Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Enfermería Global
versión On-line ISSN 1695-6141
Enferm. glob. vol.18 no.54 Murcia abr. 2019 Epub 14-Oct-2019
https://dx.doi.org/10.6018/eglobal.18.2.317281
Originals
Obstetric practices developed in two maternities for low risk mothers
1Nurse. Master in Nursing from the Federal University of Rio Grande do Norte. Brazil. isaianekarvalho@hotmail.com
2Nurse. PhD in Nursing from the Federal University of São Paulo.
2Professor of the Graduate Program in Nursing, Federal University of Rio Grande do Norte. Brazil.
Objective:
Evaluate the quality of care provided to women and children during cases of natural childbirth in municipal public maternity wards of the city of Natal/RN, Brazilian Northeast.
Method
A cross-sectional study, quantitative in two public hospitals with 314 puerperal women attending the period between April and July 2014.
Results:
The differences between the maternity wards were identified with regard to the provision of liquids orally (p=0.018), stimulus for non-supine position (p=0.002), existence of partograph (p=0.001), support or welcoming by health professionals (p=0.047) intravenous infusion (p<0.001), supine position (p<0.001), use of oxytocin (p<0.001), food and liquid restriction (p=0.002), and the fact that the touch is performed by more than one examiner (p=0.011). Assistance during the process of labor and birth showed better results in general for motherhood A.
Conclusions:
They become necessary to implement improvements and realignment of current obstetric model.
Key words: Obstetric Nursing; Health Evaluation; Quality of Health Care; Natural Childbirth
INTRODUCTION
In recent years, several changes have occurred in the obstetrics field. As an example of a reaction to the model established with the hospitalization of labor and birth, emerged a movement with a view to humanization. This brought discussions, which highlighted practices and institutional routines designed scientifically as unnecessary and contributors to transform an occasion that should bring joy and satisfaction in something frightening1.
The humanization of delivery and birth has emerged as a challenging proposal for hospitals, health professionals and society, seeking new possibilities of care practices and redefinitions of roles of the subject members of this scenario2 3. In addition, we sought to rescue the normal delivery as a physiological event, including all the complexity associated with the process of pregnancy, delivery and birth, so that the woman regain control over its child birth process4.
On the normal delivery, the routines undertaken during this period were grouped into four categories: Category A - practices that are demonstrably useful and should be encouraged; Category B - practices clearly ineffective or harmful and which must be eliminated; Category C - practice in relation to which there is no scientific evidence sufficient to support a clear recommendation and should be used with caution; and Category D - practices often used improperly5.
Even so, in spite of the advances, in many cases the practices developed in the daily life of obstetric services are in step with the recommended by public health policies. Thus, one of the ways to identify how specific assistance is provided may be upon the development of studies that address the quality evaluation. The city of Natal, capital of Rio Grande do Norte, Northeastern Brazil, constitutes itself as a reference in the obstetrical care state. However, the insecurity prevailing in the obstetric services within the state contributes to that, sometimes, the displacement of the parturients toward the capital. This fact favors the overload of local services, which have difficulties to provide quality assistance outside the excessive demand of pregnant women6. Thus, this study aimed to evaluate the quality of obstetric care provided to women and child during normal delivery in public maternity hospitals in the city of Natal/RN.
MATERIAL AND METHOD
This was a cross-sectional study, with a quantitative approach and based on the protocol of Strengthening the Reporting of Observational Studies in Epidemiology7. The study was developed in two municipal public maternity hospitals (A and B) located in the city of Natal. This is inserted on the coast of the state of Rio Grande do Norte in the Northeast region of Brazil, and corresponds to the capital of the state, with a land area of 168.53 km2(8. The maternity A, for not having a surgical center, performs only normal deliveries. In turn, the maternity unit B performs in addition to normal deliveries, cesarean surgery.
The study participants understood puerperal women, whose son was born alive, transpel way, with onset of spontaneous labor or induced, and that showed physical and emotional conditions to answer the questions proposed. Puerperal women were excluded from the study adolescents who were not accompanied by their legal guardians at the time of the interview, in order to authorize their participation in the research. Also the exclusion was performed when the delivery occurred at home. Based on the number of births that occurred in the year of 2012, we calculated the size of the sample considering an α=5% and a margin of error of 0.05, which resulted in a value equal to 314 puerperal women allocated proportionally to each maternity leave (Maternity A: 112; Maternity B: 202).
The data collection instrument was built based on the recommendations of the WHO5for the assistance to normal delivery and passed through the validation process, having the final version obtained excellent concordance (k=0.96; CVI=0.99). The data collection occurred in the period from April to July 2014, and the visit to the maternity ward took place consecutively, with intervals of 24 hours, counting from the beginning of the first day of the collection. The rapprochement with the puerperal women gave themselves through oral invitation during a visit to the housing assemblies and after acceptance of the contacted, began the structured interview. Additional information was obtained from the medical records: number of prenatal consultations; gestational age; Apgar scores; weight of the newborn; presence of trace; use of oxytocin; performance of episiotomy; epidural analgesia.
The data collected were entered in a spreadsheet in Microsoft Excel® program Oficce 2010 version and then exported to the program IBM SPSS Statistics® version 20.0. For the analysis of the categories related to the recommendations of who we used absolute and relative frequency. Qui-Square tests of Pearson and Fisher's exact test, the latter for the cases in which the frequency expected was lower than 5, comparing the differences observed between the two maternities. It is considered in all statistical tests, the significance level of 5%
The project was approved by the Research Ethics Committee at the Rio Grande do Norte Federal University, under nº 562,313 of 28 February 2014 and Presentation Certificate for Ethics Consideration: 25958513.0.0000.5537.
RESULTS
ATables 1and2show the use of the WHO recommendations for normal delivery assistance by categories. On the category, there has been providing oral liquids in labor and childbirth (45.54%), respect for privacy (90.13%), companion presence (85.67%), answered questions in case of doubts/questions (96.43%) and aid for pain relief through non-invasive and non-pharmacological methods (79.30%). The methods most often used corresponded to the bathroom to shower (46.18%), walking (45.86%) and achievement of massages (34.71%). Were also cited the wheelie (33.12%), breathing exercises (27.07%) and ball of calving (8.92%). The last method was available exclusively to the maternity unit A.
Furthermore, it was observed that fetal monitoring by means of cardiac auscultation (96.18%), guidance as to the possibility of non-supine positions during labor (59.24%), existence of trace (2.23%), direct skin contact early, at least 30 minutes in the first hour of life, between mother and son (78.66%), guidance regarding the initiation of breastfeeding in the first hour postpartum (78.34), support or acceptance by health professionals (92.36%), and prior choice of motherhood by puerperal women (51.91%). It was identified differences between maternity units for the variables offer of liquids orally (p=0.018), a stimulus to no-supine positions (p=0.002), existence of trace (p=0.001) and support or acceptance by health professionals (p=0.047).
In terms of category B, was not reported the achievement of enema and trichotomy in the institutional framework in none of the cases. There was intravenous infusion during labor (48.73%), supine position during the whole labor (23.57%), delivery in lithotomy position (99.68%) and use of oxytocin before delivery (52.87%). In the case of categories C and D were checked pressure in the uterus (22.29%), hydric restriction and food (18.15%), more than three vaginal rings (31.60%), more than one examiner (60.77%) and performance of episiotomy (50.64%). Information about epidural analgesia were not present in any of the cases evaluated.
Table 1. Use of WHO recommendations for care of normal delivery in maternity wards A and B (Category A). Natal/RN, Brazil, 2014.
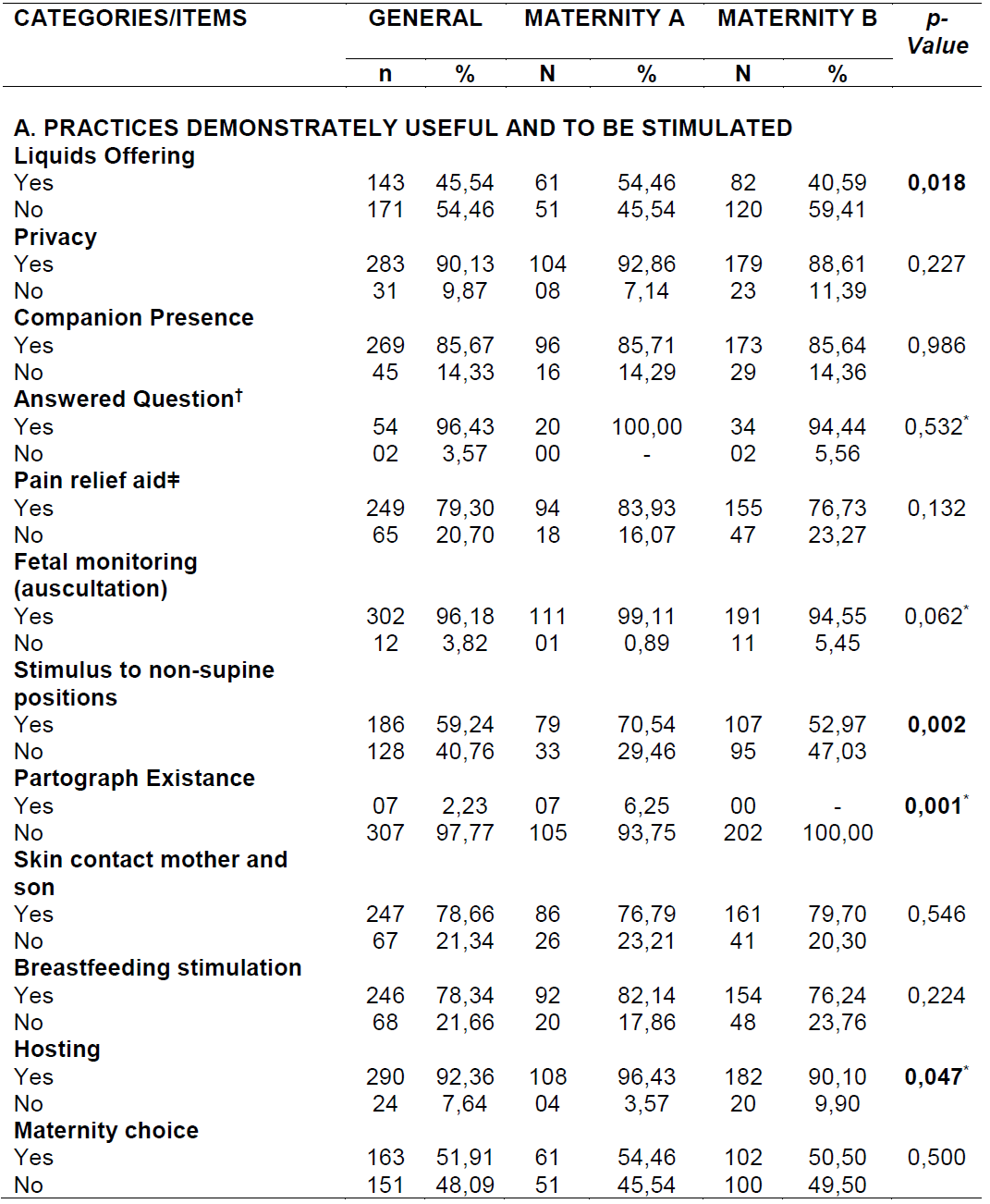
Caption:*Fisher's exact test; † Values for puerperal women who asked questions (17.83%, n = 56); Não Non-invasive and non-pharmacological methods.
Source: Own research (2014)
Table 2. Use of WHO recommendations for care of normal delivery in maternity rooms A and B (Categories B, C and D). Natal/RN, Brazil, 2014.
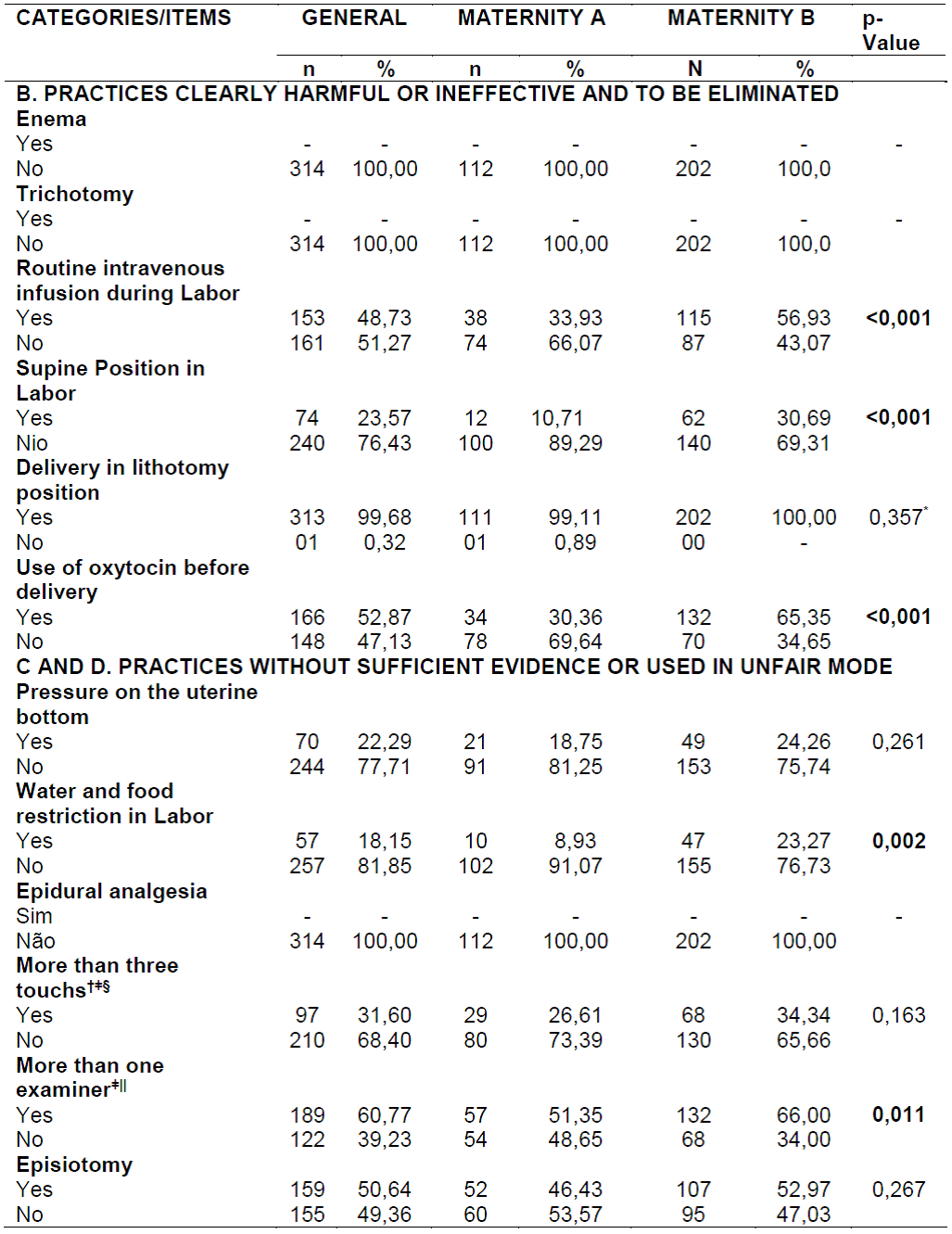
Caption: Own research (2014);*Fisher's exact test; † Value of the median used for categorization; ǂValues for puerperal women in whom a vaginal touch was performed (99.68%; n = 313); §Excluded: did not know to inform (1,92%; n = 06); || Deleted: could not report (0.64%, n = 02).
Source: Own research (2014)
DISCUSSIONS
The data revealed that the practices of category A presented better results in maternity A, but should be encouraged in both maternities, especially for some evaluated items. In terms of Category B, C and D practices, some are no longer part of the routine of institutions. However, those that continue to be performed presented high percentages, being the largest observed in maternity B.
Oral delivery of fluid in labor occurred to less than half of puerperal women, with poorer outcomes for B maternity. However, the results were higher than those found in a survey that assessed the use of WHO practices in a birth center in the Southeast of the country, 39%. The study also considered the possibility of solid and liquid foods and in this case the percentage increased to 56.6%9A systematic review on the subject concluded that there are no benefits or harms associated with this practice for women at low risk of complications. Furthermore, given the lack of research with women who present a higher risk of complications, there is no evidence to support the restriction10.
Privacy was reported by a large number of puerperal women. However, this result should be evaluated with caution, since it was remarkable during the responses that for many puerperas the lack of privacy was something inherent in the process of childbirth and birth. Thus, even in the face of this occurrence, her ideas did not permit real identification, denoting the need for deeper investigations into what is privacy for the puerperal woman in the birth scenario. In contrast to this result, an investigation conducted at a maternity school identified that only 15% of parturients reported having privacy11. Moreover, a Brazilian population-based study evidenced some factors associated with greater privacy during the birth and delivery process, such as high schooling, cesarean sections, presence of companions and private payment sources12.
Concerning the presence of the companion, inferior results were obtained in a research developed in Brazil, where a percentage of 75.5% was obtained for some companion type during hospitalization13. This shows that gradually the presence of the companion during labor begins to be integrated as part of the institutional routine in the maternity hospitals investigated. A systematic review has demonstrated that ongoing support has significant clinical benefits, is harmless and therefore should be available to all women in the parturition process14.
Few women asked, but those who did, for the most part, had their doubts clarified. A study related to the satisfaction of the woman during the parturition process identified that the clarity of the explanations was associated to the birth in the Southeast and South Regions of Brazil, presence of companion and source of private payment12. Thus, the provision of explanations and information to women is fundamental to the understanding of this moment, and this item should receive special attention from the service providers.
In terms of the use of non-invasive and non-pharmacological methods for pain relief, the results obtained were close to those found in a research study developed in a university hospital in the southeast of the country (77%). Such situation also occurred in this research. This reality demonstrates the acceptance of puerperal women to non-pharmacological methods for pain relief in labor, when they are available at institutional level.
A study conducted to summarize the evidence of systematic reviews on the efficacy and safety of nonpharmacological and pharmacological interventions for the management of labor pain has concluded that most nonpharmacological methods are noninvasive and appear to provide safety to the woman in labor and to your child. However, its efficacy is uncertain due to limited evidence of high quality. Some methods like water immersion, massage and relaxation can smooth labor pain. Thus, it is necessary to consider the needs and circumstances of each woman16.
In fetal monitoring, only cardiac auscultation was verified, and this was reported by practically all women, emphasizing the importance given by professionals to this procedure, different from what occurred in a study on the quality of normal delivery assistance in a city in the Center of the country, where auscultation was not performed in 29.1% of the cases17.
The stimulus to non-supine positions, specifically for labor, was described by slightly more than half of the puerperae, with better results in maternity A. Regarding this subject, there is clear evidence that walking and vertical positions, compared to reclining positions or bed care, reduce labor time, cesarean section risk, need for epidural analgesia, and appear to be unrelated to the increase in negative effects on the mother and child. Women at regular risk should be informed about the benefits associated with upright position, and encouraged to assume the one that best suits their needs18.
The partograph was not practically part of the institutional reality of the evaluated maternity hospitals, only existing low percentage in maternity A in the presence of medical students. Differently from that observed, a study carried out in school maternity hospitals located in the Northeast Region of Brazil found a frequency of 42% regarding the use of the partograph19. The current available evidence does not allow a routine recommendation of the partograph. In this sense, the authors of the systematic review, when considering its wide acceptance, recommended that its use should be determined locally until stronger evidence emerges20. This fact, considering the influence of this tool to reduce cesarean rates, as well as the context of the Brazilian reality with high rates of this surgery, should be encouraged in the institutions evaluated.
Skin-to-skin contact between mother and child reported in both maternities was superior to that found in a survey that evaluated this practice in Brazil (41.9% for vaginal deliveries). When comparing the types of delivery, newborns vaginally presented a greater chance of having this contact in relation to the cesarean section. Likewise, the stimulus to breastfeeding in the first hour of life was also higher (78.34%). The authors of the national survey obtained a percentage equal to 59.2% for this practice, with a greater chance of its occurrence in vaginal deliveries21. These results are associated with the adaptation of the newborns of the present study to extrauterine life, a condition that favors the development of these interventions. In addition, it may be a reflection of the fact that both maternities are Child Friends Hospitals.
According to this initiative, in step number 4, early skin contact between mother and child should occur immediately after delivery for at least one hour, in addition to encouraging breastfeeding. The mentioned recommendation stipulates that at least 80% of the women interviewed should refer to the implementation of these practices during the institutional evaluation process22. Such contact may bring benefits related to breastfeeding, as a greater probability of breastfeeding between one and four months after birth and does not present any visible or short-term adverse effects in the short or long term23.
Regarding the host (92.36%), lower results were obtained in the study by Figueiredo et al.11, where 78% of the puerperae reported being welcomed. Within the scope of the Stork Network, among its guidelines, there is a guarantee of the reception and classification of risk. It should be emphasized that the act of welcoming is not reduced to kind behavior from some professionals, nor a physical reorganization of the service or institution of a service triage, once when developed it deviates from its real purposes24. Thus, it is understood that this component is a relevant aspect for the process of evaluating service quality, especially when expressing the user's vision.
Regarding respect for the woman’s choice of the place of birth, the Stork Network recommends the existence of a link between the pregnant woman and the care network from the prenatal period, including the maternity expected to perform the delivery24. In addition, Law nº 11,634, dated December 27, 2007, ensures the right to be bonded to the maternity where the pregnant woman will receive care in the SUS25. However, little more than half of the women interviewed had the opportunity to choose the institution in which the childbirth would be performed, reflecting disrespect for this right. On the other hand, those who did not have the possibility to choose were more likely to be pilgrims from various institutions and expose themselves to the numerous risks associated with this problem, considering the possibility of not being bound.
The use of enema and trichotomy was not identified in any of the maternity hospitals evaluated, demonstrating that these procedures were definitively eliminated from the routine of institutional obstetric practices. However, on the trichotomy, although the procedure was not performed in the maternities, the interviewees reported having done so in their homes, proving to be something culturally instituted and accepted by women. Studies such as d'Orsi et al.26, with data collection between 1998 and 1999, identified for enema (17% and 38.4%) and trichotomy for vaginal deliveries in public and private maternity hospitals (63.3% and 41.1%). In Canada, research developed between 2005 and 2006 presented percentages of 5.4% and 19.1% for enema and trichotomy respectively27.
On the enema, a systematic review with four clinical trials, with 1,917 women, concluded that there is no benefit in terms of the rate of puerperal infection and neonatal infection. Likewise, no significant differences were identified regarding perineal laceration and mean duration of labor. Thus, their routine use is discouraged28.
For routine trichotomy in the admission of labor, a systematic review showed no difference in maternal febrile morbidity, perineal wound infection and dehiscence of the perineal wound. So, the authors concluded that there is no evidence to recommend this practice29. In this sense, with the recommendations of the researches developed in recent years, the enema and the trichotomy were progressively excluded from the routine of obstetrical procedures.
The intravenous infusion in labor was present in both maternities with the worst percentages for B. However, higher results were found, considering the national coverage (73.8%) and the Northeast Region (71.5%)30. Its indication is usually related to hydration and nutritional support and a possible reduction of labor time. However, a systematic review of this practice in nulliparous women at usual risk has demonstrated the lack of robust evidence to recommend it31.
About supine delivery, such a position is routinely adopted in both maternities. In Brazil, in a study considering all the Regions of the country, this position was present in 91.7% of the habitual risk births evaluated30. However, when other positions are available, women tend to assume them, such as semi-settled (82.3%) and lateral (16.0%)9.
A survey identified 38.2% of births at normal risk in Brazil, with the highest in the Southeast (47.2%), South (46.1%) and Northeast (30, 9%)30, results lower than those found in maternity B. This shows that this is a practice widely used in the daily obstetric services investigated, making it necessary to develop other research on the real need for indication. Systematic review of the use of oxytocin compared to no treatment or delayed treatment for slow progress in the first stage of labor has concluded that although reducing labor for some women is important, if the goal is to reduce cesarean sections, other aspects should be considered32.
Regarding the pressure in the uterine bottom, a percentage of 37.3% was identified for this maneuver in pregnant women with habitual risk in Brazil, with the Central West (45.5%) and Northeastern (40.6%) Regions obtained the worst results, which shows values above those identified in the present study (22.29%)30. Regarding this issue, a study on the effects of the Kristeller maneuver on the pelvic floor revealed that such intervention did not modify the functionality of the pelvic floor, but increased episiotomy rates (66% vs. 25.3%, p <0.0001)33. A systematic review has concluded that there is no evidence available for making claims about the benefits or harms of this maneuver34. In view of the observed episiotomy rates, especially in maternity B, the frequency of pressure on the uterine fund should be reviewed in order to minimize possible damage to maternal and fetal health.
Epidural analgesia is not part of the routine procedures of any of the maternity hospitals investigated. In Brazil, the use of this practice was 31.5% for deliveries at usual risk30. In a study with multiparous women, there was an association between cesarean section and epidural or spinal anesthesia35. Systematic review has identified that epidural analgesia appears to be effective in reducing pain during delivery but increases the chance of an instrumental delivery 36.
When evaluating their frequency in a Scottish hospital, it was found that 75.52% of the women had three or more vaginal exams during labor, with a mean of 2.9 ± 1.5, and variation between one and seven touches, the mean being close to that obtained in the present investigation (3.09 ± 1.91)37. A systematic review study of routine vaginal exams to assess the progress of labor found no evidence to support or reject the routine use of this examination during delivery38. Given the lack of evidence, it should be considered that vaginal exams are invasive procedures, uncomfortable, and in some cases cause pain39.
Finally, the percentage of episiotomy obtained (50.64%) was similar to that found for Brazil (56.1%)30. A policy of restrictive episiotomy compared to its routine execution seems to present a number of benefits, such as less severe perineal trauma, suturing, and healing complications. However, there was an increase in anterior perineal trauma with restrictive episiotomy40. It is noteworthy that in situations where delivery is attended by obstetrical nurses, lower percentages of this procedure are identified, demonstrating that these professionals perform fewer unnecessary interventions at perineal level41. Thus, considering the percentages identified in the two maternities evaluated, it is necessary to reconsider the frequency with which this practice occurs, with a view to reducing the physical and emotional damages that it entails in the woman, as well as to encourage the attendance at the usual risk delivery by the nurse obstetrician.
CONCLUSIONS
In view of the results presented, it was verified that the practices of category A need to be increasingly stimulated, especially in maternity B, such as the use of partograph, the provision of liquids and the stimulation of non-supine positions. In an articulated way, prenatal care needs to ensure the existence of a link between pregnant women and the maternity in which the delivery will probably occur. On the contrary, the practices present in the other categories should be reviewed, such as delivery in a lithotomy position, the use of oxytocin in labor, vaginal touch performed by more than one examiner and the occurrence of episiotomy.
REFERENCIAS
1. Silveira SC, Camargo BV, Crepaldi MA. Assistência ao parto na maternidade: representações sociais de mulheres assistidas e profissionais de saúde. Psicol Reflex Crit. 2010; 23(1): 1-10. [ Links ]
2. Bessa LF, Mamede MV. Ação educativa: uma perspectiva para humanização do parto?. Rev Baiana Enferm. 2010; 24(1,2,3): 11-22. [ Links ]
3. Busanello J, Kerber NPC, Fernandes GFM, Zacarias CC, Cappellaro J, Silva ME. Humanização do parto e a formação dos profissionais da Saúde. Ciênc Cuid Saúde. 2011; 10(1): 169-75. [ Links ]
4. Gonçalves R; Aguiar CA, Merighi MAB, Jesus MCP. Experiencing care in the birthing center context: the users' perspective. Rev Esc Enferm USP. 2011; 45(1): 62-70. [ Links ]
5. World Health Organization. Care in normal birth: a pratical guide. Geneva: World Health Organization; 1996. [ Links ]
6. Carvalho IS, Costa Júnior PB da, Macedo JBPO, Brito RS. Epidemiologic characterization of parturitions and births: an ecological study based on an information system. J Nurs UFPE on line. 2014; 8(3): 616-23. [ Links ]
7. Strengthening the Reporting of Observational Studies in Epidemiology. STROBE Statement: checklist of items that should be included in reports of cross-sectional studies. 2007. Available from: http://www.strobe-statement.org/fileadmin/Strobe/uploads/checklists/STROBE_checklist_v4_cross-sectional.pdf. Cited 2013 Aug 10. [ Links ]
8. Natal. Anuário Natal 2013. Natal: Secretaria Municipal de Meio Ambiente; 2013. [ Links ]
9. Silva FMB, Paixão TCR, Oliveira SMJV, Leite JS, Riesco MLG, Osava RH. Care in a birth center according to the recommendations of the World Health Organization. Rev Esc Enferm USP. 2013; 47(5): 1031-8. [ Links ]
10. Singata M, Tranmer J, Gyte GML. Restricting oral fluid and food intake during labour. Cochrane Database Syst Rev. 2013; (8): CD003930. [ Links ]
11. Figueiredo MS, Oliveira DKMA, Vieira NRS, Davim RMB, Silva RAR. Possíveis indicadores da assistência obstétrica a parturiente em uma maternidade escola. Cogitare Enferm. 2013; 18(4): 722-8. [ Links ]
12. d'Orsi E, Brüggemann OM, Diniz CS, Aguiar JM, Gusman CR, Torres JA, et al. Social inequalities and women's satisfaction with childbirth care in Brazil: a national hospital-based survey. Cad Saúde Pública. 2014; 30(sup 1): S1-15. [ Links ]
13. Diniz CSG, d'Orsi E, Domingues RMSM, Torres JA, Dias MABD, Schneck CA, et al. Implementation of the presence of companions during hospital admission for childbirth: data from the Birth in Brazil national survey. Cad Saúde Pública. 2014; 30(sup 1): S1-14. [ Links ]
14. Hodnett ED, Gates S, Hofmeyr GJ, Sakala C, Weston J. Continuous support for women during childbirth. Cochrane Database Syst Rev. 2013; (7): CD003766. [ Links ]
15. Stancato K, Vergílio MSTG, Bosco CS. Avaliação da estrutura e assistência em sala de pré-parto, parto e pós-parto imediato-PPP de um hospital universitário. Ciênc Cuid Saúde. 2011; 10(3): 541-8. [ Links ]
16. Jones L, Othman M, Dowswell T, Alfirevic Z, Gates S, Newburn M, et al. Pain management for women in labour: an overview of systematic reviews. Cochrane Database Syst Rev. 2012; (3): CD009234. [ Links ]
17. Giglio MRP, França E, Lamounier JA. Avaliação da qualidade da assistência ao parto normal. Rev Bras Ginecol Obstet. 2011; 33(10): 297-304. [ Links ]
18. Lawrence A, Lewis L, Hofmeyr GJ, Styles C. Maternal positions and mobility during first stage labour. Cochrane Database Syst Rev. 2013; (10): CD003934. [ Links ]
19. Barros LA, Veríssimo RCSS. Uso do partograma em maternidades escola de Alagoas. Rev RENE. 2011; 12(3): 555-60. [ Links ]
20. Lavender T, Hart A, Smyth RMD. Effect of partogram use on outcomes for women in spontaneous labour at term. Cochrane Database Syst Rev. 2013; (7): CD005461 [ Links ]
21. Moreira MEL, Gama SGN, Pereira APE, Silva AAM, Lansky S, Pinheiro RS, Gonçalves AC, et al. Clinical practices in the hospital care of healthy newborn infant in Brazil. Cad Saúde Pública. 2014; 30(sup 1): S1-12. [ Links ]
22. Ministério da Saúde. Iniciativa Hospital Amigo da Criança: revista, atualizada e ampliada para o cuidado integrado: módulo 1: histórico e implementação. Fundo das Nações Unidas para a Infância. Brasília: Ministério da Saúde; 2008. [ Links ]
23. Moore ER, Anderson GC, Bergman N, Dowswell T. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database Syst Rev. 2012; (5): CD003519. [ Links ]
24. Ministério da Saúde. Manual de acolhimento e classificação de risco em obstetrícia. Secretaria de Atenção à Saúde. Departamento de Ações Programáticas Estratégicas. Brasília: Ministério da Saúde; 2014. [ Links ]
25. Ministério da Saúde. Lei nº 11.634, de 27 de dezembro de 2007. Dispõe sobre o direito da gestante ao conhecimento e a vinculação à maternidade onde receberá assistência no âmbito do Sistema Único de Saúde. Diário Oficial da União 2007; 28 dez. [ Links ]
26. d'Orsi E, Chor D, Giffin K, Angulo-Tuesta A, Barbosa GP, Gama AS, et al. Qualidade da atenção ao parto em maternidades do Rio de Janeiro. Rev Saúde Pública. 2005; 39(4): 646-54. [ Links ]
27. Chalmers B, Kaczorowski J, Levitt C, Dzakpasu S, O'Brien B, Lee L, et al. Use of routine interventions in vaginal labor and birth: findings from the maternity experiences survey. Birth. 2009; 36(1): 13-25. [ Links ]
28. Reveiz L, Gaitán HG, Cuervo LG. Enemas during labour. Cochrane Database Syst Rev. 2013; (7): CD000330. [ Links ]
29. Basevi V, Lavender T. Routine perineal shaving on admission in labour. Cochrane Database Syst Rev. 2000; (1): CD001236. [ Links ]
30. Leal MC, Pereira APE, Domingues RMSM, Theme Filha MM, Dias MAB, Nakamura-Pereira M, et al. Obstetric interventions during labor and childbirth in Brazilian low-risk women. Cad Saúde Pública. 2014; 30(sup 1): s1-31. [ Links ]
31. Dawood F, Dowswell T, Quenby S. Intravenous fluids for reducing the duration of labour in low risk nulliparous women. Cochrane Database Syst Rev. 2013; (6): CD007715. [ Links ]
32. Bugg GJ, Siddiqui F, Thornton JG. Oxytocin versus no treatment or delayed treatment for slow progress in the first stage of spontaneous labour. Cochrane Database Syst Rev. 2013; (6): CD007123. [ Links ]
33. Sartore A, Seta F, Maso G, Ricci G, Alberico S, Borelli M, et al. The effects of uterine fundal pressure (Kristeller maneuver) on pelvic floor function after vaginal delivery. Arch Gynecol Obstet. 2012; 286(5): 135-9. [ Links ]
34. Verheijen EC, Raven JH, Hofmeyr GJ. Fundal pressure dung the second stage of labour. Cochrane Database Syst Rev. 2009; (4): CD006067. [ Links ]
35. Pádua KS, Osis MJD, Faúndes A, Barbosa AH, Moraes Filho OB. Factors associated with cesarean sections in Brazilian hospitals. Rev Saúde Pública. 2010; 44(1): 70-9. [ Links ]
36. Anim-Somuah M, Smyth RMD, Jones L. Epidural versus non-epidural or no analgesia in labour. Cochrane Database Syst Rev. 2011; (12): CD0000031. [ Links ]
37. Shepherd A, Cheyne H. The frequency and reasons for vaginal examinations in labour. Women Birth. 2013; 26(1): 49-54. [ Links ]
38. Downe S, Gyte GM, Dahlen HG, Singata M. Routine vaginal examinations for assessing progress of labour to improve outcomes for women and babies at term. Cochrane Database Syst Rev. 2013; (7): CD010088. [ Links ]
39. Borders N, Lawton R, Martin SR. A clinical audit of the number of vaginal examinations in Labor: a NOVEL idea. J Midwifery Womens Health. 2012; 57(2): 139-44. [ Links ]
40. Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database Syst Rev. 2009; (1): CD000081. [ Links ]
41. Pereira ALF, Nagipe SFSA, Lima GPVL, Nascimento SD, Gouveia MSF. Care and outcomes of relaxation room assistance at a public maternity hospital, Rio de Janeiro, Brazil. Texto contexto - enferm. 2012; 21(3): 566-73. [ Links ]
Received: January 05, 2018; Accepted: June 02, 2018











 texto en
texto en 


