| CLINICAL NOTE |
Diffuse cavernous hemangioma of the rectum: an atypical cause of rectal bleeding
D. Hervías, J. P. Turrión, M. Herrera, J. Navajas León, R. Pajares Villarroya, N. Manceñido, P. Castillo and J.M. Segura
Service of Digestive Diseases. Hospital Universitario La Paz. Madrid, Spain
ABSTRACT
Objective: cavernous hemangioma of the rectosigmoid colon is a rare disease, with no more than 200 cases reported in the literature. The rectosigmoid is the most common site of this disease in the gastrointestinal tract.
Case report: we report the case of a 31-year-old male with recurrent episodes of rectal bleeding, who was finally diagnosed of diffuse cavernous hemangioma of the rectum. The tumor, of 12 x 10 x 9 cm in size, occupied the rectum to the margin of the anal sphincter. A surgical procedure was ruled out because of the inability to carry out a safe anastomosis while preserving anal sphincters. ]]>
Discussion: rectal hemangiomas are less frequent vascular malformations. The clinical presentation of a cavernous hemangioma of the rectum is usually acute, recurrent or chronic rectal bleeding. Other symptoms stem from the possible compression or invasion of adjacent structures, such as lumbar or perianal pain, metrorrhage, hematuria, etc. This diagnosis is commonly made in younger patients.
Colonoscopy is without doubt the diagnostic technique of choice, and it allows to establish the localization, morphology, and total extension of the lesion; its characteristic image is a red-purplish nodule with great vascular congestion. According to the opinion of most authors, biopsy is not advisable during colonoscopy, since imaging techniques are sufficient for an accurate diagnosis, and the risk of bleeding while manipulating this lesion is not negligible. Computed tomography and particularly magnetic resonance imaging, given their high precision to delimit the lesion and its relations to adjacent structures, are imaging studies that are mandatory before surgical treatment. Other techniques such as selective angiography, barium enema, gastrointestinal transit, and upper-tract endoscopy may be supplementary and help locate more lesions along the gastrointestinal tract.
Failure to recognize the exact diagnosis and extent of diffuse cavernous hemangioma may lead to failed surgical treatment and severe complications.
Complete surgical excision of the lesion with a sphincter-saving procedure is the primary mode of treatment: conservative proctectomy with coloanal anastomosis.
Key words: Rectum. Cavernous hemangioma. Rectal bleeding. MRI. Colonoscopy.
Hervías D, Turrión JP, Herrera M, Navajas León J, Pajares Villarroya R, Manceñido N, Castillo P, Segura JM. Diffuse cavernous hemangioma of the rectum: an atypical cause of rectal bleeding. Rev Esp Enferm Dig 2004; 96: 346-352.
Recibido: 09-06-03.
Aceptado: 22-07-03.
Correspondencia: Daniel Hervías Cruz. Avda. Monforte de Lemos, 169, 4º-4. 28029 Madrid, Spain. Telfs.: 91 373 48 15 - 699 85 21 74. e-mail: dhervias@jazzfree.com
]]> INTRODUCTION
Diffuse cavernous hemangioma of the rectum is an uncommon disease with less than 200 reported cases that affects mainly young adults. The rectosigmoid is the most common site of location of this disease in the gastrointestinal tract. The clinical presentation is usually acute, recurrent or chronic rectal bleeding. Symptoms usually manifest early in the disease, but the diagnosis of cavernous hemangioma is seldom established until adulthood.
Diagnosis is usually reached by barium enema examination, colonoscopy, findings on selective inferior mesenteric artery angiography, and other imaging studies such as computed tomography (CT) and magnetic resonance imaging (MRI). The latter imaging study is mandatory to confirm the diagnosis and to evaluate the full extent of the disease. CT and MRI provide information about the dimensions of the tumor and the involvement of adjacent structures.
Failure to recognize the exact extent of a diffuse cavernous hemangioma in the rectosigmoid colon may lead to failed surgical treatment and severe complications. Complete surgical excision of the lesion with a sphincter-saving procedure is the primary mode of treatment (conservative proctectomy with coloanal anastomosis). We present the case of a 31-year-old male with a diffuse cavernous hemangioma of the rectum.
CASE REPORT
A 31-year-old man was attended in our center because of recurrent rectal bleeding during the last 4 years.
In his medical history, besides an active smoking habit, a previous vascular hamartoma in the rectum-sigma stands out. This was operated 15 years before by means of sigmoid resection and end-terminal anastomosis.
In successive colonoscopies after each episode of rectal bleeding, the patient was diagnosed of grade III/IV internal hemorrhoids and subsequently of ulcerative proctitis, without any histological confirmation or improvement following treatment with 5-aminosalicylic acid. No other hemorrhage-associated symptoms, such as abdominal pain, fever, consumptive syndrome, or anemia developed.
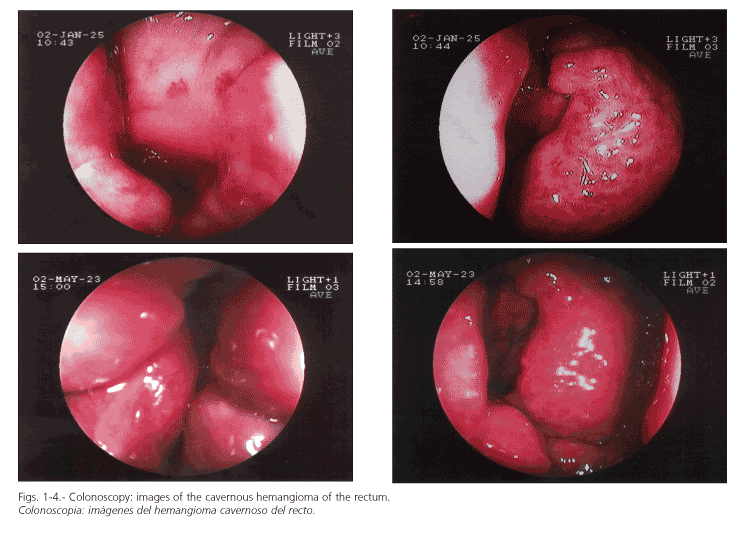
Following another episode of open rectal bleeding, a colonoscopy was carried out. Endoscopy displayed a pseudotumoral, smooth, embossed, vessel-like mass, which occupied the rectum and extended to the margin of the anal sphincter (Figs. 1-4). No biopsy samples were taken because a high risk of hemorrhage has been described during manipulation of these vascular lesions.
]]>An oral endoscopy was carried out to exclude the presence of vascular lesions at this level. A bowel follow-through suggested the presence of nodular lesions compatible with angiomas in the jejunum (Figs. 5 y 6). Selective arteriography did not describe any alterations at the level of the inferior mesenteric artery, and an embolization of the lesion was not possible during this test.
Given the recurrence of bleeding, the possibility of more severe hemorrhage (even occult) and the size of the lesion, a surgical procedure was suggested, but was then ruled out since a safe anastomosis with sphincter preservation was deemed impossible.
DISCUSSION
Rectal hemangiomas are uncommon vascular malformations generally associated with self-limited rectal bleed-ing as their primary symptom (1-3). Other symptoms stem from a possible compression or invasion of adjacent structures, such as lumbar or perianal pain, metrorrhage, hematuria, etc. (4).
]]> Large lesions may be associated with coagulation disturbances as a result of coagulation factor consumption, or as a consequence of platelet destruction secondary to intravascular coagulation within the lesion. As was the case in our patient, a large number of these malformations are near missed or falsely diagnosed, since symptoms are attributed to internal hemorrhoids, polyps, ulcerative colitis, etc. (1-3). Furthermore, many patients show a previous surgical history, especially hemorrhoidectomy, which of course did not prevent further rectal bleeding.Colonoscopy is undoubtedly the diagnostic technique of choice, and it allows to establish the localization, morphology, and total extension of the lesion; its characteristic image is a red-purplish nodule with severe vascular congestion (1-3). Occasionally, ulcerations or an endoscopic image indistinguishable from that of a proctitis may be observed.
It is essential to determine the relation of the lesion with the sphincters, a must in view of a future surgical resection, where sphincter preservation is always pointed out.
According to the opinion of most authors, biopsy collection is not advisable during colonoscopy, as imaging techniques are sufficient for an accurate diagnosis, and the risk of bleeding during manipulation of this lesion is not negligible (1-3).
CT (5) and particularly MRI are highly accurate in delimiting the lesion and its relation to adjacent structures. Therefore, these techniques are of choice for this condition (6,7). In this sense, MRI is, at present, almost a mandatory option before surgical procedures are taken (8).
Other radiologic techniques such as barium enema and gastrointestinal follow-through may be supplementary, but do not generally provide more information, except for the diagnosis of "diffuse intestinal hemangiomatosis". This condition consists of numerous cavernous hemangiomas in the stomach, small intestine and colon (frequently associated with the same lesions in the skin and the soft tissues of the head and neck) (9).
Selective arteriography may detect these lesions, but it is of little importance for the diagnosis. In addition, it shows normal results in most patients, because of the presence of thrombosis in dilated vascular spaces within the hemangioma.
It has been recently suggested that radionuclide studies, particularly Tc-99 scans, may play a role in the assessment of the extension of these lesions.
Once a diagnosis has been established, eradication of the lesion should be recommended.
Although alternative therapies such as sclerotherapy, criotherapy or argon fulguration have been used, these procedures are only of limited value in the case of well-defined, small lesions; because of this, most authors have been abandoned these treatment nowadays.
]]> Commonly used surgical techniques include abdominal-perineal amputation and "sleeve" coloanal anastomosis (14,15).The former has the disadvantage of leaving the patient with a permanent stoma, and it may also cause sexual and/or urinary dysfunction.
Coloanal anastomosis requires a wide mucosectomy of the rectum, keeping a muscular "sleeve" of rectal wall (12).
Although total eradication of the hemangioma is not possible with this technique, there seems to be no risk for new hemorrhage.
The main disadvantage of this anastomosis lies in the difficulty implied by such wide mucosectomy, and severe hemorrhage may develop from vascular dilations at a submucosal level.
REFERENCES
1. Lyon DT, Mantia AG. Large bowel hemangiomas. Dis Colon Rectum 1984; 27: 404-14. [ Links ]
2. Terence CF, Tan MD, Wang JY. Diffuse cavernous hemangioma of the rectum complicated by invasion of pelvic structures: report of two cases. Dis Colon Rectum 1998; 41: 1062-6. [ Links ]
3. Tanaka N, Onda M, Furukawa K, Kumazaki T. Diffuse Cavernous Haemangioma of the Rectum. Eur J Surgery 1999; 165: 280-3. [ Links ]
4. Dachman AH, Ros PR, Shekitka KM, Buck JL, Olmsted WW, Hinton CB. Colorrectal hemangioma: radiologic findings. Radiology 1988; 167: 31-4. [ Links ]
5. Poggioli G, Marchetti F, Selleri S, Fortunato C, Laureti S, Gozzetti. Coloanal anastomosis with colonic reservoir for cavernous hemangioma of the rectum. Hepato-Gastroenterol 1993; 40: 279-81. [ Links ]
6. Bell GA, McKenzie AD, Emmons H. Diffuse cavernous hemangioma of the rectum: report of a case and review of the literature. Dis Colon Rectum 1972; 15: 377-82. [ Links ]
7. Londono-Schimmer EE, Ritchie JK, Hawley PR. Coloanal sleeve anastomosis in the treatment of diffuse cavernous haemangioma of the rectum: long term results. Br J Surgery 1994; 81: 1235-7. [ Links ]
8. Castellví J, Pares D, Ramos E, Serrano T, Oca J, Martí Ragué J. Opciones en el tratamiento quirúrgico del hemangioma cavernoso difuso del recto. Rev Esp Enferm Dig 1996; 88, 8: 566-8. [ Links ]
9. Chaimoff Ch, Lurie H. Hemangioma of the rectum: clinical appearance and treatment. Dis Colon Rectum 1978; 21: 295-6. [ Links ]
10. Malone PS, Kiely EM, Spitz L. Diffuse cavernous haemangioma of the rectum in childhood. Br J Surgery 1990; 77: 338-9. [ Links ]
11. Amarapurkar D, Jadliwala M, Sandeep Punamiya. Cavernous hemangiomas of the rectum: report of three cases. Am J Gastroenterol 1998; 93: 1357-9. [ Links ]
12. Takamatsu H, Akiyama H, Noguchi H, Tahara H, Kahiya H. Endorrectal pull-through operation for diffuse cavernous hemangiomatosis of the sigmoid colon, rectum and anus. Eur J Pediatric Surgery 1992: 245-7. [ Links ]
13. Bortz, JH. Diffuse cavernous hemangioma of the rectum and sigmoid. Abdominal Imaging 1994; 19: 18-20. [ Links ]
14. Lupetin AR. Diffuse cavernous hemangioma of the rectum. Evaluation and MRI. Gastrointestinal Radiology 1990; 15: 343-5. [ Links ] ]]>