Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Farmacia Hospitalaria
versión On-line ISSN 2171-8695versión impresa ISSN 1130-6343
Farm Hosp. vol.40 no.3 Toledo may./jun. 2016
https://dx.doi.org/10.7399/fh.2016.40.3.10060
Hypoglycemic treatment of diabetic patients in the Emergency Department
Tratamiento hipoglucemiante del paciente diabético en el Servicio de Urgencias
Carmen Caballero Requejo1, Elena Urbieta Sanz1, Abel Trujillano Ruiz1, Celia García-Molina Sáez1, María Onteniente Candela1 and Pascual Piñera Salmerón2
1Pharmacy Unit. Hospital General Universitario Reina Sofía de Murcia.
2Emergency Department. Hospital General Universitario Reina Sofía de Murcia. Spain.
ABSTRACT
Objectives: To analyze if the hypoglycemic therapy prescribed in the Emergency Department adapts to the consensus recommendations available, as well as to assess its clinical impact.
Methods: A descriptive observational study, which included patients awaiting hospital admission, who were in the Observation Ward of the Emergency Department and had been previously diagnosed with diabetes mellitus, and were receiving treatment with hypoglycemic drugs at home. The management of antidiabetic treatment and its clinical impact were assessed.
Results: 78 patients were included. At admission to the Emergency Department, treatment was modified for 91% of patients, and omitted for 9%. The most prescribed treatment was sliding scale insulin (68%). The treatments prescribed coincided in a 16.7% with the recommendations by the Spanish Society of Emergency Medicine. After intervention by the Pharmacist, the omission descended to 1.3%, and the adaptation to the recommendations increased to 20.5%. Comparing patients whose treatment coincided with the recommendations and those who did not, the clinical impact was respectively: mean glycemia at 24 hours: 138.3 ± 49.5 mg/dL versus 182.7 ± 97.1 mg/dL (p = 0.688); mean rescues with insulin lispro: ± 1.6 versus 1.5 ± 1.8 (p = 0.293); mean units of insulin lispro administered: 4.6 ± 12.7 IU versus 6.6 ± 11.3 IU (p = 0.155).
Conclusions: We found antidiabetic prescriptions to have a low adaptation to consensus recommendations. These results are in line with other studies, showing an abuse of sliding scale regimen as single hypoglycemic treatment.
Key words: Diabetes mellitus; Emergency Department; Therapeutic reconciliation; Hypoglycemic agents; Insulin.
RESUMEN
Objetivo: Analizar la adecuación del tratamiento hipoglucemiante prescrito en el Servicio de Urgencias a las recomendaciones de consenso disponibles, así como evaluar su repercusión clínica.
Método: Estudio observacional descriptivo. Se incluyeron pacientes que se encontraban en la sala de observación del Servicio de Urgencias pendientes de ingreso hospitalario, con diagnóstico previo de diabetes mellitus y en tratamiento domiciliario con fármacos hipoglucemiantes. Se evaluó el manejo del tratamiento antidiabético y su repercusión clínica.
Resultados: Se incluyeron 78 pacientes. Al ingreso en el Servicio de Urgencias se modificó el tratamiento en el 91% de los pacientes, y se omitió en el 9%, siendo el tratamiento más pautado los rescates con insulina rápida (68%). Los tratamientos prescritos se ajustaron en un 16,7% a las recomendaciones de la Sociedad Española de Medicina de Urgencias y Emergencias. Tras la intervención del farmacéutico, la omisión descendió al 1,3% y la adecuación a las recomendaciones aumentó al 20,5%. Comparando los pacientes cuyo tratamiento se ajustó a las recomendaciones y los que no, la repercusión clínica fue, respectivamente: media de glucemia a las 24 horas 138,3 ± 49,5 mg/dL versus 182,7 ± 97,1 mg/dL (p = 0,688); media de rescates con insulina lispro 1± 1,6 versus 1,5 ± 1,8 (p = 0,293); media de unidades de insulina lispro administradas 4,6 ± 12,7 UI frente a 6,6 ± 11,3 UI (p = 0,155).
Conclusiones: Encontramos una baja adecuación de las prescripciones de antidiabéticos a las recomendaciones de consenso. Estos resultados van en línea con otros estudios, objetivándose un abuso de las pautas de rescate con insulina rápida como único tratamiento hipoglucemiante.
Palabras clave: Diabetes mellitus; Servicio de Urgencias; Conciliación terapéutica; Agentes hipoglucemiantes; Insulina.
Contribution to scientific literature
Diabetic patients represent 30-40% of all patients managed at the Emergency Departments. This study sheds light on the way in which these patients are managed in said hospital units, in terms of their hypoglycaemic treatment. Besides, as hypoglycaemic drugs are considered High Risk Medications, the role of the Pharmacist will become particularly important regarding the adequate preparation of the home medication history (HMH), because the hypoglycaemic treatment indicated during admission will be determined by the previous treatment received by the patient.
Introduction
Diabetes is a chronic and complex condition, which requires continuous medical follow-up with strategies for reduction of multifactorial risks beyond glycaemic control1. Diabetic patients represent 30-40% of all patients managed at Hospital Emergency Departments (ERs), and 25% of hospitalized patients2. In the majority of cases, the cause for admission is not diabetes but another intercurrent disease, and frequently, diabetes will be decompensated when hyperglycaemic management is relegated by prioritizing treatment of the condition which has led to the admission1,3.
It is also known that the hospital stay of patients with diabetes will be 1-3 days longer than that for non-diabetics; and it is more likely that those who present hyperglycaemia at admission will require admission to the Intensive Care Unit2. Different factors favour the development of hyperglycaemia in hospitalized patients, such as stress or diabetes decompensation, the interruption of hypoglycaemic drugs, or the administration of hyperglycaemic agents (glucocorticoids, enteral or parenteral nutrition)1. Currently, literature supports the fact that specific glucose control in the hospital setting will improve clinical outcomes, and there is enough evidence to associate hyperglycaemia in hospitalized patients with worse outcomes4.
However, there is a certain controversy regarding the management of diabetic patients during hospitalization5-12, and lax glycaemia values, of around 140-180 mg/dl, have been currently determined for hospitalized patients1. ERs are essential to guarantee the adequate management of diabetic patients during their hospital stay. Hyperglycaemias are frequent, but systematic care in the Observation Ward of ERs leads to a better glycaemic control in those patients who will be hospitalized afterwards13. On the other hand, there are some factors which have a negative impact on this adequate control: certain tolerability of hyperglycaemia as a safety measure against hypoglycaemia, lack of knowledge or omission of the previous treatment of the patient, and the excessive use of "sliding scales" or regimens with fast-insulin alone.
Protocols of consensus for treatment of hyperglycaemia have not yet been sufficiently implemented in ERs13. Treatment planning in said hospital unit is the key point, because it is very likely that this treatment will be continued during hospital stay, and glycaemia, type of diabetes, and previous treatment must be taken into account in order to initiate it14-18. Clinical inertia can often lead to non-modification of treatment, and this will happen frequently in those patients who are prescribed fast-acting insulin without basal insulin19,20.
A recent study21 has reached the conclusion that there is a major gap between clinical guidelines and the management of glycaemic control in hospitalized patients with diabetes. Overall, there seems to be an abuse of sliding scale insulin, while HbA1c levels are not determined, and less than three glycaemic measurements are conducted per day.
In view of all the previously stated, we decided to evaluate the way in which diabetic patients were being managed at our ER, through which 70% of admissions to our hospital take place. Particularly, our objective was to analyze the adaptation of the hypoglycaemic treatment prescribed at ER with the consensus recommendations currently available, and to assess the clinical impact of a potentially inadequate management of antidiabetic drugs.
Methods
An observational descriptive study for the assessment of patient care practice, conducted at the ER of a hospital of reference, covering a population of 195,000 inhabitants. The timeframe for the study was six months (from December, 2013 to May, 2014). The population studied was formed by >18-year-old patients waiting for admission at the ER Observation Ward, during the Pharmacist's working hours (Monday to Friday, 8 a.m. to 2 p.m.). The medication for those patients selected for the study had been previously reconciled by the ER Pharmacist, and therefore they met the inclusion criteria determined by the Therapeutic Reconciliation Procedure currently applied in the centre22. Said procedure considers those factors associated with a higher risk of error (>65-year-of age, polymedication, multiple conditions), and higher severity in case of error (high risk medications, renal impairment, etc.). The study included all those patients with reconciled medication who had been previously diagnosed with Diabetes Mellitus, and were on home treatment with hypoglycaemic drugs.
For all patients included, and within the Reconciliation Procedure, a home medication history (HMH) was prepared through clinical interview, consulting the Primary Care electronic records (Agora Plus®), and reviewing the medication when provided by patients. All those patients who could not be interviewed personally, or through their caregiver or relative, were excluded from the study. Besides, demographic data were collected, as well as pathologic background, reason for admission, and lab test results based on the electronic clinical records. The Emergency Process Data were also obtained, based on the MBDS (Minimum Basic Data Set) provided by the Documentation Unit.
A first descriptive analysis was conducted of the clinical and pharmacotherapeutical profile of patients, and more in detail regarding the antidiabetic home treatments taken by patients; the frequency of the different therapeutic subgroups was analyzed according to the Anatomical Therapeutic Classification (ATC) by the WHO, and the combinations of antidiabetic drugs used. In order to describe patient management and their treatment at hospital admission, the therapeutic decision implied in each ER prescription was classified into: omission, continuation, or modification of home treatment.
In order to measure the adaptation of the treatment prescribed, the "Protocol for Management of Patients with Diabetes Mellitus at the Emergency Unit" by the Spanish Society of Emergency Medicine (SEMES)23 was selected as reference for this study, after a review of the consensus documents available in the bibliography about management of diabetic patients at hospital admission1,2,3,23. Thus, the prescription made at ER was compared with what was indicated in said protocol, based on the clinical and pharmacological factors therein stated (Figure 1), and the consideration of adaptation or non-adaptation of treatment was determined; this was the primary variable of this study. The same comparison was conducted with the prescription obtained after the Pharmacist intervention during the Reconciliation Procedure, and the time until error resolution was also recorded.
Clinical impact was measured by determining if there was any association between the adaptation to protocol recommendations and those clinical indicators considered more relevant: glycaemia at 24 hours after admission, number of rescues and/or number of insulin units which needed to be administered. The Mann-Whitney U Test was used for this.
For descriptive analysis, frequencies and percentages were estimated in qualitative variables; and mean levels, standard or typical deviations, maximum and minimum values were estimated in quantitative measurements. A statistical significance of 0.05 was used for all analysis, and it was conducted with the SPSS statistical program, version 18.0.
Results
The population of the study was finally formed by 78 patients in total (out of the 132 with reconciled medication), who had been previously diagnosed with diabetes mellitus (97.4% Type 2 diabetes). The mean age was 73.6 ± 9.4, with 55.1% patients over 75-year-of age. Out of these patients, 53.8% were women, and 57.7% presented a Charlson Comorbidity Index (CCI) equal or superior to 3, classified as high comorbidity. The most frequent comorbidity was chronic renal impairment (69.2%), followed by heart failure (39.7%) and chronic pulmonary disease (33.3%). The most frequent diagnoses at admission were associated with the cardiovascular (41%) and the respiratory system (32%). Table 1 shows the main characteristics of the population studied, as well of the Emergency process for these patients.
In total, 1003 prescriptions were recorded for medications in these patients' home treatment, which corresponded to 217 different molecules, with a mean of 12.9 ± 4.1 medications per patient. Out of these, 149 were antidiabetic drugs (14.9%), and with a mean 1.9 ± 0.8. of this type of drugs per patient. The most frequent antihyperglycaemic drug was metformin, present in 56.4% of patients (Table 2). A 64.1% of patients were being treated at home exclusively with oral anti-diabetics (OADs), 14.1% with insulin, and 21.8% with a combination of OADs and insulin, as appears in table 3.
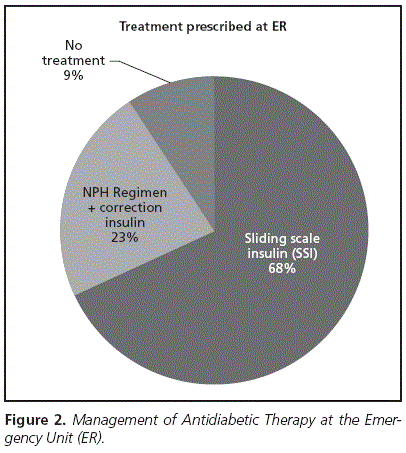
The degree of adaptation to the protocol by the SEMES of the treatments prescribed by Emergency Specialists was 16.7%. Home treatment was not continued in any case at admission to the ER Observation Ward. We found 7 patients whose hypoglycaemic treatment had been omitted (9%), 6 omissions in patients on home treatment with OADs, and 1 omission in a patient on insulin; the cause for said omissions was an incomplete (HMH). The rest of patients (91%) had their treatment modified. Treatments prescribed at ER are shown in figure 2, and the majority consist in sliding scale insulin (68%). All patients on home OADs (except for omissions) were treated with sliding scale insulin; on the other hand, for 60% of the 10 patients on insulin who received treatment, basal insulin was prescribed alongside the rescue regimen, and the remaining 40% only received sliding scale insulin. Finally, we found that out of those patients who were treated at home with a combination of OADs and insulin, 70.6% had been prescribed basal insulin on top of the rescue regimen, while 29.4% had been prescribed a sliding scale insulin exclusively.
The ER pharmacist had an intervention in those 7 patients who had their hypoglycaemic treatment omitted. There was an 85.7% acceptance of this intervention (6 patients). On the other hand, the Pharmacist recommended dose adjustment for NPH insulin in two patients, and this was accepted. The mean time for error resolution was 21.1 ± 12.8 hours. The percentage of patients with antidiabetic treatment omissions went from 9% to 1.3% after the Pharmacist intervention, though adaptation to protocol only improved in 3 patients: from the 16.7% of adaptation in prescriptions by ER specialists to 20.5% after the intervention of the ER pharmacist. Figure 3 shows the level of adaptation to the protocol by the SEMES based on home treatment, before and after the Pharmacist intervention.
Differences were found in the indicators for clinical relevance, but these were not significant in any case. Thus, the outcomes in patients whose treatment adapted to the protocol by the SEMES and in those where it did not, were respectively: glycaemia at 24 hours of admission: 138.3 ± 49.5 mg/dL vs. 182.7 ± 97.1 mg/dL (p = 0.688); mean of rescues with insulin lispro: 1± 1.6 versus 1.5 ± 1.8 (p = 0.293); number of units of insulin lispro administered: 4.6 ± 12.7 IU vs. 6.65 ± 11.3 IU (p = 0.155). It was not possible to confirm glycaemia at 24 hours for 8 patients.
Discussion
The majority of patients included in our study were on home treatment with OADs (85.9%), which means that they needed a treatment modification at admission, given the overall contraindication for the use of these drugs in hospitalized patient24,25. A great adherence to the recommendation to interrupt OADs was detected; however, the level of overall adaptation to the consensus recommendations for prescriptions made at ER was very low (16.7% of treatments), with a slight improvement after the intervention of the Pharmacist for medication reconciliation (20.5%). A high proportion of prescriptions for only sliding scale insulin regimen was mostly detected (68% of prescribed treatments). The Pharmacist prevented omissions, but he/she did not conduct an adequate treatment adjustment in the majority of cases. The highest level of adaptation was for patients who were on home treatment with OADs and insulin (23.5%), and the lowest level was for those on insulin treatment only (9%). This lack of adaptation translated into a trend to an increase in glycaemia at 24 hours after admission, as well as of the number and units of rescue insulin, though the outcomes of our study were not significant. In terms of the high mean time to resolution of the error, this is because Pharmacists only work during morning hours, while the ER admits patients 24 hours round the clock; therefore, a patient might stay for practically 24 hours without any Pharmacist intervention.
Over half of patients were over 75-year-old, with a remarkable degree of comorbidity (57.7% of patients had a CCI > 3) and with a high number of drugs taken at home per patient (12.9 ± 4.1). This is essentially due to the own inclusion criteria in the Reconciliation Procedure (patients >65-year-old, polymedicated, with multiple conditions), which intended to direct this observation towards a population group at higher risk of error in therapeutic reconciliation26. An adequate reconciliation is essential at the time of prescribing an antidiabetic treatment at admission, because the previous treatment of patients must be taken into account, as well as whether they are on insulin or not, the type and number of insulin units administered every day, or if treated with OADs. Insulin is one of the drugs most associated to medication errors in hospitalized patients27.
Comparing our study with the one conducted by Bernard et al. in an ER13 , we find they had lower mean ages (55-year-old), and a higher proportion of patients on insulin treatment at home that in our study (56-62% versus 35.9%). This corresponds with the difference in age and, therefore, with a higher prevalence in our patients of Type 2 diabetes, the treatment of choice being OADs before insulin. There are also differences with the same study regarding the management of antidiabetic treatment at admission. Thus, they observed that only 54% of patients in the control arm were treated with insulin, while 91% of patients in our study were on insulin. We can also observe that 9% of patients continued on OADs, while in our study these were discontinued for 100% of patients; this was, as pointed out before, the recommendation by the protocol of the SEMES that was totally adhered to. In contrast, one of the most important deviations regarding adaptation to recommendations was the high proportion of prescriptions of sliding scale regimen (68%), while this will be only indicated when the patient is taking OADs as chronic treatment, presents clinically stable at admission (glycaemia < 180 mg/dl or HbAlc < 7%), and has been prescribed an oral diet. These results go in line with the studies conducted in hospitalized diabetic patients, and it has been observed that there is an abuse of sliding scale insulin regimen as single hypoglycaemic treatment2,21,28,29.
Regarding the assessment of the clinical impact based on adaptation to protocol, we found limitations in our study due to the potential loss of data: the retrospective design entails the possibility that not all records for rescue insulin administered were complete, and that it was not possible to confirm the glycaemic level at 24 hours, though an estimation was conducted with those data available. The findings were, firstly, that those patients who had not been prescribed treatment adapted to protocol showed a tendency to having a higher number of rescues with insulin lispro, with more units administered, and higher glycaemic values at 24 hours after admission in the ER than the group whose treatment coincided with the protocol, though there were no statistically significant differences, probably due to the limited sample size. However, studies similar to ours have demonstrated that those patients who receive an intensive treatment following protocol will present lower glycaemic values than the control arm13,30.
The main limitation of this study is its observational nature, framed within a Reconciliation Process for patients at risk. The lack of randomization for patients to be included, as well as an estimation of the sample size required before conducting the study, reduces its external validity, and limits the application of study outcomes. However, we consider that the selection of ER is adequate for conducting the study, because it is the main gate of access for patients to hospital; and, in terms of drug therapy, it is characteristic of these units to be recipients and generators of medication iatrogenesis. Besides, the great prevalence of diabetic patients within those selected for therapeutic reconciliation (59% of these patients were diabetic) justifies the in-depth study of this group of patients, particularly taking into account that all antidiabetic drugs are considered High Risk Medications. The role of the Pharmacist will acquire special relevance in terms of the correct preparation of HMH, because the hypoglycaemic treatment indicated during admission will be determined by the previous treatment of the patient, which is essential to learn about accurately.
Finally, the evidence of lack of adherence to recommendations, both by ER Specialists and by the ER Pharmacist in our hospital, has encouraged us to set up a program for training and discussion among the different professionals involved in the management of this type of drugs at hospital admission. In our opinion, it would also be necessary to conduct studies targeted to validate the benefits of adherence to the new consensus protocols for patients admitted to our hospitals, that will allow to draw and generalize conclusions.
The authors declare there is no conflict of interests.
Bibliography
1. American Diabetes Association. Standards of Medical Care in Diabetes 2015. Diabetes Care. 2015; 38(Suppl 1). [ Links ]
2. Pérez Pérez A, Conthe Gutiérrez P, Aguilar Diosdado M, Bertomeu Martínez V, Galdos Anuncibay P, García de Casasola G, et al. Tratamiento de la hiperglucemia en el hospital. Med Clin (Barc). 2009;132(12):465-75. [ Links ]
3. Carreño Hernández MC, Sabán Ruiz J, Fernández Ballesteros A, Bustamante Fermose A, García Polo I, Guillén Camargo V. et al. Manejo del paciente diabético hospitalizado. An Med Interna. 2005;22(7):339-48. [ Links ]
4. Clement S, Braithwaite SS, Magee MF, Ahmann A, Smith EP, Schafer RG, et al. American Diabetes Association Diabetes in Hospitals Writing Committee: Management of diabetes and hyperglycemia in hospitals (Review). Diabetes Care. 2004;27(2):553-91, (errata in Diabetes Care 2004;27(3):856, and Diabetes Care. 2004;27(5):1255). [ Links ]
5. Van den Berghe G, Wouters P, Weekers F,VerwaestC, Bruyninckx F, Schetz M, et al. Intensive insulin therapy in critically ill patients. N Engl J Med. 2001;345(19):1359-67. [ Links ]
6. Malmberg K, Norhammar A, Wedel H, Rydén L. Glycometabolic state at admission: important risk marker of mortality in conventionally treated patients with diabetes mellitus and acute myocardial infarction: long-term results from the Diabetes and Insulin-Glucose Infusion in Acute Myocardial Infarction (DIGAMI) study. Circulation. 1999;99(20):2626-32. [ Links ]
7. Finfer S, Liu B, Chittock DR, Norton R, Myburgh JA, McArthur C, et al. NICE-SUGAR Study Investigators.Hypoglycemia and risk of death in critically ill patients. N Engl J Med.2012;367(12):1108-18. [ Links ]
8. Finfer S, Chittock DR, Su SY, Blair D, Foster D, Dhingra V, et al. NICE-SUGAR Study Investigators. Intensive versus conventional glucose control in critically ill patients. N Engl JMed. 2009;360(13):1283-97. [ Links ]
9. Krinsley JS, Grover A. Severe hypoglycemia in critically ill patients: risk factorsand outcomes. Crit Care Med. 2007;35(10):2262-67. [ Links ]
10. Griesdale DE, de Souza RJ, van Dam RM, Heyland DK, Cook DJ, Malhotra A, et al. Intensive insulin therapy and mortality among critically ill patients: a meta-analysis including NICE-SUGAR study data. CMAJ. 2009;180(8):821-7. [ Links ]
11. Krinsley JS. Effect of an intensive glucose management protocol on the mortality of critically ill adult patients. Mayo Clinic Proc. 2004;79(8):992-1000. [ Links ]
12. Umpierrez GE, Hellman R, Korytkowski MT, Kosiborod M, Maynard GA, Montori VM, et al. Management of hyperglycemia in hospitalized patients in non-critical care setting: an endocrine society clinical practice guideline. J Clin Endocrinol Metab. 2012;97(1):16-38. [ Links ]
13. Bernard JB, Munoz C, Harper J, Muriello M, Rico E, Baldwin D. Treatment ofinpatient hyperglycemia beginning in the emergency department: a randomizedtrial using insulins aspart and detemir compared with usual care. J Hosp Med.2011;6(5):279-84. [ Links ]
14. Umpierrez GE, Palacio A, Smiley D. Sliding scale insulin use: myth or insanity? Am J Med. 2007;120(7):563-7. [ Links ]
15. Braithwaite SS, Clement S. Algorithms for intravenous insulin delivery. Curr Diabetes Rev. 2008;4(3):258-68. [ Links ]
16. Furnary AP, Braithwaite SS. Effects of outcome on in-hospital transition fromintravenous insulin infusion to subcutaneous therapy. Am J Cardiol. 2006;98(4):557-64. [ Links ]
17. Braithwaite SS. The transition from insulin infusions to long-term diabetestherapy: the argument for insulin analogs. SeminThorac-Cardiovasc Surg.2006;18(4):366-78. [ Links ]
18. Leahy JL. Insulin management of diabetic patients on general medical andsurgical floors. Endocr Pract. 2006;12 Suppl 3:86-90. [ Links ]
19. Knecht LA, Gauthier SM, Castro JC, Schmidt RE, Whitaker MD, Zimmerman RS, et al. Diabetes care in the hospital: is there clinical Inertia? J Hosp Med.2006;1(3):151-60. [ Links ]
20. Cook CB, Castro JC, Schmidt RE, Gauthier SM, Whitaker MD, Roust LR, et al. Diabetes care in hospitalized non critically ill patients: more evidence for clinical inertia and negative therapeutic momentum. J Hosp Med.2007;2(4):203-11. [ Links ]
21. Ena J, Gómez-Huelgas R, Romero-Sánchez M, Gaviria AZ, Calzada-Valle A, Varela-Aguilar JM, et al. Hyperglycemia management in patients admitted to internal medicine in Spain: A point-prevalence survey examining adequacy of glycemic control and guideline adherence. Eur J Intern Med.2015;26(6): 392-8. [ Links ]
22. Urbieta Sanz E, Trujillano Ruiz A, García-Molina Sáez C, Galicia Puyol S, Caballero Requejo C y Piñera Salmerón P. Implantación de un procedimiento de conciliación terapéutica alingreso hospitalario por el servicio de urgencias. Farm Hosp. 2014;38(5):430-7. [ Links ]
23. Semesdiabetes.es (Internet). "Protocolo para el manejo del paciente con diabetes mellitus en Urgencias", de la Sociedad Española de Medicina de Urgencias y Emergencias (SEMES). http://www.semesdiabetes.es/protocolo_diabetes_2.pdf. [ Links ]
24. ACE/ADA Task Force on Inpatient Diabetes. American College of Endocrinology and American Diabetes Association consensus statement on inpatient diabetes and glycemic control: A call to action. Diabetes Care.2006;29(8):1955-62. [ Links ]
25. Inzucchi SE. Clinicalpractice. Management of hyperglycemia in the hospital setting. N Engl J Med. 2006; 355(18):1903-11. [ Links ]
26. Delgado Sánchez O, Nicolás Picó J, Martínez López I, Serrano Fabiá A, Anoz Jiménez L, Fernández Cortés F. Reconciliation errors at admission and departure in old and polymedicated patients. Prospective, multicenter randomized study. Med Clin (Barc). 2009;133(19):741-4. [ Links ]
27. Winterstein AG, Hatton RC, Gonzalez-Rothi R, Johns TE, Segal R: Identifying clinically significant preventable adverse drug events through a hospital's database of adverse drug reaction reports. Am J Health Syst Pharm.2002;59(18):1742-9. [ Links ]
28. Hirsch IB. Sliding scale insulin-time to stop sliding. JAMA.2009 Jan 14;301(2):213-4. [ Links ]
29. Golightly LK, Jones MA, Hamamura DH, Stolpman NM, McDermott MT. Management of diabetes mellitus in hospitalized patients: efficiency andeffectiveness of sliding-scale insulin therapy. Pharmacotherapy.2006;26(10):1421-32. [ Links ]
30. Munoz C, Villanueva G, Fogg L, Johnson T, Hannold K, Agruss J, et al.Impact of a subcutaneous insulin protocol in the emergency department: RushEmergency Department Hyperglycemia Intervention (REDHI). J Emerg Med.2011;40(5):493-8. [ Links ]
![]() Correspondence:
Correspondence:
Correo electrónico: carmencaballero.requejo@gmail.com
(Carmen Caballero Requejo).
Recibido el 21 de octubre de 2015;
aceptado el 24 de febrero de 2016.











 texto en
texto en