms in patients undergoing treatment with 5-ASA (26,29). Particularly, the most recently published studies aimed at describing the safety of MSZ have reported digestive symptoms as the most frequent adverse event, after headaches, obtaining similar percentages in both the mesalazine granule patient group and the placebo patient group (diarrhea 7.9% and 7.0% and abdominal pain 6.3% and 6.5%, respectively) (30). Thus, the results from the present study were in accordance with those of previous reports. Nephrotoxicity related to MSZ is still under debate. Some authors have found that renal impairment in IBD patients may be caused by MSZ, and this treatment-related nephrotoxicity seems to occur most often within the first 12 months of treatment (31,32). However, in our study no patients developed nephrotoxicity related to MSZ treatment. The results obtained highlight MSZ as a treatment with a sound safety and acceptability profile.
Adherence and compliance are directly related to therapeutic success. Our group demonstrated in a previous study that adherence to therapy in inflammatory bowel disease patients was not satisfactory, and worse in patients treated with MSZ. The survey identified dosing three or more times a day (OR 3; 95%CI: 1.1-8.4; p = 0.03) and feeling ill informed about their disease (OR 4.9; 95%CI: 1.1-23.8; p = 0.04) (33) as risk factors for a lower adherence. In that study we concluded that optimizing the information on the disease and adjusting dosing schedules could enhance therapeutic adherence. In the present study the global therapy adherence was good but the group of patients that took twice-daily doses of MSZ still had a better adherence than patients who took it once, which is a reflection of the need for new tools aimed to improve adherence even more in our patients. In addition to treatment complexity and the physician-patient relationship, disease and patient characteristics may affect the adherence to chronic treatments. Coenen et al. recently identified predictors of low adherence in patients with inflammatory bowel disease. They found that being aged younger than 40 years (odds ratio: 1.589 [95% confidence interval: 1.057-2.389], p = 0.026) and a higher educational level (1.961 [1.305-2.946], p = 0.001) were predictors of low adherence (34). These data are in concordance with our results; in the current study we found a trend to better adherence in older patients than younger subjects (52 ± 15.2 years vs 44 ± 15.7 years; p = 0.08). Implementation of strategies to improve medication adherence such as mobile applications could be useful tools in the group of younger patients (35). Regarding the influence that different formulations of MSZ have on the adherence to treatment, it has been described that formulations with more drug might have a better compliance and adherence to treatment (3). In our study, by contrast, we did not find adherence to treatment to be different among the different formulations.
Most of the cases of MSZ withdrawal were due to a patient request after a long time without symptoms. It is necessary to consider that the fact of being free of symptoms may be a risk factor for poor adherence to treatment (36,37). Therefore, it is preferable to reach a consensual agreement with the patient to withdraw the treatment rather than a unilateral and uncontrolled withdrawal on their own initiative.
Finally, our study has some limitations, such as the cross-sectional design without a prospective follow-up of the patients. However, the number of patients included is greater when compared to previous experience. Also, adherence to treatment was determined by an indirect method; in this case it would be better controlled by two different methods.
Conclusions
In our setting, half of our UC patients take high MSZ doses (≥ 3 g/d) as maintenance therapy, with acceptable safety and good adherence. Variable doses are used in clinical practice, highlighting the need to tailor doses according to UC behavior. Half of all patients take a single daily dose and one third needed a different commercial brand during therapy. Opting for a higher MSZ maintenance dose is a possible strategy for a satisfactory maintenance therapy. In spite of all the results obtained, the maintenance dose of MSZ must be individualized depending on the patient characteristics and UC evolution, including previous response to treatments and frequency of flare-ups.
Acknowledgments
We thank MONTERO TRADUCCIONES for kindly reviewing the English used in this paper.
References
1. Monstad I, Hovde O, Solberg IC, et al. Clinical course and prognosis in ulcerative colitis: Results from population-based and observational studies. Annals Gastroenterol 2014;27(2):95-104. [ Links ]
2. Jess T, Riis L, Vind I, et al. Changes in clinical characteristics, course, and prognosis of inflammatory bowel disease during the last 5 decades: A population-based study from Copenhagen, Denmark. Inflamm Bow Dis. 2007;13(4):481-9. DOI: 10.1002/ibd.20036. [ Links ]
3. Manosa M, Domenech E. Mesalazine old and new. Gastroenterol y Hepatol 2011;34(Suppl 3):25-9. [ Links ]
4. Grinspan A, Kornbluth A. Positioning therapy for ulcerative colitis. Curr Gastroenterol Rep 2015;17(8):29. DOI: 10.1007/s11894-015-0454-0. [ Links ]
5. Chaparro M, Gisbert JP. Maintenance therapy options for ulcerative colitis. Expert Opin Pharmacother 2016:1-11. DOI: 10.1080/ 14656566.2016.1187132. [ Links ]
6. Wang Y, Parker CE, Bhanji T, et al. Oral 5-aminosalicylic acid for induction of remission in ulcerative colitis. Cochrane Database Syst Rev 2016;4:CD000543. [ Links ]
7. Desreumaux P, Ghosh S. Review article: mode of action and delivery of 5-aminosalicylic acid - new evidence. Alimentary pharmacology & therapeutics. 2006;24 Suppl 1:2-9. DOI: 10.1111/j.1365-2036.2006.03069.x. [ Links ]
8. Bohm SK, Kruis W. Long-term efficacy and safety of once-daily mesalazine granules for the treatment of active ulcerative colitis. Clin and Experiment Gastroenterol 2014;7:369-83. [ Links ]
9. Gordon GL, Zakko S, Murthy U, et al. Once-daily mesalamine formulation for maintenance of remission in ulcerative colitis: A randomized, placebo-controlled clinical trial. J Clin Gastroenterol 2015. DOI: 10.1097/MCG.0000000000000414. [ Links ]
10. Dignass A, Lindsay JO, Sturm A, et al. Second European evidence-based consensus on the diagnosis and management of ulcerative colitis part 2: Current management. J Crohn's Colitis 2012;6(10):991-1030. DOI: 10.1016/j.crohns.2012.09.002. [ Links ]
11. Lennard-Jones JE. Classification of inflammatory bowel disease. Scand J Gastroenterol Suppl 1989;170:2-6;discussion 16-9. DOI: 10.3109/00365528909091339. [ Links ]
12. Silverberg MS, Satsangi J, Ahmad T, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: Report of a Working Party of the 2005 Montreal World Congress of Gastroenterology. Can J Gastroenterol 2005;19(Suppl A):5A-36A. DOI: 10.1155/2005/269076. [ Links ]
13. Schroeder KW, Tremaine WJ, Ilstrup DM. Coated oral 5-aminosalicylic acid therapy for mildly to moderately active ulcerative colitis. A randomized study. N Eng J Med 1987;317(26):1625-9. DOI: 10.1056/NEJM198712243172603. [ Links ]
14. Morisky DE, Green LW, Levine DM. Concurrent and predictive validity of a self-reported measure of medication adherence. Med Care 1986;24(1):67-74. DOI: 10.1097/00005650-198601000-00007. [ Links ]
15. Pica R, Cassieri C, Cocco A, et al. A randomized trial comparing 4.8 vs. 2.4 g/day of oral mesalazine for maintenance of remission in ulcerative colitis. Dig Liver Dis 2015;47(11):933-7. DOI: 10.1016/j.dld.2015.07.011. [ Links ]
16. Fockens P, Mulder CJ, Tytgat GN, et al. Comparison of the efficacy and safety of 1.5 compared with 3.0 g oral slow-release mesalazine (Pentasa) in the maintenance treatment of ulcerative colitis. Dutch Pentasa Study Group. Eur J Gastroenterol Hepatol 1995;7(11):1025-30. DOI: 10.1097/00042737-199511000-00003. [ Links ]
17. Paoluzi OA, Iacopini F, Pica R, et al. Comparison of two different daily dosages (2.4 vs. 1.2 g) of oral mesalazine in maintenance of remission in ulcerative colitis patients: 1-year follow-up study. Alim Pharmacol Therap 2005;21(9):1111-9. DOI: 10.1111/j.1365-2036. 2005.02458.x. [ Links ]
18. Lichtenstein GR, Gordon GL, Zakko S, et al. Clinical trial: Once-daily mesalamine granules for maintenance of remission of ulcerative colitis - A 6-month placebo-controlled trial. Alim Pharmacol Therap 2010;32(8):990-9. DOI: 10.1111/j.1365-2036.2010.04438.x. [ Links ]
19. Li W, Zhang ZM, Jiang XL. Once daily versus multiple daily mesalamine therapy for mild to moderate ulcerative colitis: A meta-analysis. Colorectal Dis 2016. DOI: 10.1111/codi.13393. [ Links ]
20. Hanauer SB, Sandborn WJ, Dallaire C, et al. Delayed-release oral mesalamine 4.8 g/day (800 mg tablets) compared to 2.4 g/day (400 mg tablets) for the treatment of mildly to moderately active ulcerative colitis: The ASCEND I trial. Can J Gastroenterol2007;21(12):827-34. DOI: 10.1155/2007/862917. [ Links ]
21. Hanauer SB, Sandborn WJ, Kornbluth A, et al. Delayed-release oral mesalamine at 4.8 g/day (800 mg tablet) for the treatment of moderately active ulcerative colitis: The ASCEND II trial. Am J Gastroenterol 2005;100(11):2478-85. DOI: 10.1111/j.1572-0241.2005. 00248.x. [ Links ]
22. Lichtenstein GR, Ramsey D, Rubin DT. Randomised clinical trial: Delayed-release oral mesalazine 4.8 g/day vs. 2.4 g/day in endoscopic mucosal healing - ASCEND I and II combined analysis. Alim Pharmacol Therap 2011;33(6):672-8. DOI: 10.1111/j.1365-2036. 2010.04575.x. [ Links ]
23. Takeshima F, Matsumura M, Makiyama K, et al. Efficacy of long-term 4.0 g/day mesalazine (Pentasa) for maintenance therapy in ulcerative colitis. Med Sci Monit 2014;20:1314-8. DOI: 10.12659/MSM.890567. [ Links ]
24. Rubin DT, Bradette M, Gabalec L, et al. Ulcerative colitis remission status after induction with mesalazine predicts maintenance outcomes: The MOMENTUM trial. J Crohn's Colitis 2016. DOI: 10.1093/ecco-jcc/jjw049. [ Links ]
25. Klotz U, Maier K, Fischer C, et al. Therapeutic efficacy of sulfasalazine and its metabolites in patients with ulcerative colitis and Crohn's disease. N Eng J Med 1980;303(26):1499-502. DOI: 10.1056/NEJM198012253032602. [ Links ]
26. Feagan BG, Macdonald JK. Oral 5-aminosalicylic acid for induction of remission in ulcerative colitis. Cochrane Database Syst Rev 2012;10:CD000543. [ Links ]
27. Loftus EV, Jr., Kane SV, Bjorkman D. Systematic review: Short-term adverse effects of 5-aminosalicylic acid agents in the treatment of ulcerative colitis. Alim Pharmacol Therap 2004;19(2):179-89. DOI: 10.1111/j.0269-2813.2004.01827.x. [ Links ]
28. Suzuki Y, Iida M, Ito H, et al. Efficacy and safety of two pH-dependent-release mesalamine doses in moderately active ulcerative colitis: A multicenter, randomized, double-blind, parallel-group study. Intest Res 2016;14(1):50-9. DOI: 10.5217/ir.2016.14.1.50. [ Links ]
29. Ford AC, Khan KJ, Sandborn WJ, et al. Once-daily dosing vs. conventional dosing schedule of mesalamine and relapse of quiescent ulcerative colitis: Systematic review and meta-analysis. Am J Gastroenterol 2011;106(12):2070-7;quiz 8. DOI: 10.1038/ajg.2011.296. [ Links ]
30. Zakko SF, Gordon GL, Murthy U, et al. Once-daily mesalamine granules for maintaining remission of ulcerative colitis: Pooled analysis of efficacy, safety, and prognostic factors. Postgr Med 2016. DOI: 10.1080/00325481.2016.1152876. [ Links ]
31. Van Staa TP, Travis S, Leufkens HG, et al. 5-aminosalicylic acids and the risk of renal disease: A large British epidemiologic study. Gastroenterol 2004;126(7):1733-9. DOI: 10.1053/j.gastro.2004.03.016. [ Links ]
32. Gisbert JP, González-Lama Y, Mate J. 5-Aminosalicylates and renal function in inflammatory bowel disease: A systematic review. Inflamma Bowel Dis 2007;13(5):629-38. DOI: 10.1002/ibd.20099. [ Links ]
33. Bermejo F, López-Sanromán A, Algaba A, et al. Factors that modify therapy adherence in patients with inflammatory bowel disease. J Crohn's Colitis. 2010;4(4):422-6. DOI: 10.1016/j.crohns.2010. 01.005. [ Links ]
34. Coenen S, Weyts E, Ballet V, et al. Identifying predictors of low adherence in patients with inflammatory bowel disease. Eur J Gastroenterol Hepatol 2016;28(5):503-7. DOI: 10.1097/MEG.0000000000000570. [ Links ]
35. Haase J, Farris KB, Dorsch MP. Mobile applications to improve medication adherence. Telemed J E Health 2016. DOI: 10.1089/tmj. 2015.0227. [ Links ]
36. López-Sanromán A, Bermejo F. Review article: How to control and improve adherence to therapy in inflammatory bowel disease. Alim Pharmacol Therap 2006;24(Suppl 3):45-9. DOI: 10.1111/j.1365-2036. 2006.03060.x. [ Links ]
37. Robinson A. Review article: Improving adherence to medication in patients with inflammatory bowel disease. Alim Pharmacology Therap 2008;27(Suppl 1):9-14. DOI: 10.1111/j.1365-2036.2008. 03604.x. [ Links ]
![]() Correspondence:
Correspondence:
Alicia Algaba.
Department of Gastroenterology.
Hospital Universitario de Fuenlabrada.
C/ Camino del Molino, 2.
28942 Fuenlabrada, Madrid. Spain
e-mail: alicia_algaba@hotmail.com
Received: 20-09-2016
Accepted: 05-11-2016