Contribution to scientific literature
Currently there are various protocols for the use of palivizumab for the prevention of the Respiratory Syncytial Virus, either hospital guidelines or by the different Autonomous Communities. This article intends to show for which type of preterm patients it would be cost-effective to use palivizumab in our hospital setting. To this aim, a pharmacoeconomic study has been conducted, with our own effectiveness data, and costs extracted from the databases in our centre. Even though many articles of this type have been published, the majority are based on analytical models of decision making, where various assumptions are made about efficacy, and costs are significantly different from those in our setting. The innovation of this study is that it is based on data collected in our hospital, and therefore can be more easily applied to other healthcare centres in our setting.
The outcomes reached in our study, with the limitations stated, can be useful for other healthcare centres in our setting in order to make decisions regarding the use of palivizumab.
Introduction
Bronchiolitis is the most frequent lower respiratory tract condition during the first two years of life. It appears as an epidemic during winter, and its etiology is predominantly viral, with the Respiratory Syncytial Virus (RSV) as the cause for over 50% of all cases.1
Treatment of acute bronchiolitis is symptomatic, because there is no effective etiological treatment. The prevention of bronchiolitis caused by RSV is currently based on hygienic-sanitary measures and passive immunoprophylaxis, indicated for preterm patients, those with chronic pulmonary disease (CPD) and hemodynamically significant congenital heart disease1-4.
The efficacy of palivizumab in preterm infants was shown in the IMpact clinical trial, with a reduction in hospital admissions for RSV infection, with no reduction observed in days with oxygen, mechanical ventilation and mortality. The study demonstrated that palivizumab caused a reduction in hospitalizations from 10.6 to 4.8%, with a 5.8% absolute risk reduction (ARR), and the number of patients to treat (NTT) to reduce one admission was 17, with a 1.7 ARR and 59 NTT in the Intensive Care Units5.
Efficacy data have been confirmed by subsequent studies 6,7; however, there is no unanimity in the pharmacoeconomic studies conducted, because their conclusions are very dissimilar, and in many cases contradictory, from incremental cost to important savings per avoided admission; this is basically due to the different methodologies used and assumptions made 8-14.
Based on a comprehensive review of the scientific literature published at that time, it was decided by consensus to restrict the use of palivizumab in our hospital in the 2012-2013 season (12/13) to preterm patients <9-month-old at the start of the RSV virus season, with CPD and high oxygen requirements.
The primary objective of our study was to evaluate the efficiency (cost-effectiveness) of the new protocol for using palivizumab to prevent the RSV infection in preterm infants with a GA from 29 to 35 weeks; its secondary objective was to conduct an analysis of the risk factors and severity in patients admitted during the seasons with the new protocol.
Materials and methods
The study was conducted in a third-level hospital covering the paediatric population of the Las Palmas province (Complejo Hospitalario Universitario Insular Materno-Infantil) located in Gran Canaria, with a population of 851,157 inhabitants.
Period of study
The period of study included from the bronchiolitis 08/09 season to the 13/14 season: 4 seasons with the extended protocol, and 2 seasons with the new protocol. Appendix 1 details the protocol for use of palivizumab from seasons 08/09 -11/12, from now on called the extended protocol; and Appendix 2 details the protocol for the 12/13 and 13/14 seasons, from now on the protocol by consensus.
Perspective of the study and costs analyzed
The study was conducted from the perspective of the Health System, including hospitalization costs, which were provided by the Unit of Analytical Management in our hospital; the cost of palivizumab per patient, calculated for each season, was extracted from the Pharmacy Management Application Farmatools®. In our hospital, all doses are prepared individually for a better use of the vial.
Effectiveness
In order to calculate effectiveness, the admission rate of preterm patients for RSV was estimated, excluding patients with congenital heart conditions, and stratified by GA: <29; <32 and <35.
The admission rate for each season or cumulative was determined as the ratio between admissions for RSV (from October, 1st to March, 31st) and the total number of preterm infants born in that season (from April, 1st to March, 31st) for each of the ranges previously mentioned.
The hospital admissions by bronchiolitis due to RSV (ICD-9-CM 466.11) for the seasons from 08/09 to 11/12 were extracted from the Hospital Encoding Systems, and the births from the Obstetrics Unit application.
Patients hospitalized in the seasons with the protocol by consensus, 12/13 and 13/14, were obtained prospectively, through the electronic clinical record, Selene®; the following data were collected: admissions for bronchiolitis due to RSV from October to March, date of birth, admission and discharge, age at admission in months and days, GA in weeks, weight at birth in grams, gender, CPD involvement, indication for palivizumab and risk group according to the extended protocol, prophylaxis with palivizumab and mortality.
During the 13/14 season, the following risk factors were also collected: environmental and social aspects such as exposure to smoking, social living situation, cohabitation with animals, attendance to nursery school, type of diet, educational level of parents, family history of allergies, and siblings of school age. In order to assess the episode severity, the following were collected: days of hospitalization, admission at the Intensive Care Unit (ICU), requirement of oxygen and/or mechanical ventilation, and the period used with these therapeutical resources.
Measurement of results: Incremental cost-effectiveness ratio (ICER)
The ICER was calculated as the ratio between the difference in costs (including cost per admission and the cost of palivizumab) and the difference in efficacy (deducting the admission rate with restricted protocol from the admission rate with the extended protocol). This ratio was estimated for individual data (each season with the extended protocol vs. the 12/13 and vs. the 13/14), and for cumulative data of admissions and births (period with extended protocol: from the 08/09 season to the 11/12 season vs. the period with protocol by consensus: seasons 12/13 and 13/14).
Results
Table 1 shows the patients admitted for bronchiolitis due to RSV and the total number of preterm births by season, as well as the number of patients treated with palivizumab, the cost per patient with palivizumab, and the daily cost per admission to a Hospitalization Unit.
Table 1 Data stratified by season: births, number of admissions due to RSV infection, patients treated with palivizumab, and costs per admission and palivizumab

*Patients born at each GA stratum from 6 months before the start of the season (from April, 1st to the end of the season, March, 31st)
**Admissions due to RSV in the period from October, 1st to March, 31st.
Effectiveness Calculation for Individual Data
Based on the data that appear in Table 1, the hospitalization rate for each season was calculated, as well as the ARR and NTT of the 4 seasons with the extended protocol vs. those with the protocol by consensus for each GA range. Only for the GA <35 , comparing the 08/09 season vs. the 12/13 and the 13/14, a significant reduction in hospitalization ARR was observed, from 3.6% (CI95%: 7% to 0.2%) and NTT 28 (CI95%: 500 to 15) p=0.047 and ARR 5.6% (CI95%: 9.4% to 1.9%) and NTT 18 (CI95%: 53 to 11) p=0.003 respectively. In the other 30 comparisons between seasons, no significant reduction in hospitalizations was observed; see the figure captions 1, 2 and 3.
Effectiveness Calculation for Cumulative Data of Admissions and Births
The cumulative rate of admissions with the extended protocol vs. the protocol by consensus for each GA stratum appears in Table 2. Only for GA<35, there was a significant reduction in hospitalization with the extended protocol (p=0.005).
Table 2 Effectiveness assessment with cumulative data for each GA stratum

ARR: Absolute Risk Reduction; CI: Confidence Interval; NTT: Number of patients to treat in order to obtain one additional efficacy unit (in this case, to reduce one admission).
*Statistical significance has not been calculated, because the admission rate in the protocol by consensus is lower than in the extended protocol.
** The CI of ARR includes zero, and therefore has no statistical significance; one of the NTT limits was negative, therefore including patients for whom the extended protocol was beneficial and those for whom it was detrimental.
There was no statistical significance estimated for GA <29, because the hospitalization rate was lower for the protocol by consensus than for the extended protocol. For GA< 32, the confidence interval of ARR included zero, and therefore had no statistical significance; one of the NTT limits was negative, therefore including patients for whom the extended protocol was beneficial and those for whom it was detrimental.
ICER Calculation for individual and cumulative data
Figure 1, Figure 2 and Figure 3 show the ICER Calculation implementing the median hospital stay of 7 days for each season with the extended protocol, vs. the 12/13 season and vs. the 13/14 season with the protocol by consensus.

Figure 1 Comparison between seasons for the GA stratum < 29: effectiveness and incremental cost-effectiveness ratio.
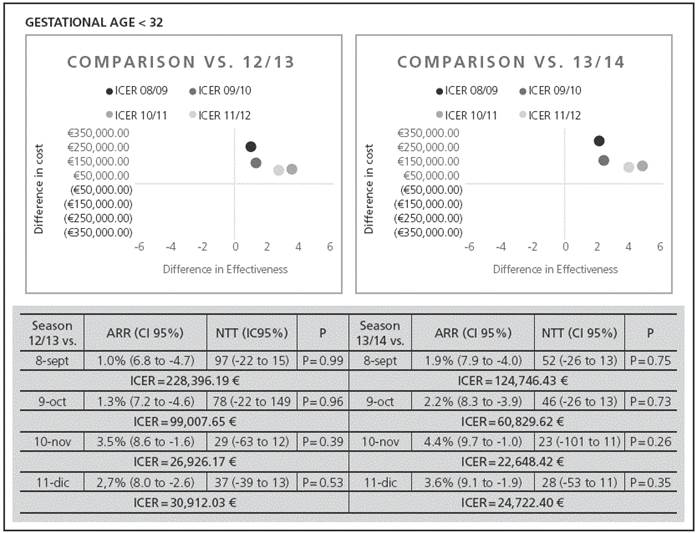
Figure 2 Comparison between seasons for the GA stratum < 32: effectiveness and incremental cost-effectiveness ratio.

Figure 3 Comparison between seasons for the GA stratum < 35: effectiveness and incremental cost-effectiveness ratio.
In the GA<29 range (Figure 1) for the 08/09 and 09/10 seasons vs. the 12/13 and 13/14 seasons, there was a negative result, derived of a higher hospitalization rate with the extended protocol vs. the protocol by consensus. The mean ICER for evaluable data was 51,346.06€ (range: 5,380.33€ to 165,759.00€). For the GA<32 (Figure 2), the mean ICER was 77,273.61€ (range: 22,648.42€ to 228,396.19€).
The resources needed to achieve a reduction in the percentage of patients hospitalized in the GA<35 range (Figure 3), the only range where a significant reduction of hospitalizations was observed, was the amount of 53,250.07€ (range: 14,793.39€ to 90,446.47€). It is worth highlighting the negative ARR of the 9/10 season vs. the 12/13 season, derived of a higher hospitalization rate in the season with the extended protocol. The ICER for the cumulative data for GA<35 was 50,525.53€ (28,688.22€ to 211,575.65€).
According to the cost of palivizumab per season, the cost per admission, and the mean 7-day stay per patient, the implementation of the new protocol for using palivizumab represented mean economic savings of 169,911.51 € per each one of the 6 seasons of the study.
Calculation of the efficiency threshold
Based on the costs and effectiveness mentioned, a simulation was conducted to calculate which should be the hospitalization rate or the cost of medication per patient in order to consider that the extended protocol was cost-effective, considering a 30,000€ efficiency threshold. The mean cost of palivizumab per patient considered cost-effective would be 1,206.67€; these costs are calculated for a maximum use of the vial. The median hospitalization rate estimated to be cost-effective would be 9.21%.
Analysis of risk factors and severity of hospitalized patients with the protocol by consensus
The following are the data collected prospectively from patients hospitalized for bronchiolitis due to RSV in the 12/13 and 13/14 seasons (data between brackets are for the 13/14 season). The number of admissions due to RSV was of 167 (153) patients. The median age in months at admission was 2(0.2-20.1) (2(0.5-18.1)), with 63.47% (63.40 %) of admissions for <3-month-old infants; Table 3. Regarding the distribution by gender, 58% (50.33%) were male. The mean weight of patients in grams was 2.990g±752 (2.930g±930). The mean GA in weeks was 38±3.00 (38.37±2.88), where 91.62% (87.58%) of patients presented a GA> 35 weeks; there is a description in Table 4 of the number of patients according to their GA.
Ten (10) (5,99%) (11 (7,19%)) met the prophylaxis criteria according to the extended protocol. None of the hospitalized patients presented bronchopulmonary dysplasia (BPD). There were no exitus.
During the 13/14 season, 52.28% of patients required oxygen, with a mean of 3.63 days (±1.9); none required mechanical ventilation. The mean stay in days in the Hospitalization Unit was 7.12 (±3.61); 6 patients were admitted to the ICU (3.9%) for a median of 5 days (2-24).
Regarding environmental risk factors, it was identified that 67.77% were not being breastfed; 46.67% were exposed to smoking; 30.76% lived in overcrowded conditions; 64.71% of parents presented a low educational level, and 6.62% had superior education; 33.33% presented a family history of atopy; 31.53% cohabited with animals, and 58.99% had siblings of school age.
Discussion
Based on the data from the study, both cumulative (Table 2) as detailed (Figure 1, Figure 2 and Figure 3), we can state that it has not been possible to demonstrate conclusively that the extended protocol has a superior effectiveness vs. the protocol by consensus in preterm infants with GA<32-weeks.
However, when analyzing the cumulative data in preterm infants with GA<35-weeks, a significant reduction in hospitalization has been confirmed with the extended protocol. In the individual analysis of data, there was only a reduction in hospitalization for preterm infants with GA<35-weeks, when the 08/09 season was compared vs. the 12/13 and 13/14 seasons; this outcome was expected, because the protocol by consensus does not include prophylaxis in this group of preterm infants without any associated conditions.
However, this effectiveness is associated to a NTT in the range of 30 and an incremental ICER of 50,525.53€ in order to achieve one additional unit of efficacy for cumulative data and for individual data by season of 67,489.68€ (12/13 vs. 08/09) and 40,548.90€ (13/14 vs. 08/09). Even though in our country there is no efficiency threshold about what would be acceptable from an economic point of view, these results are excessive for the majority of the clinical assumptions mentioned.
It is worth highlighting the higher index of admissions found with the extended protocol for the cumulative data for GA <29 and when seasons were compared individually; this higher index was observed in the 09/10 season. This can be due to the fact that we were working with a very small number of admissions due to RSV in preterm infants, and that the 09/10 season presented a higher virulence. All this leads us to think of the need to prolong the study over time, in order to minimize the limitations previously described.
We must point out at the bias that can be derived from the fact that the data for the season with extended protocol were retrospective, and those with the protocol by consensus were prospective; therefore, it should be expected to have a real admission rate higher than that described in the seasons with extended protocol. On the other hand, only those preterm infants born in our hospital have been included, and therefore these data could be underestimated by not taking into account those infants born in other healthcare centres.
Our results are compatible with those from other cost-effectiveness studies, such as the one conducted by the British Health Technology Assessment Agency in 2011, which consisted in a systematic review of scientific evidence in order to assess the cost-effectiveness of palivizumab for immunoprophylaxis of bronchiolitis due to RSV. They included 13 studies and conducted a subgroup analysis with 256 different combinations of risk factors, and reached the conclusion that prophylaxis with palivizumab would only be cost-effective for some subgroups of patients who presented BPD or congenital heart condition with a specific GA or age at the start of the season14.
Another study established that prophylaxis will only be effective in preterm infants with CPD and during the months with high risk of infection, from November to January; the cost per prevented admission in February and March amounted to 47,145€ and 105.120€ respectively15,16.
A recent study obtained incremental costs superior to ours: an incremental cost for preventing one admission for bronchiolitis of 202,635$- primarily due to the higher costs of the medication.1
However, we can find pharmacoeconomic studies in literature with a cost-effectiveness or utility balance very favourable to the use of palivizumab. As we have already pointed out, this is due to the different assumptions made, and one of the main ones is the reduction of mortality, as well as the bias found by the Payer8,11-13).
Therefore, the study conducted in our country in preterm infants with a GA from 32 to 35 weeks and two or more risk factors estimated the cost per quality-adjusted life year (QALY) in 13.849 € from the perspective of the National Health System, and in 4,605 € from the social perspective8. Other studies conducted in Austria, The Netherlands, and the United Kingdom, obtained a QALY cost in the range of 20,704€ (preterm with GA ≤35 weeks), 18,563€ (preterm with GA between 32 and 35 weeks) and 14,883€ (preterm with ≤35 GA), respectively. These studies are designed as analytical models of decision making where different assumptions are made, including a relevant reduction in mortality11-13.
We must highlight that the estimated cost of palivizumab per cost-effective patient for a threshold of expenses of 30,000€ would be less than half of the real cost of our data per patient and season. Regarding the hospitalization rate, this should be around 10%; this percentage is even lower than the one published by other authors who established that immunoprophylaxis with palivizumab is only cost-effective in patients with GA between 23 and 36 weeks, with 28 days of oxygen therapy, and discharged from hospital from September to November, a period in which they have determined a risk of hospitalization between 11 and 24.6%18-19.
Regarding the detailed analysis of the children admitted in the 12/13 and 13/14 seasons, we must take into account that these were babies, with a higher prevalence in those <3-month old; and regarding GA, 90% of them were born at term and were not included in a high-risk population; therefore, we must question the need for indiscriminate immunoprophylaxis for all preterm infants. These data coincide with those collected in different publications, where the risk factors associated with acute bronchiolitis are stated, such as having siblings of school age, rural dwelling, smoking parents, low academic training of parents, lack of breastfeeding, and a family history of allergy 20,21.
The current recommendations by the American Academy of Paediatrics (AAP) about immunoprophylaxis with palivizumab include preterm infants with GA<29 and <12-month-of age at the start of the RSV season. For GA>29 , the use of palivizumab must be determined by the existence of some associated risk factor, such as CPD (oxygen required at least during 28 days since birth); these recommendations also highlight the importance of hygienic-sanitary measures. These are similar to the recommendations established by the Canadian Academy, which limits immunoprophylaxis in the GA <29 group to patients <6-month-old at the start of the season, and classifies it as reasonable but not essential when there is no associated condition such as CPD. For patients with GA > 29 weeks, its use is not recommended if there is no associated condition, due to the low incidence of hospitalization. They also insist on health education strategies, similarly to the AAP.22-24.
The latest guidelines about vaccination against RSV collected in the 2015 Green Book of the United Kingdom still include preterm patients only if they present CPD, delimiting its cost-effectiveness based on chronological age and GA25.
The Spanish Society of Neonatology has not conducted any change in the guidelines for use of palivizumab for preterm infants with GA<29 in their first year of life and for their second season only if < 9 month-old. For the group with GA from 29 to 32 weeks, it recommends its use if the age at the start of the season is <6 months, and for the GA of 32-to-35 if they present two major risk factors 26.
The protocol adopted by consensus in our hospital has not represented a significant increase in hospitalization rates for preterm patients with GA < 32 weeks; a higher hospitalization rate has been observed in those preterm infants with GA > 35 weeks, without being able to demonstrate a higher efficiency of the extended protocol vs. the protocol by consensus.
RSV infection was associated with a significant morbidity in our setting; however, the majority of patients admitted in the seasons with the protocol by consen sus did not present certain medical factors such as CPD or premature birth, but other environmental and social risk factors already described, as well as a low postnatal age at the start of the RSV season.
The strategies for prevention of RSV infection must go beyond prophylaxis with palivizumab, and focus on education programs targeted to parents or carers, conducted from the hospital at patient discharge, regardless of their inclusion in a group of risk.











 text in
text in 




