My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Enfermería Global
On-line version ISSN 1695-6141
Enferm. glob. vol.16 n.46 Murcia Apr. 2017 Epub Apr 01, 2017
https://dx.doi.org/10.6018/eglobal.16.2.251311
Originales
Time of chronic wound healing, as part of a prevalence and incidence study
1Nursing. Centro de Salud La Marina. Insitut Catalá de la Salut
2RN. Phd. Full Professor School of Nursing. University of Barcelona
Method
A transversal, retrospective study in the field of primary care in Barcelona city, with a population of 15,589 inhabitants over 15 years of age. The study period was from 1st January to 31st December 2013. Information on the etiology of chronic wounds and the time needed for healing was collected.
Results
416 records of injuries were located, of which 10.33% were chronic wounds. The median duration was 152 days and the mean average was 311 days, with pressure ulcers taking longest to heal. A statistically significant difference (p <0.05) was observed between the mean duration of wounds treated at the health centre and those treated at home. The prevalence was 0.28% and the incidence 0.24%, the wounds with the highest prevalence and incidence were venous ulcers.
Conclusions
Healing time depends on the type of wound and the point of care. The highest prevalence and incidence occurs in lower-extremity (leg) ulcers.
Keywords skin ulcer; wound healing; primary health care; nursing care; prevalence
INTRODUCTION
Skin ulcers are an important cause of morbidity and mortality everywhere in the world, and they occur due to a number of causes, including diabetes mellitus, peripheral neuropathy, immobility, pressure, arteriosclerosis, infections and/or venous insufficiency 1.
A wound is the loss of the anatomical and physiological continuity of the skin. Wounds can be classified as acute or chronic; a wound is considered chronic when healing does not occur within the expected period of time 2. Numerous sources cite chronic wounds as those whose healing requires more than six weeks 1)(3)(4. 95% of chronic ulcers are either venous, ischemic or pressure ulcers 2, the remainder are other types of wounds that are subject to secondary intention healing 5.
Chronic wounds are a significant health care problem and have serious implications for patient and carer quality of life, and for the use of both material and professional resources. Damage to the skin can have a negative impact on the patient's general welfare, which can last a long time, with some patients spending years in the health care system 6. Studies of the prevalence and incidence of chronic wounds are scarce, however those that do exist give similar results in industrialised countries 7.
González-Consuegra and Verdú estimate the median age of active ulcers to be 210 days, with enormous variation from less than one year to over 67 years 8.
The prolongation of healing time for chronic wounds affects patient quality of life and increases the costs associated with their care. In Catalonia, it has been calculated that cost of moist wound dressing products to the region's largest provider of primary health care, the Catalan Institute of Health (ICS by its initials in Catalan) was almost 6 million Euros in 2010 9.
The aim of this study is to establish the average time that chronic wounds take to heal in the patients assigned to an urban primary care team. A secondary aim is to establish the prevalence and incidence of those wounds.
MATERIAL AND METHOD
Transversal retrospective study in an urban area of Barcelona City, conducted in the Primary Health Centre La Marina, which covers a population of 15,589 inhabitants over 15 years of age. The period of the study was from the 1st January to 31st December 2013.
The data was collected between July and October 2014 by a group of nurses from that same Primary health centre.
The study population was people with a chronic wound assigned to the Primary Health Centre La Marina, whether they were treated at home or at the health centre.
Based on a review of the available literature 1)(3)(4, chronic wounds were considered to be those whose healing took more than six weeks. Wounds that healed within 42 days were excluded, as were those where it was impossible to monitor to full healing due to death, admission to hospital and/or transfer from the area.
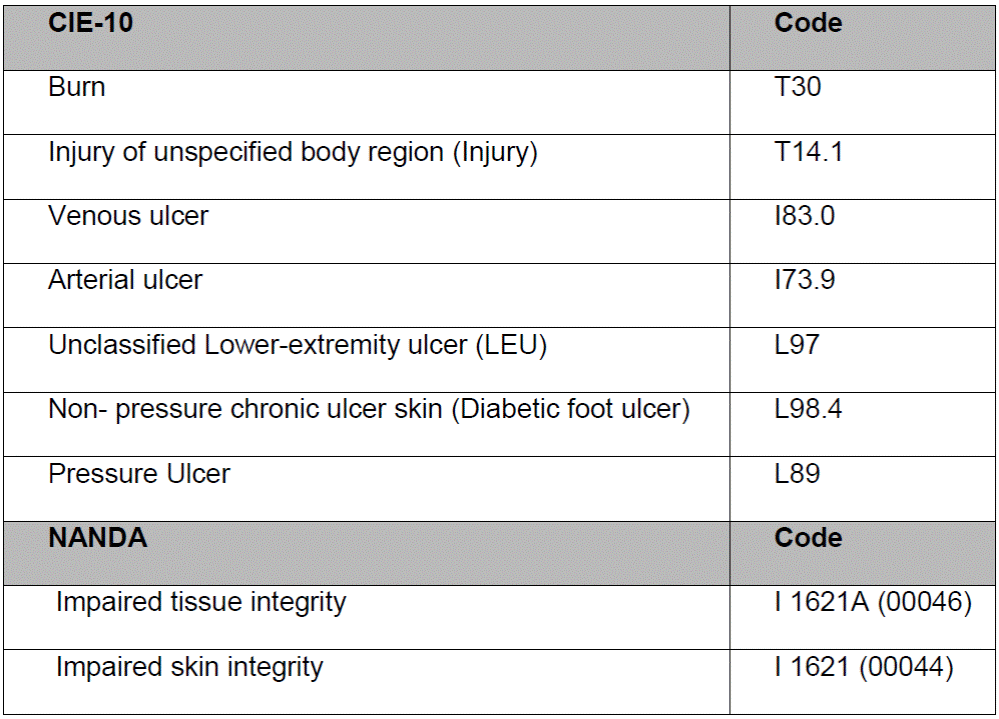
The data was obtained using the clinical primary care station (eCAP), which is the software used to manage digitalised medical records. The technical team (BASIQ) carried out a direct search using the ICD-10 (International Classification of Diseases) and NANDA (NANDA International, Inc) codes associated with wounds (Table I), date of discharge for the diagnosis, and the age and gender of the person.
The date of healing variable was obtained by reviewing the eCAP clinical history notes. It was decided to do it that way because, in our experience, and that of Puig Girbau et al 9, occasionally medical professionals do not remove the diagnoses associated with wounds although these have healed, thus creating a risk of overestimating both the prevalence and the duration of healing of the wounds.
The clinical history of wounds diagnosed under the NANDA taxonomy was also reviewed, in order to establish the origin of the wounds and include them in the study. Unlike the ICD diagnoses, NANDA diagnoses do not contain information about the causes of the wounds.
To homogenize the data collected, a database was created using Microsoft Excel 2007. A descriptive statistical analysis of the variables was conducted using the IBM programme SPSS Statistics 22.0. Prevalence and incidence were calculated using the population assigned to the ABS as the denominator. The variables were expressed as absolute and relative frequencies, medians, arithmetic means and standard deviations (SD) with a confidence interval (CI) of 95%.
To preserve patient confidentiality, an internal code was used in the database that enables us to identify each patient while at the same time guaranteeing their anonymity. Processing the data did not require any direct action with the patients nor any modification of their eCAP records. The project was approved by the ethics committee of the Primary Care Research Institute (IDIAP by its Catalan initials), part of the Jordi Gol y Gorina foundation, linked to the ICS.
RESULTS
416 records of wounds were found, of which 43 (10.33%) were chronic wounds. 53.48% were in women. The mean age of patients with chronic wounds was 72.21 years (SD 5.5) (Table II).
The median duration of healing was 152 days and the mean was 311 days (SD 135.38). The wounds taking longest to heal were the pressure ulcers, with a mean of 626 days (SD 643.78) and those taking least time to heal were injuries to an unspecified body region, with a mean of 105 days (SD 84.31) (Figure 1).
Prevalence of 0.28% and incidence of 0.24% were estimated, calculated over a population of 15,589 people over 15 years of age. Venous ulcers (0.08%) were the most prevalent. Injury of an unspecified body region and venous ulcers were the most frequent, both having an identical incidence (0.06%) (Figure 2). The diagnosis of injury to an unspecified body region included secondary intention healing of wounds of diverse etiology: surgical, traumatic, oncological or dermatological.
30.23% of chronic wounds were among patients treated as part of the home care programme (ATDOM by the Catalan acronym). A statistically significant difference (p<0,05) was observed between the mean duration of the wounds treated at the health centre and those treated at home (Table III).
Table III: Distribution of wounds by location of treatment and duration

* Representing absolute values because there is only one wound
The most prevalent wounds among the ATDOM patients were Lower-extremity ulcers (LEU), at 76.92%. In the comparison of proportions, it was observed that the proportion of patients treated at home for venous ulcers, LEU and pressure ulcers, was significantly higher than the proportion of patients treated in the health centre for the same diagnoses (p<0,05).
All the wounds had a single diagnosis, be that a NANDA or CIE-10 diagnosis. On reviewing the clinical notes, it became clear that the coded diagnosis did not always coincide with the diagnosis in the written notes. Thus, in 25.58% of the records, discord was detected in the diagnosis, in that the CIE-10 code used was different to the diagnosis mentioned in the written notes in the clinical history. The NANDA diagnostic labels of impaired skin integrity and impaired tissue integrity were respectively used to diagnose 37.21% and 4.65% of the wounds.
The monitoring of all the wounds included in this study was complete and there were no losses.
DISCUSSION
Assessing the average duration of the wounds is difficult, due to the wide dispersion that exists in the data. This dispersion also appears in the different studies reviewed by Gonzalez-Consuegra and Verdú (10) with healing durations of between two months and 50 years. Our 311 day mean is slightly more than the 252 days found by a study carried out in Sweden 11. If we only analyse the LEU we find an average healing time of 315.8 days, which agrees with the findings of Malaquias et al 12 where they indicate that 44.5% of the LEU studied take more than a year to heal. Nevertheless, our data differs considerably form the findings of Edwards et al 13 who locate the mean healing time at 12 weeks (84 days).
With regards to wounds treated at home, the average healing time obtained in our study is almost six months less than that obtained in a study in Quebec 14. This divergence could be explained by differences in the methodologies of the studies, the etiology of the wounds, the products used in their treatment or environmental or socio-economic factors.
In our study, prevalence and incidence are almost the same, at 0.28% and 0.24% respectively, a finding that was already indicated by K. Kirketerp-Møller et al 8. Total prevalence is a value very close to the 0.29% found by Ferrer-Sola et al 15) in their study in a county in the province of Barcelona, despite methodological differences between the two studies.
If we take the sum of venous ulcers, arterial ulcers and unclassified lower-extremity ulcers, we get a prevalence of LEU of 0.14%, which coincides with the data offered by the National conference on Lower-extremity Ulcers (CONUEI by its Spanish acronym) 16. Meanwhile, our UPP data amounts to less than half of the estimated prevalence in the last national study conducted by the National Study and Advice Group on Pressure Ulcers (GNEAUPP by its Spanish acronym) 17. This marked difference could be due to under-diagnosis of Grade I Pressure Ulcers in our team, although we could not confirm this as data was not collected as to the grade of the pressure ulcers.
A limitation of this study is its retrospective character, as this could lead to an underestimation of prevalence and incidence if, at the moment of diagnosis, there were wounds linked to different diagnostic codes from the ones selected for the study. We did not contemplate the collection of socio-economic data which would have enabled us to better understand the results. The manual handling of the data is also a limitation as it requires more time and increases the risk of human error.
The prevalence of chronic wounds is similar to that in other studies. Prevalence and incidence are almost the same, and the prevalence and incidence of LEU are notable for being higher that those of wounds of other etiologies.
To conclude, healing time depends on the type of wound and the place of treatment
REFERENCIAS
1. Lazarus G, Valle MF, Malas M, Qazi U, Maruthur NM, Doggett D, et al. Chronic venous leg ulcer treatment: future research needs. Wound Rep Reg. 2014; 22(1):34-42. [ Links ]
2. Situm M, Kolic M. Definicija i podjela atipicnih rana. Acta Med croatica. 2012; 66 Suppl 1:S5-11. [ Links ]
3. Formentini M, Fernandes LP. Factors that influence healing of chronic venous leg ulcers: a retrospective cohort. An Bras Dermatol. 2014; 89(3):414-422. [ Links ]
4. Cacicedo R, Castañeda C, Cossío F, Delgado A, Fernández B, Gómez MV, et al. Manual de Prevención y Cuidados Locales de Heridas Crónicas. Servicio Cántabro de Salud (Monografía en internet). Cantabria: Servicio Cántabro de Salud; 2011 [acceso 21 Feb 2014]. Disponible en: http://www.scsalud.es/documents/2162705/2163005/Manual+de+Preveci%C3%B3n+y+Cuidados+Locales+de+Heridas+Cr%C3%B3nicas_SCS.pdf [ Links ]
5. O'Meara S, Cullum N, Majid M, Sheldon T. Systematic reviews of wound care management: (3) antimicrobial agents for chronic wounds; (4) diabetic food ulceration. Health Technol Assess. 2000; 4(21):1-237. [ Links ]
6. Bateman S. Principles of preventative foot care. Br J Community Nurs. 2014; 19 Suppl 3: S30-38. [ Links ]
7. Kirketerp-Møller K, Zulkowski k, James G. Chronic Wound Colonization, Infection, and Biofilms. En Bjarnsholt T et al. Biofilm infections. Copenhagen: Springer; 2011. p. 11-24. [ Links ]
8. González-Consuegra V, Verdú Soriano J. Calidad de vida y cicatrización en pacientes con úlcera de etiología venosa. Validación del Charing Venous Ulcer Questionnaire, versión española (CCVUQ-e) y del Pressure Ulcer Scale for Healing, versión española (PUSH-e). resultados preliminares. Gerokomos. 2011; 22(3):131-136. [ Links ]
9. Puig Girbau N, Teixidó Vargas C, Estébanez Perpina JL, Bosch Fortuna S. Prevalencia de lesiones en el ámbito de la atención primaria, a propósito de las variantes de registro. Metas Enferm. 2013; 16(2):6-10. [ Links ]
10. Gonzalez-Consuegra RV, Verdú J. Quality life in people with leg ulcers: an integrative review. J Adv Nurse. 2011; 67(5): 926-944. [ Links ]
11. Öien RF, Åkesson N. Bacterial cultures, rapid strep test, and antibiotic treatment in infected hard-to-heal ulcers in primary care. Scand J Prim Health Care. 2012; 30(4): 254-258 [ Links ]
12. Malaquias GS Bachion MM, Sant'Ana SM, Dallarmi CC, Lino Junior RdeS, Ferreira PS. Pessoas com úlceras vasculogênicas em atendimento ambulatorial de enfermagem: estudo das variáveis clínicas e sociodemográficas. Rev Esc Enferm USP. 2012; 46(2): 302-310. [ Links ]
13. Edwards H, Finlayson K, Courtney M, Graves N, Gibb M & Parker C. Health service pathways for patients with chronic leg ulcers: identifying effective pathways for facilitation of evidence based wound care. BMC Health Serv Res [serie en internet]. 2013 [acceso 21 Mar 2014]; 13 (86): [aprox 10 p.]. Disponible en: http://www.biomedcentral.com/1472-6963/13/86 [ Links ]
14. Rodrigues I, Megié MF. Prevalence of chronic wounds in Quebec home care. Ostomy wound manag. 2006; 52(5):46-57. [ Links ]
15. Ferrer-Solà M, Chirveches-Pérez E, Molist-Señé G, Molas-Puigvila M, Besolí-Codina A, Jaumira-Areñas E, et al. Prevalencia de las heridas crónicas en una comarca de la provincia de Barcelona. Enferm Clin. 2009; 19(1): 4-10. [ Links ]
16. Conferencia Nacional de Consenso sobre Úlceras de la extremidad inferior. Documento de consenso CONUEI. Barcelona: EdikaMed; 2009. [ Links ]
17. Pancorbo-Hidalgo PL, García-Fernández FP, Torra Bou JE, Verdú Soriano J, Soldevilla-Ágreda JJ. Epidemiología de las úlceras por presión en España en 2013: 4.º Estudio Nacional de Prevalencia. Gerokomos. 2014; 25(4):162-170. [ Links ]
Received: February 15, 2016; Accepted: April 15, 2016











 text in
text in