Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista Española de Sanidad Penitenciaria
versión On-line ISSN 2013-6463versión impresa ISSN 1575-0620
Rev. esp. sanid. penit. vol.19 no.2 Barcelona 2017
Brief update on diabetes for general practitioners
Actualización breve en diabetes para médicos de atención primaria
A. Barquilla García
EAP Trujillo (Medical Centre of Herguijuela and Conquista de la Sierra)
ABSTRACT
Diabetes includes a group of metabolic disorders in which there is hyperglycemia. This can be due to impaired insulin secretion, insulin action or both. Chronic hyperglycemia is associated with serious long-term complications in several organs, especially in the eyes, kidneys, nerves, heart and blood vessels. In our country this disorder affects 13.8% of the population. There are several types of diabetes although most patients suffer type 2 diabetes.
We set out to review the diagnostic process, screening recommendations, prevention strategies, initial assessment upon diagnosis, therapeutic targets regarding both blood glucose levels and the other vascular risk factors while also considering healthy lifestyles and brief references to medications recommended in each section.
Key words: prisons; diabetes mellitus; prediabetic state; diagnosis; straining; hypertension; dyslipidemia; obesity; Spain.
RESUMEN
Denominamos diabetes a un grupo de enfermedades metabólicas caracterizadas por hiperglucemia. Ésta puede ser consecuencia de defectos en la secreción de insulina, en su acción, o en ambas. La hiperglucemia crónica de la diabetes se asocia con daño a largo plazo en diferentes órganos, especialmente en los ojos, riñones, nervios, corazón y vasos sanguíneos. En nuestro país esta patología afecta al 13,8% de la población. Hay varios tipos de diabetes, pero la mayor parte de los afectados sufren la diabetes tipo 2.
En este artículo vamos a revisar el proceso diagnóstico, las recomendaciones de cribado, las actuaciones para prevenir su aparición, el estudio inicial que debemos realizar tras el diagnóstico, los objetivos del tratamiento tanto en lo referente a la glucemia cómo a los demás factores de riesgo vascular, sin olvidar el estilo de vida y haremos unas breves referencias a los fármacos recomendados en cada apartado.
Palabras clave: prisiones; diabetes mellitus; estado prediabetico; diagnóstico; cribado; hipertensión; dislipemia; obesidad; España.
Diabetes
Diabetes includes a group of metabolic disorders in which there is hyperglycemia. This can be due to impaired insulin secretion, insulin action or both. Chronic hyperglycemia is associated to serious long-term complications in several organs, especially in the eyes, kidneys, nerves, heart and blood vessels1.
Classification
Type 1 diabetes mellitus (Type 1 DM) is characterized by the loss of insulin-producing beta cells in the pancreas, leading to complete insulin deficiency.
Type 2 diabetes mellitus (Type 2 DM) is characterized by insulin resistance which is progressively combined with reduced insulin secretion.
Gestational diabetes mellitus (GDM) is diagnosed in the second or third trimester of pregnancy in women without a previous history of DM. Other specific types: monogenic DM (neonatal DM, MODY DM (maturity-onset diabetes of the young) LADA DM (latent autoimmune diabetes of the adult), disorders of the exocrine pancreas (cystic fibrosis, ...) drug-induced diabetes (glucocorticoids, antiretrovirals, ...)1.
Prevalence
In our country, the Di@betes study showed that diabetes affects 13.8% of adults over 18 years old (almost half of which, 6%, remain undiagnosed)2.
Diagnosis
The classic symptoms of untreated diabetes are polyuria (increased urination), polydipsia (increased thirst), weight loss, blurry vision, polyphagia (increased hunger) although these may be absent.
Hyperglycemia progressively affects our organs without developing signs or symptoms. Therefore early diagnosis and management are essential.
We can use four different options to diagnose diabetes1:
— Glycated hemoglobin (HbA1C) ≥6.5%, or
— Fasting plasma glucose (FPG) level ≥ 126mg/dl, or
— Plasma glucose (PG) ≥200mg/dl two hours after a 75 g oral glucose load (OGL),
All of them have to be positive at least twice.— Random plasma glucose (PG) ≥ 200mg/dl with unequivocal signs of hyperglycemia.
There is no need to repeat the determination in this case.
None of the tests is superior to the rest.
HbA1c will be used if the method has been certified by the National Glycohemoglobin Standardization Program (NGSP) and standardized by the Diabetes Control and Complications Trial (DCCT).
Gestational Diabetes
DGM is defined as any degree of glucose intolerance identified from the second trimester of pregnancy. It is recommended that a test to diagnose DM be used (using standard criteria) at first prenatal visit.
The American Diabetes Association (ADA) recommends screening GDM in pregnant women without known prior diabetes at 24-28 weeks either by means of the 75g oral glucose tolerance test (OGTT) or by means of a "two-step" strategy including a 50g nonfasting GL followed by a 100g OGTT if the first is positive three hours later.
The difficulty lies in agreeing the cutoff points which define the problem since there is a continuous relation between maternal plasma glucose and perinatal outcomes. These variability regarding cutoff points entails an estimated prevalence ranging between 8.8% and 35.5%3.
GDM can damage the health of the fetus (abnormalities, miscarriage, accelerated growth, ...) and the mother, for whom it entails an important risk factor for the development of type 2 DM in the future.
Women with GDM will need further assessment between week 4 and 12 after delivery to rule out overt DM (with plasma glucose according to the National Institute for Health and Care Excellence— NICE4, with OGTT according to the ADA1).
Screening should be repeated every three years if normal and every year if any prediabetes stage is detected.
Categories of increased risk for diabetes
DM is a continuous process and we can find a special predisposition towards its development among patients with plasma glucose levels between certain limits1:
— Impaired fasting glucose (IFG): FPG between 100 and 125 mg/dl,
— Impaired glucose tolerance (IGT): 2-hr PG between 140 and 199 mg/dl,
— HbA1c between 5.7 and 6.4%
All tests are equally appropriate and for all tests the risk is continuous becoming disproportionately greater at higher ends of the range.
Screening
Diabetes has a long-term asymptomatic period during which already micro and macro-vascular complications start to develop. This makes screening strategies most advisable and all guidelines recommend carrying out screening for diabetes in high-risk patients since there is no evidence on the effectiveness of community screening.
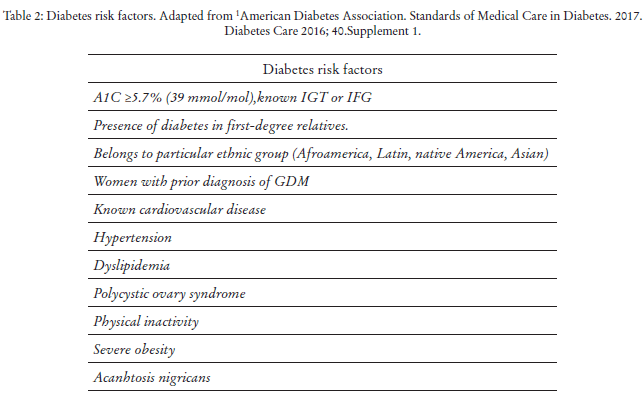
The strategy recommended by the NICE guidelines is to use a validated self-assessment questionnaire (FINDRISK) (Table 1) for people aged over 40 with no further risk factors and those aged 25-39 from high-risk and vulnerable groups (Table 2). For scores under 15 (low or intermediate risk) it is recommended to reassess the risk at least every 5 years. For scores of 15 or more (high risk), blood test should be offered to determine FPG or HbA1c and if normal, the questionnaire should be repeated at least every three years. If prediabetes is detected, prevention measures should be offered and the risk should be reassessed every year.
Patients with prediabetes should be offered training and support, including self-management programs to develop and keep healthy habits which can prevent or delay the appearance of diabetes.
These programs should be aimed at achieving and keeping 7% weight loss of initial weight, physical activity of moderate intensity (brisk walking for at least 150 minutes every week) and appropriate diet (preferably Mediterranean but according to individual preferences low— glycemic index diets, low—carb diets and high-protein meal plans can be acceptable)1,5.
Once the increased risk for diabetes has been identified, the detection and management of modifiable cardiovascular risk factors is a priority.
Treatment with metformin 1 for the prevention of T2DM should be considered for patients with prediabetes, especially with BMI≥35 kg/m2, aged under 60, women with prior GDM and those with persisting elevation of HbA1C despite correct modifications of lifestyle.
The ADA supports the high - unsaturated fat Mediterranean diet as a means to prevent diabetes. (The quality of fat is more important than its quantity).
Initial evaluation (Comprehensive Medical Assessment)
Newly diagnosed patients require complete medical assessment to classify the type of diabetes, identify cardiovascular risk factors, already developed complication, other comorbidities and medications (Table 3).
Evaluation of comorbidities other than vascular disorders
The assessment of diabetes-related complications and common disorders affecting diabetic patients can complicate the management of the disease.
Liver, pancreas, endometrial, colon/rectal, breast and bladder cancer; fatty liver (hepatic steatosis); fractures; impaired hearing; obstructive sleep apnea; periodontal disease; low testosterone in men; HIV; anxiety disorders, depression, cognitive impairment, eating behavior disorders and severe mental disorders.
Immunization
All diabetic patients need the following vaccines1:
— Influenza vaccine
— Hepatitis B vaccine
— Pneumococcal vaccine
PPSV23 (pneumococcal polysaccharide vaccine) for patients aged 2 to 64.
PCV13 (pneumococcal conjugate vaccine) for patients 65 or older (we should always leave at least one year after previous vaccination with PPSV23).
Targets
From the very beginning we should initiate therapeutic education and agree with the patient on the goals to achieve.
PLASMA GLUCOSE
HbA1c should be determined at least twice a year in patients with stable control of PG or every three months in those who modify their treatment or do not achieve previous goals.
The reasonable target for non-pregnant adults is HbA1C under 7%.
Tougher requirements (HbA1c under 6.5) are needed for individuals with no risk of hypoglycemia and especially in newly diagnosed cases treated with lifestyle modifications or metformin and no cardiovascular risk (CVR).
Higher values (HbA1c under 8%) are acceptable in patients with a history of severe hypoglycemia, reduced life expectancy or advanced micro and macrovascular complications.
Whenever these goals are not achieved we should measure preprandial plasma glucose (goal: 80-130 mg/ dl) and postprandial plasma glucose (goal <180 mg/dl).
We should question patients on symptoms of hypoglycemia in each visit and be aware of PG levels under 70 mg/dl.
The regularity of PG determination will depend on the degree of control and the type of treatment. Always question patients on signs of hypoglycemia. Table 4.
BLOOD PRESSURE (BP)
<140/90mmHg (for high cardiovascular risk patients or those with chronic kidney disease <130/80mmHg should be considered if achievable without excessively aggressive management)6.
Measure BP in each visit.
LIPIDS
Total cholesterol, LDL-cholesterol and HDLcholesterol have been recommended as risk markers and non-HDL-Chl as alternative markers. Triglycerides provide additional information.
The main target of treatment should be LDLChl but total cholesterol or non-HDL can be used if others are not available.
To determine the effect of lipid lowering medications or dose modifications we should measure lipids 6-8 weeks later and when appropriate levels are achieved, every 6-12 months.
LDL
In the presence of vascular disease the target value is LDL cholesterol <70 mg/dl (or non-HDL<100mg/dl). These values are also applicable in the absence of cardiovascular disease but in the presence of target organ lesion or any vascular risk factor7.
In the absence of vascular disease the target value will be LDL < 100mg/dl (or non-HDL <130 mg/dl)
Fasting triglycerides should remain under 150 mg/dl with lifestyle modifications and the use of fibrates (fenofibrate if combined with statins) should be considered for levels over 200 mg/dl and low HDL-cholesterol. However, their role in improving vascular risk remains unclear.
OBESITY
Measures promoting normal weight (BMI < 25 kg/m2) or progressive weight loss if needed should be implemented1.
SMOKING
The objective is to completely quit smoking. In each contact with patients we should question them on smoking, quantify and assess their degree of dependency and motivation to quit.
ALCOHOL
In each visit we should question patients on the use of alcohol.
Intensive and complete management
1. Of Plasma Glucose
Antidiabetic treatment should be individualized and adapted to each patient's particularities (age, comorbidity, education, support, economic status, ...) the degree of hyperglycemia and the evolution of the disease.
The first option upon diagnosis always includes recommendations on diet and physical activity, but even then almost all guidelines recommend the initiation of metformin (low doses at the beginning and progressively higher until maximum effective dose: 2g/d).
A wide range of antidiabetic medications is available (metformin, sulfonylureas, glinides, alpha-glucosidase inhibitors, glitazones, dipeptidyl peptidase inhibitors (DPP-4 inhibitors), glucagon-like peptide 1 (GLP-1) receptor agonists, sodium-glucose co-transporter 2 (SGLT2) inhibitors, insulins).
Patient-related features and pharmacological factors determine the best therapeutic option.
The main scientific associations worldwide periodically publish algorithms to guide the use of these medications1, 4, 8, 9.
2. Of Blood pressure
If > 120/80mmHg promote healthier lifestyles (reduced salt intake, engage physical activity, weight loss, moderate alcohol consumption, ...)
If > 140/80 mmHg initiate medication.
If >160/100 mmHginitiate dual therapy.
Preferably, angiotensin converting enzyme (ACE) inhibitors or angiotensin II receptor blockers (ARBs) should be used and are the most appropriate choice for albumin/creatinine ratios over 30 mg/g. Renal function should be monitored by means of glomerular filtration rate (GFR) and plasma potassium and both medications should never be combined. They should neither be used in pregnant women nor women of childbearing age.
Whenever needed an additional medication should be used, in which case calcium antagonists would be the most appropriate choice and thiazides for obese and patients over 60 years old especially if they have isolated systolic hypertension.
In the presence of heart failure or coronary artery disease (CAD) we should associate beta blockers (BBs) and in case of prostatic hyperplasia, alpha-blockers.
For resistant hypertension, mineralocorticoid receptor antagonists (MRAs) may be a good choice provided that potassium levels are monitored.
In case of combination therapy, one medication should be used at night.
3. Of Lipids
Nonpharmacological measures should always be implemented to improve lipid profile: avoid overweight and obesity, reduced intake of saturated fat, trans-fatty acids and cholesterol while increasing the use of omega-3 fatty acids, fiber and plant sterols as well as increased physical activity.
Statins should be used (if there is no intolerance) at moderate doses provided that there is established cardiovascular disease or high vascular risk (REGICOR > 10%) regardless of plasma cholesterol although regular monitoring is recommended to guide therapy.
Their use is also highly recommended for patients with an evolution longer than 15 years with established nephropathy (GFR<45 ml/min/ 1.73 m2 or albumin- to-creatinine ratio >300 mg/g).
In the absence of vascular disease and for low-risk patients, it seems reasonable to initiate statins when LDL-levels surpass pre-established targets in spite of nonpharmacological measures.
If despite appropriate measures targets are not achieved, ezetimibe should be added and combination with bile acid sequestrants or nicotinic acid should be considered.
In case of statin intolerance, ezetimibe, bile acid sequestrants and nicotinic acid should be considered alone or combined.
When using statins we should be aware of their specific power and basal LDL levels.
— High-intensity statins (they lower LDL-c by ≥ 50%): atorvastatin 40-80mg; rosuvastatin 20-40 mg
Fasting triglycerides should remain under 150 mg/dl with lifestyle modifications and the use of fibrates should be considered (fenofibrate if combination with statins is needed) for values over 200 mg/dl or if HDL-cholesterol is low. However, their role on vascular risk remains unclear.
If fasting levels approach 500mg/dl fibrates should be used to prevent pancreatitis.
4. Of obesity
Time-bound objectives should be established together with meal plans adapted to the needs and preferences of patients and regular physical activity.
Monitoring by a nutritionist can be more effective.
In our country there is no authorized medication for this purpose but we should consider our patient's body weight when initiating antidiabetic medication.
5. Of smoking
We should offer brief recommendations upon every visit and if necessary due to continuous failed smoking cessation, prescribe the appropriate medication (replacement therapy, bupropion, varenicline) or derivation to specialists.
6. Use of antiplatelet drugs
The use of aspirin as secondary prevention is recommended (75-162 mg/d).
For patients allergic to aspirin, clopidogrel should be used (75 mg/d).
For the first year after an acute coronary event combined therapy with clopidogrel and aspirin seems reasonable.
There is not enough evidence to recommend antiplatelet drugs as primary prevention although the ADA states that it can be considered for patients over 50 years old or with an added risk factor.
Management of lifestyle
THERAPEUTIC EDUCATION
From the moment diabetes is diagnosed we should plan individual and group education strategies to help patients achieve targets.
The main contents should include1
Information on the disease (what is DM, types of DM and risk factors), meal plans, physical activity, acute and chronic complications of DM, smoking, diabetic foot, oral antidiabetic drugs; treatment adherence, management of hypoglycemia, Self-assessment: control of PG and other parameters and interpretation and use of results to self-manage decisions; Special situations: trips, intercurrent disease, etc.
WEIGHT CONTROL
To achieve normal weight or reduce overweight educational strategies should be implemented with the support of experts, aimed basically at promoting individualized meal plans and physical activity for each patient11-13.
NUTRITION
Evidence supports that Mediterranean diet, with low high-glycemic index carbohydrates, is recommended although in order to promote adherence, individual preferences should be taken into account. There is evidence on other diets such as low-glycemic index diets, low-carb diets and high-protein meal plans being useful in the control of plasma glucose1, 10,12.
PHYSICAL ACTIVITY
Adults with T2DM should at least engage 150 minutes of moderate intensity physical activity a week, in three non-consecutive days.
Physical training should preferably be supervised, including aerobic activity in combination with strength exercise1, 10,12.
References
1. Standards of Medical Care in Diabetes 2017. Diabetes Care. 2016;40 Suppl 1:S1-S132. [ Links ]
2. Soriguer F, Goday A, Bosch-Comas A, Bordiú E, Calle-Pascual A, Carmena R, et al. Prevalence of diabetes mellitus and impaired glucose regulation in Spain: the Di@bet.es Study. Diabetologia. 2012 Jan;55(1):88-93. [ Links ]
3. Duran A, Sáenz S, Torrejón MJ, Bordiú E, Del Valle L, Galindo M, et al. Introduction of IADPSG crieria for the screening and diagnosis of gestational diabetes mellitus results in improved pregnancy outcomes at a lower cost in a large cohort of pregnant women: the St. Carlos Gestational Diabetes Study. Diabetes Care. 2014;37:2442-50. [ Links ]
4. National Institute for Health and Care Excellence (Internet). London: NICE; 2017 (updated 2016 Nov 15; cited 2017 jan 14). Pathway; (about 1 screen). Available from: http://pathways.nice.org.uk/pathways/diabetes-in-pregnancy. [ Links ]
5. National Institute for Health and Care Excellence (Internet). London: NICE; 2017 (updated 2016 nov 15; cited 2017 jan 14). NICE guideline (NG28); (about 2 screens). Available from: https://www.nice.org.uk/guidance/ng28. [ Links ]
6. Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, et al. 2013 ESH/ESC Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34(28):2159-2219. [ Links ]
7. Catapano AL, Graham I, De Backer G, Wiklund O, Chapman MJ, Drexel H, et al, 2016 ESC/ EAS Guidelines for the Management of Dyslipidaemias: The Task Force for the Management of Dyslipidaemias of the European Society of Cardiology (ESC) and European Atherosclerosis Society (EAS). Developed with the special contribution of the European Assocciation for Cardiovascular Prevention & Rehabilitation (EACPR). Atherosclerosis. 2016 Oct;253:281-344. [ Links ]
8. Jellinger PS, Handelsman Y, Rosenblit PD, Bloomgarden ZT, Fonseca VA, Garber AJ, et al. American Association of clinical endocrinologists and American College of endocrinology guidelines for management of dyslipidemia and prevention of cardiovascular disease: executive summary. Endocrine Practice. 2017 Apr;23(4):479-97. doi:10.4158/ep171764.gl. [ Links ]
9. Diabetes Canada (Internet). Toronto: Diabetes Canada; 2017 (updated 2016 Nov 15; cited 2017 jan 14). Full guidelines; (about 2 screen). Available from: http://guidelines.diabetes.ca/fullguidelines [ Links ]
10. Fundación redGDPS (Internet). Madrid: Fundación; 2017 (citado 14 en 2017). Guía de actualización en diabetes; (about 3 screens). Disponible en: http://www.redgdps.org/guia-de-actualizacionen-diabetes-20161005/. [ Links ]
11. Mediavilla JJ, coord. Guías clínicas: diabetes mellitus (Internet). Badalona: Euromedice; 2015 (citado 14 en 2017). Disponible en: http://2016.jornadasdiabetes.com/docs/Guia_Diabetes_Semergen.pdf. [ Links ]
12. Menéndez E, Barrio R, Novials A, directores. Tratado de diabetes mellitus. Madrid: Editorial Médica Panamericana; 2017. [ Links ]
![]() Correspondence:
Correspondence:
Alfonso Barquilla García
Email: alfonso.barquilla@gmail.com
Text received: 01/03/2017
Text accepted: 21/04/2017