Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Medicina Oral, Patología Oral y Cirugía Bucal (Internet)
versión On-line ISSN 1698-6946
Med. oral patol. oral cir.bucal (Internet) vol.12 no.1 ene. 2007
Evaluation of lidocaine and mepivacaine for inferior third molar surgery
Gabriela Granja Porto 1, Belmiro Cavalcanti Do Egito Vasconcelos 2,
Ana Cláudia Amorim Gomes 3, Daniela Albert 4
(1) Postgraduate Student of the MSc in Oral and Maxillofacial Surgery
(2) Senior Lecturer in Oral and Maxillofacial Surgery. Director of the Master and PhD programs in Oral and Maxillofacial Surgery
(3) Senior Lecturer in Oral and Maxillofacial Surgery
(4) Senior Resident, Department of Oral and Maxillofacial Surgery. University of Pernambuco (Recife-Brazil)
ABSTRACT
Objective: The aim of this study was to compare 2% lidocaine and 2% mepivacaine with 1:100,000 epinephrine for postoperative pain control.
Study design: A group of 35 patients, both genders were recruited, whose had ages ranged from 13 to 27 years-old and had two inferior third molars in similar positions to be extracted. The cartridges were distributed to the patients according to a randomised pattern, where lidocaine was in the control group and mepivacaine in the experimental group. Results: Results showed no significant association between the anesthetics and postoperative pain, pulp sensibility after one hour, gender, tooth position and duration of the surgical procedure.
Conclusions: It was shown that lidocaine and mepivacaine have similar time of anesthesia, they are adequate for surgical procedures that last one hour, and there was no difference between the two anesthetics in relation to the severety of post-operative pain.
Key words: Local anesthetics, post-operative pain/surgery, lidocaine/therapeutic use, mepivacaine/therapeutic use, third molar/surgery.
Introduction
Local anesthetics are the most widely used drugs in dentisty today, which when coming into contact with the nerve fiber interrupt the propagation of the nerve impulse in a lasting and reversible manner (1). A continued improvement in these injectable agents has contributed more than any other factor to the control of pain during dental surgery and especially after it.
Surgical removal of lower third molars is a common oral surgical procedure which causes more severe pain in comparison to the other types of oral surgery and can consequently interfere with the patients everyday life.
Among the several commercially available anesthetic solutions, lidocaine is the one most frequently used in dentistry, being the benchmark for comparison. It is an amide anesthetic with a short onset of action and an intermediate duration of anesthesia when associated with adrenaline (2). It has been shown that lidocaine and mepivacaine, which is also an amide anesthetic, in the same concentrations and with the same vasoconstrictors have a similar effect (3). In the reviewed literature, however, there are few studies comparing both anesthetics in relation to the postoperative effects, pain reduction and the patients comfort.
The aim of this study was to evaluate anesthetic effectiveness and postoperative pain after using 2% lidocaine and 2% mepivacaine, both with epinephrine 1:100,000 as the local anesthetic for impacted inferior third molar surgery.
Material and methods
A double-blind, randomised, longitudinal study was conducted between May and September 2004 at the Division of Oral and Maxillofacial Surgery at the University of Pernambuco in Recife, Brazil. The trial protocol was approved by the university´s Ethics Committee and the informed written consent was obtained from each patient. The total number of subjects was calculated through a pilot sample using the means and standard deviation of the intensity of pain, for a power analysis of 0.80377 the total sample was 68 surgeries.
The study sample involved thirty-five patients (25 females and 10 males), aged 13-27 years, with weights ranging from 42 kg to 76 kg and consecutively enrolled for the surgical extraction of an impacted lower third molar under local anesthesia, total of 70 surgeries. Only patients classified as ASA I by the American Society of Anesthesiology (4) and without a history of significant systemic pathology were included.
To be included in this study, each patient had to have two lower third molars in a similar position by the Pell & Gregory classification and classified as mesioangular and vertical by the Winter classification (5).
Two groups were established (n=35 each) on a randomized basis (by allotment), according to the anesthetic solution 2% lidocaine (ALPHACAINE®/DFL) and 2% mepivacaine (MEPIADRE®DFL) with 1/100,000 epinephrine.
The anesthetic technique comprised truncal blockage of the inferior dental nerve, with infiltrating anesthesia of the vestibular zone of the lower third molar. A minimum of two cartridges (1.8 ml each) was estabilished per patient; if more anesthetic was necessary the amount in millimeters was recorded.
Personal data were recorded for each patient, along with the classification of molar extraction difficulty according to Pell & Gregory and Winter, the duration of the procedure (initiated 5 minutes after the application of the anesthesia and considered finished after the suture), the amount of reanesthesia, whether osteotomy and tooth section were needed and the sensibility of the pulp to Endofrost® (cold test) after one hour of anesthesia (6, 7).
After the procedure was completed, each patient was given postoperative instructions, medication for pain (50 mg Sodium Diclofenac 8/8hs for three days and 500 mg Dipyrone in case of pain), and a questionnaire to fill out and return at the next appointment within seven days. In this questionnaire patients were asked to note the time of return of normal sensation to the lower lip, the time of the onset and intensity of pain according to a visual analog scale (100 mm scale). If the patient marked a point between 1 and 25 mm the pain was considered as mild, between 26 and 50 mm moderate, from 51 to 75 mm intense and between 76 and 100 unbearable.
Results
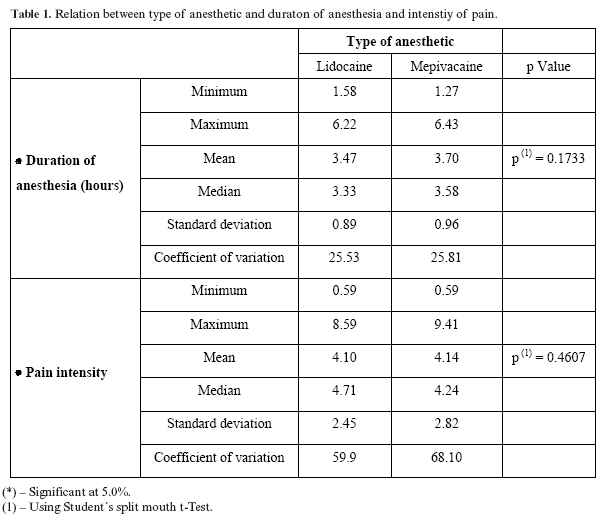
As seen in Table 1, there was no significant difference between the two local anesthetics in terms of duration of anesthesia and intensity of postoperative pain.
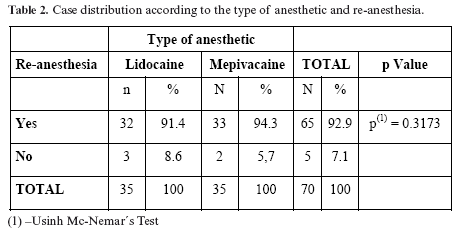
Only in five procedures was reanesthesia necessary, three of them when using Lidocaine and two when using Mepivacaine, but there were no significant differences (Table 2).
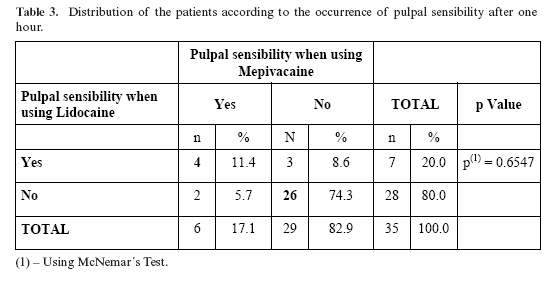
In Table 3, it is shown that there were more cases with pulpal sensibility when using Lidocaine than when using Mepivacaine (20.0% versus 17.1%) and 74.3% of all patients had no pulpal sensibility for either anesthetic one hour after the surgery had started.
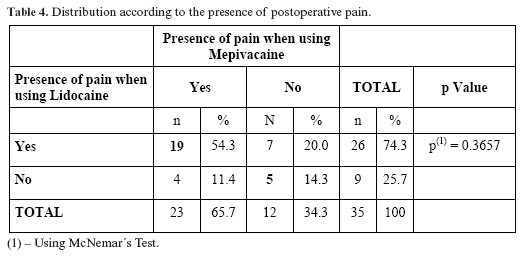
The majority of the patients felt some pain with each anesthetic, 74.3% when using Lidocaine and 65.7% when using Mepivacaine and 54.3% for both. But there were no significant differences between postoperative pain and the two anesthetics (Table 4).
About half the teeth (48.6%) were in vertical position and the other half in the mesio-angular; 42.9% were classified as B and 57.1% as C; 75.7% were classified as degree of retention II, all of which were about the same for both anesthetics.
The intensity of pain in relation to gender was greater for females than for males in each type of anesthetic, although this difference was not significant for either Lidocaine (p=0.1837) or Mepivacaine (p=0.2893).
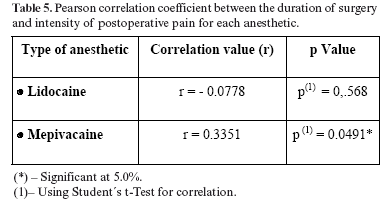
The relation between the duration of surgery and the intensity of pain was studied using the Pearson correlation coefficient, which showed that there is no proportional correlation between them for either anesthetic. Although the coefficient value for Mepivacaine was different from zero, this value is too low for these two variables to be deemed to have a proportional correlation (Table 5).
Discussion
Postoperative pain control has been the subject of continuous research in the field of oral and maxillofacial surgery, since the pain can interfere with patients quality of life. Several authors have studied ways to control it: such as the use of long-acting local anesthetics to decrease analgesic intake, the preoperative prescription of steroidal anti-inflammatory for less edema and pain and the postoperative use of soft tissues laser for better healing and decreased postoperative pain and inflammation (6, 8-12).
In this study the evaluation of postoperative pain was made using visual analog scale, reported by the literature to be a sensitive and realible method for recording pain, and considered to be better than the verbal, digital, numerical and descriptive scales (13).
The patient´s weight ranged from 42 to 76 kg and the same dosage of both solutions was used: 72 mg, which means two cartridges at different times in the same individual. The coefficient of variation was not high, which means that the weight did not influence the total dosage used. If this variation were high the total anesthetic dosage could interfere with the anesthesia, as heavier patients might be given an underdose and less heavy ones an overdose of the solution.
In Table 1, it is shown that the duration of anesthesia for Lidocaine and Mepivacaine was similar using the soft tissue benchmark, minimum and maximum durations in hours being 1.58 hr and 1.27 hr and 6.22 and 6.43 respectively.
This means the duration of the effect of both solutions was also similar, which is at variance with Aspa et al. (14) and Faria, Marzola (15) who state that Mepivacaine had a longer time of action than Lidocaine. This statement, however, is in agreement with most of the literature, which states that Lidocaines effect lasts from 170 to 180 minutes (3, 11) or from 90 to 180 minutes according to Hawkins, Moore (16) and Budenz (17). In our study the duration of action of Mepivacaine corresponds with that of Berini-Aytés, Gay-Escoda (3) and Budenz (17) who state it to be from 3 to 4 hours for soft tissues. The minimum duration for Mepivacaine in our study is in agreement with Mallamed (18).
In Table 3, pulpal sensibility using Mepivacaine for one hour was present in 20.7% of the patients and in 24.1% of those using Lidocaine. Nevertheless, 69% responded negatively for the cold test, which means that both solutions are effective for surgical procedures that last up to 60 minutes, which is in agreement with the literature reviewed here (3, 17).
In relation to postoperative pain, the figures for both anesthestics were about the same: 74.3% for Lidocaine and 65.7% for Mepivacaine (Table 4), which is in agreement with Berini-Aytés, Gay-Escoda (3) when they state that Lidocaine and Mepivacaine used with the same vasoconstrictor have a similar action.
In this study the women reported more pain than men, although this difference was not significant. Most authors state that women in general report more pain, maybe because they have a greater sensitivity and lower tolerance to pain than men (19, 20).
The length of time that it takes to remove an impacted lower third molar has no discernible bearing on the pain experienced by the patient, which is in agreement with Seymour, Blair, Wyatt (20). It was observed that even though the mean duration of surgery with Lidocaine was greater than with Mepivacaine, the intensity of postoperative pain for both was similar.
According to the Winter classification, both lower third molars of each patient were similar. In relation to the Pell & Gregory classification, the teeth were also in similar positions for both anesthetics: ¾ were classified as grade II; a little less than half were classified as B and the rest as C. Even so, the intensity of pain for both solutions varied mostly from mild to moderate, but it is to be expected that the pain would get intense as most teeth were in positions classified as difficult. Nonetheless, this may be stated, on the basis of the present study, that the intensity of pain is not related to the degree of difficulty of the procedure, which is in agreemeent with Seymour, Meechan, Blair (21) and Danielsson et al. (22), but at variance with Oikarinen (11) and Chaparro-Avendano et al. (23).
Table 5 shows the correlation coefficient between the duration of surgery and the intensity of postoperative pain. The value for Lidocaine is close to zero and for Mepivacaine a little above zero; in neither case these variables are considered to be proportional (2). This means that the duration of the surgery is not related to the intensity of pain, which is in agreement with Seymour, Blair, Wyatt (20), and at variance with Oikarinen (11), who states that the greater the duration of surgery, the more intense is the pain.
Conclusions
Lidocaine and Mepivacaine with the same vasoconstrictor had a similar action and both solutions are effective in surgical procedures lasting up to 60 minutes. There were also no significant differences between them in relation to the intensity of postoperative pain.
References
1. Pipa-Vallejo A, Garcia-Pola-Vallejo MJ. Local anesthetics in dentistry. Med Oral Patol Oral Cir Bucal 2004;9:440-3. [ Links ]
2. Oliveira PC, Volpato MC, Ramacciato JC, Ranali J. Articaine and lignocaine efficiency in infiltration anaesthesia: a pilot study. Br Dent J 2004;197:45-6.
3. Berini-Aytes L, Gay-Escoda C, eds. Anestesia Odontologica. Madrid: Ediciones Avances; 2000. p. 552.
4. Keats AS. The ASA classification of physical status – a recapitulation. Anesthesiol 1978;49:233-6.
5. Peterson LJ, Ellis E, Hupp JR, Tucker MR, eds. Cirurgia Oral e Maxilofacial Comtemporânea. Rio de Janeiro: Guanabara Koogan; 2000. p. 702.
6. Oka S, Shimamoto C, Kyoda N, Misaki T. Comparison of lidocaine with and without bupivacaine for local dental anesthesia. Anesth Prog 1997;44:83-6.
7. Smith E, Dickson M, Evans AL, Smith D, Murray CA. An evaluation of the use of tooth temperature to assess human pulp vitality. Int Endod J 2004;37:374-80.
8. Bouloux GF, Moorthy AP. Bupivacaine versus lidocaine for third molar surgery: a double-blind, randomized, crossover study. J Oral Maxillofac Surg 1999;57:510-4.
9. Dionne RA, Wirdzek PR, Fox PC, Dubner R. Suppression of postoperative pain by the combination of a nonsteroidal anti-inflammatory drug, flubiprofen, and a long-acting local anesthetic, etidocaine. JADA 1984;108:598-601.
10. Gay-Escoda C, Berini-Aytés L, eds. Cirugía Bucal. Madrid: Ergon; 1999. p. 934.
11. Oikarinen K. Postoperative pain after mandibular third-molar surgery. ACTA Odontol Scand 1991;49:7-13.
12. Rosenquist JB, Nystrom E. Long-acting analgesic or long-acting local anesthesic in controlling immediate postoperative pain after lower third molar. Anesth Prog 1987;6:6-9.
13. Tuffin JR, Cunliffe DR, Shaw SR. Do local analgesics injected at the time of third molar removal under general anaesthesia reduce significantly post operative analgesic requirements? A double-blind controlled trial. Br J Oral Maxillofac Surg 1989;27:27-32.
14. Aspa RM, Fabregat MP, Penalva MP, Aytés BL, Gay-Escoda C. Evaluación de los efectos anestésicos obtenidos con dos soluciones diferentes de mepivacaína al 3% después de un bloqueo mandibular. Archivos de Odonto-Estomatologia 2000;16:239-47.
15. Faria FAC, Marzola C. Farmacologia dos anestésicos locais – considerações gerais. BCI 2001;8:19-30.
16. Hawkins JM, Moore PA. Local anesthesia: advances in agents and techniques. Dent Clin North Am 2002;46:719-32.
17. Budenz AW. Local anesthesics in dentistry: then and now. J Calif Dent Assoc 2003;31:388-96.
18. Mallamed SF. Local anesthetics: dentristrys most important drugs. J Am Dent Assoc 1994;125:1571-6.
19. Chapman PJ. Postoperative pain control for outpacient oral surgery. Int J Oral Maxillofac Surg 1987;16:319-24.
20. Seymour RA, Blair GS, Wyatt FAR. Post-operative dental pain and analgesic efficacy. Br J Oral Maxillofac Surg 1983;21:290-7.
21. Seymour RA, Meechan JG, Blair GS. An investigation into post-operative pain after third molar surgery under local analgesia. Br J Oral Maxillofac Surg 1985;23;410-8.
22. Danielsson K, Evers H, Holmlund A, Kjellman O, Nordenram A, Persson NE. Long-acting local anaesthetics in oral surgery: clinical evaluation of bupivacaine and etidocaine for mandibular nerve block. Int J Oral Maxillofac Surg 1986;15:119-26.
23. Chaparro-Avendano AV, Perez-Garcia S, Valmaseda-Castellon E, Berini-Aytes L, Gay-Escoda C. Morbidity of third molar extraction in patients between 12 and 18 years of age. Med Oral Patol Oral Cir Bucal 2005;10:422-31.
![]() Correspondence:
Correspondence:
Prof. Dr. Belmiro Cavalcanti do Egito Vasconcelos
Faculdade de Odontologia de Pernambuco.
Universidade de Pernambuco.
Av. General Newton Cavalcanti, 1650
Camaragibe – Pernambuco. CEP: 54753-220
E-mail: belmiro@fop.upe.br
Received: 1-10-2005
Accepted: 16-06-2006