Introduction
The increase of chronic kidney disease (CKD) prevalence in patients with underlying lifestyle-related disorders (hypertension and diabetes mellitus) has become a a social and health problem1. well known, not without controversy. Changes in renal structure in older adults, a normal progressive and slow phenomenon according to some authors, have been linked with the decrease of glomerular filtration rate (GFR)2. Thus, lower GFR values in comparison to those of younger individuals does not necessarily imply the existence of a disease, but an expression of the aging process3.
CKD patients usually present osteoporosis and therefore high risk of suffering fractures4. Some authors have related low GFR values with increased risk of vertebral and hip fractures among older adults5,6. Renal function may be impaired in patients who suffer a hip fracture, and in turn, previous kidney disease may negatively affect treatment outcomes in aged patients who suffer a hip fracture7-10.
Incidence of hip fracture is high among older adults and the associated morbidity and mortality positions it as one of the most relevant age-related health problems11.
Renal function worsening in surgically treated older adults after hip fracture seems to be associated to a worse outcome12, which indicates the relevance of renal function in the internal homeostasis of this patients population. Moreover, as it is well known, renal dysfunction is frequently associated with osteoporosis and, therefore, with higher risk of fracture13-15. Renal function should be considered in the patient’s general clinical condition, it could be also demarcated by ranges of laboratory values. Hip fracture involves different degrees of bleeding or hydro-electrolytic disorders, among other possible alterations that may be detected through kidney-related laboratory tests.
The clinical situation of some older adults may be altered after a hip fracture, with the consequent worsening of their prognosis. Renal dysfunction affects patients’ internal homeostasis and the pharmacodynamics of their current medication, which may interfere with the management of the fracture. Early detection of altered laboratory values can help prevent complications should a patient suffer a hip fracture.
In this study, we aimed to determine the relationship between estimated GFR admission values (eGFR) and the outcomes after surgical treatment of hip fractures in a large cohort of older adults, paying special attention to patients with CKD.
Material and methods
Prospective study that included all patients >65 years of age who had suffered a hip fracture, had been surgically treated for primary hip fracture, with no pathologic or high-energy trauma aetiology, admitted to the Orthogeriatric Unit of Hospital Universitario de Salamanca (Salamanca, Spain) (a tertiary teaching hospital) between January 1, 2018 and December 31, 2019.
The following variables were recorded at admission:
- Demographic: sex (male, female), age (years and >80 years of age), place of residence (urban or rural considering < 13,000 inhabitants), previous living in an institution;
- Laboratory: haemoglobin (g/dL), lymphocyte count (x103/µL), albumin (g/dL), glucose (mg/dL), parathyroid hormone (PTH, pg/mL), vitamin D (ng/mL), creatinine (mg/ dL), urea (mg/ dL);
-
- Kidney damage and function: eGFR as a continuous variable (mL/min/1.73 m2) using the CDK-EPI equation16, as the single point-by-point variation may be highly dynamic, we also classified patients in five categories according to their eGFR ranges at admission:
- Fracture-related: type of hip fracture (extracapsular, intracapsular) and surgical procedure (osteosynthesis, partial replacement, total replacement).
From the patient´s medical records we collected previous diagnosis of renal and cardiovascular risk comorbidities (CKD, any cardiovascular risk, hypertension, type I and II diabetes, chronic cardiac insufficiency, ischemic heart failure) and medications related to cardiovascular risk (anticoagulant and antiplatelet agents).
For CKD patients, we collected laboratory data at three moments: basal (from records up to 6 months before being admitted to the hospital for hip fracture), at hospital admission, and at discharge (after hip fracture surgery).
While in the hospital, the relatives of the patients were interviewed to find out about their previous functional situation (Comprehensive Geriatric Assessment, CGA). Data were analysed using different geriatric scores:
- The Katz index (KI) to evaluate independence of daily functions (bathing, dressing, toileting, transferring, continence, eating), from A (independent) to G (dependent for all the evaluated functions).
- The Barthel index (BI) to measure the performance in activities in daily living (feeding, bathing, grooming, dressing, bowels, bladder, toilet use, transfers, mobility, stairs), from 0 (total dependency) to 100 (totally independent) using a five-item scale. Score was categorized in < 20: total dependency, 20-35: severe dependency, 40-55: moderate dependency, 60-95 slight dependency; 100: independent).
- The Lawton-Brody index (LBI) to evaluate independent living skills (use of a telephone, shopping, food preparation, housekeeping, laundry, transportation, responsibility for own medications) from 0 (low function/dependent) to 8 (high function/independent). No discrimination by gender was found.
- The Physical Red Cross scale (PRCS) to evaluate the physical ambulatory ability from 0 (full capability without the need of assistance) to 5 (bed-ridden patients).
We also collected the following factors: waiting time to surgery, whole Length of Stay (LOS), incidence of post-surgical complications (any, seroma, wound bleeding), and medical postoperative complications (any, renal, digestive, cardiac, respiratory, neurologic complications, and need for transfusion).
Upon hospital discharge, in-hospital mortality rates, and 30- and 90-day mortality rates were recorded.
The study was conducted following the Declaration of Helsinki and approved by the Institutional Review Board of CEIm Hospital Universitario de Salamanca (ref. code: 2020 09 563). All participants (or their relatives) signed an informed consent before their inclusion in the study.
Statistical Analysis
Qualitative variables were presented as percentage and outlined by contingency tables; the Chi-square test was used to determine if there were any inter-variable statistical significant differences. Quantitative variables were presented as mean ± standard deviation and median and interquartile range (IQR). The Kolmogorov-Smirnov and Levene tests were used to assess normality and homogeneity. An ANOVA (followed by a post hoc Bonferroni test) was performed to compare inter-group variables. The Wilcoxon matched-pairs signed-rank test was used to compare quantitative variables between two paired groups from basal situation to hospital admission and hospital discharge.
Association between variables were addressed by odds ratio (OR) with its confidence interval at 95% (95%CI) from the binary logistic model (for binary dependent variables) and by β (95%CI) from the linear regression model (for quantitative dependent variables); for the multilevel dependent variables, the β (95%CI) for the most significant category is shown from a mixed-effects model.
All data were analysed with IBM SPSS Statistics version 23 and R version 3.6.2 (2019-12-12). In all cases, a p-value <0.05 was considered statistically significant. Patients with incomplete data records were excluded from statistical analysis.
Results
Nine hundred and forty-five patients met the inclusion criteria. Three patients were transferred prior hospital discharge, thus, 942 patients were included in the study (attrition rate 0.003%); 72.8% of the patients were female and mean age was 86.2±6.8 years (range 65-103).
Mean eGFR at hospital admission was 58.2±20.2 mL/min/1.73m2 (median: 59; IQR: 42-76). Based on eGFR levels at admission, the 942 study patients were classified into five groups (Table 1); most study patients (84.7%) had eGFR values of 30-89 mL/min/1.73m2. Around half of the patients had an eGFR at admission >60 mL/min/1.73m2 (48%, n = 452), and 101 (10.7%) patients had values <30 mL/min/1.73m2.
Table 1. Biodemographic summary and frequency (%) of previous diagnosis of renal and cardiovascular risk comorbidity of older patients surgically treated for hip fracture based on the estimated glomerular fraction rate range.
| Admission eGFR ranges (mL/min/1,73m2) | Total | ≥90 | 89-60 | 59-30 | 29-15 | <15 | p-value |
|---|---|---|---|---|---|---|---|
| n (%) | 942 | 43 (4.6) | 409 (43.4) | 389 (41.3) | 92 (9.8) | 9 (1.0) | |
| Sex (women, %) | 72.8 | 58.1 | 74.6 | 72.5 | 75.0 | 55.6 | 0.140 |
| Age (years) | |||||||
| Mean ± SD | 86.2±6.8 | 77.3±6.6 | 84.8±6.6 | 88.1±5.9 | 88.7±6.5 | 85.2±5.4 | <0.001 |
| ≥80 (%) | 83.9 | 30.2 | 80.4 | 91.5 | 92.4 | 77.8 | <0.001 |
| Place of residence (rural, %) | 48.1 | 45.2 | 49.9 | 46.0 | 49.5 | 66.7 | 0.621 |
| Institution-living (%) | |||||||
| At admission | 32.4 | 34.9 | 29.6 | 34.8 | 34.8 | 22.2 | 0.512 |
| At discharge | 54.1 | 51.2 | 51.0 | 56.8 | 59.8 | 44.4 | 0.369 |
| Extracapsular fracture (%) | 57.2 | 58.1 | 53.3 | 59.1 | 64.1 | 77.8 | 0.164 |
| Surgical procedure (%) | |||||||
| Osteosynthesis | 55.7 | 55.8 | 53.3 | 56.6 | 60.9 | 77.8 | 0.175 |
| Partial replacement | 42.2 | 37.2 | 44.0 | 41.9 | 39.1 | 22.2 | |
| Total replacement | 2.1 | 7.0 | 2.7 | 1.5 | - | - | |
| Comorbidity | |||||||
| Chronic kidney disease | 15.2 | 2.3 | 3.2 | 17.2 | 57.6 | 100 | <0.001 |
| Cardiovascular risk (any) | 87.2 | 69.8 | 81.4 | 92.5 | 96.7 | 100 | <0.001 |
| Hypertension | 74.3 | 48.8 | 65.5 | 82.5 | 90.2 | 77.8 | <0.001 |
| Diabetes (type I and II) | 26.8 | 32.6 | 21.8 | 27.8 | 39.1 | 55.6 | 0.002 |
| Chronic cardiac insufficiency | 9.5 | 7.0 | 10.0 | 14.7 | 25.0 | 22.2 | 0.002 |
| Ischemic heart failure | 12.8 | 11.6 | 8.8 | 15.9 | 19.6 | 0.0 | 0.006 |
| Pharmacologic treatment | |||||||
| Antiplatelet | 34.2 | 34.9 | 32.8 | 35.0 | 34.8 | 55.6 | 0.677 |
| Oral Anticoagulant | 20.7 | 2.3 | 19.3 | 21.9 | 31.5 | 11.1 | 0.002 |
eGFR: estimated glomerular filtration rate; SD: standard deviation; significant differences among eGFR ranges are marked in bold.
Table 1 summarizes the demographic characteristics of the study population. Patients with and eGFR ≥90 at admission were younger. We observed a decrease in eGFR values with increasing age (β = -0.967 mL/min/1.73m2 per year; 95%CI: -1.152 to -0.781; p < 0.001). As for the place of residence, no statistically significant differences were found; however, overall, individuals who lived in rural areas showed an eGFR <15 mL/min/1.73m2. In all eGFR groups, institutionalization increased ~ 20% at discharge.
The most frequent type fracture was extracapsular, which increased with decreasing eGFR ranges. Osteosynthesis was the most performed procedure, mostly in patients with eGFR <15 mL/min/1.73m2; total hip replacement was performed when eGFR ≥30 mL/min/1.73m2.
An increasingly higher number of patients with lower eGFR values (from 2.3 to 31.5%, p = 0.002; OR per mL/min/1.73m2 = 0.528; 95%CI: 0.296 to 0.760; p = 0.003) were under oral anticoagulant treatment. However, there were no statistically significant differences among patients taking any antiplatelet treatment.
As for laboratory tests at admission, besides the clear differences in creatinine and urea levels (both highly increased with decreasing eGFR), we found statistically significant differences in haemoglobin, glucose, and PTH serum levels (Table 2). With pairwise comparisons, we confirmed decreasing haemoglobin and increasing PTH with decreasing eGFR. Moreover, we determined differences in glucose levels at admission, mainly due to the differences between patients within the eGFR ranges 29-15 and 89-60 mL/min/1.73m2 (155±56 vs 134±33; p = 0.033).
Table 2. Biochemical values (mean±standard deviation) at admission of older patients who suffered hip fracture and were surgically treated based on the estimated glomerular fraction rate range.
| Admission eGFR | ≥90 | 89-60 | 59-30 | 29-15 | <15 | p-value |
|---|---|---|---|---|---|---|
| (mL/min/1,73m2) | (n=43) | (n=409) | (n=389) | (n=92) | (n=9) | |
| Haemoglobin (g/dL) | 12.5±2.2 | 13.0±1.6 | 12.5±1.7(388) | 11.3±1.7 | 11.5±1.2 | <0.001 |
| Lymphocyte count (x103/µL) | 1.3±0.7 | 1.3±1.1 | 1.3±0.7(388) | 1.2±0.7 | 1.2±0.8 | 0.574 |
| Albumin (g/dL) | 3.9±0.5(35) | 3.9±0.4(344) | 3.9±0.4(336) | 3.9±0.5(81) | 3.6±0.7(7) | 0.353 |
| Glucose (mg/dL) | 134±33 | 138±42 | 146±54(384) | 155±56 | 144±34 | 0.031 |
| PTH (pg/mL) | 54.0±34.3(10) | 58.4±32.0(127) | 71.5±46.0(138) | 120.8±82.7(41) | 132.8±64.8(3) | <0.001 |
| VitaminD (ng/mL) | 13.6±10.9(11) | 11.5±8.5(121) | 12.5±8.9(134) | 12.6±9.9(41) | 7.7±-(1) | 0.785 |
| Creatinine (mg/dL) | 0.6±0.1 | 0.8±0.1 | 1.2±0.2 | 2.0±0.4 | 5.2±1.8 | <0.001 |
| Urea (mg/dL) | 33.7±9.5 | 43.5±12.4(398) | 61.3±19.0(387) | 106.4±38.3 | 122.6±45.2 | <0.001 |
(n): valid n for specified cell; PTH: paratohormone; significant differences are marked in bold.
We observed a statistically significant relationship between the eGFR and functional status of the patient (Table 3) based on different CGA variables: the lower the eGFR value the worse the functional status, which was manifested by the need of some type of support, measured using the Physical Red Cross scale.
Table 3. Description of the functional status of older patients who suffered hip fracture and were surgically treated based on the estimated glomerular fraction rate range.
| Admission eGFR (mL/min/1,73m2) | ≥90 | 89-60 | 59-30 | 29-15 | <15 |
|---|---|---|---|---|---|
| Katz Index | n=40 | n=393 | n=372 | n=91 | n=9 |
| A | 40.0% | 37.2% | 29.0% | 17.6% | 44.4% |
| B | 10.0% | 15.0% | 17.2% | 18.7% | 11.1% |
| C | 20.0% | 16.0% | 19.6% | 26.4% | 0.0% |
| D | 2.5% | 13.0% | 12.6% | 16.5% | 11.1% |
| F | 12.5% | 7.4% | 9.1% | 11.0% | 11.1% |
| G | 2.5% | 3.6% | 6.2% | 4.4% | 11.1% |
| Barthel Index | n=40 | n=389 | n=371 | n=90 | n=9 |
| 100 | 37.5% | 22.1% | 14.6% | 10.0% | 22.2% |
| 60-95 | 37.5% | 54.0% | 59.8% | 63.6% | 44.4% |
| 40-55 | 25.0% | 15.9% | 15.1% | 18.9% | 22.2% |
| 20-35 | 0.0% | 5.4% | 8.4% | 6.7% | 0.0% |
| <20 | 0.0% | 2.6% | 2.2% | 1.1% | 11.1% |
| Lawton-Brody Index | n=42 | n=390 | n=368 | n=89 | n=9 |
| 0 | 21.4% | 19.5% | 24.2% | 21.3% | 11.1% |
| 1 | 19.0% | 11.5% | 14.7% | 27.0% | 22.2% |
| 2 | 11.9% | 19.0% | 18.8% | 18.0% | 0.0% |
| 3 | 14.3% | 11.8% | 10.3% | 10.1% | 33.3% |
| 4 | 2.4% | 5.9% | 5.7% | 5.6% | 0.0% |
| 5 | 7.1% | 3.6% | 4.1% | 0.0% | 22.2% |
| 6 | 0.0% | 4.6% | 4.1% | 2.2% | 0.0% |
| 7 | 9.5% | 9.0% | 8.7% | 10.1% | 11.1% |
| 8 | 14.3% | 15.1% | 9.5% | 5.6% | 0.0% |
| Physical Red Cross Scale | n=42 | n=396 | n=378 | n=90 | n=9 |
| 0 | 143% | 5.3% | 2.6% | 0.0% | 0.0% |
| 1 | 38.1% | 29.8% | 29.4% | 17.8% | 22.2% |
| 2 | 19.0% | 34.6% | 40.2% | 40.0% | 44.4% |
| 3 | 28.6% | 25.5% | 23.5% | 38.9% | 22.2% |
| 4 | 0.0% | 4.5% | 3.7% | 3.3% | 11.1% |
| 5 | 0.0% | 0.3% | 0.5% | 0.0% | 0.0% |
We observed longer mean length of hospital (LOS) stays of patients with low eGFR values (Table 4). This extended stay coupled with longer mean waiting times to surgery, significantly increased in patients with lower eGFR values. However, the number of patients operated within the first 24 hours or 48 hours was similar in all groups (confirmed by pair-wise comparisons).
Similar incidence of postoperative surgical complications were found in the five study groups, but patients with lower eGFR values showed higher incidence of medical postoperative complications.
Specifically, at lower eGFR at admission there was increased exacerbation of postoperative renal dysfunction, leading to increased incidence of hyperkalaemia (OR = 0.949; 95%CI: 0.925 to 0.972; p <0.001). Likewise, higher incidence of digestive complications was observed in patients with eGFR in the 29-15 mL/min/1.73m2 (p = 0.0048) range, as well as increased need for blood transfusion, particularly in patients with eGFR <60 mL/min/1.73m2 onwards. Incidence of cardiac and respiratory complications increased with decreasing eGFR ranges, although without statistical significance.
As for in-hospital mortality, no statistically significant differences were observed between eGFR ranges; however, a noticeable increase in the most underdiagnosed group of patients (eGFR 59-30 ml/min/1.73m2) was identified. The 30-day mortality rate showed a staircase pattern, increasing with decreasing eGFR. Ninety days after hospital discharge, we had all the data for 502 patients and found a statistically significant increase in the mortality rate with lowering eGFR values at the time of hospital admission (Table 4).
Table 4. Outcome measurements of surgically treated older patients with hip fracture on potential CKD stages based on the estimated glomerular fraction rate range.
| Admission eGFR ranges (mL/min/1,73m2) | p-value | ||||||
|---|---|---|---|---|---|---|---|
| ≥90 | 89-60 | 59-30 | 29-15 | <15 | |||
| (n=43) | (n=409) | (n=389) | (n=92) | (n=9) | |||
| Quantitative variables | β (95%CI) | mean ± standard deviation | |||||
| Length of stay | 0.014 | 8.7±4.5 | 8.4±4.1 | 8.7±4.1 | 9.8±3.9 | 9.7±2.2 | 0.002 |
| (-0.031 to -0.004) | |||||||
| p=0.011 | |||||||
| Time to surgery | -0.011 | 2.4±2.5 | 2.8±2.7 | 2.9±2.5 | 3.5±2.4 | 3.0±1.8 | 0.024 |
| (-0.019 to -0.003) | |||||||
| p=0.007 | |||||||
| Qualitative variables | OR (95%CI) | % | p-value | ||||
| TTS <24h | 1.011 (1.002 to 1.019) | 20.9 | 21.8 | 16.7 | 13.0 | 11.1 | 0.203 |
| p = 0.016 | |||||||
| TTS <48h | 1.010 (1.003 to 1.017) | 39.5 | 39.4 | 35.7 | 26.1 | 11.1 | 0.074 |
| p = 0.003 | |||||||
| Surgical postoperative complications | |||||||
| Any | 18.6 | 25.6 | 27.2 | 25.0 | 11.1 | 0.623 | |
| Seroma | 14.0 | 19.2 | 22.8 | 19.6 | 11.1 | 0.498 | |
| Wound bleeding | 4.7 | 3.7 | 3.6 | 5.4 | 0.0 | 0.887 | |
| Medical postoperative complications | |||||||
| Any | 0.983 (0.974 to 0.991) | 65.1 | 73.1 | 79.6 | 89.1 | 88.9 | 0.002 |
| p <0.001 | |||||||
| Renal | 0.984 (0.977 to 0.991) | 20.9 | 30.0 | 34.9 | 52.2 | 11.1 | <0.001 |
| p<0.001 | |||||||
| Digestive | 23.3 | 23.8 | 23.0 | 38.0 | 22.2 | 0.048 | |
| Cardiac | 4.7 | 4.9 | 9.0 | 10.9 | 0.0 | 0.085 | |
| Respiratory | 9.3 | 15.7 | 16.0 | 19.6 | 22.2 | 0.629 | |
| Neurologic | 7.0 | 15.2 | 17.6 | 18.5 | 11.1 | 0.400 | |
| Transfusion | 0.983 (0. 977 to 0.991) | 34.9 | 32.8 | 42.6 | 56.5 | 77.8 | <0.001 |
| p <0.001 | |||||||
| Mortality | |||||||
| In-hospital | 0.0 | 2.2 | 4.6 | 3.3 | 0.0 | 0.229 | |
| 30-day | 0.0982 (0.970 to 0.997) | 0.0(39) | 4.4(385) | 7.6(369) | 9.0(89) | 11.1(9) | 0.107 |
| p = 0.016 | |||||||
| 90-day | 0.0979 (0.969 to 0.990) | 0.0%(22) | 12.3(211) | 22.7(211) | 34.6(52) | 16.7(6) | <0.001 |
| p < 0.001 | |||||||
OR: odds ratio (only significant values); 95%CI: 95% confidence interval; (n): valid n per cell; TTS: time to surgery; significant differences are marked in bold.
Six patients died before hospital discharge: one from lung cancer, two from heart diseases (ischemic heart disease and congestive heart failure), and three due to multiorgan failure associated to significant comorbidity.
Chronic Kidney Disease patients
Eleven (7.7%) from the 142 CKD older patients had been receiving dialysis before suffering a hip fracture. We determined significant differences between the basal situation and at hospital admission (n = 102) in lymphocyte count (p <0.001), calcium (p <0.001, n = 33), glucose (p 0.001), and phosphorus (p= 0.029, n = 30). Upon hospital discharge, there was a significant decrease in haemoglobin and albumin serum levels compared to hospital admission levels (p <0.001). The comparison between the basal situation and the discharge status (n = 88) revealed significant differences in lymphocyte count (p <0.001) and serum albumin (p <0.001) (Table 5).
Table 5. Basal, hospital admission, and discharge laboratory data (mean and standard deviation).
| Biochemical parameter (unit) | Basal situation | At admission | At discharge | |||
|---|---|---|---|---|---|---|
| n | x_±SD | n | x_±SD | n | x_±SD | |
| eGFR (mL/min/1.73m2) | 102 | 40.6±19.1 | 141 | 38.5±19.6 | 119 | 41.6±22.9 |
| Creatinine (mg/dL) | 101 | 1.7±1.3 | 142 | 1.8±1.1 | 121 | 1.7±1.1 |
| Urea (mg/dL) | 103 | 77.1±36.9 | 142 | 83.4±41.2 | 119 | 84.7±45.8 |
| Haemoglobin (g/dL) | - | - | 141 | 11.7±1.9 | 139 | 10.3±1.1 |
| Lymphocyte count (x103/µl) | 103 | 1.7±0.8 | 141 | 1.2±0.7 | 140 | 1.2±0.5 |
| Albumin (g/dL) | 6 | 3.8±0.9 | 115 | 3.8±0.4 | 3 | 3.0±0.5 |
| Glucose (mg/dL) | 102 | 110±38 | 141 | 146±47 | - | - |
| Calcium (mg/dL) † | 8 | 9.1±0.7 | 1 | 8.5±0.7 | - | - |
| Phosphorus (mg/dL) † | 3 | 3.3±0.6 | 6 | 3.7±.0 | - | - |
| Paratohormone (pg/mL) † | 2 | 173.7±130.0 | 2 | 100.6±72.6 | - | - |
| Vitamin D (ng/mL) † | 0 | 17.5±12.4 | 9 | 14.3±9.8 | - | - |
Basal: from records up to 6 months before being admitted to the hospital for hip fracture; at discharge: after hip fracture surgery; ?: serum levels of calcium, phosphorus, paratohormone, and vitamin D were only recorded once during the hospital stay, either pre or post-surgically.
It is noteworthy that patients with clinically significant variations in admission eGFR (increases/decreases >5 mL/min/1.73m2) in comparison to baseline values (n = 56) showed higher in-hospital mortality rate than CKD patients without these admission eGFR variations (n = 46) (10.7 vs 2.2%, respectively). From another point of view, 85.7% of the CKD patients who died early after hip fracture surgery showed a clinically significant eGFR variations in comparison to baseline values.
From the 56 CKD hip fracture patients with clinically significant eGFR variations, 37 (66.1%) showed decreased eGFR values at admission in comparison to baseline values, with 45.9% presenting eGFR <30 mL/min/1.73m2. Three patients died before hospital discharge. eGFR for the remaining patients at discharge was significantly higher (p = 0.002), but without reaching baseline values (p = 0.024) (Fig. 1A). Conversely, 19 patients showed a clinically significant increase of the eGFR at admission compared to baseline levels; from these, three died before being discharged. This increased eGFR was maintained upon hospital discharge and did not reach baseline values (p = 0.003) (Fig. 1B).
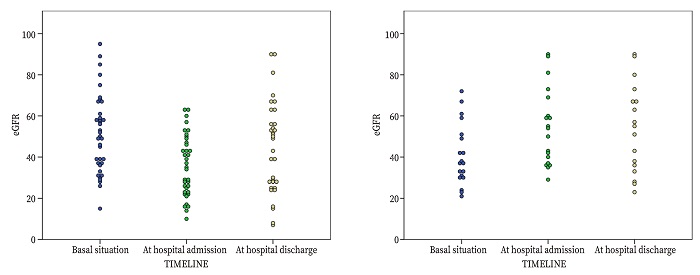
Figure 1. Estimated glomerular filtration rate misbalance through the hip fracture process in chronic kidney disease patients. A. Patients with a significant decrease of the estimated glomerular filtration rate upon admission. B. Patients with a significant increase of the estimated glomerular filtration rate upon admission.
Discussion
In this study, we show that lower values of eGFR, a widely used parameter in early evaluations of older patients who suffer hip fracture, is a bad prognostic factor in terms of postoperative complications and mortality.
At admission, half of our study population (942 patients who suffered hip fracture) had an eGFR >60 and 101 patients <30 mL/min/1.73m2; 82.2% of the individuals with an eGFR between 60 and 30 at admission had no prior medical history of CKD, which may imply CKD underdiagnoses among the aged13.
Cardiovascular comorbidity of patients with eGFR <60 ml/min/1.73m2 is significantly higher than that of the patients with higher eGFR at admission. The relationship between the incidence of cardiovascular pathology and renal dysfunction, i.e., cardiorenal syndrome, has been previously described17 and may explain the worse prognosis of these patients.
Our results are in line with other studies that report a reduction of eGFR values with increasing age. Advanced age has also been associated with a higher rate of complications and mortality after a hip fracture10,18. We observe an increasing trend in the incidence of extracapsular hip fractures with decreasing eGFR, but without statistical significance. This type of trochanteric fractures have been traditionally associated with the frailest patients and we should bear in mind that the mean age of our study population was greater than that reported elsewhere10,12.
Moreover, we measured the functional status of the patients through the CGA and show that lower eGFR values at hospital admission relate to a worse functional status of the patient. Our results are in line with other works in which the authors defend that kidney-related diseases have a high impact on the functional ability and mortality rate of hip fracture patients19.
Renal dysfunction implies some impaired physiologic conditions, including metabolic homeostasis and anaemia12. Therefore, our results should point to lower haemoglobin and higher PTH at admission of patients with lowered eGFR values, as we show. The higher incidence of anaemia may be related to a greater number of postoperative blood transfusions. This does directly relate to a worse prognosis20, but it may reflect the higher incidence of fractures in CKD patients21,22. On the other hand, blood transfusions in patients with impaired renal function requires careful management due to possible volemia alterations.
The clinical situation of a patient with lower eGFR values must be optimized before surgical treatment, with the consequent delay of hip fracture treatment6. The pharmacodynamics (i.e., half-life) of medication may differ from the reference levels, and hereafter widens the clinical optimization of hip fracture patients before surgery. LOS and mean TTS significantly increase with decreasing eGFR at admission, which may indicate that the management of these patients is more complex. There is no significant relationship between eGFR value ranges and surgical postoperative complications. Contrarily, we show a significant increase in postoperative medical complications, which is in agreement with the observed increased LOS. The intensification of renal impairment is significantly more prevalent in patients with lower eGFR at admission, along with postoperative constipation. Although there are no statistically significant differences in the increase of incidence of cardiac and respiratory complications versus eGFR values, the trend should be studied further.
There is a pattern of increasing mortality, but without significance in early mortality and a noticeable increase in the in-hospital mortality rate of most underdiagnosed patients (eGFR 59-30 mL/min/1.73m2). As for the 90-day follow-up, the mortality increases with lower eGFR values. Some authors have pointed out excess mortality after hip fracture in haemodialysis patients7,23,24, emphasizing that hip fracture is a critical event for the survival of this group of patients. A higher mortality rate in patients with advanced CKD has been shown in femoral neck fracture patients14, and in all types of hip fractures in the longer term19.
In the diagnosed CKD patients in this work, we observe a deterioration of renal function related to the hip fracture, manifested by increased creatinine, urea, phosphorus, and glucose values, and decreased haemoglobin, lymphocyte count, and calcium values. These findings indicate the need of a multidisciplinary careful management of older CKD patients who suffer a hip fracture. Changes in laboratory values have been reported by other authors8,25, but no paired baseline data have been previously studied. To the best of our knowledge, our study examines for the first time the evolution of these laboratory values during a hip fracture care process, considering the baseline values of each patient. A relevant aspect of our study is the detection of patients whose eGFR varies by more than 5 mL/min/1.73m2 from baseline values and are associated with a worse prognosis. This occurs in cases with decreased or increases eGFR values and, for the time being, we have no clear explanation. This eGFR variation may indicate greater lability of these patients compared to those who present a more stable renal function; this early renal autoregulatory dysfunction may be a warning of CKD progression26.
There are some limitations to this study. Firstly, although the study population (942 patients) is large compared to other similar single-centre studies, the number of patients with eGFR values <15 mL/min/1.73m2 is still small. Secondly, the longer follow-up of patients, 90 days after hospital discharge, showed an attrition rate of 46.7%. Lastly, we could not establish baseline laboratory parameters before the admission of the patients for hip fracture.
We conclude that admission eGFR values provide information on the outcome of surgically treated older adults who suffer a hip fracture. Lower eGFR values implies a worse outcome, in terms of postoperative complications and mortality. We therefore suggest a protocol for the detection and follow-up of patients according to their renal function on hospital admission for hip surgery (Appendix I).
Initially, we noted a high incidence of older adults with hip fracture (without a prior diagnosis of CKD) with decreased eGFR levels at admission. On the other hand, significant eGFR variations upon hospital admission after a hip fracture may be associated with increased in-hospital mortality of CKD patients. We also report a significant relationship between lower eGFR value ranges with 90-day mortality rate after hip fracture surgery.
Our findings highlight the need of careful monitoring in patients with impaired renal function who are undergoing surgical treatment for hip fracture. To record and analyse eGFR values upon hospital admission of older adults who suffer a hip fracture may facilitate the assignment of resources throughout the process of hip management.














