Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Enfermería Global
versión On-line ISSN 1695-6141
Enferm. glob. vol.15 no.43 Murcia jul. 2016
REVISIONES
Significance of anaemia in the different stages of life
Significado de la anemia en las diferentes etapas de la vida
Guzmán Llanos, María José*; Guzmán Zamudio, José L.** and LLanos de los Reyes-García, M.J.***
*Pediatric Nurse. Hospital SAS de Jerez de la Frontera (Cádiz). E-mail: mariyouguzman@hotmail.com
**Phd.Médical Hematologist.
***Nurse. Hospital de Día de Hematología-Oncología Hospital del SAS de Jerez de la Frontera (Cádiz)
ABSTRACT
Overview: Anemia is very common in primary care consultations and pediatrics, and IDA is the cause of 50% of all cases of anemia.
Methodology: Literature review and documentary descriptive analysis of the pathogenesis of iron-deficiency anemia, the basic diagnostic tests to study IDA and the significance of such using a specific time period in the documentary search and inclusion criteria that takes into account factors that are analyzed in the study: Ideas about the metabolism of iron. Ideas about hematopoiesis. Laboratory diagnosis and classification of anemia. Clinical features of iron deficiency anemia. Causes of iron deficiency.
Results and conclusion: The staged documentary study covers the publications on the pathogenesis of iron deficiency anemia, the basic diagnostic tests to study the IDA and the significance of such, and it shows how important this data is for professional nursing in the area of primary care and pediatrics, to identify it and act accordingly.
Key words: Iron deficiency anemia; anemia in pregnancy; anemia in seniors.
RESUMEN
Resumen: La anemia presenta una elevada prevalencia en las consultas de atención primaria y pediatría, y la ADH representa el 50% de todos los casos de anemia.
Metodología: Revisión bibliográfica y análisis descriptivo documental sobre etiopatogenia de la anemia ferropénica, las pruebas diagnósticas básicas para el estudio de la ADH y su significado, utilizando una temporalidad determinada en la búsqueda documental y criterios de inclusión atendiendo a las dimensiones que se analizan en el estudio: Nociones acerca del metabolismo del hierro. Nociones acerca de la hematopoyesis. Diagnóstico por el laboratorio y clasificación de las anemias. Clínica de la anemia ferropénica. Causas de la deficiencia de hierro.
Resultados y conclusión: EL estudio documental efectuado nos presenta la existencia de publicaciones con contenidos sobre etiopatogenia de la anemia ferropénica, las pruebas diagnósticas básicas para el estudio de la ADH y su significado, evidenciando la importancia de este contenido para el profesional de enfermería en el área de la atención primaria y pediatría.
Palabras clave: anemia por deficiencia de hierro; anemia en la gestación, anemia en el anciano.
Introduction
The WHO defines anemia as being the drop in the hemoglobin level two standard deviations below that of the normal value for the age and gender in question (1). In practical terms the values of 13 g/dl in men, 12 g/dl in women and 11 in pregnant women can be used. In children aged 6 months to 6 years old 11 /g/dl and from 6 years old to 14, 12 g/dl. These criteria are based on studies of the population that do not include seniors over 65, which means that perhaps it cannot be used for elderly people.
Anemia is highly prevalent in primary care consultations, pediatrics, and during pregnancy. Iron deficiency (ID) is not the same as iron deficiency anemia (IDA). The latter is the most common cause of anemia in the world and it is a major health problem mainly in underdeveloped countries. The IDA is very widespread, so much so that it affects 5% of children and adolescents, 10% of premenopausal women and 1% of men; and it can affect as many as 40% of the seniors who are looked after at home.
The majority of health services have clinical guidelines on how to control anemia in general and/or anemia during pregnancy (2, 3)
Anemia during pregnancy is considered to be a risk factor and it can lead to anemia in new-borns due to the short supply of iron. (4)
Pediatric anemia: IDA affects the growth and the development of children, it decreases their immune system resistance against infections and it alters their psychomotor development and cognitive function. (5,6)
According to the WHO report for the 1993-2005 period, IDA affected 47.4% of preschoolers and any figure over 40% is considered to be a serious health problem for this organisation. (7).
Gastrointestinal bleeding always has to be ruled out when it comes to IDA in postmenopausal women, adults and seniors.
Objective
The objective of this paper is to identify the pathogenesis of iron deficiency anemia, the basic diagnostic tests to study the IDA and the significance of such using a literature review, and recognize the different stages of iron deficiency early on at primary care consultations, in pediatrics and during pregnancy as a preventive measure and as a chance to improve all the work involved in these processes in nursing.
Methodology
Literature review published on the pathogenesis of iron deficiency anemia and diagnostic testing to analyze the IDA and the significance of such.
Descriptive documentary study using different bibliographic sources and databases on the subject matter under analysis.
The bibliographic search focused on the years 2000-2014, and there were other publications on the topic used for reference whose temporality was outside this time period.
The inclusion criteria in the bibliographical search focus on articles and the documentation published on the subject matter, within the chosen time period, which was refined according to their content and factors to be analyzed (Ideas about iron metabolism. Ideas about the hematopoiesis. Laboratory diagnosis and the classification of the different types of anemia. Clinical features of iron deficiency anemia. Causes of iron deficiency.)
Descriptors or key words of the search have been used such as: Iron deficiency anemia in children (4368 articles), iron deficiency anemia during pregnancy (up to 2173 articles) and in seniors (4605) and a selection has been made from these in compliance with the inclusion criteria of the review carried out.
Results
1.-The metabolism of iron
Iron is important because it is part of the hemoglobin and the cytochromes. When you stop growing, the body iron levels remain constant within very tight margins. The body iron is hoarded and recycled through various iron storage pools. (8, 9)
- Absorption: The iron consumed through the food that we eat must be absorbed, then it is carried through the blood and finally it is stored to form part of the iron storage pool (the iron supply). The iron consumed through the food comes in the form of Fe +++ although it is absorbed in the duodenum and upper jejunum as Fe ++, which means that it undergoes a reduction process involving ascorbic acid. Only 10% of iron is absorbed from food, which stands for 0.25 % of the total amount of body iron. Different factors favour or hinder iron absorption.
The amount of iron absorbed depends on the amount of iron the body actually needs. Iron absorption is favoured by iron deficiency anemia. Iron metabolism is unique in that the iron balance is basically controlled by the absorption more than by the excretion.
Dietary iron: the dietary iron intake is approximately 10 to 30 mg/day for adults. With the absorption of 5 to 10% of dietary iron (0.5 a 1 mg), the amount increases to 20% in the case of iron deficiency and it decreases if there is an overload of iron.
- Transport: The iron in the blood binds to its carrier protein (transferrin). The iron-transferrin complex is captured in the cells by a specific receptor.
The transferrin is synthesized in the liver and the transferrin concentration in the blood exceeds the iron binding capacity and approximately two thirds of the binding capacity is unsaturated.
Finally, iron has to be stored as ferritin and/or hemosiderin; approximately 1 microgram/L of serum ferritin represents 10 mg of stored iron.
Iron distribution: the most important iron storage pool is in the red blood cells as the hemoglobin contains approximately 2500 mg of iron. Another 40 mg is found in the myoglobin. The storage organs of iron contain 800 to 1200 mg. Only 4 mg of iron binds to the transferrin.
Iron requirements and balance: Healthy adults and post-menopausal women need approximately 1 mg/day.
Women of fertile age and blood donors, etc. need 5 mg of iron.
Pregnant women need 7 mg/day.
The elimination of iron from the body is not so well controlled; approximately 1 mg a day is excreted through the intestines, urine and perspiration. During menstruation between 15 to 30 mg of iron is lost, which can be made up for by increasing the amount absorbed, although this is more difficult to make up for in the case of menorrhagia; iron can also be lost when blood is donated frequently and during childhood, when taking too many blood tests can also result in an iron deficiency.
2.-Hematopoiesis
The formation of the main components of blood (leucocytes, red blood cells and platelets) takes place in the bone marrow and the process is called hematopoiesis. Derived from a pluripotent stem cell and stimulated by the erythropoietin, this stem cell would, after cellular differentiation, give rise to the formation of the mature red blood cell process known as erythropoiesis. (10) The erythropoietin (EPO) is the main growth factor needed to regulate the erythropoiesis. This is produced in the kidneys. It stimulates the proliferation of the erythroid series and the release of the reticulocytes from the bone marrow. Approximately 20-30% of the stem cells differentiate towards the erythropoiesis. The red blood cell is a nucleated cell, whose main function, thanks to the hemoglobin (Hb), is to carry the oxygen to the body tissues.
Hemoglobin is synthesized in the normoblast stage, and when this is totally hemoglobinized the nucleus is extruded and the reticulocyte is produced.
Normal hematopoiesis is maintained through an adequate iron supply together with a suitable concentration of vitamin B-12 and folic acid.
The Hb is made up of a protein part (globin) and the heme group (that contains an iron atom).
As red blood cells get older they are phagocytized by the cells of the mononuclear phagocyte system. This occurs at approximately 120 days and approximately 0.8% of the pool of erythrocytes is lysed, which keeps a balance between what is produced and what is destroyed.
3. - Laboratory diagnosis and classifying anemia
3.1. - The laboratory in diagnosing iron deficiency anemia. (4) Firstly it has to be confirmed that the patient has anemia and then it has to be determined whether this is due to an iron deficiency and to this end we will ask for:
- The most basic complete blood count (CBC) test, which provides us with a lot of information such as the number of red blood cells, the total amount of hemoglobin in the blood and the red blood cell indices MCV, MCH. As well as the number of leukocytes and platelets. All this data is useful when it comes to classifying the anemia. Iron deficiency anemia is often a risk factor for reactive thrombocytosis.
- Parameters related to the metabolism of iron: Serum iron, transferrin, transferrin saturation percentage, and the soluble transferrin receptor (sTfR).
- Assessment of iron storage pools: serum ferritin.
- Blood smear test: This shows the hemoglobin (hypochromia) content, the changes in shape (poikilocytosis) and the size (anisocytosis) that help make a correct diagnosis.
Clinical significance of the different proteins that are involved in carrying and storing iron.
Ferritin: This is the most important iron storage protein. High concentrations of this protein are found in the liver, the spleen and the bone marrow. It contains between 15 and 20% of the body iron.
A small amount of the ferritin produced is secreted by the cells and goes into the bloodstream. There is a direct correlation between the amount of this protein and the iron stored so that: 1 mcg/L of serum ferritin represents 10 mg of iron stored. The serum ferritin is a good indicator of the storage iron pools. But the fact that ferritin is also an acute-phase reactant should also be taken into account, as it means that sometimes the C-reactive protein (CRP) test also has to be carried out in order to rule out the existence of any infections/ inflammatory processes. Ferritin is therefore very useful to evaluate the metabolism of iron. Values of < 12 ng/ml point to the existence of a latent iron deficiency. A high ferritin value of > 400 ng/ml implies that there is an iron overload.
Transferrin, transferrin saturation: Transferrin is a protein that is synthesized in the liver and between 15 and 45% is saturated with iron. If there is a functional iron deficiency more of this protein will be synthesized; high values are found in iron deficiency and during pregnancy.
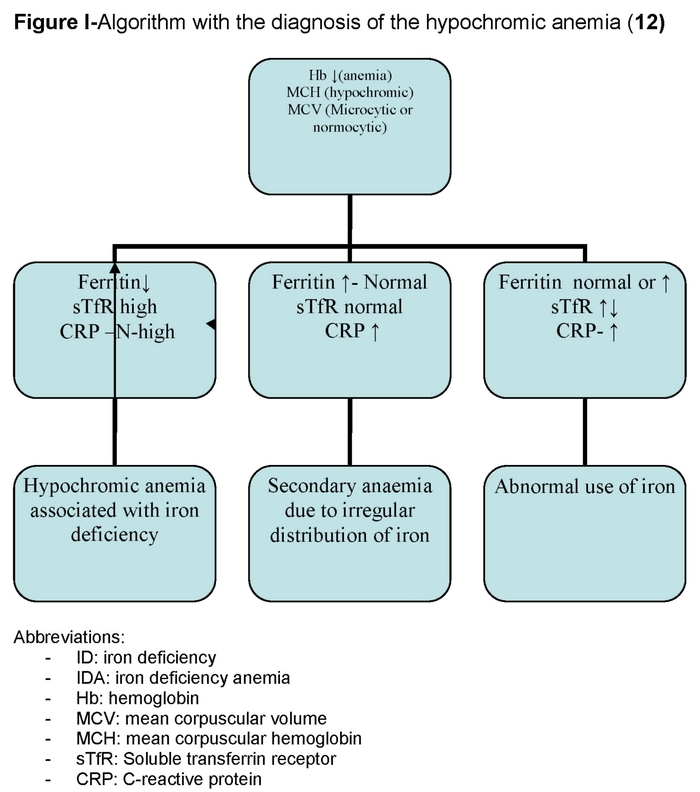
Soluble transferrin receptor (sTfR): Approximately 75% of the transferrin receptors are found in the erythroid precursors. The number of transferrin receptors increases when there is a functional iron deficiency. The soluble form is known as (sTfR). This is the only biological marker that associates an iron deficiency with erythropoiesis. It therefore complements ferritin. The sTfR is not affected by the acute-phase reactants so it highlights an iron deficiency where there is an infection, inflammation and/or tumours. (12)
3.2- Classifying anemia
A practical way of classifying anemia is by focusing on the red blood cell size (MCV) and the hemoglobin amount per red blood cell (MCH). These are two of the parameters that provide us with the reading of any hemogram using modern cell counters.
- The size can point to normocytic anemia, microcytic anemia and macrocytic anemia and according to Hb amount (MCH) normochromic anemia, hypochromic anemia and hyperchromic anemia 13 (Table I).
Microcytic anemia and hypochromic anemia are normally caused by iron deficiency anemia.
- According to the clinical severity:
• Severe anemia: Hb < 7.0 g/dl
• Moderate anemia 7.1 -10.0 g/dl
• Mild anemia 10.1 - 10.9 g/dl
The IDA is the final stage of a process that begins with the latent iron deficiency, where there is no anemia only a deficiency of iron; then the iron-transport deficiency, where as well as low ferritin levels, the TSAT is below 15% and finally the IDA with low ferritin levels, TSAT < 15% and anemia. (Table II)
- Other types of anemia due to the irregular distribution of iron: 14, 15
Anemia of chronic disease (AEC): In these cases there is a redistribution of iron with an increase in the iron storage pools and a relative shortage of iron supplied to the erythropoietic cells due to less transferrin being synthesized. This shortage of iron would have a protective effect against infection.
Kidney disease anemia: In this case the iron storage pools are normal but the iron mobilization is impaired (low transferrin saturation), which could lead to inadequate erythropoiesis and a functional iron deficiency. Iron cannot be taken orally because absorption is impaired.
Sometimes anemia of chronic kidney disease is complicated by a hemolytic factor.
- Abnormal erythropoiesis that is caused by iron: Vitamin B-12 and folic acid deficiency
Thalassemia: This disease involves a decrease or absence of the globin chain synthesis. The globin chain structure is normal. Thalassemia can be alpha, beta, gamma or delta, depending on the amount of the globin that is affected. It usually occurs with microcytosis, hypochromia and anemia of variable intensity. 13, 14
Microcytosis and hypochromia can be mistaken for iron deficiency anemia.
Alpha thalassemia minor and beta thalassemia minor are the most common. The fact that children with thalassemia can also have iron deficiency anemia should be taken into account, which is why they could need some type of iron treatment taken orally. As less of a globin chain is synthesized, the synthesis of other globins increases (Hb A2, Hb F). Quantifying these hemoglobins helps us classify them.
However, not all microcytic and hypochromic anemia are caused by iron deficiency and in this group those in which there is a misuse of iron, such as anemia of chronic disease should be highlighted etc.
4. - Clinical features of iron deficiency anemia.
The clinical features of iron deficiency anemia are no different from those of the other types of anemia, that is to say, it is unspecific; and basically the symptoms are fatigue, tiredness, weakness; although these symptoms depend more of the speed that the anemia sets in than the actual hemoglobin levels.
Many of the symptoms can be explained by the iron deficiency.
Pagophagia: compulsive tendency to eat ice. Geophagia: tendency to eat clay-rich dirt
Changes in the epithelium: koilonychia, angular cheilitis, atrophy of taste buds on tongue, changes in the intestinal mucosa.
Exercise intolerance, behavior changes: the child becomes apathetic and irritable.
5. -Causes of iron deficiency:(16)
The physiologic needs for iron increase: growth, menstruation, pregnancy, breast feeding
Bleeding: gastrointestinal, urogenital, iatrogenic
Poor iron absorption: gastrectomy, chronic atrophic gastritis, drugs
Inadequate supply: seniors, vegetarians
The IDA is part of a more complex diagnosis and its relevance varies in the different stages of life.
A. - During childhood it could be due to the fact that the body needs more iron as it grows. In the case of a sick child the number of blood samples taken for tests and the amount extracted is very important. (17, 18, 19)
New-borns start life with about 80 mg of iron per Kg of weight and 50 g/Kg of this forms part of the Hb. The body iron in a new-born is determined by the body weight and the circulating hemoglobin mass. Immediately after the umbilical cord is cut when a baby is born 15% to 30% of the total body iron is lost. The concentration of Hb in new-borns has nothing to do with the mother's Hb and body iron levels. There is no correlation between the mother's levels of ferritin and the umbilical cord blood either.
The new-borns of diabetic women can have iron deficiencies in spite of their high birth weight.
During the first 5 months new-borns can double their body weight without depleting their iron stores. After that iron absorption is important to maintain the iron balance.
During the first year of life a child needs more iron than in the rest of their life. Children need 0.5 mg/d to satisfy the iron requirements as they grow. It is highly unlikely that milk can supply this amount of iron; however, iron deficiency anemia is rare in breastfed babies. This could explain why up to 80% of the iron from milk is absorbed. The nutritional status of breastfed babies is much better than babies fed with cow's milk. Breastfed babies aged between 6 and 12 months can develop an iron deficiency.
The prevalence of ID is associated with the socioeconomic status of the family. It is also related to the cognitive function and even with febrile seizures.
B. - In fertile women the iron lost could be explained by menstruation, pregnancy and breastfeeding. (20)
During menstruation the majority of women lose 40 ml of blood, which is equal to 20 mg of iron. In Europe our diet contains enough iron to make up for the loss of 80 ml of blood, which is the same as 1.2 mg/d. Heavy menstrual bleeding is the main cause of anemia and it affects 9-14% of women. (21)
During pregnancy approximately 680 mg of iron is lost. This is much more than what can be absorbed, which is why iron supplements are needed during gestation.
Currently more than 40 million pregnant women in developing countries have iron deficiencies. Anemia caused by iron deficiencies stand for 75%-95% of the cases of anemia during pregnancy. Iron deficiency anemia during pregnancy has been associated with premature babies, low birth weight, and maternal mortality. The body needs different amounts of iron throughout pregnancy. Between 4 and 5 mg of iron is needed during the 2nd and 3rd trimester. The best way to make up for this deficiency is oral iron prophylaxis. During pregnancy the physiological iron requirements cannot be made up for just by taking folic acid. 60 mg of iron plus folic acid is recommended for women without anemia.(22)
C. - In postmenopausal women, adults and seniors the diagnosis could be more serious and gastrointestinal bleeding has to be ruled out. (23)
The Hb levels are not so well defined in seniors to diagnose anemia.
In seniors a normal ferritin level does not always rule out an iron deficiency, which is why the cut-off level to predict iron deficiency has to be raised to 50 micrograms/L.
In this group of patients a gastrointestinal tract study is recommended given the high incidence of hidden lesions that are detected.
In 68% of the patients over 75 with iron deficiency anemia for whom an endoscopy was carried out, the cause was found to be bleeding and in up to 11% of the cases it was due to a synchronous lesion.
The absence of an iron deficiency does not rule out the existence of digestive system neoplasms (24). What causes anemia in between 20-30% of seniors is unknown and this is referred to as the "Idiopathic Anemia of Aging".
Conclusions
- The diagnosis and the classification of IDA is based on simple techniques that are readily available in any clinical laboratory,
- The IDA is the end of a process that begins with iron deficiency.
- The clinical features of IDA are similar to those of other types of anemia although there are specific symptoms that can be attributed to iron deficiency.
- IDA is the most common type of anemia in all stages of life.
- During infancy babies aged between 6 and 12 months old who are fed exclusively on cow's milk can develop an iron deficiency. A major cause of IDA in children admitted into hospital is the high number of blood samples taken.
- IDA is the cause of between 75%-95% cases of anemia during pregnancy.
- In the case of postmenopausal women, adults and seniors gastrointestinal bleeding always has to be ruled out.
- In 20-30% of the cases of IDA in seniors the etiology is unknown.
Received January 15, 2015;
Accepted: February 24, 2015
References
1. World Health Organization. Iron deficiency anaemia assessment, prevention and control. A guide for programme managers. Geneva, Switzerland. World Health Organization 2001. [ Links ]
2. Proceso asistencial anemia. Proceso de anemia. Proceso asistencial integrado (Sevilla) Conserjería de Salud 2013. http://hdl.handle.net/10668/1683. [ Links ]
3. Ministerio de Salud Pública. Guía de práctica clínica. Diagnóstico y tratamiento de la anemia en el embarazo. 1a Edición, Quito. Dirección Nacional de normalización. 2014. http://saludgob.ec. [ Links ]
4. Matthew W, Domagalski, JE. Iron deficiency anemia: evaluation and management. American Family Physician 2013, vol 87, 2, 98-104. [ Links ]
5. Baker RD. Clinical report Diagnosis and prevention of iron deficiency and iron-deficiency anemia in infants and Young children (0-3 years of age) Pediatrics vol 126: %, 1040-1051, 2010. http://www.bcguidelines.ca/pdf/iron_deficiency.pdf. [ Links ]
6. Lukens J N. Iron metabolism and iron deficiency. Chapter 6. Blood Diseases of Infancy and Childhood. 7-o edition.1995 Mosby. [ Links ]
7. OMS 1993-2005.Worldwide prevalence of anaemia.- 1993-2005 WHO. Global database on anaemia. http://whqlibdoc.who.int/publications/2008/978924159657_eng.pdf. [ Links ]
8. Aisen P. Conceptos actuales sobre el metabolismo del hierro1-18; Clínica Hematológica; vol 10/2. Trastorno del metabolismo del hierro 1984. Salvat Editores. [ Links ]
9. Wick M, Pinggera W, Lehmann P. Clinical aspects and laboratory iron metabolism, anaemias. Novel concepts in the anemias of malignancies and renal and rheumatoid diseases. Fifth, enlarged edition. 2013 Springer Wien New York. [ Links ]
10. Rapaport S.I. Eritropoyesis. Capítulo 1, 2-5 Introducción a la hematología 1974. Salvat Editores. [ Links ]
11. Goddard AF, James MW; Mcintyre AS, Scott BB; British Society of Gastroenterology. Guidelines for the management of iron deficiency anaemia. Gut. 2011; 60 (10): 1309-1316. [ Links ]
12. Mast AE, Blinder MA, Gronosky AM, Chumley C, Scott MG. Clinical utility of the soluble transferrin receptor and comparison with serum ferritin in several populations. Clin Chem. 1998; 44(1): 45-51. [ Links ]
13. Tefferi A, Hansen CA, Inwards DS. How to interpret and pursue abnormal complete blood cell count in adults. Mayo Clin Proc 2005, 80: 923-936. [ Links ]
14. Wick M, Pinggera W, Lehmann P. Clinical aspects and laboratory iron metabolism, anaemias. Diagnosis of disturburbances of iron metabolism. Disturbances of erythropoiesis. Fifth, enlarged edition.2003. Springer Wien New York. [ Links ]
15. Goddard AF, James MW, Mcintyre AS, Scott BB; British Society of Gastroenterology. Guidelines for the management of iron deficiency anaemia. Gut. 2011; 60 (10); 1309-1316. [ Links ]
16. Orkin HS, Nathan DG. The thalassemias. Chapter 21. Nathan and Oski's Hematology of Infancy and childhood. 5a Edition.1998 W. B. Saunders Company. [ Links ]
17. Lee GR. Microcytosis and the anaemias associated with impaired hemoglobin synthesis. Chapter 25. Wintrobe's Cllinical Hematology. Ninth Edition.1993. LEA and FEBIGER. [ Links ]
18. Verga M E. Iron deficiency in infancy: is an immigrant more at risk? Swiss Med Wkly 2014; 144w14065. [ Links ]
19. Carter RC, Jacobson JL, Burden M et al. Iron deficiency anemia and cognitive function in infancy. Pediatrics 2010; 126 (2) 427-434. [ Links ]
20. Mohammad Reza Sharif, Davood Kheirkhah, et al. The relationship between iron deficiency and febrile convulsion: a case-control study. Global Journal of Health Science. Global Journal of Health Science. 2016. Vol 8 (2)185-189. [ Links ]
21. Breyman C. Iron deficiency in pregnancy. Seminars in hematol;2015; vol 52 (4) 339-347. [ Links ]
22. Fraser IS, Langhan S, Uhl- Hochgraeber K. Health-related quality of life and economic burden of abnormal uterine bleeding. Expert Rev Obstet Gynecol 2009; 4 (2):179-189. [ Links ]
23. Ioannou GN, Rockey DC, Bzyson C, Weis NS. Iron deficiency and gastrointestinal malignancy: a population based cohort study. Am J Med 2002. 113(4):276-280. [ Links ]
24. Joosten E, Ghesquiere B, Lindhoudt, et al. Upper and lower gastrointestinal evaluation of elderly impatiens who are iron deficient. Am J Med 1999: 107: 24. [ Links ]











 texto en
texto en