Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Cirugía Oral y Maxilofacial
versión On-line ISSN 2173-9161versión impresa ISSN 1130-0558
Rev Esp Cirug Oral y Maxilofac vol.29 no.5 Madrid sep./oct. 2007
Mandibular metastases of gastric adenocarcinoma. A case report
Metástasis mandibular de adenocarcinoma gástrico. Presentación de un caso
J. Ferreras Granado1, Á. García-Rozado González1, G. Gómez Oliveira2, I. Vázquez Mahía1, J.L. López-Cedrún Cembranos3
1 Médico Adjunto.
2 Médico Residente.
3 Jefe de Servicio.
Servicio de Cirugía Oral y Maxilofacial. CHU Juan Canalejo. La Coruña, España
ABSTRACT
Malignant tumors of the mouth and jaws represents approximately 5% of all malignant neoplasms in the body, and only 1-4% are considered to be metastatic. They are most frequently located in the mandible (80%), fundamentally in the molar region. Metastases to the jaws are usually from breast, lung, kidney, thyroid gland, intestines, and prostate gland; and less frequently from stomach, testes, and bladder.
They are more frequent in elderly patients (between 4th and 7th decades) with no gender differences.
Treatment is usually palliative and based on the use of radiotherapy, chemotherapy and hormonal therapy. Surgery is only used in selected cases.
A case of mandibular metastases as first sign of malignant disease of gastric adenocarcinoma is reported.
Key words: Mandibular metastases; Gastric adenocarcinoma.
RESUMEN
Los tumores malignos de la cavidad oral y mandíbula representan aproximadamente un 5% de todas las neoplasias malignas del cuerpo, y sólo entre el 1 y el 4% son consideradas como metástasis. Tienen su localización más frecuente a nivel de la mandíbula (80%), fundamentalmente en la región molar. Las metástasis mandibulares, cuando aparecen, suelen tener su origen en tumores primarios que asientan en la mama, pulmón, riñón, tiroides, intestinos y próstata; y con menor frecuencia en el estómago, testículos y vesícula biliar.
Suelen afectar a pacientes de edad avanzada (4ª-7ª décadas de la vida) sin predilección por el sexo.
El tratamiento en general es paliativo y pasa por el uso de la radioterapia, quimioterapia y hormonoterapia, reservando la cirugía para casos aislados. Describimos un caso de metástasis mandibular en un paciente adulto como primera manifestación clínica de un adenocarcinoma gástrico.
Palabras clave: Metástasis mandibular; Adenocarcinoma gástrico.
Introduction
Malignant tumors in the oral cavity and mandible represent approximately 5% of all malignant neoplasms of the body, and only between 1 and 4% are considered to be metastatic.1,2 They are most commonly located in the mandible (80%), fundamentally in the molar region.3,4 The most common origin is from primary tumors that arise in the breast, lung, kidneys, thyroid gland, intestines and prostrate; and to a lesser extent in the stomach, testes and bladder.5-7
They tend to affect the elderly (4th to 7th decades of life) and there are no gender differences,1,6,7 although there are authors that claim that there is a greater incidence in females compared with males.4,5
The most common clinical presentation is of a painful mass that grows relatively rapidly in the mandibular molar region.1,4,5,7 Other less common manifestations include paresthesia of the lower lip, movement or loss of teeth, as well as the presence of intraoral bleeding.8- 10 Bilateral or multicentric involvement has been described in the mandible, although this is exceptional.11 Radiological diagnosis is complicated as there is no pathognomonic appearance and sometimes there will be inexistent radiologic findings. When there are findings, these show a radiolucid image with badly defined margins, although at times, as in the case of breast or prostate metastases, the image can be radiopaque.9,10
The differential diagnosis includes various entities with a radiologic appearance that is similar to osteomyelitis, abscesses and bone cysts, primary malignant bone neoplasms, myelomas or histiocytosis X.1,4
Treatment tends to be palliative and it is based on the use of radiotherapy, chemotherapy and hormonotherapy, 4,12-17while surgery is to be kept for isolated cases.18
Generally it has a bad prognosis with survival after diagnosis of less than a year.4,5,17
Case report
A Caucasian male, 59 years old was sent to our department complaining of a leftsided stabbing pain in the mandibular body as well as hypoesthesia of the lip and chin on the same side, which had been evolving for over a month. The intraoral examination was normal. A radiographic study was carried out that included an orthopantomography and a CAT scan that revealed the presence of an osteolytic lesion that was well-defined, with a diameter of less than 2.5 cm, and which was located in the left ascending ramus of the mandible (Figs. 1 and 2). A biopsy of the lesion was carried out. The histological analysis revealed an image that was compatible with a metastatic adenocarcinoma lesion, probably of the mucosecretory type (Fig. 3). A bone gammagraphy was carried out that revealed hyperuptake in the left ascending ramus of the mandible, left vertebral body by T12, 8th rib on right side and costochondral joint of 6th rib on right side (Fig. 4). The thorasic-abdominal CAT scan revealed a large mass that affected the gastric body and antrum, with regional adenopathy, and a nodule in the upper lobe of the left lung (Fig. 5). Combined radio and chemotherapy was administered. The patient died two months later. The autopsy confirmed the gastric origin of the metastases.
Discussion
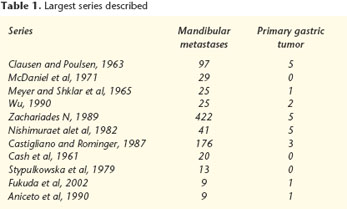
Mandibular metastases are very uncommon. Clausen and Poulsen 3 defined some criteria for judging a mandibular tumor as metastasic or not: 1) The lesion represents a metastasic carcinoma in the bone, and any extension from adjacent soft tissue should be excluded; 2) it should be histologically confirmed; 3) the primary location of the tumor should be identified; and 4) when the primary lesion is anatomically close to the metastasis, direct extension should be ruled out and a wide tumor-free margin around the tumor itself should be identified. These four criteria have not been correctly applied in some cases of mandibular metastasis previously described in the literature,1,4 and the incidence rate as a result could be even lower. The case described in this article meets these four criteria perfectly.
In 1965 Meyer and Shklar studied 2400 cases of carcinoma. Twenty-five were metastases and only in one case was the primary tumor in the stomach.4 Similar results were reported by Zachariades and cols.6 who reviewed 204 publications up until 1989 on metastases in the maxillofacial region, and they found 422 metastatic lesions. Of these, only five had a gastric origin. In a series of 2409 malignant tumors of the oral cavity and mandible, Wu found that only 25 were metastatic and that in only two cases had the primary tumor arisen in the stomach.8 In most of the studies that have been carried out the most common location of metastases in the maxillofacial area is intraosseous,4,6 and the mandible is affected in 61% of cases, and the maxilla in 24%. More than 20% of the metastases cases located in the tongue were detected postmortem during the autopsy, which would suggest that the tongue is affected more than has previously been thought. On the other hand Nishimura and cols., in a revision of the Japanese literature found greater frequency of gingival metastases than bone.5,6
Bone metastases of gastric carcinoma are clinically uncommon findings. However, this probably occurs with greater frequency than has been demonstrated in radiological studies due to complete bone studies not being carried out during autopsies. Between 5 and 11% of bone metastases of gastric adenocarcinoma has been described, arising most commonly in the vertebrae.9 It is very rare for the facial bones to be affected although Hashimoto and cols.10 in a study on autopsies of deceased patients due to gastric carcinomas, found mandibular metastases in 3 cases (25%).
Different hypotheses have been put forwards in an attempt to explain the fact that most of the metastases occur towards the back of the mandible. Thus Hashimoto and cols.10 and Carroll and cols.11 believe that the hematopoietic areas in mandibular bone marrow could favor the early deposit of tumor cells. Holland and cols.12 are of the opinion that this is due to the fact that bone metastases occurs with greater frequency in red bone marrow than in yellow. The type of predominant bone marrow in the mandible is yellow. Red bone marrow cannot be detected in up to 75% of adults, but when it exists it tends to be located in the region behind the incisors. However, this does not explain why most metastases occur in the mandible and not in the maxilla where there is greater medullar bone. In order to explain why some mandibular metastases appear without first affecting the lungs, a description has been made of Batsons plexus that supplies arterial blood to an area that extends from the skull base to the sacrum, and that in Willis´polygon anastomosis occurs with the internal carotid artery, and lung filtration is in this way avoided.6,13
Men and women are affected at the same rate,6 although there is a slight female predominance (52-62%).5 The age at presentation varies between the 4th and the 7th decades in life.3,4,14 Although in general mandibular metastasis on its own is described, it can sometimes be bilateral although this is exceptional.15
The principal clinical signs are the presence of a mass and pain. Other authors8,16 found sensory disturbance of the lower lip, as occurred in this case of ours. In approximately 20-30% of cases metastasis was diagnosed before the primary tumor,4,17,18 and most of these patients died within a year of being diagnosed. There appears to be a difference in the survival times of patients who are diagnosed with metastases before the primary tumor is diagnosed, compared with those whose primary tumor is diagnosed before the metastasis, as the latter have a greater survival rate.17
Palliative treatment should be chosen for this type of patient and this includes radiotherapy, chemotherapy and hormonotherapy,17 surgery is reserved for selected cases, fundamentally when there is no other metastasis or for purely aesthetic reasons.5,18
![]() Correspondence:
Correspondence:
Dr. José Ferreras Granado
CHU Juan Canalejo
Servicio de Cirugía Oral y Maxilofacial
As Xubias de Arriba, 84
15006 La Coruña, España
Email: joseferreras@terra.es
Recibido: 06.02.06
Aceptado: 18.12.06
References
1. McDaniel RK, Luna MA, Stimson PG. Metastatic tumors in the jaws. Oral Surg Oral Med Oral Pathol 1971;31:380-6. [ Links ]
2. Batsakis JG. Tumors of head and neck: clinical and pathologic considerations. 2nd ed. Baltimore: William & Wilkins 1979;240. [ Links ]
3. Clausen F, Poulsen H. Metastatic carcinoma to the jaws. Acta Pathol Microbiol Scand 1963;57:361-74. [ Links ]
4. Meyer I, Shklar G. Malignant tumors metastatic to mouth and jaws. Oral Surg Oral Med Oral Pathol 1965;20:350-62. [ Links ]
5. Nishimura Y, Yakata H, Kawasaki T, y cols. Metastatic tumors of the mouth and jaws: A review of the Japanes literature. J Maxillofac Surg 1982;4:253-8. [ Links ]
6. Zachariades N. Neoplasms metastatic to the mouth, jaws and surrounding tissues. J Craniomaxillofac Surg 1989;17:283-90. [ Links ]
7. Stypulkowska J, Barktkowski S, Pana M, y cols. Metastatic tumors to the jaws and oral cavity. J Oral Surg 1979;37:805-8. [ Links ]
8. Wu YT. Metastatic carcinoma to the oral tissues and jaws: a study of 25 cases. Zhonghua Kou Qiang Yi Xue Za Zhi 1990;25:258-61. [ Links ]
9. Catone GA, Henny FA. Metastatic gastric adenocarcinoma of the mandible: report of a case. J Oral Surg 1969;27:36-40. [ Links ]
10. Hashimoto N, Kurihara K, Yamassaki H, y cols. Pathological characteristics of metastatic carcinoma in the human mandible. J Oral Pathol 1987;16:362-7. [ Links ]
11. Carroll MK, Krolls SO, Mosca NG. Metastatic carcinoma to the mandible. Oral Surg Oral Med Oral Pathol 1993;76:368-74. [ Links ]
12. Holland DJ. Metastatic carcinoma to the mandible. Oral Surg Oral Med Oral Pathol 1953;6:567-72. [ Links ]
13. Wolujewicz MA. Condilar metastasis from a carcinoma of the prostate gland. Br J Oral Surg 1980;18:175-82. [ Links ]
14. Cash CD, Royer RQ, Dahlin DC. Metastatic tumours of the jaws. Oral Surg 1961; 14:897-901. [ Links ]
15. McMillan MD, Edwards JL. Bilateral mandibular metastases. Oral Surg Oral Med Oral Pathol 1975;39:959-66. [ Links ]
16. Rohrer MD, Colyer J. Mental nerve paresthesia: Symptom for a widespread skeletal metastatic adenocarcinoma. J Oral Surg 1981;39:442-5. [ Links ]
17. Fukuda MF, Miyata M, Okabe K, Sakashita H. A case series of 9 tumors metastatic to the oral and maxillofacial region. J Oral Maxillofac Surg 2002;60:942-94. [ Links ]
18. Aniceto GS, Penín AG, de la Mata R, y cols. Tumors metastatic to the mandible: Análisis of nine cases and review to the literature. J Oral Maxillofac Surg 1990; 48:246-51. [ Links ]











 texto en
texto en