Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.109 no.3 Madrid mar. 2017
https://dx.doi.org/10.17235/reed.2017.4565/2016
ORIGINAL PAPERS
Post-ERCP pancreatitis: early precut or pancreatic duct stent? A multicenter, randomized-controlled trial and cost-effectiveness analysis
Pancreatitis post-CPRE: ¿precorte temprano o prótesis pancreática? Ensayo aleatorizado, multicéntrico y análisis de costo-efectividad
Hui Jer Hwang1, Martín Guidi1, Cecilia Curvale1, Juan Lasa2 and Raúl Matano1
1Hospital de Alta Complejidad El Cruce. Buenos Aires, Argentina.
2Hospital Nacional Dr. Alejandro Posadas. Buenos Aires, Argentina
ABSTRACT
Background: Pancreatitis is the most frequent complication due to ERCP. Pancreatic duct stent placement has been described as a preventive measure. There is also evidence pointing towards the preventive effect that early precut may provide.
Aim: To determine and compare the cost-effectiveness of an early precut approach versus pancreatic duct stent placement for the prevention of post-ERCP pancreatitis.
Methods: This was a multicenter, randomized-controlled pilot study with a cost-effectiveness analysis performed between early precut (group A) and pancreatic duct stent (group B) for the prevention of pancreatitis in high-risk patients. Patients with a difficult biliary cannulation and at least one other risk factor for post-ERCP pancreatitis were enrolled and randomized to one of the treatment arms. Both effectiveness and costs of the procedures and their complications were analyzed and compared.
Results: From November 2011 to November 2013, 101 patients were enrolled; 50 subjects were assigned to group A and 51 to group B. There were no significant differences in terms of baseline characteristics of patients between groups. Two cases of mild pancreatitis were observed in each group. The overall costs were U$ 1,242.6 per patient in group A and U$ 1,606.5 per patient in group B. The cost in group B was 29.3% higher (p < 0.0001).
Conclusion: Early precut showed a better cost-effectiveness profile when compared to pancreatic duct stent placement.
Key words: Early precut. Pancreatic duct stent. Post-ERCP pancreatitis. ERCP. Precut. Post-ERCP complications.
RESUMEN
Introducción: la pancreatitis es la complicación más frecuente de la colangiopancreatografía retrógrada endoscópica (CPRE). La colocación de una prótesis pancreática es una medida preventiva. Hay evidencias, también, sobre el efecto protector que tendría la realización de un precorte temprano en los casos con canulación difícil.
Objetivo: determinar y comparar el coste-efectividad entre la realización de precorte temprano y colocación de una prótesis pancreática en la prevención de pancreatitis post-CPRE.
Métodos: estudio piloto, prospectivo, aleatorizado, multicéntrico y análisis de coste-efectividad entre precorte temprano (grupo A) y prótesis pancreática (grupo B) en la prevención de pancreatitis en pacientes de alto riesgo. Se incluyeron pacientes con canulación biliar dificultosa y otros factores de riesgo de pancreatitis. Se analizaron la efectividad y el coste de los procedimientos y sus complicaciones.
Resultados: durante dos años se incluyeron 101 pacientes y se aleatorizaron 50 sujetos en el grupo de precorte y 51 sujetos en el grupo de prótesis. No hubo diferencias en las características demográficas de los participantes ni en las indicaciones del estudio. Se registraron dos pancreatitis leves en cada grupo. El coste fue de 1.242,6$ por paciente en el grupo A y 1.606,5$ por paciente en el grupo B. El coste del grupo B fue un 29,3% mayor (p < 0,0001).
Conclusiones: el precorte temprano es más coste-eficaz que la prótesis pancreática en la prevención de pancreatitis post-CPRE.
Palabras clave: Precorte temprano. Prótesis pancreática. Pancreatitis post-CPRE. CPRE. Precorte. Complicaciones post-CPRE.
Introduction
Pancreatitis is the most common adverse event after an endoscopic retrograde cholangiopancreatography (ERCP). Its incidence varies between 1-7% and can reach values of up to 25% in high-risk patient groups. The vast majority of post-ERCP pancreatitis (PEP) are mild or moderate; however, 1-5% of patients may develop severe pancreatitis which may result in prolonged hospitalization and the need for endoscopic or surgical procedures (1-4).
There have been several lines of investigation related to PEP prevention. There are several pharmacologic agents that were tested for this purpose, most of them showing disappointing results, except for rectal indomethacin or diclofenac (5). On the other hand, pancreatic duct stent deployment during ERCP in high-risk subjects has been proposed as an effective prophylactic measure (6-11). A meta-analysis published by Mazaki et al. in 2014 included 14 randomized-controlled trials and observed a significant reduction of PEP incidence (RR = 0.39 [0.29-0.53]) in favor of pancreatic duct stent placement among high-risk subjects (patients with sphincter of Oddi dysfunction, difficult biliary cannulation, pancreatic sphincterotomy, precut sphincterotomy, sphincteroplasty or endoscopic ampullectomy) (12). A cost-effectiveness analysis of pancreatic duct stent placement regarding prevention of PEP showed that this approach exhibited a good cost-effectiveness profile only when considering high-risk patients (13).
Patients with difficult biliary cannulation constitute a group with a significant risk for the development of PEP. Difficulties in biliary cannulation can occur in up to 5 to 15% of ERCPs. Precut sphincterotomy is a technique that can be used in this endoscopic scenario, but has been associated with a non-negligible incidence of adverse events (16,17). Some authors suggest that the complications following precut sphincterotomy (especially PEP) may be due to papillary trauma as a result of multiple attempts to cannulate the biliary duct or due to the involuntary cannulation of the pancreatic duct (18). This raised the hypothesis that early precut may even act as a potential prophylactic measure against PEP in patients with a difficult biliary cannulation (17,19,20). Cennamo et al. published a meta-analysis of randomized-controlled trials comparing both successful cannulation incidence as well as complication incidence between early precut and persistence in biliary cannulation with a standard technique. Six studies were included, and pooled analysis showed a successful cannulation rate of 90% in both groups, but with a significantly lower risk of PEP in the early precut group (OR = 0.47 [0.24-0.91]) (21).
To our knowledge, there is only one published trial comparing early precut versus pancreatic duct stent placement as PEP prophylactic measures (22). This trial showed that early precut was non-inferior to pancreatic duct stent for this purpose. There are no published studies assessing the comparative cost-effectiveness of both techniques in high-risk patients presenting with difficult biliary cannulation. Hence, we sought to determine the cost-effectiveness of the aforementioned techniques in the setting of high-risk patients undergoing ERCP with difficult biliary cannulation.
Material and methods
Design
This was a multicenter, prospective, randomized-controlled pilot study, with cost-effectiveness analysis comparing the use of the early precut technique versus pancreatic duct stent placement for the prevention of PEP in high-risk subjects with a difficult biliary cannulation.
Enrolled patients were randomized into the following treatment arms:
- Group A: early precut sphincterotomy.
- Group B: pancreatic duct stent placement (with or without precut).
Study population
This study was undertaken in two public tertiary referral centers in the Buenos Aires metropolitan area between November 2011 and November 2013.
Inclusion criteria were age > 18 years and difficult biliary cannulation, with at least one of the following PEP risk factors: female gender, age < 40 years, clinical suspicion of sphincter of Oddi dysfunction, history of previous acute pancreatitis and/or non-dilated common bile duct (< 8 mm).
Patients with previous sphincterotomy, coagulation disorders, altered bilio-pancreatic anatomy or those unavailable for further follow up were excluded.
Difficult biliary cannulation was defined as the impossibility to cannulate the common bile duct after eight minutes, or guidewired-cannulation of the main pancreatic duct at least twice or contrast injection into the main pancreatic duct.
Early precut sphincterotomy was performed immediately after randomization. Late precut was performed after eight minutes of attempting a biliary cannulation. All the enrolled subjects signed an informed consent. The study protocol was approved by the Ethics Committees at both institutions and all investigators were committed to follow the Ethics recommendations described in the Declaration of Helsinki of 1975 (reviewed in 2013).
Procedure description
ERCP
This procedure was performed by expert endoscopists with adequate experience (> 300 ERCPs/year). Fujinon© Therapeutic duodenoscopes were used (4.2 mm channel, Series 450) (Fujifilm Corporation Latin America) as well as Pentax® duodenoscopes (Pentax America, New Jersey, USA). Patients were sedated using fentanil, propofol and succinicoline; orotracheal intubation was used in every case.
Selective biliary cannulation was attempted by means of a sphyncterotome (Tritome PC Triple Lumen, Cook, Indiana, USA) using the guide-wire technique (Jagwire Straight Tip, Boston Scientific, Boston, Massachusetts, USA). If eligibility criteria were fulfilled, patients were randomized during the ERCP into one of the following treatment arms:
- Group A: early precut sphincterotomy was performed. The endoscopist in each case chose the most appropriate precut technique to be performed: septotomy, infundibulotomy, standard precut.
- Group B: a 5-7 Fr pancreatic stent, 3 to 5 cm long and with internal flaps or a pigtail with internal flap, was placed with or without late precut.
Sphyncterotomies as well as precut sphyncterotomies were performed with an electrosurgical source (Emed ES 350) using pure cut mode at 50 W. Precut sphyncterotomies were performed with Microknife XL Triple Lumen (Boston Scientific, Massachussetts, USA).
Follow up
After the ERCP procedure, patients were admitted to the hospital for 24 hours. After discharge, they were controlled in the outpatient clinic or by telephone contact a week later. Those patients with pancreatic duct stent placement were evaluated with abdominal x-rays to check for stent migration. In case of stent persistence, these would be endoscopically removed.
Adverse effects
Post-ERCP pancreatitis: this was defined as the occurrence of intense and continuous abdominal pain, with an increase in amylase levels > 3 times the normal upper limit value during the first 24 hours after the procedure, and/or pancreatic swelling with glandular enlargement as observed by an adequate imaging test (23,24).
Post-ERCP bleeding: this was defined as the presence of melena with or without hemodynamic compromise, or the decrease in the value of hemoglobin by at least 2 g/dl, or the need for red blood cell transfusion after the procedure.
Perforation: this was defined as the presence of pneumoperitoneum or retropneumoperitoneum by an adequate imaging test with the accompanying clinical presentation.
The severity of these adverse events are further described in table I.
Cost analysis
For this variable the following aspects were estimated: cost of ERCP, number of necessary interventions, length of hospital stay, pancreatic duct stent costs, as well the costs related to outpatient clinic assessment, x-rays and the eventual endoscopic extraction of stents. Table II describes the aforementioned costs. It is worth mentioning that in our healthcare system, the costs related to ERCP with anesthesia support include all the necessary materials for the procedure except for metallic or plastic stents and balloons.
Sample size estimation
According to previously published data in PEP high-risk patients, we estimated a projected PEP incidence of 10% in the pancreatic stent group and 30% in the early precut group. Considering an alpha error of less than 5% and a beta error of less than 20%, 120 patients (60 patients per treatment arm) would be sufficient to detect the above-mentioned difference.
Randomization
A centrally-generated, computer based simple randomization was performed. This was done by means of the Research Randomizer software. The randomization list was uploaded to the web so that it was readily available for the allocation of patients at both institutions.
Statistical analysis
Epi Info (version 3.1.2) was used for statistical analysis. Categorical variables were compared using the Chi-squared test or Fisher's test, when appropriate. Student's t-test or Mann-Whitney test were used for the comparison of numerical parametric and non-parametric variables, respectively; 95% confidence intervals were estimated. A p value of less than 0.05 was considered as statistically significant.
Results
From November 2011 to November 2013, 1,498 ERCPs were performed. We initially screened 131 patients who fulfilled the inclusion criteria, but only 101 patients signed the informed consent and, consequently, were enrolled in the study. Fifty patients were randomized to the early precut group and 51 to the pancreatic duct stent group. There were no significant differences in terms of demographic features, reason for referral or PEP risk factors between groups, as seen in table III.
ERCP procedure
Successful biliary cannulation was achieved in 98% (49/50) of patients from group A and in 96% (49/51) of patients from group B. The three patients in which initial biliary cannulation was not achieved were subject to a subsequent endoscopic intervention that proved to be successful in every case. The latter procedures were also contemplated in the overall costs of each group. All the enrolled patients had their biliary condition resolved endoscopically. There were no significant differences in terms of the therapeutic interventions needed between groups (biliary stent deployment, sphyncteroplasty, biliary stone retrieval).
Adverse events.There were two cases of PEP in each group, all of them mild and each of them required two days of admission (OR 1.02 [0.13-7.54]). There were two cases of post-ERCP bleeding in group A: one of them responded after adrenaline injection (1:20,000) without the need for further hospital admission and the other one ceased spontaneously. There were two perforations in group A, both of them related to the therapeutic approach of biliary stenosis. Although these perforations were not directly related to the precut procedure, we included the costs derived from the care of such cases in our cost-effectiveness analyses.
Cost-effectiveness analysis
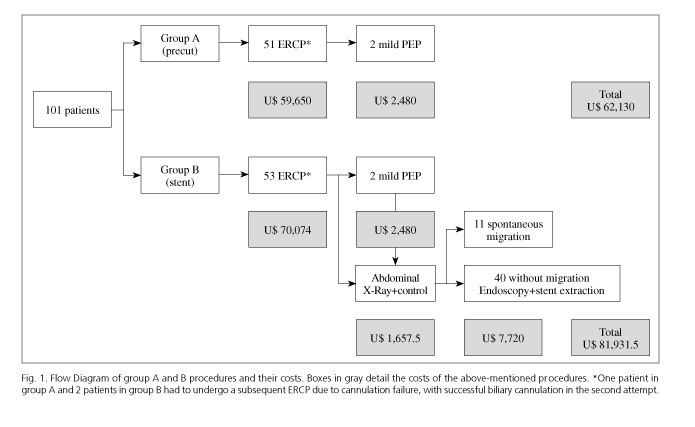
The cost of the endoscopic procedures in group A (early precut) was U$ 59,650. In addition, the cost of the two admissions due to mild PEP was U$ 2,480. Hence, the overall costs in group A was U$ 62,130 (U$ 1,242.6 per patient). This estimation does not include the cost related to the cases of biliary perforations mentioned previously: if this was included, then the cost of admission (U$ 8,680 for both patients), antibiotic therapy (U$ 252 for both patients) and CT scans (U$ 717.3 for both patients) would give a final cost of U$ 71,775.3 (U$ 1,435.5 per patient).
The cost of endoscopic procedures in group B, including pancreatic duct stent placement, was U$ 70,074. Additionally, the cost of the two hospital admissions due to mild PEP was U$ 2,480. Furthermore, the cost associated with outpatient follow up and radiological confirmation of stent dislodgement plus endoscopic retrieval of pancreatic stents in 40 patients was U$ 7,720 (11 patients had spontaneous stent migration). The overall cost in group B was U$ 81,931.5 (U$s 1,606.5 per patient).
The comparison of the overall costs between groups showed a significant difference (p < 0.0001); the cost implicated in group B was 29.3% higher when compared to group A, without considering the cost of the medical care of the patients with perforations. If the latter were included, the difference was still significantly different: the cost implicated in group B was an 11.9% higher than the cost implicated in group A (p < 0.0001)
Discussion
The hypothesis that PEP in patients with a difficult biliary cannulation in which precut sphyncterotomy is used could actually be caused by the papillary edema due to the numerous attempts of cannulation was proposed by the study published by Zagalsky et al. (22). This study actually suggests that early precut is not inferior to what is considered to be the "gold-standard" in terms of PEP prophylaxis, that is to say pancreatic duct stent placement. Based on these findings, our study aimed to analyze both approaches for high-risk patients from a cost-effectiveness point of view.
The relatively low incidence of PEP in the population studied (4% vs 3.96%), even though they were patients with risk factors for PEP, highlights the importance of a rapid approach to biliary cannulation, which results in less papillary damage and thus behaves as a prophylactic measure itself.
The meta-analysis published by Cennamo et al. shows that an early precut strategy when facing a possible difficult biliary cannulation could reduce PEP incidence. It is very likely that the trauma originated due to the persistence of cannulation by a conventional method and the number of involuntary cannulations, or even contrast injections in the pancreatic duct, could be responsible for the increased risk of PEP (19).
On the other hand, Mazaki et al. published a meta-analysis assessing the efficacy of pancreatic duct stent placement for the prevention of PEP; they found a pooled relative risk of 0.39 (0.29-0.53), which shows that this technique is effective as a preventive measure against PEP, especially in high-risk patients (12).
In the study published by Das et al., the authors suggest that this approach has a good cost-effectiveness profile when considering patients with a high risk of developing PEP.
Our study compared an early precut approach versus pancreatic duct stent in high-risk patients; we found no significant differences in the incidence of PEP. Additionally, although no differences were found in terms of preventive efficacy among high-risk patients, we found significant differences in the costs of each approach.
To our knowledge, this is the first cost-effectiveness study comparing both techniques. In the pancreatic duct stent group the higher costs can be explained by the inherent costs of the pancreatic stents, the follow up to check if spontaneous dislodgement of the stent has occurred and the endoscopic procedures for stent retrieval. It is worth mentioning that in the early precut group, two perforations occurred that did not have a direct association with precut sphincterotomy; even so, if the costs generated by the medical treatment of such complications (hospital admission, antibiotic therapy, CT scans) are also included in the analysis, early precut is still a more suitable approach from a cost-effectiveness perspective.
The limitations should be mentioned. First of all, the relatively small sample size of enrolled patients may underestimate the true incidence of complications; however, there is no tendency towards any difference between both approaches. On the other hand, the costs of procedures, materials and hospital admissions were based on the references provided by public hospitals; significant differences may exist if we consider private hospitals' costs. It is important to stress that this was a multicenter, randomized controlled trial in a high-risk population.
In conclusion, both early precut and pancreatic duct stent placement seem to behave in a similar way as preventive measures against PEP in high-risk patients with a difficult biliary cannulation. However, the pancreatic duct stent placement approach implicated a 29% increased cost when compared to early precut.
References
1. Cotton PB, Garrow DA, Gallagher J, et al. Risk factors for complications after ERCP: A multivariate analysis of 11,497 procedures over 12 years. Gastrointest Endosc 2009;70:80-8. DOI: 10.1016/j.gie.2008.10.039. [ Links ]
2. Loperfido S, Angelini G, Benedetti G, et al. Major early complications from diagnostic and therapeutic ERCP: A prospective multicenter study. Gastrointest Endosc 1998;48:1-10. DOI: 10.1016/S0016-5107(98)70121-X. [ Links ]
3. Masci E, Toti G, Mariani A, et al. Complications of diagnostic and therapeutic ERCP: A prospective multicenter study. Am J Gastroenterol 2001;96:417-23. DOI: 10.1111/j.1572-0241.2001.03594.x. [ Links ]
4. Vandervoot J, Soetikno RM, Tham TC, et al. Risk factors for complications after performance of ERCP. Gastrointest Endosc 2002;56:652-6. DOI: 10.1016/S0016-5107(02)70112-0. [ Links ]
5. Elmunzer BJ, Scheiman JM, Lehman GA, et al. A randomized trial of rectal indomethacin to prevent post-ERCP pancreatitis. N Engl J Med 2012;366:1414-22. DOI: 10.1056/NEJMoa1111103. [ Links ]
6. Fazel A, Quadri A, Catalano MF, et al. Does a pancreatic duct stent prevent post-ERCP pancreatitis? A prospective randomized study. Gastrointest Endosc 2003;57:291-4. DOI: 10.1067/mge.2003.124. [ Links ]
7. Smithline A, Silverman W, Rogers D, et al. Effect of prophylactic main pancreatic duct stenting on the incidence of biliary endoscopic sphincterotomy induced pancreatitis in high-risk patients. Gastrointest Endosc 1993;39:652-7. DOI: 10.1016/S0016-5107(93)70217-5. [ Links ]
8. Sofuni A, Maguchi H, Itoi T, et al. Prophylaxis of post-ERCP pancreatitis by an endoscopic pancreatic spontaneus dislodgement stent. Clin Gastroenterol Hepatol 2007;5:1339-46. DOI: 10.1016/j.cgh.2007.07.008. [ Links ]
9. Tarnasky PR, Palesch YY, Cunningham JT, et al. Pancreatic stenting prevents pancreatitis after biliary sphincterotomy in patients with sphincter of Oddi dysfunction. Gastroenterology 1998;115:1518-24. DOI: 10.1016/S0016-5085(98)70031-9. [ Links ]
10. Ito K, Fujita N, Noda Y, et al. Can pancreatic duct stenting prevent post-ERCP pancreatitis in patients who undergo pancreatic duct guidewire placement for achieving selective biliary cannulation? A prospective randomized controlled trial. J Gastroenterol 2010;45:1183-91. DOI: 10.1007/s00535-010-0268-7. [ Links ]
11. Sofuni A, Maguchi H, Mukai T, et al. Endoscopic pancreatic duct stents reduce the incidence of post-ERCP pancreatitis in high-risk patients. Clin Gastroenterol Hepatol 2011;9:851-8. DOI: 10.1016/j.cgh.2011.06.033. [ Links ]
12. Mazaki T, Mado K, Masuda H, et al. Prophylactic pancreatic stent placement and post-ERCP pancreatitis: An updated meta-analysis. J Gastroenterol 2014;49:343-55. DOI: 10.1007/s00535-013-0806-1. [ Links ]
13. Das A, Singh P, Sivak M, et al. Pancreatic stent placement for prevention of post-ERCP pancreatitis: A cost-effectiveness analysis. Gastrointest Endosc 2007;65:960-8. DOI: 10.1016/j.gie.2006.07.031. [ Links ]
14. Freeman ML, Guda NM. ERCP cannulation: A review of reported techniques. Gastrointest Endosc 2005;61:112-25. DOI: 10.1016/S0016-5107(04)02463-0. [ Links ]
15. Shakoor T, Geenen JE. Pre-cut papillotomy. Gastrointest Endosc 1992;38:623-7. DOI: 10.1016/S0016-5107(92)70537-9. [ Links ]
16. Larkin CJ, Huibregtse K. Precut sphincterotomy: Indications, pitfalls, and complications. Curr Gastroenterol Rep 2001;3:147-53. DOI: 10.1007/s11894-001-0012-9. [ Links ]
17. Tang SJ, Haber GB, Kortan P, et al. Precut papillotomy versus persistence in difficult biliary cannulation: A prospective randomized trial. Endoscopy 2005;37:58-65. DOI: 10.1055/s-2004-826077. [ Links ]
18. Sriram PV, Rao GV, Nageshwar RD. The precut: when, where and how? A review. Endoscopy 2003;35:S24-S30. [ Links ]
19. Cennamo V, Fuccio L, Repici A, et al. Timing of precut procedure does not influence success rate and complications of ERCP procedure: A prospective randomized comparative study. Gastrointest Endosc 2009;69:473-9. DOI: 10.1016/j.gie.2008.09.037. [ Links ]
20. De Weerth A, Seitz U, Zhong y, et al. Primary precutting versus conventional over-the-wire sphincterotomy for bile duct access: A prospective randomized study. Endoscopy 2006;38:1235-40. DOI: 10.1055/s-2006-944962. [ Links ]
21. Cennamo V, Fuccio L, Zagari RM, et al. Can early precut implementation reduce ERCP related complication risk? Meta-analysis of randomized controlled trials. Endoscopy 2010;42:381-8. DOI: 10.1055/s-0029-1243992. [ Links ]
22. Zagalsky D, Guidi M, Curvale C, et al. Early precut is as efficient as pancreatic stent in preventing post-ERCP pancreatitis in high-risk subjects: A randomized study. Rev Esp Enferm Dig 2016;108(9):558-62. [ Links ]
23. Cotton PB, Lehman G, Vennes J, et al. Endoscopic sphincterotomy complications and their management: An attempt at consensus. Gastrointest Endosc 1991;37:383-93. DOI: 10.1016/S0016-5107(91)70740-2. [ Links ]
24. ASGE Standards of Practice Committee. Complications of ERCP. Gastrointest Endosc 2012;75(3):467-73. [ Links ]
![]() Correspondence:
Correspondence:
Cecilia Curvale.
Hospital de Alta Complejidad El Cruce.
Av. Calchaquí 5401, Florencio Varela.
Buenos Aires, Argentina
e-mail: cecicurvale@hotmail.com
Received: 26-08-2016
Accepted: 22-12-2016











 texto en
texto en