Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.109 no.8 Madrid ago. 2017
https://dx.doi.org/10.17235/reed.2017.4851/2017
Adult gastric duplication: an unknown condition within the spectrum of gastric submucosal lesions
La duplicación gástrica en el adulto: una entidad desconocida dentro del espectro de lesiones submucosas gástricas
Yurena Caballero-Díaz1, Macarena Centeno-Haro2, Ángel Turégano-García1 and Juan Ramón Hernández-Hernández1
Services of 1General Surgery and Digestive Diseases, and 2Anatomic Pathology. Complejo Hospitalario Universitario Insular-Materno Infantil de Gran Canaria. Las Palmas de Gran Canaria, Spain
ABSTRACT
Background: Gastric duplication is an uncommon condition in adults representing only 4-8% of all gastrointestinal duplications. It develops as a cystic growth within the thick gastric wall that is surrounded by a layer of smooth muscle and lined with gastric mucosa. It is usually asymptomatic but may present with nonspecific abdominal symptoms as well as cyst-related complications such as gastrointestinal (GI) bleeding, ulceration and even pancreatitis. They are difficult to distinguish from other gastric submucosal lesions and may also mimic a gastrointestinal tumor (GIST) or mucinous cyst of the pancreas. Endoscopic ultrasound (EUS) is the most widely used diagnostic procedure and histology provides a definitive diagnosis.
Case report: We report the case of a 36-year-old female patient with a history of a "contained" perforated gastric ulcer that was managed conservatively. The patient was diagnosed with a gastric GIST which prompted a laparoscopic subtotal gastrectomy and Roux-en-Y reconstruction with a good postoperative outcome.
Discussion: The definitive histological diagnosis was gastric duplication. Thus, the previous diagnosis of a "contained" perforated gastric ulcer was in fact a complication of the gastric duplication itself.
Key words: Gastric duplication. Stomach. Submucosal tumors. Gastrointestinal stromal tumor. Mucinous pancreatic cyst.
RESUMEN
Introducción: La duplicación gástrica es una entidad poco frecuente en el adulto que supone solo el 4-8% del total de las duplicaciones gastrointestinales. Consiste en una tumoración quística en el espesor de la pared gástrica rodeada de capa muscular lisa y revestida por mucosa gástrica. Suele ser asintomática, pudiendo presentar síntomas abdominales inespecíficos, así como complicaciones del propio quiste como hemorragias digestivas, úlceras e incluso episodios de pancreatitis. Son difíciles de diferenciar del resto de lesiones submucosas gástricas, ya que pueden simular una tumoración gastrointestinal (GIST) e incluso un quiste mucinoso pancreático. La ecografía endoscópica destaca como método diagnóstico, sin embargo, el diagnóstico definitivo es histológico.
Caso clínico: Presentamos el caso de una paciente mujer de 36 años de edad con antecedentes de un episodio de úlcera gástrica perforada "contenida" que fue manejado de forma conservadora. En la actualidad es diagnosticada de un GIST gástrico, motivo por el cual es intervenida y se le realiza una gastrectomía subtotal laparoscópica con reconstrucción en Y de Roux con buena evolución postoperatoria.
Discusión: El diagnóstico histológico definitivo informa de una duplicación gástrica, por lo que el antecedente de úlcera gástrica perforada "contenida" presentado por la paciente se corresponde con una complicación de la propia duplicación gástrica.
Palabras clave: Duplicación gástrica. Estómago. Tumores submucosos. Tumor del estroma gastrointestinal. Quistes mucinosos pancreáticos.
Introduction
Gastric duplication is a rare congenital malformation representing only 4% of gastrointestinal (GI) tract duplications. It develops as a cystic tumor within the gastric wall surrounded by a smooth muscle layer and lined with gastric mucosa, although it may also contain ectopic duodenal or pancreatic mucosa (1,2). It is considered as a rare condition in adults. The lesion is usually asymptomatic and difficult to distinguish from other submucosal growths. Thus, it is often mistaken for a GI stromal tumor or a mucinous pancreatic tumor. We report the case of a 36-year-old female patient with a history of a gastric ulcer who was subsequently diagnosed with a gastrointestinal stromal tumor (GIST) after work-up for dyspepsia. After surgery the patient received a definitive histological diagnosis of a gastric duplication.
Case report
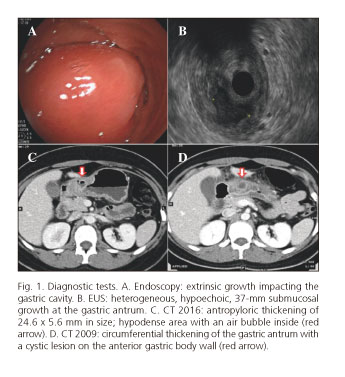
A 36-year-old female patient with an unremarkable history underwent an upper GI endoscopy for epigastric abdominal pain and dyspepsia in 2004, which revealed a gastric antral ulcer with no signs of complication. In 2009, the patient presented to the Emergency Room with severe abdominal pain and no other associated symptoms and a perforation of a previously identified ulcer was found on CT scan. This was managed conservatively with a favorable clinical outcome (Fig. 1D). She subsequently complained of dyspepsia and a follow-up upper GI endoscopy revealed an extrinsic growth at the gastric antrum-lesser curvature level (Fig. 1A) that bulged into the gastric cavity. An abdominal CT scan showed a thickened, 5.6 cm-long antropyloric wall segment at 24.6 mm with an air bubble inside (Fig. 1C). An endoscopic ultrasound (EUS) study plus fine-needle aspiration puncture (FNAP) was performed, showing a submucosa-dependent antral lesion of 37 mm in length (Fig. 1B). FNAP revealed GI cells and some fusiform cells that may have derived from the gastric muscular layer or a benign lesion such as leiomyoma or GIST without atypia or mitotic activity. The case was discussed during a specialist tumor committee meeting and surgery was scheduled due to the patient's history and the potential GIST-like nature of the lesion.
A laparoscopic subtotal gastrectomy with Roux-en-Y reconstruction was performed. The patient had a favorable postoperative course, she tolerated liquids on the third day and was discharged from hospital on the sixth day after surgery.
The pathology analysis described a subtotal gastrectomy specimen 14 x 6 x 3 cm in size with no gross changes either externally or after opening the specimen. Serial slices of the specimen revealed a cystic cavity 0.8 cm in diameter within the gastric wall, with mucinous-looking contents. Microscopically, the gastric mucosa exhibited normal characteristics and a cystic cavity lined with normal gastric mucosa was found within the wall with a well delimited muscular wall and focal pancreatic metaplasia. These findings were consistent with gastric duplication (Fig. 2).
Discussion
Gastrointestinal tract duplications are defined as cystic structures adjacent to a GI segment (1,2). The ileum is the most commonly involved site (35%), followed by the jejunum, colon and stomach in only 2-9% of cases (2). It is considered as a congenital malformation that is identified in over 70% of cases in patients younger than 12 years of age. Diagnosis of this lesion is rare during adulthood.
Patients are usually asymptomatic or have vague abdominal symptoms, and this condition is often detected as an incidental finding. The presence of ectopic gastric, duodenal or pancreatic tissue is characteristic and clinically significant as it may result in complications such as upper GI bleeding, ulcer and episodes of pancreatitis (2). In rare cases it may become malignant and mainly develops into adenocarcinoma. Most are isolated from the lumen of the GI tract and 50% are associated with other congenital abnormalities (pancreatic duplications, ectopic or annular pancreas) or spinal disorders (spina bifida) (3). Pancreas related abnormalities reflect the common embryonic origin of the pancreas and stomach.
The etiopathogenesis remains unknown. The condition is thought to originate from the dorsal aspect of the primitive gut tube during development. Thus, most cases involve the greater curvature of the stomach (4) and only 5.5% are located at the lesser curvature. These duplications develop before the epithelium differentiates into the several types present in adults, and are thus designated according to the associated organ. Multiple theories exist, of which three are of interest: a) persistence of a vacuole or diverticulum during bowel development; b) failed fusion of longitudinal gastric folds resulting in an epithelial bridge; and c) traction diverticulum formation from anomalous endodermal and notochordal development (5).
Most cases reported in adults are preoperatively diagnosed as GISTs or mucinous pancreatic cysts (4) with a definitive diagnosis achieved by the histological examination of the surgical specimen. This suggests a lack of awareness with regard to this condition, particularly from the radiographic and echoendoscopic perspectives. Contrast-enhanced CT shows cystic growths with thick walls near the stomach with inner layer enhancement. These radiographic features are similar to those of mucinous pancreatic cysts, which makes an accurate diagnosis difficult. Magnetic resonance imaging does not improve identification and both imaging techniques are estimated to yield an incorrect diagnosis in up to 43-70% of cases.
EUS is highly advisable for the characterization of gastric submucosal lesions. This technique is key for the identification of these lesions as cyst type and location can be defined. FNAP can be performed for the differential diagnosis from other submucosal lesions and it informs about potential malignant sites (5-7). The lesion is observed as an anechoic round or ovoid image lined with a thin echogenic layer and surrounded by a hypoechogenic muscle layer, giving the impression of a "double wall" or a "muscular rim" (8,9).
Diagnosis requires histological confirmation according to the Rowling's criteria: the cyst wall should be contiguous with the gastric wall and the lesion must be surrounded by smooth muscle in continuity with the gastric muscle and lined with gastric, epithelial or intestinal mucosa (5).
There is no standard treatment. Symptomatic or complicated cases should be treated surgically. However, no consensus exists with regard to asymptomatic patients. Some researchers consider that these patients only require follow-up while others advocate for surgery after diagnosis, regardless of symptoms, as there is a risk for malignancy or complications (5). Enucleation and endoscopic submucosal resection have been reported (10), but complete excision is recommended, as in this case.
This rare congenital malformation in an adult is a lesson to be learned as it is an uncommon condition initially diagnosed as a simple perforated ulcer and, subsequently, as a gastric submucosal mass. The contained perforated ulcer event the patient experienced in 2009 may have been a complication of the gastric duplication itself. In conclusion, we consider that gastric duplication should be included in the differential diagnosis of gastric submucosal growths, where EUS plays a key role for preoperative diagnosis. These lesions should be surgically removed once diagnosed due to the risk of complications or malignization. A minimally invasive surgical approach is the most appropriate approach in these cases.
References
1. Geng YH, Wang CX, Li JT, et al. Gastric foregut cystic developmental malformation: Case series and literature review. World J Gastroenterol 2015;21:432-8. DOI: 10.3748/wjg.v21.i2.432. [ Links ]
2. Doepker MP, Ahmad SA. Gastric duplication cyst: A rare entity. J Surg Case Rep 2016;2016(5):rjw073. DOI: 10.1093/jscr/rjw073. [ Links ]
3. Bhatti ZS, Anderson MA, Wasnik AP. Complete gastric duplication in an adult with associated anomalies. Clin Imaging 2016;40:244-6. DOI: 10.1016/j.clinimag.2015.11.016. [ Links ]
4. Yoda T, Furihata M, Nagao S, et al. An adult gastric duplication cyst mimicking a gastrointestinal stromal tumor. Intern Med 2016;55:2401-4. DOI: 10.2169/internalmedicine.55.6402. [ Links ]
5. Seijo Ríos S, Lariño Noia J, Abdulkader Nallib I, et al. Adult gastric duplication cyst: Diagnosis by endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA). Rev Esp Enferm Dig 2008;100:586-90. [ Links ]
6. Eloubeidi MA, Cohn M, Cerfolio RJ, et al. Endoscopic ultrasound-guided fine-needle aspiration in the diagnosis of foregut duplication cysts: the value of demonstrating detached ciliary tufts in cyst fluid. Cancer 2004;102:253-8. DOI: 10.1002/cncr.20369. [ Links ]
7. Varas MJ, Miquel JM, Abad R, et al. Interventionist endoscopic ultrasonography. A retrospective analysis of 60 procedures. Rev Esp Enferm Dig 2007;99:138-44. [ Links ]
8. Landi B1, Palazzo L. The role of endosonography in submucosal tumours. Best Pract Res Clin Gastroenterol 2009;23:679-701. DOI: 10.1016/j.bpg.2009.05.009. [ Links ]
9. Fazel A, Moezardalan K, Varadarajulu S, et al. The utility and the safety of EUS-guided FNA in the evaluation of duplication cysts. Gastrointest Endosc 2005;62:575-80. DOI: 10.1016/j.gie.2005.06.014. [ Links ]
10. Eom JS, Kim GH, Song GA, et al. Gastric duplication cyst removed by endoscopic submucosal dissection. Korean J Gastroenterol 2011;58:346-9. DOI: 10.4166/kjg.2011.58.6.346. [ Links ]
![]() Correspondence:
Correspondence:
Yurena Caballero Díaz.
Service of General Surgery and Digestive Diseases.
Complejo Hospitalario Universitario Insular Materno-Infantil de Gran Canaria.
Av. Marítima del Sur, s/n.
35016 Las Palmas de Gran Canaria, Spain
e-mail: yurenacaballero@hotmail.com
Received: 06-02-2017
Accepted: 03-04-2017











 texto en
texto en