Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Enfermedades Digestivas
versión impresa ISSN 1130-0108
Rev. esp. enferm. dig. vol.110 no.6 Madrid jun. 2018
https://dx.doi.org/10.17235/reed.2018.5355/2017
CASE REPORT
Magnesium poisoning, multi-organ failure and ischemic colitis secondary to chronic ingestion of a parapharmacy product
1Servicio de Medicina Intensiva. Hospital Universitario Central de Asturias. Oviedo. Spain
2Grupo de Microbiología Traslacional ISPA. Instituto Investigación Principado de Asturias. Oviedo. Spain
3Departamento de Medicina. Universidad de Oviedo. Oviedo. Spain
4Grupo de Investigación Traslacional en el paciente crítico ISPA. Instituto Investigación Principado de Asturias. Oviedo, Spain
INTRODUCTION
Hypermagnesemia is defined as a serum magnesium level greater than 1 mmol/l 1. The cause is usually iatrogenic and there is a higher risk associated with elderly patients, chronic renal failure with reduced excretion and gastrointestinal disorders with increased absorption 2,3.
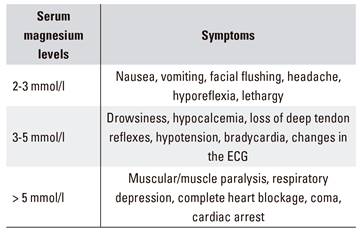
Mild hypermagnesemia can be asymptomatic 4 and symptoms start to appear when the levels are > 2.5 mmol/l 1, as shown in table 1. A relationship has been described between hypermagnesemia and the need for vasopressor drugs, a higher risk of respiratory failure and an increased mortality 5,6,7.
Hypermagnesemia treatment depends on the levels and is based on stopping magnesium administration, increasing the excretion by loop or thiazide diuretics, proper fluid administration and calcium salts to protect the myocardium. Severe cases require renal replacement to decrease magnesium levels to a non-toxic level in a short period of time 1.
CASE REPORT
The case was a 70-year-old woman with a history of mantle cell lymphoma, pudendal neuralgia and painful bladder syndrome treated with opioid and intravesicular botulinum toxin. The last dose was administered ten months prior to being admitted. Furthermore, she had a history of chronic constipation, even before starting opioid treatment, and was taking magnesium in a granulated formulation from a parapharmacy. The product was Magnesium Carbonate(r), which contained 290 mg of magnesium per each gram, and the patient was taking one tablespoon per day. The product label recommended to "dissolve two tablespoons in half a glass of water or juice after meal digestion and before bedtime". There was no other information or cautions in the case of an overdose.
The patient developed vomiting and weakness and was initially treated at home by the extra hospital Emergency Service. She was alert and orientated (Glasgow coma scale of 14 point), with a blood pressure (BP) of 104/57 mmHg and paresis in the four limbs with a muscle strength of 1/5. She also presented areflexia, respiratory failure with tachypnea of 32 breaths/min and an oxygen saturation of 83%. Non-invasive mechanical ventilation was applied with an improvement in oxygen saturation to 98%. During the medical interview, the patient admitted to taking magnesium carbonate as a laxative on a daily basis. Therefore, magnesium intoxication was suspected and treatment with fluids was started at 0.5 mg IV of calcium chloride and 20 mg of furosemide. The patient was transferred to the Emergency Room of her reference hospital and remained hemodynamically unstable (BP 98/64 mmHg) despite fluid administration, and was therefore treated with vasoactive drugs.
The muscular weakness turned into an areflexic tetraplegia that required non-invasive mechanical ventilation support to maintain oxygen saturation and the blood gas analysis within normal values. Serum magnesium levels were 7.35 mmol/l and therefore energic fluid therapy plus 1 g of calcium gluconate was administered. The patient was transferred to the Intensive Care Unit (ICU) and became more hemodynamically unstable (BP 74/37 mmHg) with oligoanuric renal failure and respiratory failure due to the tetraplegia, requiring intubation and invasive mechanical ventilation. Given the severity of the case, hemodiafiltration was performed. Despite a decrease in the serum magnesium level to 4.55 mmol/l after three hours of renal replacement, the shock persisted and noradrenaline at > 1.5 mcg/kg/min was required. The patient had severe metabolic acidosis and lactate levels of 9.7 mmol/l. An echocardiography was performed and there were no relevant findings due to a poor echographic window.
During the first few hours after admission, the patient developed an important abdominal distension with massive diarrhea. An abdominal-pelvic computed tomography (CT) scan identified a severe dilatation affecting the entire colon without signs of intestinal ischemia (Fig. 1). These findings were considered as a toxic megacolon secondary to a magnesium intoxication.
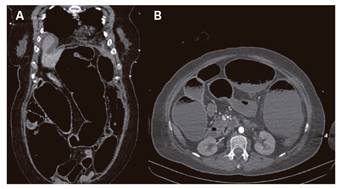
Fig. 1 Abdomino-pelvic CT with contrast in the coronal (A) and axial (B) sections showing a severely dilated colon, fecal and fluid retention without signs of obstruction, pneumatosis or an intestinal loop.
After ten hours of renal replacement, the serum magnesium level dropped to 3.1 mmol/l. The hemodynamic situation progressively improved and the magnesium levels decreased in parallel. The noradrenaline infusion was stopped 72 h after admission. However, abdominal distension and diarrhea persisted, accompanied by a fever of 38.7 °C. New complications were discarded after an abdominal CT scan on the 4th day of the clinical course. Afterwards, clinical improvement continued and extubation was achieved on the 7th day. The patient was discharged from the ICU on the 10th day of the clinical course.
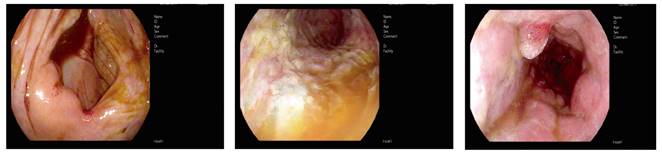
A colonoscopy was performed due to persistent diarrhea that identified signs of ischemic colitis on a 30 cm segment length of the colon (Fig. 2). The abdominal affectation recovered very slowly and hospital discharge was delayed until the 67th day.
DISCUSSION
Magnesium salts are commonly used as osmotic laxatives for patients suffering from chronic constipation 8 and is recommended by both gastroenterology specialists and general practitioners due to it proven efficacy 9. However, they are not always prescribed by health professionals as they are accessible in parapharmacies. A chronic intake of magnesium products with no medical control can lead to severe intoxications that can cause multiple organ failure and death (Table 1) especially in people with the risk factors mentioned previously such as elderly cases, chronic renal failure and gastrointestinal disorders.
In the most severe gastrointestinal manifestations, hypermagnesemia can cause toxic megacolon and ischemic colitis due to an altered intestinal blood flow. This leads to a decrease in bowel motility caused by fecal impactation and an increase in the intraluminal pressure exacerbated by a prolonged hypotension 10, as in this case.
Parapharmacy products are not considered as "drugs" by the consumer. Thus, patients have a false feeling that they can safely take this medication in an uncontrolled manner and do not mention this during the medical interview. Furthermore, the posology information of these products can be ambiguous and does not alert the consumers to the risk of overdose.
This case report highlights the risks of self-medication with parapharmacy products that contain magnesium. Therefore, when intoxication is suspected, this etiology should be considered and assessed via a rigorous medical interview.
BIBLIOGRAFÍA
1. Torregrosa JV, Torres A. Alteraciones del metabolismo del calcio, del fósforo y del magnesio. En: Farreras Rozman. Medicina Interna. XVII Ed. Elsevier España; 2016. pp. 799-807. [ Links ]
2. Kala J, Abudayyeh A. Magnesium: an overlooked electrolyte. J Emerg Med 2017;52(5):741-3. DOI: 10.1016/j.jemermed.2017.01.011 [ Links ]
3. Karahan MA, Kuckuc A, Buyukfirat E, et al. Acute respiratory and renal failure due to hypermagnesemia, induced by counter laxatives in an elderly man. J Clin Diagn Res 2015;9(12):UL01. DOI: 10.7860/JCDR/2015/ 16630.6939 [ Links ]
4. Yoon HE, Kim YW, Ha KS, et al. Hypermagnesemia accompanied with colonic perforation in a hemodialysis patient. Yonsei Med J 2013;54:797-800. DOI: 10.3349/ymj.2013.54.3.797 [ Links ]
5. Onish S, Yoshino S. Cathartic-induced fatal hypermagnesemia in the elderly. Intern Med 2006;45:207-10. DOI: 10.2169/internalmedicine.45.1482 [ Links ]
6. Celi LA, Scott DJ, Lee J, et al. Association of hypermagnesemia and blood pressure in the critically ill. J Hypertens 2013;31:2136-41. DOI: 10.1097/HJH.0b013e3283642f18 [ Links ]
7. Thongprayoon C, Cheungpasitporn W, Srivli N, et al. Admission serum magnesium levels and the risk of acute respiratory failure. Int J Clin Pract 2015;69:1030-8. DOI: 10.1111/ijcp.12696 [ Links ]
8. Cheungpasitporn W, Thongprayoon C, Quian Q. Dysmagnesemia in hospitalized patients: prevalence and prognostic importance. Mayo Clin Poc 2015;90:1001-10. DOI: 10.1016/j.mayocp.2015.04.023 [ Links ]
9. Weng YM, Chen SY, Chen HC, et al. Hypermagnesemia in a constipated female. J Emerg Med 2013;44:57-60. DOI: 10.1016/j.jemermed.2011.09.004 [ Links ]
10. Sugiyama M, Kusumoto E, Ota M, et al. Induction of potentially lethal hypermagnesemia, ischemic colitis, and toxic megacolon by a preoperative mechanical bowel preparation: report of a case. Surg Case Rep 2016:2(1):18. DOI: 10.1186/s40792-016-0145-6 [ Links ]
Received: November 06, 2017; Accepted: February 06, 2018











 texto en
texto en