INTRODUCTION
It is estimated that 1 in 100,000 individuals identify as transgender or gender non-conforming, however this estimation is grossly conservative and some studies have shown drastically different numbers such as 1 in 200 individuals.1-3 This discrepancy is due to deficiencies in official records, stigma, and faults in the methodologies of studies targeting the demographic variables of transgender populations.3,4 Official records such as the US Census do not include data on gender identity.5 Moreover, past studies where surveys are used to collect demographic data on the transgender population have failed in using standardized questions that consider the gender identity of the respondents. This lack of representation creates a barrier when trying to determine health disparities faced by transgender and gender non-conforming individuals.
In a survey that included 6,450 transgender and gender non-conforming participants from all 50 states, the District of Columbia and Puerto Rico, 50% of the participants showed health disparities such as lack of insurance and frequent discrimination in the form of refusal of care or verbal harassment by health providers.6 These are significant healthcare barriers that can be attributed in part to the lack of knowledge health providers display regarding the care of transgender patients. In fact, this gap in knowledge left half of the transgender patients reporting the need to “teach” their medical providers on how to provide appropriate care. The lack of knowledgeable healthcare providers, coupled with the fear of being denied basic care, may be one contributing factor to the health disparities this community faces when compared to their cis-gender counterparts. Additionally, 41% of respondents had attempted suicide, 28% postponed medical care, and over a quarter of respondents had abused drugs or alcohol to cope with the experiences of stigma related to their gender identity or expression. Although limited to a smaller sample size (n=59), we encountered similar findings in a study on the social determinants of health of transgender populations in Puerto Rico.7 In this study, the main barrier to healthcare was the lack of knowledge from healthcare providers (59.6%). Study participants also identified discomfort in health encounters (55.8%) and provider discrimination (42.3%) as part of their experiences. These health disparities have generated concerns among healthcare providers and have brought to light serious gaps in healthcare provider knowledge.
Many pharmacists have become aware of their limited knowledge regarding transgender care and recognize the importance of proficiency to provide effective pharmaceutical care.8,9 A study of community pharmacist residents found that 82.7% of respondents recognized that pharmacists play an important role in the care of transgender patients, yet 71% reported they had not received education on transgender care in pharmacy school.8 By improving access to medications, linking patients to culturally sensitive healthcare providers, and serving as an educational resource, pharmacists play a key role in improving healthcare access for this population.10,11 However, for more pharmacists to actively partake in the care of transgender individuals, certain elements like education and increased cultural competency must be implemented.12
Pharmacists’ lack of knowledge may in part be due to the lack of inclusion of transgender care or LGBT issues in pharmacy school curricula.12-14 One recent commentary on the topic concluded that “pharmacists are the healthcare providers with the least training on transgender healthcare”.15 Although there are limited examples of integrating transgender care into PharmD curriculum, some positive outcomes have been reported following integration of this topic into curriculum. In a 2018 study at the New England University College of Pharmacy, a two-hour lecture on transgender health added to the therapeutics course showed an increase in knowledge and confidence in the students who attended the course compared to the ones that didn’t participate.16 In addition to didactic courses, others have suggested integrating transgender health into interprofessional courses, skills-based laboratories, elective courses, and advanced pharmacy practice experiences.17,18 Overall, however, these limited examples are demonstrative of a lack of preparation that students in pharmacy schools receive related to the care of transgender patients and the value that could be obtained by providing a continued education course to pharmacists.
When focusing on the needs of the transgender community in Puerto Rico it is important to note that currently there is no education for pharmacists regarding transgender care in Puerto Rico, and training opportunities within the greater US are limited. This hinders the wellbeing of transgender patients and may further exacerbate the disparities in healthcare which they already face. In 2017, research was conducted in Puerto Rico to assess pharmacists’ knowledge and attitudes in providing pharmaceutical care to transgender patients, and the transgender patients’ perceptions of received pharmaceutical care.9 In this study, 61% of transgender participants perceived pharmacists to be ill-informed about the transgender community and their healthcare needs. Similarly, 76% of the pharmacists were unable to correctly define the term “transgender” and only a few could correctly identify hormonal treatments for transgender males and females. The main knowledge gaps identified among pharmacists were included transgender identity, pharmacologic treatment, and routine health screening (e.g., cancer screening). Despite being concerned about the lack of knowledge displayed by pharmacists, 87.1% of transgender patients indicated they believe that pharmacists play an important role in their health.
These results lead us to believe that pharmacists in Puerto Rico have the potential to be valuable partners in the care of transgender patients and that a continuing education course might be valuable in addressing this knowledge gap. Continuing education programs may be an effective way to improve pharmacists’ knowledge and skills across a variety of practice areas.19 Continuing education programs can expand basic pharmacy education and enhance therapeutic management skills. For a program focused on transgender health, continuing education could be designed to strengthen knowledge on cultural competence, transgender medicine, drug therapies, risks and side effects associated with gender-affirming hormone therapy, surgery, and potential drug interactions.20,21
Given the knowledge deficits previously observed among pharmacists in Puerto Rico and the potential role they may play in improving care for transgender patients, we designed a three-hour continuing education course on providing pharmaceutical care for transgender patients. To evaluate the effectiveness of this continuing education course, we developed and validated an assessment to be administered before and after the educational intervention. We hypothesized that participating pharmacists will show significant improvements in knowledge of transgender care following this educational intervention.
METHODS
Design
This is a quasi-experimental, one-group pre-/post-test study designed to measure the effect of a three-hour continuing education course on the knowledge of pharmacists to provide pharmaceutical care for transgender patients. Participants were recruited from two continuing education courses: the first one held at the 2019 Convention of the College of Pharmacists of Puerto Rico (the largest professional organization of pharmacists in Puerto Rico) and the second one held as part of the Continuing Education Program of the School of Pharmacy at the Medical Sciences Campus of the University of Puerto Rico. Both educational programs were voluntary and required advanced registration by pharmacists. All study procedures for this study were approved by the University of Puerto Rico-Medical Sciences Campus’ Human Research Subjects Protection Office Institutional Review Board (Protocol #: B0250119).
Sample description
Participants were licensed pharmacists who practice in Puerto Rico. A non-probabilistic convenience sampling method was used where all participants in the continuing education sessions were invited to participate in the study. Participation in the study was voluntary and not a requirement for continuing education credit. After the two continuing education sessions were concluded with 108 pharmacists total in attendance, a total of 68 pharmacists participated in the study (participation rate of 63%), of which 64 completed the pre-test and 58 completed the post-test. A total of 54 pharmacists completed both the pre- and post-test.
Three inclusion criteria for the study were considered: (1) being a pharmacist licensed in Puerto Rico, (2) being a current member of the College of Pharmacists of Puerto Rico (a legal requirement to practice in Puerto Rico), and (3) currently practicing pharmacy in Puerto Rico. Those not meeting the aforementioned criteria were excluded from this study.
Instrument description
Data collection was made through a pre- and post-assessment test that was developed and validated by the researchers. Three domains of pharmacists’ knowledge needed to provide pharmaceutical care for transgender patients were identified: (1) foundations of gender-affirming care, (2) health disparities and the specific needs of transgender patients, and (3) hormone treatments for transgender patients. The selection of these domains was based on previous findings from research describing the knowledge and attitudes of pharmacists in Puerto Rico regarding the care of transgender patients.9 A review to verify the existence of a suitable test was performed, but researchers were not able to find an instrument that addresses the domains as intended for this study. Therefore, a novel data collection instrument was designed.
The process to develop and validate the instrument was adapted from the three phase process suggested by Boateng and colleagues.22 For each of the three domains, multiple-choice questions matching each domain were developed and an item bank was generated with a total of 47 drafted items. The item bank was then reviewed by experts in: (1) pharmaceutical care, (2) curriculum and evaluation, (3) professional continuing education, (4) clinical practice of gender-affirming care, and (5) theoretical frameworks on providing care for sexual and gender minorities. Following these expert reviews and recommendations, 14 items were modified and 5 items were dropped, yielding an instrument draft with 42 items. Afterwards cognitive interviews were conducted with a pilot group of 8 pharmacists with a similar background to the target educational audience. Their suggestions were incorporated, and a finalized assessment tool was obtained with improved clarity in syntax. This final assessment tool consisted of 42 multiple-choice items distributed across the 3 units: foundations of gender-affirming care (7 items), health disparities and the specific needs of transgender patients (14 items), and hormone treatments for transgender patients (21 items). Every item on the final assessment had a set of 5 alternatives.
Identical assessment tools were then administered to 64 pharmacists on paper before beginning and after completing the continuing education intervention Execution scores (the percent of correct answers by unit and for the complete test) were calculated to allow for better comparison between units and when comparing pre-test vs. post-test. The KR20 version of Cronbach alpha analysis was performed (Table 1) to measure the internal correlations of the items in the instrument. The value obtained for the instrument was 0.653, which suggests that the instrument had a fair internal consistency. Also, as part of the basic psychometric analysis performed, the discrimination index showed that, on most questions, the test was able to discriminate between the participants who answered an individual item correctly or not due to their knowledge, reducing the possibility of obtaining a result drawn by chance or bias. Lastly, item total correlation (ITC) was used as a measure of predictive power of each individual item when compared to the total score.23 ITC may also be useful to provide predictive validity of the total test, where a positive correlation of those who performed well on a specific item also performed well on the test, and conversely, those who performed poorly on a specific item also performed poorly on the test. About 67% of pre-test items and 71% of post-test items demonstrated an item-total correlation of 0.20 or more, indicating an acceptable predictive power.
Table 1. Pre-test instrument evaluation results
| Statistical Test | Value |
|---|---|
| Kuder-Richardson Formula 20 (KR-20) | 0.653 |
| Discrimination Index | 28 of the items had a discrimination index >0.2 |
| Item difficulty index | 0.078 to 0.938 |
| Item-Total Correlation (ITC) | 19% (8) of the items with ITC > 0.3 |
| 14% (6) of the items with ITC < 0.0 | |
| 67% (28) of the items with 0 < ITC < 0.3 |
Continued education course description
The continuing education activity was conducted by a panel of presenters and was divided into three 1-hour units: (Unit 1) Transgender Patient Care Introduction, (Unit 2) General Health Issues of Transgender Patients, and (Unit 3) Gender Affirming Hormone Therapy. A complete description of learning objectives can be found in Online appendix 1. The activity incorporated a combination of didactic presentations as well as facilitated group discussions of cases that focused on the basics of transgender care and appropriate pharmacotherapy. Unit 1 covered the topics of gender development, the prevalence of transgender individuals, appropriate terminologies, preferred pronouns, and medical record documentation. Unit 2 covered health disparities and social determinants of health affecting transgender patients and appropriate preventative screening tests. Unit 3 focused on medications used in gender-affirming care including hormone replacement therapy, the application of sex-based clinical calculations, and off-label medication use. Active learning strategies such as interactive questions with learners and facilitated case discussions were integrated throughout all three units. All participants completed a pre-assessment (pre-test) before the three-hour course. The same assessment test (post-test) was then provided at the end of the continued education course to evaluate if there was an improvement in knowledge of the participating pharmacists.
Research procedures
The pre- and post- assessment tool was administered on paper in the same room in which the continuing education session was offered. The participants were first presented with an information sheet explaining the purpose of the study, the procedures, and that participation was voluntary. After reading the information sheet, the participants were then able to complete the pre-test or opt out by not completing it. The pre-test collection sheet also included a basic demographic section that collected information such as age, sex, gender identity, geographic information, and previous training and experience related to transgender care. After participants completed the pre-test, one of the researchers collected the completed forms prior to the start of the continuing education session. Following the three-hour continuing education session, participants were instructed to complete the post-tests which were then collected by members of the research team. Although participants had access to a paper copy of the continuing education material (print out), they were instructed by the researchers to put these away while answering the post-assessment. Researchers closely monitored the participants to make sure they had no access to other material while answering the post assessment. No personal information that could link the subject to the research was collected. Pre- and post-tests were pre-printed with matching codes to allow matching of the results for the final analysis.
Data analysis
Demographic data was analyzed by standard deviation, arithmetic average, and percentages. To measure and describe the knowledge-based scores, the arithmetic mean, and standard deviation were obtained. Inferential analysis to compare changes in knowledge between the pre- and post-tests used an ANOVA, with Tukey post-hoc test. Individual comparisons were performed for scores of each unit as well as composite scores for the entire assessment.
RESULTS
Data collection was conducted in August 2019 and November 2019 during the continuing education courses previously described. A total of 68 pharmacists participated in the study. Of those 68 participants, 64 completed the pre-test and 58 completed the post-test. A total of 54 pharmacists had matched pre- and post-test data available for the comparative analysis. Demographic characteristics of the participants are summarized in Table 2. The majority of participants were cisgender, heterosexual women who had never received formal training related to transgender care. Those participants with previous education on providing care for transgender patients reported receiving it through continuing education programs, education as part of the pharmacy curriculum, conferences, or self-study.
Table 2. Sociodemographic characteristics
| Category | Participants, n=68 (100%) |
|---|---|
| Work setting as a pharmacist | |
| Community pharmacy | 29 (42.6) |
| Hospital pharmacy | 4 (5.9) |
| Pharmaceutical industry | 9 (13.2) |
| Other | 17 (25.1) |
| Unanswered | 9 (13.2) |
| Mean age (range) | 47.1 (24-69) |
| Sex, n (%) | |
| Male | 8 (11.8) |
| Female | 54 (79.4) |
| Unanswered | 6 (8.8) |
| Gender identity | |
| Masculine | 7 (10.3) |
| Feminine | 53 (77.9) |
| Transgender | 1 (1.5) |
| Queer | 1 (1.5) |
| Unanswered | 6 (8.8) |
| Sexual orientation | |
| Bisexual | 2 (2.9) |
| Heterosexual | 56 (82.4) |
| Homosexual/lesbian | 2 (2.9) |
| Unanswered | 8 (11.8) |
| Received formal training related to transgender care before | |
| Yes | 7 (10.3) |
| No | 53 (77.9) |
| Unanswered | 8 (11.8) |
| Type of training received | |
| Self-study | 3 (4.4) |
| Continuing education program | 1 (1.5) |
| Continuing education program, education as part of the pharmacy curriculum, conferences, and self-study | 2 (2.9) |
| Other | |
| Government training | 1 (1.5) |
| Medical plan training | 1 (1.5) |
| Work | 1 (1.5) |
| Unanswered | 59 (86.8) |
Pre-test results
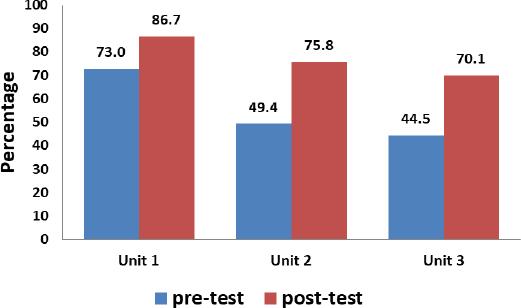
Table 3 includes the results of the execution scores of each Unit 1, 2 and 3. A complete listing of average participant scores for each item can be found in Online appendix 2. Participants had their highest scores in Unit 1, “Introduction to the Care of Transgender Patients” (mean percent execution score of 72.99%, SD=0.216; Figure 1). The item most frequently answered incorrectly in this unit assessed participants’ ability to differentiate between gender identities and sexual orientations (percentage of respondents answering correctly 56.25%, SD=0.500). Participants performed highest on the item assessing their knowledge of pharmacy services that should be offered to transgender patients (percentage of respondents answering correctly 93.75%, SD=0.243).
Table 3. Pre-test and post-test execution scores
The mean percent execution score of Unit 2, “General Health Issues of Transgender Patients”, was 49.44% (SD=0.135). In this unit, participants performed lowest on the item that assessed their ability to identify barriers transgender patients could face if they decide to have gender affirmation surgery (percentage of respondents answering correctly 7.81%, SD=0.270). On the other hand, most of the participants were able to correctly identify how some transgender patients may face barriers to accessing medically supervised hormone replacement therapy (percentage of respondents answering correctly 93.75%, SD=0.244).
“Gender Affirming Hormone Therapy” (Unit 3), had the lowest score among the participants (mean percent execution score of 44.49%, SD=0.135; Figure 1). In this unit the participants executed poorly in the item that addressed their knowledge on how hormone replacement therapy can affect the interpretation of laboratory results (percentage of respondents answering correctly 12.50%, SD=0.333). Participants performed highest on the item that assessed the need to educate a transgender man about a teratogenic medication (percentage of respondents answering correctly 85.94%, SD=0.350).
The total maximum score that a pharmacist could obtain in the test was 42. The minimum observed total score of the pre-test was 11, the maximum observed score was 31, and the mean score was 21.37 (SD=4.671) out of 42 items.
Post-test results
After the implementation of the continuing education course, the participants were re-administered the same assessment as a post-test and the results are summarized in Table 3. Again, Unit 1 had the highest performance. However, in the post-test Unit 3 had the next highest score followed by Unit 2. Nonetheless, percent execution scores improved in each of the 3 units (Figure 1).
In Unit 1, the item with the poorest performance was the same as the pre-test with 68.9% respondents answering correctly (SD=0.466). Even though the item continued to have the lowest execution score there was an improvement in the score. For the item with the highest execution score on the post-test, nearly all participants were able to correctly define the term transgender (percentage of respondents answering correctly 98.3%, SD=0.131).
In Unit 2, the item with the lowest and highest execution scores were different from the ones in the pre-test. The item with the lowest execution score tested if the participant could differ and select what transgender patient needed to be monitored for cancer given different scenarios (percentage of respondents answering correctly 15.51%, SD=0.365). Participants performed highest on the item assessing their knowledge of the screening tests that should be recommended to transgender men (percentage of respondents answering correctly 89.6%, SD=0.307).
Finally, in Unit 3 the participants scored lowest in the item assessing their ability to identify the appropriate hormone therapy for transgender woman (percentage of respondents answering correctly 18.9%, SD=0.395). The item with the highest score did not differ from the one in the pre-test, with the difference of a slight increase in the score (percentage of respondents answering correctly 86.2%, SD=0.184).
Overall, the post-test minimum observed score was 15, the maximum observed score was 40, and the mean score was 30.0 (SD=5.254) out of 42 items.
Comparison of pre- and post-test results
A total of 54 participants completed both the pre- and post-test and therefore had scores available for analysis to evaluate change in knowledge. The results are summarized in Table 4. Before analyzing the change in knowledge, a Kolmogorov-Smirnov test of normality was performed. Results from the pre-test indicated a normal data distribution (p=0.200). However, results from the post-test did not meet the cut-off for normal distribution (p=0.008). This result was heavily influenced by two very low outlier values in the post-test data set. Following the removal of the two outliers, both the pre-test and the post-test data demonstrated a normal distribution (p-values 0.200 and 0.070, respectively).
Table 4. Mean improvement in execution score after continuing education intervention (n=54)
| Unit | Average Score | Percent Improvement | |
|---|---|---|---|
| Pre-Test | Post-Test | ||
| Unit 1: Introduction to the Care of Transgender Patients | 72.49% | 85.71% | 13.22% |
| Unit 2: General Health Issues of Transgender Patients | 50.79% | 66.53% | 15.74% |
| Unit 3: Gender Affirming Hormone Therapy | 45.06% | 70.28% | 25.22% |
| Total Performance | 51.54% | 71.6% | 20.06% |
The ANOVA analysis revealed a difference in knowledge between the pre- and post-tests. The improvements in knowledge observed were significant (p<0.001) for each unit (Table 5). The average total score for the pre-test was 52.15% and for the post-test was 72.89% (mean increase in performance of 20.42%, [p<0.001]). Of note, this level of significance was maintained even when the two outliers were not excluded from the final analysis.
Table 5. Analysis of variance table for percentage by pre-post test
| Unit | SS | df | F | P-Value | ηp2 |
|---|---|---|---|---|---|
| Unit 1: Introduction to the Care of Transgender Patients | 0.47 | 1 | 12.93 | <0.001 | 0.11 |
| Unit 2: General Health Issues of Transgender Patients | 0.67 | 1 | 37.46 | <0.001 | 0.26 |
| Unit 3: Gender Affirming Hormone Therapy | 1.72 | 1 | 71.98 | <0.001 | 0.40 |
SS-Sum of squares df: degrees of freedom F: F-statistic ηp2: partial eta squared
A total of 28 (66.7%) of the items in pre-test and 30 (71.4%) items in the post-test presented a moderate or better Discrimination Index (DI) of 0.20 or more. Cronbach's alpha coefficient analysis was performed to measure the internal consistency of the items in the instrument in both instances (pre and post-test). The alpha value obtained for the pre-test was alpha=0.65 (95%CI: 0.52-0.76), and when administered as post-test was alpha=0.77 (95%CI: 0.68-0.85). Overall internal consistency improved for the instrument when administered as a post-test modality.
DISCUSSION
Pharmacists are healthcare providers that must be able to address healthcare barriers and disparities faced by minorities such as transgender people in order to provide adequate patient care. Pharmacists need to be culturally competent, aware of major barriers, and knowledgeable of the particular health issues of the transgender community when offering healthcare services. For this to happen, schools of pharmacy should consider a proactive approach in incorporating LGBT contents throughout the PharmD curriculum.14,17 However, to date most pharmacy schools do not include the provision of pharmaceutical care for transgender patients as part of their curriculum.12,15 This led us to develop this study aiming to evaluate the effect of a three-hour continuing education course on the knowledge needed by practicing pharmacists to provide pharmaceutical care for transgender patients.
For each of the 3 units assessed, an improvement was observed between the pre- and post-test measurements. The statistically significant increase in performance after completing the educational intervention suggests that the participants who attended the continuing education course gained knowledge in areas such as cultural competence, gender-affirming therapy, relevant drug interactions, and risks and side effects associated with hormone replacement therapies and adjunctive therapies. It is important to note that the administration of a comprehensive pre-test may have had a positive effect on post-test performance. In fact, a pre-testing effect before being exposed to learning content has demonstrated enhancement of content retention.24
Although to our knowledge this is the first formal evaluation of a transgender health continuing education for pharmacists, the results are consistent with previous research which found continuing education resulted in increased knowledge and comfort in pharmacists regarding patient care in HIV positive patients.25 The previously mentioned 2018 study of the integration of transgender care into a pharmacy therapeutics curriculum demonstrated similar improvments in student knowledge.16 The results from the current study demonstrate that by allowing practicing pharmacists to obtain training to provide appropriate pharmaceutical care to transgender people, a continuing education course may be one tool to address this area in which many pharmacists did not receive prior training .
When comparing the Cronbach's alpha coefficient (α) of the test, results showed an improvement in α with repeated administrations. This improvement is not unexpected, given previous work that has identified a similar pattern of α improvement when administering the same instrument to the same (or nearly the same) respondents.26-28 These findings contribute to the instrument validity and our confidence in the findings, as having an instrument with at least moderate internal consistency and adequate discrimination indices allows for more reliable measurements and results. We consider these psychometric properties to be a strength of the study.
It should be noted that before taking the continuing education course, pharmacists performed most poorly in the unit related to hormone treatment for gender affirmation. These findings were consistent with previous findings which suggested that pharmacists have gaps in knowledge regarding hormone replacement treatment for gender affirmation.8,9 The pharmacists that completed the continuing education course demonstrated the largest increase in execution in the unit related to hormone treatment for gender affirmation. This positive change in knowledge will hopefully translate into increased opportunities for pharmacists to positively contribute toward the individualized pharmacotherapy needs of the gender affirmation process. Future research investigating the impact of additional training on patient outcomes would help confirm a positive impact on clinical care.
Some limitations should be noted when interpreting the findings of this study. First, the number of participants in the study was limited to the number of pharmacists who voluntarily chose to attend each continuing education course, potentially leading to a selection-bias. Moreover, the intervention was limited to a single didactic lecture and the post-test was given shortly after the end of the course, which is primarily a measure of short-term memory retention. However, previous research has demonstrated that short-term knowledge gains are associated with long-term retention, although not necessarily reflective of the magnitude of long-term knowledge gained.29-32 Nonetheless, to better understand the effect of the continuing education course over time, future assessments to examine the long term impact of a continuing education course on pharmacists’ knowledge in providing pharmaceutical care to transgender patients are recommended. Additionally, assessments of how improvements in knowledge are associated with increased pharmacist confidence as well as practical skills and abilities are warranted.
CONCLUSIONS
Pharmacists that attended the three-hour continuing education course demonstrated improvements in knowledge related to the care of transgender patients. The results of the pre- and post-tests showed a mean increase in performance of 20.42% (p<0.001), with improvements observed in each of the three units assessed. The instrument developed and used to assess pharmacists’ knowledge to provide pharmaceutical care for transgender patients may be useful as an assessment for other short-term continuing education interventions. Further instrument examination and use may be conducted to determine its usefulness when measuring gains in knowledge over the long term. Ultimately, until the inclusion of transgender healthcare in the curricula of schools of pharmacy and residencies is universally adopted, continuing education interventions as described here will be essential in enhancing pharmacists’ knowledge to provide appropriate pharmaceutical interventions for transgender patients.