Mi SciELO
Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Citado por Google
Citado por Google -
 Similares en
SciELO
Similares en
SciELO -
 Similares en Google
Similares en Google
Compartir
Revista de Osteoporosis y Metabolismo Mineral
versión On-line ISSN 2173-2345versión impresa ISSN 1889-836X
Rev Osteoporos Metab Miner vol.6 no.1 Madrid ene./mar. 2014
https://dx.doi.org/10.4321/S1889-836X2014000100006
Migratory arthralgia and sclerosing bone lesions. Differential diagnosis
Artralgias migratorias y lesiones óseas esclerosantes. Diagnóstico diferencial
Pedraz Penalva M.T.
Sección de Reumatología - Hospital del Vinalopó - Elche (Alicante)
SUMMARY
Osteopokilosis is a rare benign bone dysplasia that may result in musculoskeletal pain, although it is usually asymptomatic. It is frequently suspected and diagnosed by the incidental finding of characteristic bone lesions on plain radiographs requested for another reason. Identifying these lesions and ruling out other possible causes is crucial to carry out a correct differential diagnosis and to avoid unnecessary invasive studies. We describe a case of a patient 32 years old who was referred to our rheumatology department because of joint pain.
Key words: sclerosing bone disorders, sclerosing bone dysplasias, osteopoikilosis, osteosclerosis, sclerotic bone metastases, radiography, diagnosis.
RESUMEN
La osteopoiquilia es una rara displasia ósea benigna que puede cursar con dolor musculo-esquelético, aunque suele ser asintomática. Habitualmente se sospecha y se diagnostica ante el hallazgo incidental de las lesiones óseas características en los estudios radiológicos solicitados por otro motivo. Identificar estas lesiones y descartar otras posibles causas es crucial para realizar un correcto diagnóstico diferencial y evitar estudios invasivos innecesarios. A continuación describimos un caso clínico de una paciente de 32 años remitida al servicio de Reumatología por dolor articular.
Palabras clave: enfermedades esclerosantes óseas, displasias esclerosantes óseas, osteopoiquilosis, osteosclerosis, metástasis óseas escleróticas, radiografía, diagnóstico.
Introduction
Osteopoikilia or disseminated condensing osteopathy is a benign bone dysplasia related to an anomaly in the endochondral maturation process. Clinically, it is usually asymptomatic, although the patients may present with joint pain, skin alterations, various developmental anomalies or other associated pathologies. The bone metabolism-related laboratory parameters are usually normal, and the diagnosis is usually made as a result of the incidental discovery in radiological studies of characteristic bone lesions. The radiological images typically show multiple radiodense bone lesions, of small size, rounded or oval, distributed in the periarticular regions of the long bones1. Understanding and indentifying the radiological patterns which characterise the different bone pathologies is, along with the clinical history, fundamental to carrying out a precise diagnosis.
Below, we describe a clinical case of a patient admitted due to articular pain.
Clinical case
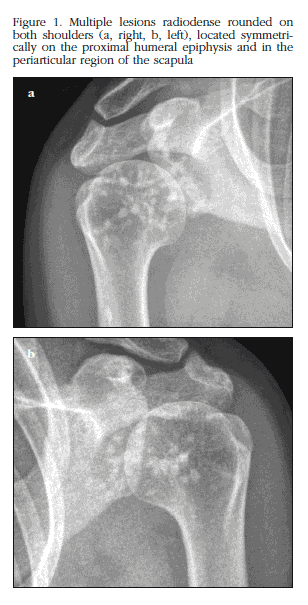
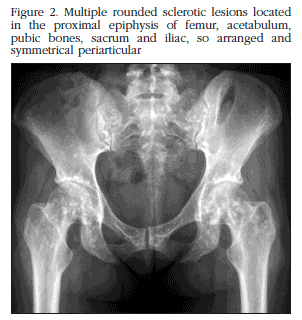
A woman of 32 years of age was admitted for a rheumatology assessment in relation to migratory arthralgia worsening after exertion during the last two years. The articular pain disappeared with non-steroidal anti-inflammatories. The patient did not suffer from any systemic disease or take any pharmacological treatments. In the physical examination slight pain was reported with the passive abduction of both shoulders, and pain on palpation of both pertrochanteric regions and the right wrist. No tumefaction was found, or limited movement in any joints. No cutaneous lesions or other anomalies were found. The laboratory studies carried out (haemogram, transaminase biochemistry, renal function, alkaline phosphatase, calcium, phosphorous, thyroid hormones and parathyroid hormone, electrolytes, proteinogram, VSG, C-reactive protein (CRP), 25(OH) vitamin D, markers for bone resorption, calciuria in urine at 24 hours, antinuclear antibodies (ANA), rheumatoid factor (RF), anti-cyclic citrullinated peptide antibodies (anti-CCP), and hepatitis B and C serology) were normal. In the X-rays there was evidence of multiple small, rounded, sclerotic bone lesions, distributed symmetrically bilaterally, and located in the head of the humerus, the periarticular section of the scapula (Figure 1), metacarpals and phalanges of the hands, pelvis, acetabulum, femoral head and condyle (Figure 2), proximal and distal thirds of the tibia and in the bones of the foot.. No affectation in the cranium or vertebral bodies was observed. The bone gammagraphy with technetium showed no pathological radiotracer deposits. The patient was diagnosed with osteopoikilosis on the basis of the clinical findings, the normality of the laboratory parameters and the characteristic X-ray images.
Discussion
Osteopoikilia or osteopoikilosis is a hereditary bone dysplasia of unknown etiology, related to an alteration in the resorption of the secondary spongy bone tissue and in the normal formation of trabeculae along the tension lines during the process of endochondral maturation2. A pattern of dominant autosomal inheritance has been identified, although sporadic cases have also been report. There is a similar incidence in both sexes, with an estimated prevalence of 1/50,000 inhabitants3. The patients frequently remain asymptomatic, which means that the diagnosis can occur at any age, on the incidental discovery of the typical radiological lesions in X-ray studies requested for other reasons. These bone lesions appear during embryonic development and in infancy, and usually remain throughout the patient's life, although both increases and decreases in their size, and even their disappearance, have been reported4. However, not infrequently patients have manifestations of the condition such as pain or joint leakage (15-20% of cases), or cutaneous lesions (25%). Connective tissue nevi are the most common cutaneous lesions, followed by the tendency to develop keloids and sclerodermiform lesions5. The coexistence of dermatofibrosis lenticularis disseminata, a hereditary connective tissue disorder characterised by the appearance of fibromatose papules (nevi) on the back and the extremities, and osteopoikilia, called osteodermatopoikilosis or Buschke-Ollendorff syndrome6. Patients with osteopoikilosis may also have stenosis of the medullar canal, anomalies of the craneo-cervical hinge (Klippel-Feil syndrome), craneo-facial and dental alterations, syndactyly, growth anomalies (dwarfism), renal or cardiac malformations, urogenital defects, endocrine pathologies (early pubescence) and autoimmune rheumatological conditions, aortic coarctation and other vascular problems7. The articular clinical condition may be related to the osteopoikilia itself or to associated autoimmune diseases such as systemic erythematosus lupus, rheumatoid arthritis, spondyloarthropathies or familial Mediterranean fever. Although our patient reported joint pain which worsened in various locations with activity, there were no signs which suggested the coexistence of an associated systemic pathology, either in the physical examination or in the complementary studies carried out. Neither were cutaneous alterations or other anomalies detected. The X-ray images characteristic of osteopoikilosis show multiple small osteosclerotic lesions, which may vary from being millimetres to centimetres in size, of homogeneous density and morphologically, generally rounded or oval. These lesions have a typical periarticular distribution, usually located in the metaphysis and epiphysis of the long bones. In up to 90% of cases they appear in symmetrical bilateral form. The small bones of the hands and feet (phalanges, metacarpals, metatarsals, the carpal and tarsal bones), the pelvis, the femur, the cubit, the radius, the sacrum, the tibia, the fibula, the scapula and the proximal section of the humerus are the bones most commonly affected2,8. The X-ray images from our patient showed the typical rounded radiodense lesions distributed periarticulately and located in the humeral and femoral heads, the scapula, the pelvis, the femoral condyles (Figures 1 and 2), the proximal and distal thirds of both tibias and bones of the hands and feet. The location of these lesions in the cranium, ribs or the vertebral bodies is not normal, except in osteomesopycnosis, a variant of osteopoikilosis characterised by the presence of irregular sclerotic lesions located in the vertebral bodies, close to the edge of the vertebral end plates2. There seems to be a close relationship between the alterations underlying the different bone dysplasias, which makes it impossible to differentiate them histologically on some occasions. Furthermore, those patients with osteopoikilia frequently display other dysplasias such as enostosis, osteomas, striated osteopathy, melorheostosis or multiple exostosis9. The histological study of lesions in patients with osteopoikilosis shows, as with enostosis, condensations of compact lamellar bone (sclerotic areas) located in the spongy bone, consistent with the radiological findings4,10. The coexistence of alterations which suggest the presence of osteopoikilosis, striated osteopathy and melorheostosis in the same patient is known as mixed sclerosing bone dystrophy2. As with other bone dysplasias, those patients with osteopoikilia have an increased risk of pathological fractures, although there is no evidence or any anomaly in the process of bone scarring following fractures1.
Occasionally, the neoplastic degeneration of some of the osteosclerotic lesions has been reported, especially in the direction of chondrosarcoma and osteosarcoma. A bone gammagraphy with 99m technetium-MDP is usually normal in patients with osteopoikilosis, and carrying it out may help to differentiate it from other processes such as blastic metastasis or to identify a malignant transformation of the lesions4,11. However, the presence of an anomalous focus of radiotracer captation does not exclude this dysplasia, since some large lesions during growth, especially in young patients, may show this alteration12,13. In our case, no hypercaptation of the radiotracer was observed in any location.
The diagnosis of this bone dysplasia is usually made from the typical osteosclerotic lesions in the X-ray images. Other complementary studies are not usually required and the need for a bone biopsy is exceptional, a tool limited to those cases in which there is diagnostic doubt or suspicion of neoplastic degeneration. Numerous pathologies of different degrees of severity and prognosis have been linked to the presence of sclerosing bone lesions. Blastic metastases are the most common cause of multiple radiodense bone lesions in adults, notable both for their incidence and their seriousness. Breast neoplasia in women and prostate carcinoma in men are the tumours most commonly associated with them. Bone metastases are generally asymmetrical, variable in size, and have a predilection for the axial skeleton, the ribs and the diaphysis of the long bones. On rare occasions they appear in the carpal or tarsal bones. Radiologically, they are characterised by the presence of bone destruction and periostic reaction, as well as by the finding of numerous captation foci in bone gammagraphy14. On the other hand, various congenital and/or hereditary pathologies have been associated with the appearance of osteosclerotic lesions throughout a patient's period of growth, notable of which are the heterogeneous group of bone dysplasias and, among these, osteopetrosis, striated osteopathy, melorheostosis, pycnodysostosis, dysosteosclerosis, multiple osteochondromatosis, enostosis, osteomas, and fibrous bone dysplasia4,9,10. Other diseases such as neurofibromatosis type 115, tuberous sclerosis16 or pachydermoperiostosis17 have also been associated with these bone anomalies, as well as various acquired pathologies, notable among which are myelofibrosis10, VHC infection18, lipid granulomatosis9, mastocytosis19, sarcoidosis8, Paget disease20 and renal osteodystrophy9. Frequently, the morphology of the lesions, their position in the skeleton, and their location in the bone (epiphysary, metaphysary or diaphysary, the affectation of the cortical or spongy bone, or compromise of trabecular pattern) offer characteristic radiological patterns which, combined with the clinical history, are usually sufficient to make a correct differential diagnosis and to establish a precise diagnosis.
In conclusion, we consider that the evaluation of patients with joint pain associated with multiple osteosclerotic radiological lesions should be carried out exhaustively, taking in to account the possible pathologies involved and discounting the related diseases which may be coexistent. Understanding the different radiological patterns is essential in order to make a correct differential diagnosis, and to avoid diagnostic errors or the unnecessary use of invasive tests. Blastic metastases are a challenge for which the performance of a bone gammagraphy with 99m Technetium-MPD may help resolve7.
Finally, a regular assessment of patients with osteopoikilosis is recommended due to the risk of malignant transformation described.
![]() Correspondence:
Correspondence:
Ma Teresa Pedraz Penalva
Sección de Reumatología
Hospital del Vinalopó
Tónico Sansano Mora, 14
03293 Elche
Alicante (España)
Correo electrónico: tpedraz2000@yahoo.es
Date of receipt: 10/03/2014
Date of acceptance: 15/04/2014
Bibliography
1. Woyciechowsky TG, Monticielo MR, Keiserman B, Monticielo OA. Osteopoikilosis: what does the rheumatologist must know about it? Clin Rheumatol 2012;31:745-8. [ Links ]
2. Greenspan A. Sclerosing bone dysplasias--a target-site approach. Skeletal Radiol 1991;20:561-83. [ Links ]
3. Benli IT, Akalin S, Boysan E, Mumcu EF, Kis M, Türkoglu D. Epidemiological, clinical and radiological aspects of osteopoikilosis. J Bone Joint Surg Br 1992;74:504-6. [ Links ]
4. De Vernejoul MC, Kornak U. Heritable sclerosing bone disorders: presentation and new molecular mechanisms. Ann N Y Acad Sci 2010;1192:269-77. [ Links ]
5. Benli IT, Akalin S, Boysan E, Mumcu EF, Kis M, Türkoglu D. Epidemiological, clinical and radiological aspects of osteopoikilosis. J Bone Joint Surg Br 1992;74:504-6. [ Links ]
6. De Vernejoul MC. Sclerosing bone disorders. Best Pract Res Clin Rheumatol 2008;22:71-83. [ Links ]
7. Ozdemirel AE, Cakit BD, Erdem HR, Koc B. A rare benign disorder mimicking metastasis on radiographic examination: a case report of osteopoikilosis. Rheumatol Int 2011;31:1113-6. [ Links ]
8. Di Primio G. Benign spotted bones: a diagnostic dilemma. CMAJ 2011;183:456-9. [ Links ]
9. Ihde LL, Forrester DM, Gottsegen CJ, Masih S, Patel DB, Vachon LA, et al. Sclerosing bone dysplasias: review and differentiation from other causes of osteosclerosis. Radiographics 2011;31:1865-82. [ Links ]
10. Van Hul W, Vanhoenacker F, Balemans W, Janssens K, De Schepper AM. Molecular and radiological diagnosis of sclerosing bone dysplasias. Eur J Radiol 2001;40:198-207. [ Links ]
11. Tuncel M, Caner B. Osteopoikilosis: a major diagnostic problem solved by bone scintigraphy. Rev Esp Med Nucl Imagen Mol 2012;31:93-6. [ Links ]
12. Mungovan JA, Tung GA, Lambiase RE, Noto RB, Davis RP. Tc-99m MDP uptake in osteopoikilosis. Clin Nucl Med 1994;19:6-8. [ Links ]
13. An YS, Yoon JK, Lee MH, Joh CW, Yoon SN. Abnormal bone scan in an adult with osteopoikilosis. Clin Nucl Med 2004;29:856-8. [ Links ]
14. Choi J, Raghavan M. Diagnostic imaging and image-guided therapy of skeletal metastases. Cancer Control 2012;19:102-12. [ Links ]
15. Lu-Emerson C, Plotkin SR. The Neurofibromatoses. Part 1: NF1. Rev Neurol Dis 2009;6:E47-53. [ Links ]
16. Avila NA, Dwyer AJ, Rabel A, Darling T, Hong CH, Moss J. CT of sclerotic bone lesions: imaging features differentiating tuberous sclerosis complex with lymphangioleiomyomatosis from sporadic lymphangioleiomymatosis. Radiology 2010;254:851-7. [ Links ]
17. Hansen-Flaschen J, Nordberg J Clubbing and hypertrophic osteoarthropathy. Clin Chest Med 1987;8:287-98. [ Links ]
18. Lormeau C, Falgarone G, Roulot D, Boissier MC. Rheumatologic manifestations of chronic hepatitis C infection. Joint Bone Spine 2006;73:633-8. [ Links ]
19. Spivacow F, Sarli M, Nakutny R. Mastocitosis sistémica: repercusión ósea. Medicina (Buenos Aires) 2012;72: 201-6. [ Links ]
20. Smith SE, Murphey MD, Motamedi K, Mulligan ME, Resnik CS, Gannon FH. Radiologic spectrum of Paget disease of bone and its complications with pathologic correlation. Radiographics 2002;22:1191-216. [ Links ]











 texto en
texto en