My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista Española de Enfermedades Digestivas
Print version ISSN 1130-0108
Rev. esp. enferm. dig. vol.109 n.10 Madrid Oct. 2017
https://dx.doi.org/10.17235/reed.2017.5120/2017
LETTERS TO THE EDITOR
A patient with Castleman's disease mimicking acute pancreatitis
Key words: Castleman's disease. Giant lymph node hyperplasia. Acute pancreatitis.
Dear Editor,
Castleman's disease is a rare condition that gastroenterologists should be aware of. We present a case of Castleman's disease mimicking acute pancreatitis.
Case report
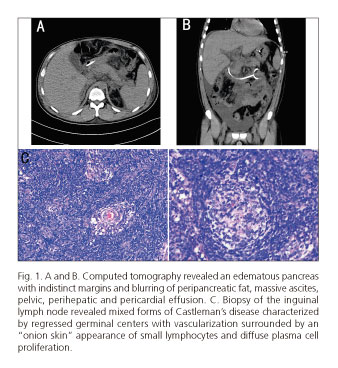
A 34-year-old man presented with epigastric pain, fever and abdominal distention for five days. There was no history of alcohol abuse or drug abuse. Physical examination showed multiple cervical, axillary and inguinal lymphadenopathy. Laboratory tests showed increased levels of inflammatory markers (white cell count of 17.19 × 109/l, 83.1% neutrophils and C-reactive protein of 92 mg/l) and serum amylase was normal. Rheumatologic, infectious and viral tests were all negative. Computed tomography (CT) revealed acute edematous pancreatitis, massive ascites, pelvic, perihepatic and pericardial effusion (Fig. 1A and B). There was no evidence of gallstones and no other underlying etiological factors of acute pancreatitis were detected. The patient was treated with antibiotics. The fever and abdominal pain subsided but the abdominal distention did not improve. An excisional biopsy from the inguinal lymph node revealed mixed forms of Castleman's disease (Fig. 1C). Immunohistochemical analysis showed expression of CD3, CD20, CD21 and CD38. The patient underwent six courses of CHOP chemotherapy. The symptoms disappeared and a repeat CT showed absorption of the above effusion. The patient remains well and there was no recurrence after one year of follow-up.
Discussion
Castleman's disease (CD) is a rare lymphoproliferative disorder and its pathogenesis remains poorly understood (1). On a clinical basis, the disease is separated into uni-centric CD and multi-centric CD, and it is pathologically classified as hyaline vascular variant (HVV), plasma cell variant (PCV) and mixed forms as both HVV and PCV (1,2). CD involving the pancreas is extremely rare and, to date, around 20 cases have been reported. However, almost all these cases presented as a pancreatic mass or tumor, and over half of them were HVV (3,4). To our knowledge, this is the first reported CD case presenting as acute pancreatitis. The acute pancreatitis and multiple effusion in the present case may be attributed to the acute systemic inflammatory reaction caused by excessive proinflammatory hypercytokinemia in the setting of multi-centric CD (5). This case is reminiscent of acute pancreatitis with multiple lymphadenopathy that should raise a suspicion of CD.
Jie Wu, Liang Lv and Chunlian Wang
Department of Gastroenterology.
The Second Xiangya Hospital of Central South University.
Changsha, Hunan. China
References
1. Roca B. Castleman's Disease. A Review. AIDS Rev 2009;11:3-7. [ Links ]
2. Cronin DM, Warnke RA. Castleman disease: An update on classification and the spectrum of associated lesions. Adv Anat Pathol 2009;16:236-46. DOI: 10.1097/PAP.0b013e3181a9d4d3. [ Links ]
3. Fu L, Wang XL, Babu SR, et al. Pancreatic Castleman's disease: Studies of three cases and a cumulative review of the literature. Indian J Surg 2013;75:34-8. DOI: 10.1007/s12262-012-0495-7. [ Links ]
4. Matsumoto T, Okuwaki K, Kida M, et al. A patient with pancreatic Castleman's disease arising around the main pancreatic duct. Intern Med 2015;54:2007-12. DOI: 10.2169/internalmedicine.54.4665. [ Links ]
5. Fajgenbaum DC, Van Rhee F, Nabel CS. HHV-8-negative, idiopathic multicentric Castleman disease: Novel insights into biology, pathogenesis, and therapy. Blood 2014;123:2924-33. DOI: 10.1182/blood-2013-12-545087. [ Links ]