Introduction
The incidence and prevalence of scabies in western countries and Spain are unknown. Over the final decades of the last century, it was regarded as a very rare disease in developed countries and was considered to be practically eliminated, but in fact successive isolated outbreaks have taken place since 1970, especially in enclosed or semi-enclosed communities such as geriatric residences, hospitals and prisons1-8. There were alarms in 2018 and 2019 when the Spanish media, using information that was not always very effectively contrasted, implied that outbreaks were spreading exponentially. A degree of sensationalism could be noted in newspaper headlines such as: “The resurgence of scabies”4, “New outbreak of scabies in Catalonia”5, “Catalonia with seven outbreaks of scabies this year”6, “69 healthcare professionals and 2 family members need treatment in outbreak of crusted scabies at Galdakao hospital”7, “The Salto del Negro, the prison with most cases of scabies in Spain”8, and many others.
In our prison, isolated cases of scabies are detected every year, which have been successfully controlled with permethrin, elimination of contaminated objects and treatment of contacts. However, in recent months we witnessed an unexpected increase of cases amongst new inmates, along with a very worrying number of potential therapeutic failures. The situation forced us to reconsider if the previously established intervention protocols to control the disease were in fact appropriate.
Scabies is an external skin condition caused by the mite Sarcoptes scabiei hominis, which causes characteristic itchy skin lesions. The parasite is transmitted by close contact and sexual relations, although it can also be transmitted by close contact without sex and via infested items, such as bedclothes and towels1-3. The main risk factors for the disease are poverty, homelessness, under-development, overcrowding, malnutrition, sexual promiscuity and poor hygienic conditions1-3,9.
The incubation period from when infestation commences until the time when it starts to present varies from 2 to 6 weeks, except in cases of recurrence, when this period is shorter10-13. In this period, the person affected by the disease may infect others, without presenting any symptoms themselves. The customary diagnosis is clinical and typical skin lesions take the form of trails, blisters and nodules. Secondary lesions may also be seen, such as inflamed papules, signs of scratching, broken skin, eczema and bacterial super-infection. The inflamed papules are almost always present, but more specific lesions such as trails, blisters and nodules, may not be present. In classic scabies, itchiness is common and there is a characteristic distribution of lesions. The mite trails can be seen in the wrists, spaces between the fingers and the back of the feet. The papules often appear on the torso, armpits and thighs. In men, the nodules usually appear on the penis and scrotum1-3.
The aim of this study is to provide clinical and epidemiological data about new cases of scabies observed in a centre for young offenders, and to report on our investigations into the literature and how we found a more effective way to control infestation in enclosed and semi-enclosed communities.
Materials and method
The details of the electronic health records of all the cases of scabies diagnosed in the Young Offenders' Detention Centre of La Roca del Vallès (Barcelona) between November 2018 and November de 2019 were checked.
The cases were visited by a specialist prison primary healthcare team that had years of experience in the clinical diagnosis of scabies and in auxiliary diagnostic tests. The cases were isolated in the nursing ward to enable us to carry out the customary intervention protocol. This consisted of topical treatment with permethrin cream at 5% (Sarcop® 50 mg/g), left for at least 8 hours at night while sleeping. Isolation ended after 24 hours, and permethrin was applied again one week later. In addition to the drug treatment, the patients' personal clothes were changed and their clothing, bedclothes, mattresses, towels and other personal items were treated to eliminate any potential parasite infestation. The infested cells were disinfected and left empty for four days. All nearby contacts (cellmates) were checked and treated.
To check our protocol, we carried out a systematic information search in the Medline (PubMed) database, using the following key words: “scabies community” and “scabies prison”, with the Boolean operator “AND” in both searches. Articles or documents that provided data of interest on dealing with scabies in closed communities, especially prisons, were selected.
Results
Clinical and epidemiological results
A total of 762 inmates entered the centre, of whom 275 were Moroccan, 182 Spanish, 75 Algerian, 28 Romanian, 19 Chilean, 18 Pakistani, 17 Albanians, while the others were from other countries. Over this period, 61 cases of scabies were diagnosed, 39 of which were Moroccan, 11 Algerian, 3 Spanish while the other cases were of different nationalities. 39 of the 61 cases had the pathology detected at the time of entry into the centre and another 11 cases more in the first six weeks during their stay, which matches the potential incubation period. The other patients were diagnosed after spending more than six weeks at the centre and could therefore have been infected in this period.
The scabies was detected mainly amongst North African inmates, 14.7% from Algeria and 14.2% from Morocco, compared to 1.6% Spanish cases. They were all between 18 and 24 years of age, 26 cases did not understand Spanish, 18 cases had no fixed place of abode and at least 12 cases lived in illegally occupied houses.
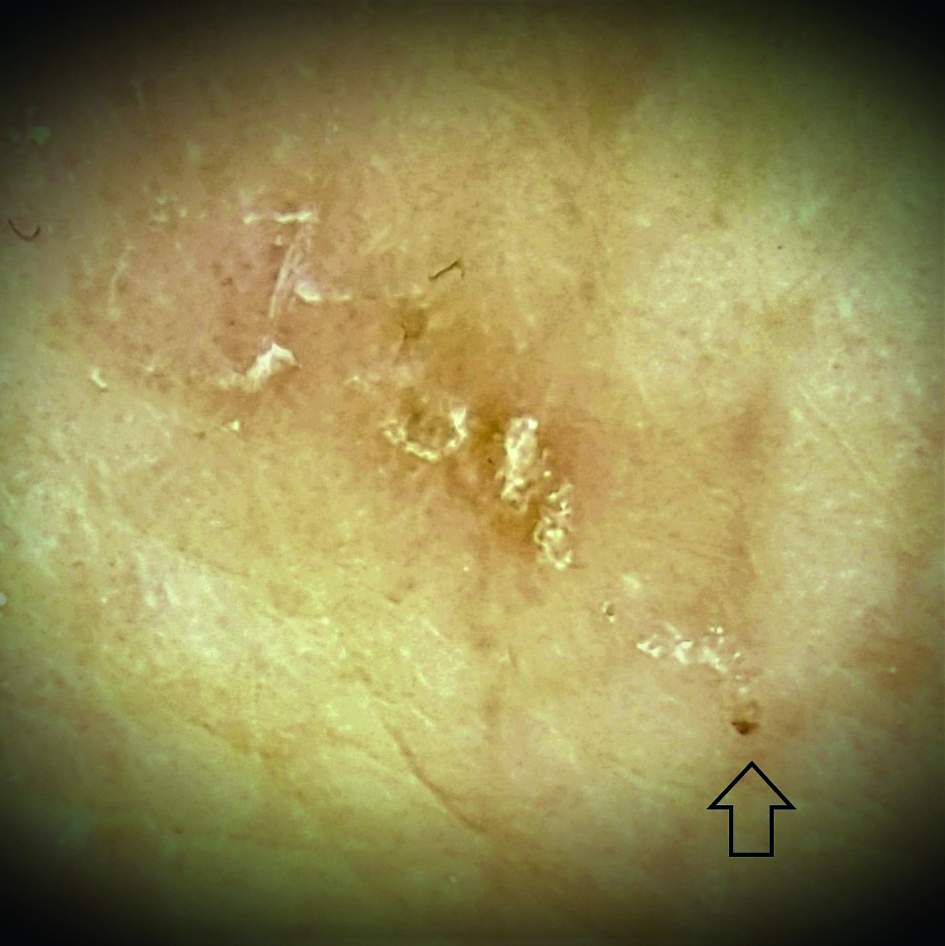
The diagnosed cases presented clinical signs of classical scabies with typical lesions and associated itching that was generally intense and mostly took place at night. They all presented papules, generally on the front of the wrists, the hands (within the palms) and/or the genital area. Mite trails were seen a large number of cases. All the cases were very characteristic and the medical team had little doubt about the accuracy of their diagnosis (Figure 1). In some cases, Indian ink applied to the skin and wiped off with alcohol showed the trails (Figure 2). On other occasions, the images of the dermatoscopic images confirmed the disease by showing mite trails ending in a distinctive “hang glider” image, which corresponds to the front of the parasite's body (Figure 3).
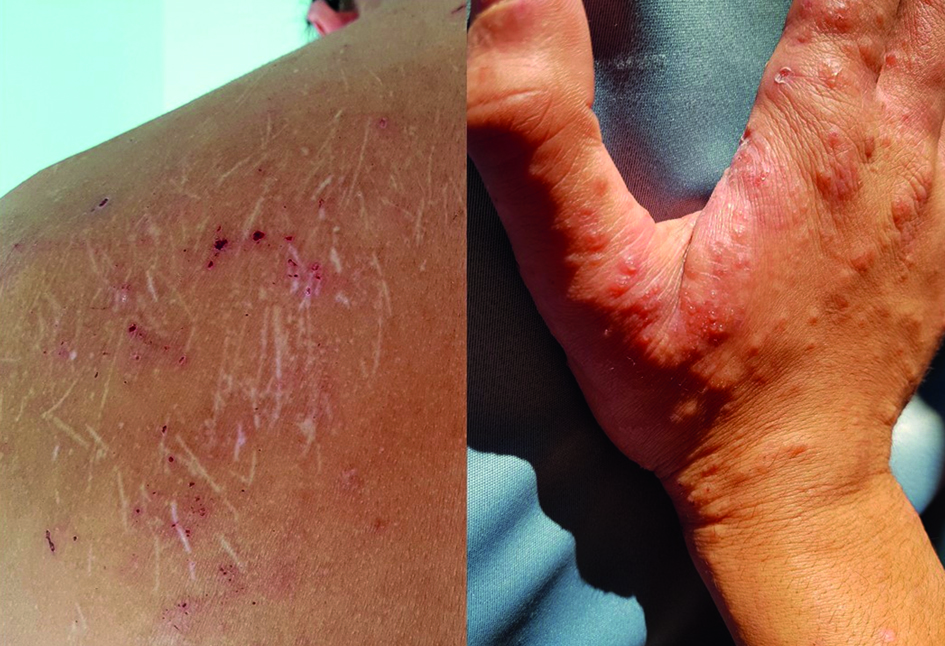
Figure 1. Scabies lesions all over the body in different stages of evolution, with notable signs of scratching.
Therapy consisted of 5% permethrin cream. In eight cases it was considered necessary to apply a second cycle of treatment because of persisting lesions and itching. Five of the repeat treatments were carried out after four weeks, meaning that the first cycle of treatment may well have failed or that another infestation had taken place. A third cycle of topical permethrin had to be applied in two of these cases, although one of them had been to another prison before the third course of treatment.
Bibliographical results
After completing the search mentioned in the materials and methods section, 34 articles were selected. These covered general issues of interest on cases of scabies in enclosed or semi-enclosed communities. 15 articles were about cases of scabies in prison. To update and improve our response protocol, we decided to select six clinical intervention guides, based on expert consensus, with some degree of difference between them, published in Spain, Europe and North America11-16. The bibliography of the guides contained some of the articles mentioned above.
The following results were obtained, based on the literature that was consulted and the experts' recommendations:
Oral and topical ivermectin are highly effective for treating scabies. According to the 2017 European guide, both treatments have a level of evidence based on clinical assays (Ib) and a grade A level of recommendation. Ivermectin and permethrin are both recommended for initial treatment of classical scabies, except in pregnant women and children under 15 kg, where topical permethrin is recommended12.
In comparison to permethrin, the use of ivermectin is still very limited in Spain. A recent intervention protocol for epidemic outbreaks issued by the Catalonian Public Health Agency (2018) makes no mention of ivermectin anywhere as a treatment for epidemic outbreaks in the medical setting11. Another similar document issued by the Madrid Healthcare Council (2018) only recommends ivermectin when topical treatment fails, or as an initial treatment for cases of crusted scabies14.
A new protocol by the Catalonian Public Health Agency recognises the potential advantages of ivermectin for treatment in enclosed or semi-enclosed communities, but does not clarify if it should be regarded as the first choice in treatment with regard to permethrin in such situations16.
Treatment with topical permethrin is only effective when the entire surface of the body is suitably covered, including under the nails, which should be cut back as far as possible. The genitals should also be completely covered with the cream11-17.
The drug of first choice for treating scabies in prison should be oral ivermectin, since it is highly effective and easy to administer. It is also easy to see that the therapy is complied and the risk of outbreaks in this setting is reduced12,13,15-20.
The clinical intervention guide of the FBP (Federal Bureau of Prisons, Washington D. C., USA) regards oral ivermectin as the only drug of first choice for scabies in prison. When topical permethrin is used, the medical staff should check that the cream is correctly applied so as to ensure future outbreaks13.
Clothing. towels and bedclothes may be safely cleared of parasites by washing and drying at temperatures of 50 ºC or higher11-16.
Another safe way to eliminate parasites from clothing and objects that cannot be washed is to put them in sealed plastic bags for a week11-16.
The room occupied by an infected person should be thoroughly disinfected and cleaned with a vacuum cleaner11-16.
Discusión
Persons with scabies have always entered prison18-25. The incidence of cases is higher in prisons because inmates are often socially marginalised, where environmental conditions can favour propagation of the parasite. According to a study at a women's prison in Valencia, and observations made at our centre, scabies is one of the infections that has always worried inmates21. Paradoxically, for socio-cultural reasons, infected North African inmates rarely acknowledge the importance of correctly treating the disease. On the other hand, prison officer and workers who come into contact with inmates are very frightened of being infected, and it is not uncommon for alarms to be raised and supposed cases of infection to be sent to the medical services to ensure that they do not have the disease.
We do not know the possible external epidemiological factors that might explain the recent entry of so many infected inmates. According to our information and the bibliographical search, the series presented here is the largest case study in a such a short time period to be reported in a European prison. The figures observed here exceed the ones seen in the prison of Salto del Negro, in Gran Canaria, which have not been reported in the scientific literature8. Figures alarming as these have only been described in African prisons26. One of our current hypotheses is that there are one or more temporary residences that are infected, which are successively occupied by young marginalised homeless persons who are sexually promiscuous and do not have hygienic habits, who have ended up in prison for theft and drug dealing.
The entry into prison of a certain type of population that not only comes from situations of social exclusion, but also persons from other countries with no family links, with no stable residence or ways to earn a living, may create conditions that can favour infection with and transmission of scabies. In fact, the results suggest that there is a characteristic type of infected person: North African, often unable to speak Spanish or with limited knowledge of the language, who arrives in Spain as part of a phenomenon of unaccompanied minors who live in illegally occupied houses in overcrowded and unsanitary conditions.
The apparently simple treatment methods in our setting are made more complicated for a number of reasons. The patient lacks hygienic habits and it is difficult for him to accept the isolation measures and collaborate with the process of changing clothing. An added problem is ignorance of the language and it is hard for them to understand that when they go to the bathroom or wash their hands, they have to apply the cream again in the areas where it was removed. They also find it hard to accept that they have to cut their nails and stay in isolation for 24 hours after the treatment. Female nursing staff face limitations when they have to check that the inmate has applied cream all over his body, including the genital area, in a patient from an Islamic culture. It is not easy for the workers of the centre to rigorously follow the protocols for washing clothing, keeping items that cannot be washed in a plastic bag for several days and disinfect the cell and potentially infested objects such as pillows and mattresses. It is also difficult to detect possible contacts with other inmates, since they interact in group and sports activities, where they often exchange clothing, and a few cases even deny that they have the disease or conceal it.
Evidently then, factors such as these could lead to an epidemic in the centre, and the fact that it has not reached such a state is due to a great extent to the hard work of the medical staff and to the fact that most of the diagnoses took place when the patients entered the centre, making it possible to isolate them before coming into contact with other inmates.
The bibliography shows that oral ivermectin should be the drug of first choice for treating patients and contacts in prison12,13,15-20. It is very effective, but it does not destroy the eggs, and so a second dose is required a week later. Treatment with topical permethrin also requires a second dose a week later, which was the regimen we followed. One limitation of oral ivermectin is that it is catalogued as a foreign drug and is only available with a signed, individual prescription for each patient. However, it can be obtained in pharmacies where it is prepared on the premises as a compound. Given that oral ivermectin is a highly necessary drug in cases of crusted scabies in prisons and other enclosed institutions, health authorities should facilitate its use12,13,15-20,27-31.
The situation described in the results led us to modify our intervention protocol. To overcome the potential limitations in applying topical permethrin, oral ivermectin at doses of 200 micrograms/kg in one dose repeated after one week was established as a first-line treatment, for the patient and for contacts. Both singles doses are administered in one direct dose taken in the presence of a health professional to ensure compliance. If the patient rejects the medication, the magistrate is informed and the patient is kept in isolation. In addition, a new order was drawn up by the centre management containing the treatment protocols for treating clothing that is infested and supplying new garments, using the recommendations taken from the bibliography. The period estimated for secure elimination of parasites in plastic bags is extended from four to seven days. Requests have been made for doses of oral ivermectin for infected persons, cellmates and contacts.
In any enclosed or semi-enclosed community, oral ivermectin has advantages over topical permethrin and may reduce the risk of epidemics29-31. Such communities include schools, campsites, barracks, hospitals, senior citizens' residences, hostels for the homeless, youth detention centres and centres for the mentally ill, disabled and drug users. The risk of epidemics in each centre depends to a great extent on the possible entry of infected individuals. Scabies is not distributed randomly throughout society, risk factors do exist. The medical teams that operate in enclosed communities should monitor the admission of possible cases and have specific guidelines to prevent epidemics27-31. It is important to take additional precautions in certain situations, since when the skin lesions are not sufficiently characteristic, but are associated with risk factors such as lack of hygiene and homelessness, the likelihood of a problem being scabies is multiplied. The typical profile of an infested person described in the Lancet9 journal, bears a close resemblance to our description of homeless North African people, who make up the vast majority of the cases. It is very likely that many affected individuals are even younger and have not yet entered prison, but may cause epidemics in internment centres and foster homes.
We had never witnessed so many cases of scabies in such a short time at our centre. The changes to our protocols and the use of oral ivermectin may help to prevent major outbreaks. The health authorities should take measures in view of the huge number of press releases that imply a large increase in new cases. Further precautions should be taken and the use of invermectin to prevent epidemics in enclosed and semi-enclosed communities should be recommended in Spain. Good hygiene and health education are the best tools for preventing scabies.