INTRODUCTION
The substantial success of immunization in ameliorating human health by preventing, controlling, and for some cases, eradicating infectious diseases has been well documented.1,2 Globally, a rough estimate of 2 to 3 million deaths due to diphtheria, whooping cough (pertussis), measles, and tetanus were averted annually because of immunization.3 Over the last two decades, in the Western Pacific Region alone, immunizations have saved millions of lives and prevented disabilities in children, stopped the spread of wild poliovirus, and visibly dropped the spread of measles and hepatitis B virus.4
The impetus of vaccination program that can reach global population is the Expanded Program on Immunization (EPI) which was established by World Health Assembly in 1974 and took focus on developing or maintaining immunization and surveillance programs against poliomyelitis, tuberculosis, diphtheria, whooping cough (pertussis), and measles.5 Tetanus was later added to the program.1 Proper storage of vaccines from manufacturing process to administration must be done to ensure the effectiveness of immunizations.6 Therefore, cold chain, or vaccine cold chain, plays a pivotal role in the activities of this EPI program.7 Cold-chain system is designed to cope with inherent temperature sensitivity of vaccines due to either their antigen structure or their additives and adjuvants.8
Three main components of cold chain include transport and storage equipment, personnel training, and efficient management procedures.6 Potency loss of vaccines can occur during every part of the chain including the long-term storage, shipping from the manufacturers to distribution centers, and just before the administration.2 The causes of potency loss can be excessive exposure to heat, freeze, or light.7 The temperature range recommended to store and transport vaccines by the WHO is 0-10ºC. This range is intended for diptheria-tetanus containing vaccines, tetanus toxoid (TT), hepatitis A and B, human papillomavirus (HPV), meningitis C, pneumococcal (PCV), cholera, influenza, haemophilus influenza b (Hib), typhoid and inactivated poliovirus (IPV).9,10 Ideally, vaccine should not be stored in a dormitory-style refrigerator because it does not support temperature regulation and monitoring.6
Problems related to cold chain occur in every country that has had a surveillance for vaccine temperature monitoring; meaning it may certainly not only happen in developing countries.8 Although cold chain is commonly thought to avoid vaccine inactivation due to exposure to heat, it is necessary to also highlight potency loss due to exposure to freezing temperatures resulting to inactivation of aluminum added as adjuvant to vaccines.2,10 Vaccines such as OPV, measles, varicella, oral typhoid are unstable to heat, while other vaccines such as DTP, HepA, HepB, and TT are sensitive to freezing.8 It is believed that overheating problem is more common in developing countries; conversely accidental exposures to freezing temperatures are more likely in developed countries.7 The latter has an estimated 33.3% of vaccine storage units exposed to freezing temperatures, while in the former, the figure was slightly higher, 37.1%.10 This figure is surprisingly higher than the findings in 2007 that the occurrence of exposure to temperatures below the recommended range was 29% in developed countries and 21.9% in developing countries.10 Several responsible factors of overheating in developing countries are tropical climates, unreliable electricity, and shortage of resources (equipment, finances, and manpower).7 Research in Cameroon highlighted that excessive exposure to heat was recorded in 24% of surveyed refrigerators and this was linked with the absence of alternative source of power (OR=6.5, p=0.03).7
Improving cold chain capacity and logistics throughout innovation becomes an activity of the Global Vaccine Action Plan in the Western Pacific.4 Since 2003, 80 provinces, 38 cities, and 16 regions in the Philippines have been upgraded with the cold chain equipment.11 However, it seems that research on this matter is still limited in number. In a recent thorough literature review, only one study about cold chain from the Philippines in 2010 was included.10 Therefore, this study aimed to assess current cold chain management of the rural health units of Consolacion and Liloan, Cebu, Philippines.
METHODS
Study Design and Setting
This cross-sectional analytical survey was conducted from August to September 2017 in the towns of Consolacion and Liloan, Cebu. Both towns were chosen to be surveyed to assess the functionality of the cold chain management of vaccines in their respective Rural Health Units (RHU). Letters of permission were sent to the municipal mayor of each town and were referred to their respective planning departments on May 2017. In Consolacion, the head of the planning office disseminated an endorsement letter to each barangay health center that served as notification for the conduct of the cold-chain survey. In Liloan, the head of the rural health unit endorsed the request to the medical health officer and nurse supervisor and was eventually granted permission.
Data was obtained using a structured questionnaire, which was developed based on the US CDC Pinkbook12 and some research reports of cold-chain survey.13,14 This questionnaire was administered to one personnel who is responsible for the storage and maintenance of vaccines in each barangay health center. Thirty minutes was allotted to explain the consent form and questionnaire to the respondent, as well as answering clarifications from the respondents. The respondent, who gave consent, was given 10-15 minutes to answer the questionnaire.
Participants, Eligibility Criteria, and Sample Size
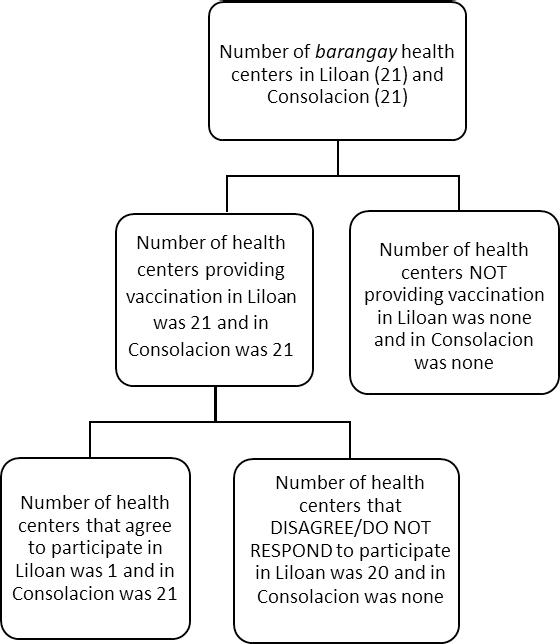
Participants in this study were the personnel-in-charge of each health centers in both towns. A total number of 42 barangay health centers were identified from Liloan and Consolacion. Only health centers that provide vaccination in both towns were included in the study as some health centers do not provide vaccination services. An informed consent was presented to the personnel-in-charge of each health center and those that signed the consent were included in the survey. Thus, health centers that gave their consent were counted as an eligible health center for the study, which was the basis for the sample size (Figure 1).
Variables
Outcome variable is the knowledge of personnel in terms of vaccine storage management. Explanatory variables were divided into three major groups: the basic information of health centers, cold-chain facilities, and socio-demographic information of health personnel assigned to fill up the questionnaire. Variables about the identity of health centers include urban/rural status, number of staff, types of vaccines provided, and an updated population in the area. Cold-chain facility variables comprise the availability of functional refrigerators, freezers, cold boxes, ice packs, and thermometers. Variables related to facilities also include source of electricity, availability of generator sets, availability of voltage stabilizers, and a standard procedure if outage happens. Variables related to health personnel include age, sex, professional status, and experience to participate in a workshop of cold-chain management.
Statistical Methods
Descriptive statistics in the form of percentage was used for qualitative data. Pearson’s Chi-Square or Fisher’s Exact Test with Cramer’s V value was used to explore the association between the statuses of PHCs to store vaccine and the level of knowledge of health personnel. Statistical analyses were conducted using Stata v. 13 (StataCorp, College Station, Texas, USA) and an alpha of 0.05 was used as cut-off for significance.
Ethical Considerations
Prior to the actual survey, ethical review was sought to the Ethics Committee of University of San Carlos, Cebu City, Philippines. Approval was granted with the number 008-2017-06. During the actual survey, informed consent was sought from all barangay health centers. The researchers allotted 30 minutes to read and explain the informed consent and the questionnaire, as well as to answer any clarifications from the respondents. Once the respondents signed the consent paper, the questionnaire was administered immediately. The name of the health personnel in each barangay health center interviewed by the researchers were coded as initials. Identity of involved health centers were also coded. Raw data can only be accessed by the research team. Data was presented as aggregate within any publication generated by this research.
Withdrawal Criteria
The respondents may refuse to participate in the study at any time without affecting their relationship with the investigators of the study. Their decision would not result in any loss or benefits to which they were otherwise entitled to. They had the right not to answer any single question, as well as to withdraw completely from the interview at any point during the process; additionally, they had the right to request that the interviewer should not use any of the interview material.
RESULTS
Table 1 presents the availability of storage units and equipment of PHCs surveyed. Out of 22 respondents, only 5 (22.7%) store vaccines. Four out of five have functional refrigerator/freezer; the other carried more than one unit. The other 17 facilities claimed to provide vaccination services but lack the basic equipment essential for storing vaccines as only 7 had at least one functional refrigerator/freezer. All 22 PHCs have cold boxes and ice packs available for 24-hour vaccine storage and transport. As vaccination is part of the service provided by primary health centers, appropriate equipment for storage is important.
Table 1. Availability of Storage Units and Equipment
| Storage units and equipments | Store Vaccine | |
|---|---|---|
| Yes (%) | No (%) | |
| Functional refrigerators available in the PHC | ||
| None | 0 | 10 (45.5) |
| One | 4 (18.2) | 7 (31.8) |
| > 1 | 1 (4.5) | 0 |
| Functional freezers available in the PHC | ||
| None | 0 | 10 (45.5) |
| One | 4 (18.2) | 7 (31.8) |
| > 1 | 1 (4.5) | 0 |
| PHC with available cold boxes | 5 (22.7) | 17 (77.3) |
| PHC with available ice packs | 5 (22.7) | 17 (77.3) |
Table 2 shows the power source available and necessary back-ups for the PHCs. All 22 PHCs use electricity as their main power source. Only 1 out of 5 PHCs that store vaccine had a back-up generator for use in the event of power outage. The same trend is seen in the use of an automatic voltage stabilizer. Five PHCs have available contingency plans in case of power outage but only 2 out of 5 posted their plan near the refrigerator.
Table 2. Source of Power
| Electricity | Store Vaccine | |
|---|---|---|
| Yes (%) | No (%) | |
| Main source of power supply | ||
| Electricity | 5 (22.7) | 17 (77.3) |
| Gas | 0 | 0 |
| Kerosene | 0 | 0 |
| Accessible generator | ||
| Yes | 1 (4.5) | 1 (4.5) |
| No | 4 (18.2) | 16 (72.7) |
| The refrigerator is connected to an automatic voltage stabilizer | ||
| Yes | 1 (4.5) | 1 (4.5) |
| No | 4 (18.2) | 8 (36.4) |
| Don’t know | 0 | 8 (36.4) |
| A contingency plan for outage available in the PHC | ||
| Yes | 5 (22.7) | 7 (31.8) |
| No | 0 | 2 (9.1) |
| Don’t know | 0 | 8 (36.4) |
| The contingency plan is pasted near the fridge | ||
| Yes | 2 (9.1) | 6 (27.3) |
| No | 2 (9.1) | 2 (9.1) |
| Don’t know | 0 | 8 (36.4) |
| Other | 1 (4.5) | 1 (4.5) |
Table 3 lists the temperature monitoring and availability of thermometers. Of the 5 PHCs that store vaccines, 4 have refrigerators equipped with a functional thermometer and they are placed inside the refrigerators. Four PHCs monitor the temperature of the refrigerator twice daily while the other indicated no pattern of monitoring. All 5 PHCs had at least one refrigerator with temperature between 2ºC-8ºC and only stores vaccine inside.
Table 3. Temperature monitoring and other items inside the refrigerator
| Temperature Monitoring and Other Items | Store Vaccine | |
|---|---|---|
| Yes (%) | No (%) | |
| Refrigerator is equipped with a functional thermometer | ||
| Yes | 4 (18.2) | 11 (50.0) |
| No | 1 (4.5) | 2 (9.1) |
| Don’t know | 0 | 4 (18.2) |
| Thermometer is placed inside the refrigerator | ||
| Yes | 5 (22.7) | 9 (40.9) |
| No | 0 | 3 (13.6) |
| Don’t know | 0 | 5 (22.7) |
| Temperature monitoring chart is maintained regularly | ||
| No | 1 (4.5) | 2 (9.1) |
| Once daily | 0 | 2 (9.1) |
| Twice daily | 4 (18.2) | 1 (4.5) |
| >Twice daily | 0 | 7 (31.8) |
| Don’t know | 0 | 5 (22.7) |
| At the moment of observation, at least one refrigerator is with temperature between common recommended range (2ºC-8ºC) | ||
| Yes | 5 (22.7) | 11 (50.0) |
| No | 0 | 3 (13.6) |
| Don’t know | 0 | 3 (13.6) |
| Other items, especially non-medicine ones, are present with vaccines. | ||
| Yes | 0 | 0 |
| No | 5 (22.7) | 17 (77.3) |
| Don’t know | 0 | 0 |
In Table 4, the respondents (n=22) unanimously agreed that incidence of vaccine-preventable diseases are related to improper handling and storage of vaccines; that its potency may decrease when mishandled; that patients’ confidence in the vaccines may decrease and cost due to wastage and re-vaccination increased. Some respondents (77.3%) did not know the best method to store vaccines while 59.1% did not know where the thermometer must be placed in the storage units. Majority of the respondents (95.5%) did not believe that each transport of vaccines may increase the risk of their exposure to improper storage conditions compromising their quality and potency.
Table 4. Knowledge Assessment on the Personnel-in-charge of the Cold Chain System
| Questions | Answer (n=22) | |
|---|---|---|
| Correct (n,%) | Incorrect (n, %) | |
| Do you think that the incidence of vaccine-preventable diseases are correlated with proper storage and handling of vaccines? | 22 (100) | 0 |
| Do you think improper storage and handling of vaccines can decrease potency and effectiveness? | 22 (100) | 0 |
| Do you think improper storage and handling of vaccines can increase cost due to wasted vaccine and revaccination? | 22 (100) | 0 |
| Do you think improper storage and handling of vaccines can enhance patient confidence? | 22 (100) | 0 |
| Do you think it is better to not vaccinate than to administer a dose of mishandled vaccine? | 21 (95.5) | 1 (4.5) |
| Do you think the temperature in storage unit(s) (i.e. refrigerator) should be monitored at least twice a day? | 16 (72.7) | 6 (27.3) |
| Which method is best applied to store the vaccines? | 5 (22.7) | 17 (77.3) |
| Do you think all vaccines must not be stored in freezer? | 20 (90.9) | 2 (9.1) |
| Do you think food and beverages should be allowed to be stored in the same unit with vaccines? | 22 (100) | 0 |
| Do you think that an emergency plan must be made to anticipate unwanted situations such as outage and disaster? | 14 (63.6) | 8 (36.4) |
| Where should be the temperature monitoring device (i.e. thermometer) placed inside the storage unit(s)? | 9 (40.9) | 13 (59.1) |
| Do you think each transport may increase the risk that vaccines could be exposed to improper storage condtion? | 21 (95.5) | 1 (4.5) |
There was no significant relationship between the statuses of PHCs to store vaccine and the level of knowledge based on Fisher’s exact test (p=0.159). However, this result could be because of the relatively small sample size. Additionally, the Cramer’s V value is moderate in measuring the strength of the relationship (0.4).
DISCUSSION
This small study was conducted to evaluate the functioning status of the cold chain system in the northern part of Cebu, particularly the towns of Consolacion and Liloan. Initially, the researchers planned to survey all PHCs in the towns of Consolacion and Liloan, in which both have 21 PHCs and would have totaled to 42 PHCs/respondents. However, only 1 PHC, which was the main health center have been surveyed in Liloan since the medical health supervisor did not consent for the survey in other PHCs around town. Therefore, a total of 22 respondents have been surveyed for this study which was also equivalent to 22 PHCs evaluated.
Stated in RA No. 3720 also known as Food, Drugs, and Cosmetics Act, as amended by EO No. 175 and in line with the objectives of the Department of Health AO No. 56 s 1989, 27 s 2001, and 47-A s 2001, are the requirements for outlets handling vaccines and other biological products to ensure cold chain management efficiency. This covers facility and equipment, monitoring tools, and personnel requirements. Only 22.7% of the 22 respondents store vaccines and the remaining 77.3% do not store vaccines but claimed to provide vaccination. This setup is prevalent in most places in Cebu since not all public health centers are equipped with a functional refrigerator or has a personnel who is trained in the proper storage and handling of vaccines. The respondents stated that the PHCs that do not store vaccines obtained the vaccines from another PHC. These vaccines were used on that same day of delivery. That is why 100% of the respondents have cold boxes and ice packs in their respective PHCs for a short-time storage and delivery of vaccines around town. This practice may result to predisposing vaccines to overheating and long term exposure which can consequently lead to damage and loss of potency as observed in a study in Cameroon.13 The PHCs that do not carry vaccines ideally should not provide immunization services. However, due to geographical challenges, residents near the PHC requests that vaccination be made available. That explains why the vaccines should be transported by some means and that poses a risk on the quality of the vaccines being provided to the residents.
Power outage is common in developing countries15; hence, each of the PHCs should have an accessible generator or a contingency plan for vaccine storage in order to ensure the vaccines’ shelf life. The personnel-in-charge must have a standard operating procedure (SOP) that must be strictly followed and these should be placed in an accessible area, preferably near or on the refrigerator where everyone could read it. Among the 5 respondents who store vaccines, only 1 has an accessible generator while 4 of them do not. Fluctuations of electric current could be a concern so voltage stabilizers are used to feed constant voltage to the refrigerator and protects it from damage due to fluctuations. Of the 5 respondents that store vaccines, only 1 had a refrigerator connected to a voltage stabilizer while the other 4 were not. A study by Buledi et al.16 reported similar predicament in Pakistan where among 42 respondents, 74% had no voltage regulators and 90% did not have standby power generators. Power outage and fluctuations are common and standby generators and voltage regulators are not common in PHCs. The appropriate government agencies must look into this to avoid wasting of expensive vaccines that may be damaged as a consequence of inefficient power supply and poor address of power outages and fluctuations.
All vaccines have a designated storage condition that would determine the temperature for its storage and handling. These conditions must be strictly followed to retain the vaccines’ potency and therapeutic effectiveness. Therefore, all refrigerators should have a working thermometer to monitor its temperature. The personnel-in-charge in each PHC should monitor the temperature at least twice a day as suggested by the Food and Drug Administration (FDA) Philippines to ensure that the storage conditions of every vaccine is followed. A temperature monitoring chart for each refrigerators should be made available.17 Surprisingly, the researchers found out that one PHC that carries vaccines does not update the temperature monitoring chart at all. A report from Pakistan found out that 43% of 42 centers do not maintain twice daily temperature monitoring.16 Another study found that 55.3% (n=425) did not have temperature logging charts at all. 65.4% had no thermometers and among those who have only 90.5% were functional. A similar study conducted in India in 2012 shows that all their surveyed PHCs had dial thermometers for monitoring the temperature.18 Dial thermometers are no longer recommended as they lose their calibration over time especially when they are dropped.19 WHO states that the use of thermometers are as back-up device for temperature monitoring as they do not require batteries or power supply to use. They have been replaced by more efficient and better devices.19 While the thermometers no longer meet the requirement of WHO, these have remained useful especially in developing countries. Over time, ideal monitoring devices such as 30-day electronic temperature logger should be used.
The knowledge of personnel-in-charge of handling vaccines on cold chain system was assessed and revealed some worrisome results. Some respondents (27.3%) were not aware that temperature in the refrigerator must be monitored at least twice daily.19 A study by Naik et al.20 had better findings citing 95% of their respondents know appropriate monitoring frequency. The present study reports 77.3% did not know the best method to store vaccines as opposed to only 10% from the same cited study. Another study by Rao et al.18 shows 97.4% knows the ideal equipment for storage of vaccines while findings in this study has a lower value, at 90.9%. The cited studies were conducted in India, also a developing country yet it appears their personnel are more adept and knowledgeable in handling vaccines and about the cold chain system. This study reported that 59.1% of the personnel in PHCs in Liloan and Consolacion, Cebu did not know where the thermometer must be placed inside the refrigerator for correct temperature monitoring. Even if regular monitoring of temperature is done, incorrect reading may be recorded if the thermometer is not placed correctly. Some respondents (36.4%) did not see the need for an emergency plan to anticipate situations such as power outage and disaster. Stressing on the cost of these vaccines, not having a backup plan in case of emergency may result to wastage of the vaccines or the risk of administering ineffective vaccines to recipients. The researchers would like to point out that the need for updating the training of the personnel be given priority. As there are limitations in terms of ideal equipment availability, investment should be placed on updating the training of the personnel so that no further compromise may be placed on potency of vaccines. National guidelines must be disseminated to all personnel handling vaccines and be followed accordingly. An interesting commentary article mentions that countries can no longer rely on a few trained personnel to distribute vaccines that are costly.21 Improvement of distribution will require substantial increase on the number, training, and retention of logistics staff. It is good to note that several countries have started to offer degree programs in health supply chain management at the Masters level.21 This signifies that advance degrees and leadership development programs create a capable workforce who understands the sensitivity of vaccines.
The data collected is based on the answers of each respondents on the provided structured-survey questionnaires. Hence, those who do not answer truthfully or is having difficulty in recalling the right information predisposes the results obtained to dishonesty and recall bias. Not all targeted PHCs/respondents gave consent to the study thus, the non-response rate had affected or biased the final results of the study. The same limitations from a study by Yakum et al.13 indicated that there could be bias in the results knowing that the study was conducted at a particular period of the year and that the researchers could hardly know what happens throughout the year. Furthermore, updating the temperature twice daily or at the moment of observation with a thermometer may not actually show the extent of vaccine exposure to sub-optimal temperatures since the study only reported the exposure of vaccines to sub-optimal temperatures at the storage unit or equipment and vaccines can equally be exposed to sub-optimal temperatures during transfer and transportation to other PHCs.
CONCLUSIONS
The results of the study indicated that the availability of storage units and equipment was acceptable. The availability of power supply was also satisfactory since all PHCs use electricity. However, in terms of temperature monitoring, the results were not satisfactory. In the assessment of knowledge for each personnel, it was revealed from the statistical analysis made that there was no relationship between the statuses of public health centers to store vaccines and the level of knowledge of each personnel handling them. However, it is difficult to make a definite conclusion for this since the sample size was too small. Improvement of cold-chain management for vaccines in PHCs in Cebu is necessary. The main emphasis should be on power supply-related issues and the knowledge of health professionals who handles vaccines.