Contribution to scientific literatura
The recently published report by the Spanish Society of Hospital Pharmacy “on the situation of the Hospital Pharmacy Units in Spain: infrastructures, resources and activity” shows different aspects regarding the degree of implementation of new technologies in Pharmacy Units. The objective of this study is to offer a more specific view about the material resources used for the preparation of intravenous chemotherapy in the Autonomous Community of Madrid.
The conclusions of this study can be used by different Pharmacy Units in order to conduct a comparison based on the assessment of their own materials and methodologies, with the aim to implement an improved patient care.
Introduction
“High risk medications” are those that, when not used adequately, present a higher likelihood of causing severe damage or even death to patients. Cytostatic medications, both parenteral and orals, are included in the “high risk medications” list published by the Institute for Safe Use of Medications (ISMP)1.
Based on the “Self-assessment questionnaire on safety culture in the use of medications by ISMP Spain”2, the Ministry of Health, Social Services and Equality published the outcomes of the study “Evolution of the implementation of safety practices for the use of medications in Spanish hospitals (2007-2011)”. This publication confirms the shortcomings in the medication safety culture, regarding technologies, access to basic information on patients during prescription, dispensing and administration of medications, as well as the implementation of bar codes in administration3. Even so, the implementation of new technologies for the preparation of intravenous mixtures (IVM) for chemotherapy (Ct) has led in recent years to an increase in the safety of patients, handlers, and pharmacotherapeutical quality.
Within the specific objectives in the “Patient Safety Strategy by the National Health System” in its latest update (2015-2020)4, the development of assisted electronic prescription (AEP) has been highlighted, with systems to aid clinical decision that have proven efficacy, the implementation of safe practices with high risk medications, and the promotion of self-assessment of the safety in the system for use of medications in healthcare centres.
Along this line, the “TECNO” Work Group for New Technologies from the Spanish Society of Hospital Pharmacy (SEFH) prepared in 2006 a survey to assess on a national level the degree of implementation of computer systems, such as AEP, the administration by bar codes in order to identify patient / medication, etc.5. Besides, the SEFG has also published recently the “Report on the situation of Hospital Pharmacy Units in Spain: infrastructures, resources and activity”, with a descriptive analysis of information systems and the quality and safety of work in Hospital Pharmacy Units6.
On the other hand, the International Society of Oncology Pharmacy Practitioners (ISOPP) recommends the use of closed systems both for preparation (reconstitution of lyophilized agents, dilution of vial contents, and transfer to the final container), and for the administration of IVMs to patients, due to the reduction in the risk of accidental spillages and spray formation (IVMs with carmustine, cyclophosphamide, ifosfamide, etc.). Closed systems are devices that prevent mechanically the transfer of environmental contaminants inside the device, as well as the leakage of high risk medications or their vapours outside the device7. In their guidelines for handling hazardous drugs, The American Society of Health-System Pharmacists (ASHP) reaches the conclusion that closed systems cannot replace Biological Safety Cabinets (BSCs) and that their effectiveness must be demonstrated in independent studies8.
In our work setting, it is necessary to have a continuous assessment of the preparation and administration process for Ct IVMs. For this reason and what we have mentioned earlier, our objective was to understand the degree of technological implementation in hospitals of the Autonomous Community of Madrid in these settings, through a survey that could be used to group the type of development by hospital.
Therefore, we have conducted this study aimed at understanding the current degree of implementation of new technologies for handler and patient safety in the preparation and administration of cytostatic agents in different hospitals of the Autonomous Community of Madrid.
Methods
An observational descriptive study was designed, through the preparation of a questionnaire in Microsoft Word® format, including 22 questions and divided into two parts. The first part asked for demographic information about the hospital (3 questions): number of beds, functional dependency, and healthcare purpose. The questions in the second part were associated with the implementation of new technologies in the processes for preparation and administration of cytostatic drugs for parenteral administration; the 19 questions included were: availability of AEP in Day Hospital, availability of AEP in the Oncology Ward, availability of AEP in the Haematology Ward, AEP program available at the hospital, Intravenous Ct, availability of BSCs, use of individual protection equipment (IPE), use of closed systems in the reconstitution, transfer and/or administration of cytostatic agents, re-labelling of cytostatic vials at reception and information included, sequential gravimetric control in preparation and provider company, voice-controlled preparation and provider company, bar code reading and provider company, communication system, and analysis of errors. The majority of questions were closed, and respondents could choose between various options in the drop-down menu; a free-text field was provided for those cases where the answer was not included in the multiple options.
The study population was formed by the hospitals in the Autonomous Community of Madrid that prepared cytostatic agents for their parenteral administration (inclusion criteria). Therefore, the study excluded all hospitals for psychiatric care, geriatrics and/or long-stay, maternity, orthopaedic surgery, and/or rehabilitation. The data collection period started on March, 2016 and ended on August, 2016.
The “National Catalogue of Hospitals 2015” 9, updated on December, 31st, 2014, was consulted in order to obtain a list of hospitals, and to select those within the Autonomous Community of Madrid.
A telephone conversation was held with the staff from the different hospitals in the study population which met the inclusion criteria established (preparing Ct IVMs), in order to confirm this fact. The survey was targeted to the clinician staff of the Hospital Pharmacy Units; or failing this, the nursing staff who were responsible for preparing Ct IVMs. The survey was sent through e-mail. Those persons who did not answer to the first round were contacted again through this means, and in case of no response, the contact person was phoned. On the other hand, and with the objective to resolve any inconsistencies detected in the answers to some surveys, the persons who had completed them were contacted again.
A Microsoft Excel® 2010 spreadsheet was developed for the record and statistical processing of data, including the items collected in the survey. This study has not been previously assessed or authorized by a Research Ethics Committee.
Results
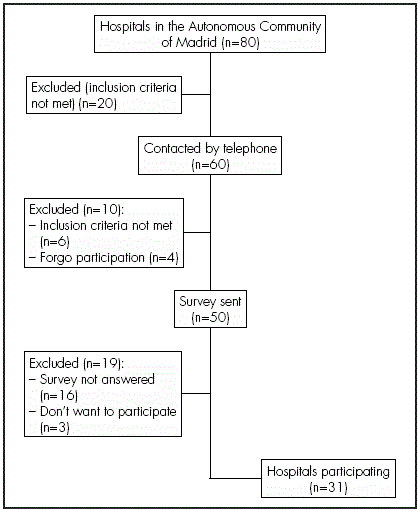
The flow of participating hospitals can be seen in Figure 1.
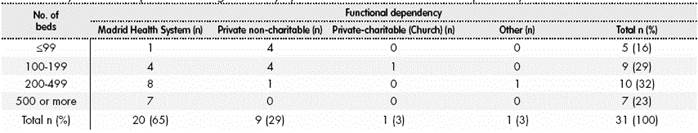
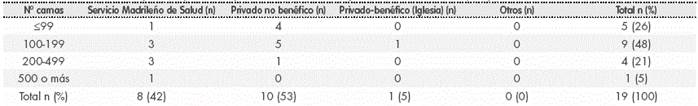
Hospitals were grouped by number of beds, as: ≤99 beds, from 100 to 199 beds, from 200 to 499 beds, and >500 beds. The distribution by number of beds and healthcare purpose of the hospitals included in the survey appears in Table 1. The hospitals that completed the survey were homogeneous in terms of number of beds; moreover, 65% of hospitals belonged to the Madrid Health Service, and 29% to a non-charitable Private Society. On the other hand, Table 2 collects the characteristics of those hospitals that did not answer the survey after this was sent. Almost half of these hospitals (48%) had 100-199 beds and only one hospital with >500 beds (5%) did not answer the survey.
Table 2 Analysis of the hospitals not answering the survey by number of beds and functional dependency

It was observed that the majority of large hospitals that answered the survey (>200 beds) had AEP in the Day Hospital and the Oncology and Haematology wards (Table 3). Besides, the study confirmed the variety of AEP programs available in the Community of Madrid (Oncofarm®, SAP®, Farmatools®, FarHos®, SELENE®, Casiopea 2.0®, Hospiwin®).
Table 3 Degree of implementation of Assisted Electronic Prescription according to number of beds

AEP: Assisted Electronic Prescription.
Practically in all centres included in the survey (30 out of 31 centres), Ct IVMs were prepared in the Pharmacy Unit, and all centres had BSCs and IPE. However, only one of the 31 hospitals in the survey re-labelled chemotherapy vials when received in the Pharmacy Unit, which allows a higher traceability of the mixtures prepared in a centralized way.
Regarding the preparation process, the record of the components used through bar code reading had been implemented in 11 of 31 centres (35.4%) and under trial period in 6 centres (19.4%); the voice-controlled technique for assistance in preparation was not implemented in any of the 31 centres, though it was under trial period in 2 centres (6.4%); the final examination of preparations through gravimetric control was very low, because it had been completely implemented only in 2 of 31 centres (6,4%), and under trial phase in 3 centres (9.6%).
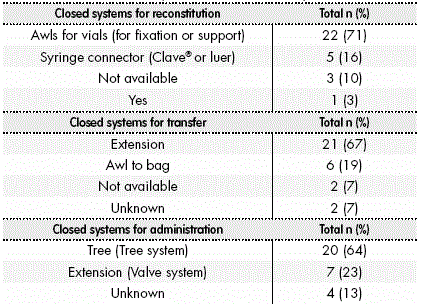
The use of closed systems at different points in the preparation-administration process is shown in Table 4. The most frequently used closed systems were: awls for vial reconstitution, extensions for transfer, and tree administration system. When a tree-type closed system is used for administration of cytostatics, the extension is the closed transfer system; and when administration is conducted through a valve system, the closed system transfer is awl to bag. Finally, the systems for communication and analysis of medication errors in the preparation and dispensing of Ct IVMs had been completely implemented in 24 out of the 31 centres (67.8%). In only one centre, the implementation of these markers was in the trial phase.
Discussion
The response index obtained (62%) was higher than that of a similar study by T. Bermejo Vicedo et al.5, which reached 38.6%. Anyway, there could be a selection bias, given that 48% of hospitals that did not answer the survey had 100-199 beds, and one (5%) was a hospital with >500 beds. The workload volume regarding chemotherapy IVMs will usually be directly proportional to hospital size; therefore, it seems reasonable to think that larger hospitals (with a higher number of beds) will have higher safety systems than smaller hospitals; though another variable to be studied as a workload criterion could have been the number of intravenous mixtures prepared. However, it could be confirmed in this study that 80% of medium-large size (200-499 beds) hospitals included in the survey had an AEP at Day Hospital and the Oncology and Haematology wards (Table 3). This percentage was higher than that of larger hospitals (>500 beds) with 57% figures, which can be due to the difficulty for hospitals with high healthcare activity to implement new technologies. On the other hand, in small size hospitals (≤99 beds), there was a higher percentage without AEP implemented at Day Hospital and Oncology and Haematology wards. These data are in line with the Report on the Situation of Hospital Pharmacy Units in Spain 6, because if we group medium-sized hospitals (from 100 to 499 beds), 53% of them has AEP; and considering all hospitals participating in the survey, regardless of degree of implementation, we see that there has been an increase in the percentage from 31.5% in 20065 to 80.6%.
However, hospital size should not justify the lack of safety for patients and healthcare professionals who prepare chemotherapy in smaller hospitals; therefore, the involvement by the management staff in these centres will be essential for the safe use of medications. And here is where the role of Hospital Pharmacists becomes important, as they must be able to promote quality and safety policies in their work setting.
The study also demonstrated the variety of AEPs existing in the different centres involved in the survey in the Autonomous Community of Madrid. Each centre negotiates separately the purchase and implementation of these programs, but it would be advisable to have rules forcing the companies that design these programs to meet a series of minimum requirements, such as those described by the “Spanish Network of Agencies for Evaluation of Healthcare Technologies and Services by the National Health System”. At European level, there are other healthcare technology networks, such as the EUnetHTA (European network for Health Technology Assessment), which could be used as a reference for determining these minimum requirements. Regarding the degree of compliance with material requirements by internationally acknowledged scientific societies, such as the NIOSH (National Institute for Occupational Safety and Health) and the ISOPP, as well as different European and national guidelines, this was very high in those cases where there was a centralized unit for chemotherapy preparation (Pharmacy Unit on 97%), a BSC available (100%), in a controlled environment and with IPE (100%). At this point, it is worth remembering that cytotoxic medications are potentially carcinogenic, mutagenic and/or tetarogenic substances, which can also cause irritation by direct contact as well as ulcers and even tissue necrosis. Therefore, it is important to work in a safe environment when handling this type of substances. These results are on line with those obtained in the 2015 National Report6.
Centralized IVM preparation in Pharmacy Units offers, on one hand, technical advantages, such as the highest guarantee of physicochemical stability, asepsis, storage and expiry date; and on the other hand, healthcare advantages, because a standard preparation of IVMs entails a reduction in the risk of developing drug-related problems, and increases the involvement by the Pharmacist in dosing individualization and their integration in the healthcare team10. Thus, the Pharmacist will be responsible for the preparation of Ct IVMs11 in adequate conditions of sterility, correct labelling, storage and distribution12. Finally, a centralized preparation streamlines the use of material and staff resources, which represents important economic savings10.
Regarding transfer systems, an extension is used in most hospitals; even though it is necessary to purge the system, this will present a lower risk of environmental contamination (formation of sprays, drops or spillage) than the use of awls for bags. On the other hand, there is no formal national register of these closed systems for drug transfer, and the specific requirements that these closed systems should meet in order to be certified have not been determined.
Regarding the implementation of gravimetric control systems, voice-controlled preparation, and bar code reading, it was observed that these technologies were not available in the majority of hospitals, except for bar code reading. The main difficulty in the implementation of these technologies is the economic investment required for setting them up. There should be a speech recognition system with headphones and microphone inside the BSC (for voice-controlled preparation), bar code (BC) readers, or data matrix, scales, etc. Likewise, for administration control, an identification system is required (label with BC) for the finished product, at the different points of administration (beds, armchairs) and administration equipment (pumps), as well as an identifying system for the nursing (cards with BC) and a WiFi PDA system to read the BCs of the different elements mentioned.
Additionally to the economic investment entailed by all we have mentioned, we will also find the need to re-label the cytostatic and saline vials used with the product information (description), lot and expiry date, which represents extra time of work for the Pharmacy staff. This problem could be solved with further involvement by the pharmaceutical industry, incorporating in each product unit one BC with the information required.
Scientific evidence demonstrates a reduction in dispensing errors by the use of BC reading (qualitative control of the process), which in some cases can reach 85%13,14, as well as the reduction in potential adverse events15. Likewise, through sequential gravimetric control, it can be detected if the weight of the finished product falls within the determined margin of error, typically between 5 and 10%. Therefore, this will be a quantitative control of the process. On the other hand, the same companies that design AEP programs will develop these new technologies.
Only in one of the centres included in the survey, Ct IVMs were prepared by a robot in automated way. The use of a robot presents a series of advantages, such as the integration of the new technologies mentioned (bar codes, gravimetric methods, etc.), as well as higher accuracy and reliability16. As drawbacks, we should highlight their high cost, restrictions regarding the size and volume of certain products (e.g. because these are very bulky), and that one error in the database can affect many IVMs.
As in any other process, it is important to measure the quality of the results obtained, and quality indicators for preparation procedures must be used to this aim. The previously mentioned international societies (NIOSH, ISOPP) have published criteria and standards for cytostatic handling that can be used to describe the indicators of compliance.
There has been an increase in recent years in patient and healthcare professional safety during the preparation and administration of medication, due to the evolution of information systems (AEP, use of robots for chemotherapy preparation, etc.) and the preparation of technical guidelines and protocols in the different hospital units, such as the Guidelines for Good Practices for staff with occupational exposure to cytostatic agents by the A.M.M.T.A.S. (Madrid Society of Occupational Medicine in the Healthcare Setting)17. Moreover, different guidelines have been developed at European and national level regarding the exposure to carcinogenic or mutagenic agents in the work setting, such as the European Rule 2004/37/EC, Royal Decree 665/1997, the technical note for prevention by the National Institute for Occupational Safety and Health: NTP-740, and the ESS/1451/2013 order on “Prevention of lesions caused by needles and other sharp instruments in the hospital and healthcare setting”, as well as the recent publication by the National Institute for Occupational Safety and Hygiene (INSHT): “Hazardous drugs. Prevention measures for their preparation and administration18.
The SEFH also has a strong positioning regarding this matter, as can be seen in different items from the “2020 Strategic Plan”, where various objectives are determined regarding organizational development and safety practices in the management of these treatments in order to achieve a higher quality of care. These objectives and strategic lines include the incorporation of new technologies in order to improve the structure and quality of the Pharmacy Units, as well as to implement improvements in the system for use of medications. All this will be done through computer systems for management of integrated processes, AEP, and administration systems that are linked and/or integrated in the clinical record, including databases of information on medications and administration support, systems facilitating the control, traceability and safety of the process for preparation, handling and administration of high-risk medications or systems for management of risks and standard procedures for a safe handling of medications. In hospitals in the Community of Madrid where there is CT preparation, there is a medium degree of implementation of technologies for bar code reading, while the degree of implementation of vial re-labelling and gravimetric and voice-controlled preparation is low; therefore, there is a wide room for improvement in terms of traceability for the process of preparation and administration of Ct IVMs. For this reason, there should be a joint collaboration in order to achieve these objectives, at least in those hospitals included in the Madrid Health System.











 text in
text in