INTRODUCTION
Metabolic syndrome (MS) is a recent concept in medicine due to it was thirty years ago when it started to group the different MS components as a common pathology. In 1999, the World Health Organizations defined MS as the accumulation of hypertension, glucose intolerance, obesity and dyslipemia1 since then several diagnostic standards have been introduced. One of the most accepted is the definition of the National Cholesterol Education Program Adult Treatment Panel III (NEPATP III)2. This criterion describes MS as the presence of at least three risk factors. Risk factors are obesity (high waist circumference), triglyceride concentration (>150mg/dL or drug treatment), low HDL cholesterol (<40mg/dL in men and <50mg/dL in women), high blood pressure (>130mmHg systolic or >85mmHg diastolic) and fasting blood glucose (>100mg/dL or drug for DM). Similar definitions have been reported by the Japan Society for the Study of Obesity (JASSO) and the International Diabetes Federation (IDF), whereas in these models waist circumference is a required factor. Later, the American Heart Association (AHA), the National Heart, Lung and Blood Institute (NHLBI) and the IDF reported a new definition considering at least three risk factors where waist circumference was not a required factor. The main objective of this review was going further into different aspects of MS in order to shed some light on this syndrome. PubMed and Medline databases were searched to identify eligible studies.
EPIDEMIOLOGY OF METABOLIC SYNDROME
It has been reported that MS is already presented in almost all developed and undeveloped countries. Consequently it has become in a global health issue, preventive health procedures should be carried out. Young people affected by MS incidence will lead to an adult population with an increased risk for chronic diseases. Consequently, it would be really necessary to establish preventive strategies in young population in order to reduce possibilities to suffer MS.
Generally, it is thought that MS is highly common in western countries, even it was estimated that more than 70% of adult population has at least one clinical sing of MS3. In 2009 a study mentioned that in US the prevalence of MS was 24% while in Europe was between 24.6-30.9%4. Another study5 determined MS prevalence in participants from the US, examining different variables of MS. They discovered that 38% showed MS and from them more than half presented severe MS. It is also the case that MS prevalence has been determined in US working subjects6, observing a high occurrence and MS subjects affected showed more health risks. Exactly, the prevalence of MS in Spain is 31% with little changes in function of gender7. The authors examined 24,670 subjects from 10 areas to represent Spanish mature population. Furthermore, the prevalence of metabolic premorbid syndrome was 24% and this condition also increases coronary risk. Vosátková et al.8 determined the MS prevalence in population from the Czech Republic. They reported a mean value of 29.9% for women and 32.5% for men.
Traditionally, countries with an oriental culture have been characterized by low prevalence of obesity, MS and chronic pathologies. However, one research9 investigated MS prevalence in Korean population; MS was 14.3% for parents and 7.2% for offspring. Song et al.10 studied the MS prevalence in 15,477 individuals from another oriental country, China. They detected a prevalence of 27.4%. It seems that one consequence of globalization may be the loss of protection of these areas against MS and chronic pathologies. Another research11 analyzed the MS incidence in Nigerian hypertensive patients. They observed a prevalence of 40.74% and the most common MS element was abdominal obesity. MS prevalence has been also analyzed in South America. A recent study12 studied MS affliction in Brazilian adult population. Obtaining that one in three subjects studied was diagnosed with MS. Additionally, more than half adult population from Chile has been classified with MS13. In Colombian population MS incidence has been also determined; obtaining that one third of participants studied suffered MS14.
A crucial point in MS management is the prevalence in young population because MS rate has been increased among them in last times. A recent paper15 examined MS incidence in teenagers from Iran. They obtained that 6% of adolescents presented MS and sex variations were found (9.3% in man and 2.4% in woman). Furthermore, MS factors were very common, 42.4% have low HDL, hypertensive profile 16.3%, increased triglycerides concentration 15.6%, and high waist circumference 8.6%, etc. Rerksuppaphol et al.16 analyzed MS prevalence in obese children from Thailand. Half of them suffered MS and had high abdominal obesity, blood pressure, fasting glucose levels, triglycerides concentration and skinfolds thickness. The authors concluded that it would be necessary to treat and prevent MS in Thai children.
ETIOLOGY AND DEVELOPMENT OF METABOLIC SYNDROME
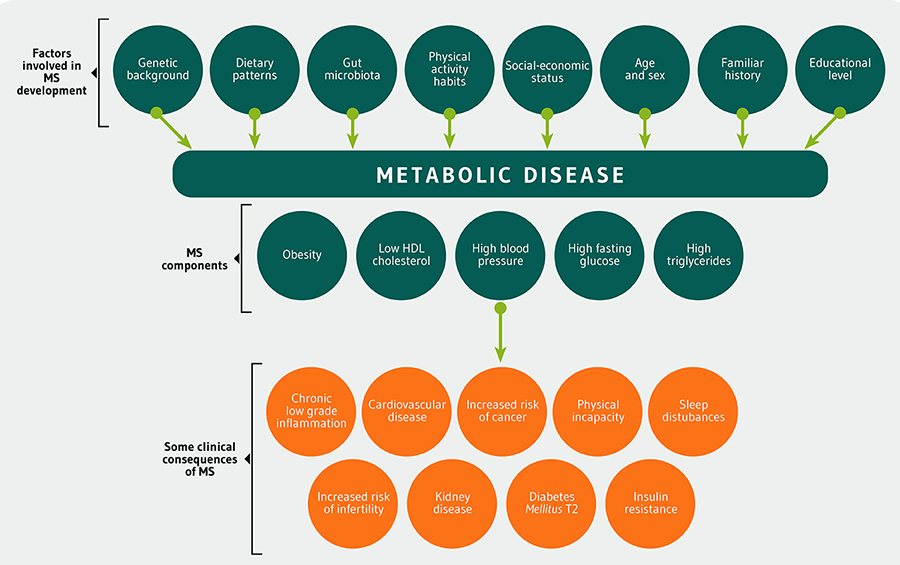
A huge cluster of factors may be involved in MS incidence: relatives, social-economic status, educational levels, genetic background, age, sex, hyperpalatable processed food environment, gut microbiota, dietary patterns and physical activity habits. These factors affects differently to each MS patient.
It is really difficult define exactly which one would be the cause of MS. Interestingly, a review3 suggested that several points could take part in MS prevalence such as age, genetic background, dietary patterns, physical activity habits and sex structure. As it could be thought environmental components could play an important role in MS development as can be seen in Figure 1. One study9 examined the effect of familial concordance in MS affliction. They observed that husbands whose wives presented MS exhibited 1.43 higher risk of suffering MS; wives whose husbands showed MS had 1.41 more chances of MS. Interestingly, children with at least one parent who experienced MS had 2.56 higher risks of MS, when both parents suffer MS, their children exhibited 3.31 higher possibilities of MS. Subsequently, MS affliction could increase risk of this condition in relatives. Even, it has been proposed that belong to a specific ethnic group could affect to MS occurrence17.
Other essential factors in MS development would be age and sex, one previous study18 examined age and sex importance in the clustering of MS factors. They analyzed men and women from US. MS prevalence was 26% in young and 55% in older population. In young male participant’s high triglycerides, low HDL cholesterol and elevated blood pressure were the most common factors while in young women were triglycerides, low HDL cholesterol and high waist circumference. However, in old population, the most prevalent combination was waist circumference, triglycerides, high blood pressure, low HDL cholesterol and impaired glucose tolerance. Sheu et al.19 reported that specific MS elements could be used independently to predict MS affliction and these factors differ in function of sex. It seems likely that MS prevalence and expression could differ in function of age and sex. Bahrani and contributors15 reported that MS is significantly more widespread in obese population. They viewed positive correlation between MS in adolescent and parental education grade, domestic monthly earnings and school position. Even, a relation between a previous familiar obesity history and MS development was detected. Several investigations have proposed that genetic background could influence MS origin. Particularly, Alnory et al.20 studied the influence of specific polymorphisms in leptin and vaspin blood levels and the risk of suffering MS. A genotype of leptin polymorphisms was associated with metabolic risk development and high leptin concentration. Another study21 found that specific variations in FTO, SCG3 and MTMR9 genes could increase risk of MS. More recently, Zhao et al.22 refuted associations between genetic variations and MS. Even, it has been shown that MS elements could be connected with gut microbiota23. Changes in microbiota could improve MS. Philco et al.17 reported that depression could be considered a MS risk factor.
Environmental factors play a crucial role in MS genesis. One research8 reported correlations between MS and consume of margarine, butter, fatty dairy products, low-fat dairy products, amount of daily meals and weight changes in the last ten years. For this reason, it would be necessary to address life style factors in the management of MS. Hunter et al.24 studied the effect of a high fat high sucrose diet (HFHSD), characteristic western diet. They obtained that the HFHSD increased oxidative stress and affected to cardiovascular function and remove female protection again cardiovascular dysfunction. Another research25 studied possible associations between soda ingestions and MS and diabetes mellitus type 2 (DMT2). They observed that daily soda consumption was connected to a 36% and 67% risk increased of MS and DMT2 occurrence in contrast with non-intake. A study26 explored a possible association between MS affliction with nutritional habits in teenagers from USA. Better nutritional habits were connected with less MS prevalence. One interesting research27 analyzed food advertising on television, the authors found that 54.9% of advertising examined were about unbalanced energy profile food or high in energy. Even, the ratio between unbalanced energy profile or high energy food advertising and nutrient dense, low energy advertising was lower than a previous analysis six years before and this ratio was increased on thematic channels for children. Therefore, an exposure to unhealthy food would contribute to an unhealthy environment that might increase MS incidence. Furthermore, higher physical activity levels were related with lower MS prevalence. A lower fitness level has been associated to an increased risk of metabolic syndrome in children28. In addition, a lower level of physical exercise has been related with higher possibilities of occurrence of hypercholesterolemia, DMT2 and MS29. Additionally, it has been described a correlation between body composition measures, HDL-cholesterol and MS with insulin resistance in obese adolescents30. Subsequently, it would be recommended to evaluate insulin resistance in MS progression. Furthermore, MS has been associated with abdominal visceral fat distribution and higher levels of inflammation, quantified by interleukin-6, tumor necrosis factor- α and plasminogen activator inhibitor-1 in old obese subjects31.
EFFECTS OF METABOLIC SYNDROME ON HEALTH
MS increase comorbidities of other chronic pathologies such as DM, insulin resistance or some kinds of cancer, besides MS may amplify chance of cardiovascular diseases and sleep disturbances occurrence. MS suffering affects to quality of life because it increases physical incapability that could impact on daily activities of patients, consequently, MS could affect to health and quality of life of patients.
A MS status maintained for long time has unquestionably effects on health increasing comorbidities as can be observed in Figure 1. MS affliction could be associated with higher risk of colon or rectal cancer as consequence of abdominal obesity and insulin resistance4. Particularly, the authors focus on this relation in high levels of leptin, low adiponectin, elevated C-peptide, high body mass index, elevated insulin growth factor-1, low insulin growth factor binding protein-3 and hyperinsulinemia status. In addition, Harding et al.32 found that patients with five components of MS exhibited 1.12 and 2.07 increased risk for overall and colorectal cancer. Bjørge et al.33 analyzed women from Austria, Norway and Sweden to examine a possible connection between breast cancer and MS. They discovered that MS increased 1.23 risk of breast cancer mortality. Another study34 examined the MS prevalence in breast cancer patients. MS prevalence in breast cancer subjects was 59.2%, higher than in controls. More importantly, they found a positive and independent association between MS and breast cancer incidence (2.49). Another review35 determined that several factors characteristic of MS such as visceral adiposity, hyperglycemia, hyperinsulinemia, IGF-I, estrogen signaling and inflammation could be also implicated in carcinogenesis and tumor evolution. The authors proposed that it would be essential to discern the possible connections between these factors and cancer risk, certainly methodological studies would be really necessary to comprehend the role of these determinants. Cowey and Hardy36 presented that elements from MS such as insulin resistance, adipokine formation or oxidative stress could collectively raise cancer risk.
Guo et al.37 thought that it would be possible that MS could be related with a common gastrointestinal disorder, irritable bowel syndrome. They reported that irritable bowel syndrome was highly present in MS patients. It is also true that MS has been connected with the origin of chronic kidney disease38. The authors found that MS condition was involved in development of chronic disease dysfunction in Japanese population (ratio 2.12) and this risk was increased with more MS components accumulated. Furthermore, another study39 determined the repercussion of MS on long course kidney role and stone return rates after percutaneous nephrolithotomy. Authors obtained that MS profile was related with higher recurrence rates and worse renal function at long time after the operation. Moreover, it has been described that MS is connected with physical incapacity5. Another condition which has been related to MS is the sick euthyroid syndrome in adult population40. Another previous study41 mentioned that hyper-insulinemia, a highly factor present in MS, has been connected all aspects of polycystic ovary syndrome, a cause of infertility in women. Generally, it has been related MS with higher risk of cardiovascular disease. More significantly, MS could increase the chance to suffer atrial fibrillation, an usual arrhythmia42. Factors involved would be oxidative stress, high blood pressure, low grade of inflammation, left atrial and ventricular remodeling and activation of renin-angitensin-aldosterone system. Another study7 declared that men and women who have MS present 2 and 2.5 higher coronary risk, even coronary risk was increased in people with metabolic premorbid syndrome, 1.5 and 2 for men and women. Additionally, Rejeb et al.43 determined the relationship between MS and coronary stenosis in Tunisian participants. Coronary stenosis risk was 3.38 higher in MS, this risk was increased with the number MS components and the highest was with five metabolic factors (4.48). Another research44 commented that people with MS presents a 1.5 to 3 increase in the risk of suffering stroke and coronary heart disease.
Recently, it has been suggested45 that people affected with mental disorders have more possibilities to suffer MS. The authors concluded that it was really common to be affected by MS in bipolar disorder patients. Moreover, it has been examined46 a possible relation between MS and the cognition level in elderly population using the Mini-mental State Examination (MMSE). Individuals with MS have lower MMSE scores and the numbers of MS factors could be an independent predictor of lower MMSE scores. Additionally, biochemical modifications at cellular level produced in MS such as changes in endothelial cell activities, variations on fatty acid metabolism or irregular insulin and leptin metabolism could be related with neurological disorders as depression, Alzheimer´s disease and stroke47. Sasanabe et al.48 examined a possible relation between MS and sleep apnea. Men and women with obstructive sleep apnea syndrome exhibited a higher risk of MS. Even, psoriasis has been connected to metabolic syndrome, cytokines and adipocytokines could be in part responsible of this relation49. A previous study6 has observed that MS employees higher health-care and pharmaceutical cost and short-term disability. Even, MS subjects showed more productivity losses. MS suffering could do a worker less efficient and it would affect to company productivity. Another study50 reported that MS components, hyperglycemia and dyslipemia, could be connected with insulin resistance aggravation.
NUTRITIONAL TREATMENTS PROPOSED
Apart from dietary patterns, there are other elements in MS management such as exercise, drugs, surgery or psychological support. Nevertheless, based on the studies reviewed in the current paper, it seems that nutritional treatments play an essential role in MS recuperation. More importantly, nutritional therapy should teach to MS patients to have healthy dietary patterns in order to prevent future regressions. Between the different nutritional treatments reviewed, it is clear that fruits, vegetables, fish, nuts, legumes and whole grain cereals intake are directly connected with MS improvements and remissions. However, simply sugar, highly present in ultra-processed food, is associated to MS suffering. In terms of nutrients enough protein and monounsaturated fats consume should be provided by diet to improve MS status.
Panagiotakos et al.3 proposed that people who suffer MS would improve their health through diet, exercise and lifestyle changes. De Flines et al.44 mention that it would be necessary to pay attention to diet, physical activity, obesity, components of MS and insulin resistance in MS management. They suggested that lifestyle changes are an adequate method to lead MS components and only in the case that this intervention would be not enough, a pharmacological mediation should be contemplated. In general, it is thought that dietary patterns could play an important role in MS remission. A previous research51 explored the effect of a dietary intervention in order to study salt sensitivity on blood pressure. A decrease in sodium intake could be used to modulate blood pressure in MS due to a significant reduction in arterial blood pressure was detected with a low sodium ingestion. Supplementary, another study52 examined salt sensitivity in MS; blood pressure reacted to salt ingestions in an increased way in MS. Interestingly, a reduction in salt ingestions achieved systolic blood pressure decrease in patients with three or more MS components. A recent review53 analyzed the evidence of nutritional therapies in MS. They determined that a low calorie diet connected with exercise intervention showed the higher efficiency; nonetheless they highlighted the importance of life changes in the MS remission.
Anderssen et al.54 evaluated diverse methods of intervention in one year of intervention in male with MS. Exercise and diet reduce MS prevalence to 32.6%, isolated diet to 64.7% and exercise alone to 76.5%. Diet intervention consisted on individualized nutritional counseling and including energy restriction; fish consume and decreased saturate fats and cholesterol intake. Physical activity based on endurance exercise and composed of 60 minutes of aerobics, circuit training and fast walking at the 60-80 peak heart. Another study55 mentioned that high fruits, vegetables and minimal processed cereals intakes are related to a reduced risk of MS while high meat ingestion, highly processed cereals and fried food were related with MS. The authors highlighted the magnitude of diet quality in MS apparition and evolution. Another review56 proposed that vegetarian and vegan diets could improve MS and these dietary patterns are characterized by low energy intake, saturated fat and processed fat whereas high fruits, vegetables and fiber ingestions. Esposito and Giugliano57 suggested that higher adherence to Mediterranean diet showed less occurrence of MS. This dietary pattern, characterized by lower carbohydrate intake and high monounsaturated fats intake could contribute to improve MS, particularly blood lipids, insulin resistance and liver perform. Another research58 detected a relation between nuts, legumes and seeds consume and a lower risk MS suffering.
Another previous study59 examined the protein content in obese participants for 12 months. They were assigned to a high protein diet (1.34g per kg of BM) or to a standard protein diet (0.8g per kg of BM) and a calorie restriction of 500kcal per day. Obtaining that high protein group reported a higher body weight loss and fat mass loss compared with another group, furthermore biochemical parameter were better with the high protein regimen. Besides, 64.5% participants of the high protein diet did not fulfill three or more components of MS at the end. As a result protein enriched diet could be an instrument in the control of MS. Klemsdal et al.60 examined a low glycemic load (LGL) diet in contrast with a low fat diet in participants with different grades. After the first three months of intervention, subjects assigned to LGL presented higher weight loss and one year after, blood pressure decreased more in LGL diet. They concluded that LGL diet could be appropriate with subjects diagnosed with MS.
Esposito et al.61 commented that nutritional habits similar to Mediterranean diet characterized by high fruit and vegetables intake and high monounsaturated fats are inversely associated to MS. They also indicated that drugs treatment presented slightly lower weight loss that lifestyle intervention based of nutritional changes. Another study29 suggested that beneficial effects for MS could be obtained from diets rich in fruits, vegetables, legumes, whole grains, fish and nuts. The authors considered that simple carbohydrates like sugar are directly involved in MS progress and highlighted that polyunsaturated and monounsaturated fats could prevent components of MS. More interestingly is that authors reported that society needs to create a consciousness of the importance of life style components, particularly dietary and physical activity patterns in the prevention of MS.
CONCLUSIONS
On balance, the present study shows MS is a widespread condition in almost all areas. It seems that a cluster of factors are involucrate in MS development such as dietary habits, physical activity levels, genetic heritage, social economic grade, age, sex, educational level or gut microbiota, it would necessary to focus on each one of these elements to determine MS cause. Obviously, MS status has consequences on health such as cardiovascular diseases, increased risk of some kind of cancers, DM, sleep abnormalities. However, an important effect of MS is physical incapacity because it could probably affect to quality of life of the patient. In MS management there several treatments involved such as exercise programs, drugs therapies or surgical procedures. However, it has been reviewed that nutritional treatment has a notable importance in MS prevention and recovery, particularly dietary patterns with high intakes of fruits, vegetables, fish, nuts, legumes and whole grain cereals intakes are directly connected with MS alleviation. In terms of nutrients, an adequate consumes of monounsaturated fats and proteins would be recommended. However, more studies with long term follow-up period should be performed to understand MS multiple causality, clinical consequences associated to MS and nutritional treatments.