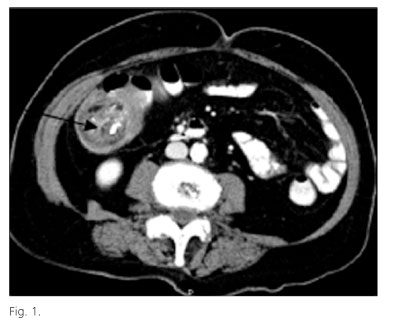
Colocolonic intussusception secondary to high grade colonic leiomysarcoma
Invaginación colocólica secundaria a leiomisarcoma de colon de alto grado
Key words: Intestinal intussusception. Intestinal obstruction. Colonic leiomyosarcoma
Palabras clave: Invaginación intestinal. Obstrucción intestinal. Leiomiosarcoma de colon.
Dear Editor,
Acute bowel obstruction is a common condition for gastroenterologist and surgeons as it accounts for 17.9 to 57.2% of all the causes of acute abdomen. Differential diagnosis of bowel obstruction includes a wide range of etiologies. Through all of them, the intussusception represents an atypical cause of bowel obstruction in adult patients (from 1 to 5% according to most of the series) (1,2).
]]>Case report
We report the case of 69-year old woman, otherwise healthy, who presented at our emergency department with a 5-day history of dull epigastric pain, abdominal distension, rectal bleeding, altered bowel habits, hyporexia and fever. Physical examination revealed a hemodynamically stable status and a palpable painful mass in the upper right quadrant of the abdomen without showing signs of peritonitis. Laboratory test showed the presence of an elevated protein C-reactive, high white blood cell count with neutrophilia and anemia. Plain chest X-rays showed no alterations; plain abdominal X-rays revealed evidence of a dilated bowel loop in the right abdomen with multiple surrounding air-fluid levels. A contrast enhanced computed tomography (CT) found a colocolic intussusception, with no signs of complete obstruction (Fig. 1). In the head of the intussusception a 4 cm tumor-like lesion was found. An urgent laparotomy confirmed the diagnosis of colocolic intussusception and a right ileocolic colectomy was performed. Histological analysis reported an ulcerated atypical mesenchymal neoplasm affecting the whole bowel wall with negative involved lymph nodes (0/12). Immunohistochemistry was positive for vimentin, actin and calponin and negative for C-Kit. The tumor showed also a high mitotic index (42 mitosis per 10 high power fields). The final diagnosis was compatible with a high-grade colonic leiomyosarcoma.
Discussion
Two major points resume the interest in the present clinical case. Firstly, the report of a colocolic intussusception in an adult patient which is uncommon and, secondly, because it was caused by a colonic leimomyosarcoma which is a rare entity. In fact, colon sarcomas represent less than 1% of the malignant tumors of the colon (3).
Ileocolic or colocolic intussusception in adults has a low incidence (0.3/100,000 inhabitants per year) and accounts only for 1 to 5% of all bowel obstructions. The average age of onset varies between 50 and 65 years (1). While the exact mechanism of the instussucecption is unknown, it has been linked to a wide variety of causes such as inflammatory bowel disease, postoperative adhesions, colonic tumors or metastasic implants of some tumors such as melanoma. About 30% of cases of ileocolic intussusception are caused by malignant disease (usually metastatic disease) (1,2). In contrast, a colocolic intussusception is secondary to colon cancer most of the times (> 90%) although there have been reported cases of colocolic intussusception caused by benign disease such as pedunculated lipomas. The classic triad of abdominal pain, palpable mass, and bleeding as showed in the clinical case presented above is rare (2). The CT is considered the best diagnosis tool, with a sensitivity ranging from 58-100% compared to plain abdominal X-rays or an abdominal ecography. Therefore, surgical treatment may be indicated in almost all cases (2).
As mentioned before, colon cancer (usually adenocarcinoma) represents the most common cause of colocolic intussusception while colonic stromal tumors are extremely rare (< 5%). In particular, the incidence of leiomysarcomas is very low 0.45/106 inhabitants per year. Leimyosarcomas are most frequently found in the upper gastrointestinal tract (stomach or small bowel) and colonic locations are considered to be exceptional. They usually affect patients in their 40-60's decades and gender (more frequently seen in males compared to females (1.8:1) as well as racial (higher incidence among Afro-Americans) disparities have been described (4,5). The definitive diagnosis of these group tumors is based on histological features. Some factors such as tumor size (> 5 cm), a high mitotic index or negative immunoreactivity for C-Kit are considered poor prognostic factors (4,5). To date, the only consensus on the treatment of colonic leimyosarcoma includes a complete oncological resection when its possible. It is still controversial whether chemotherapy or radiotherapy may add any benefit in the treatment of this type of tumors (6).
]]> Manuel Bellver1, Iago Rodríguez Lago2, Francisco Queipo3, Carlos Pastor1,
References
1. Azar T, Berger DL. Adult intussusception. Ann Surg 1997;226 (2):134-8. [ Links ]
2. Gustafsson BI, Siddique L, Chan A, Dong M, Drozdov I, Kidd M, et al. Uncommon cancers of the small intestine, appendix and colon: an analysis of SEER 1973-2004, and current diagnosis and therapy. Int J Oncol 2008;33(6):1121-31. [ Links ]
3. Marinis A, Yiallourou A, Samanides L, Dafnios N, Anastasopoulos G, Vassiliou I, et al. Intussusception of the bowel in adults: a review. World J Gastroenterol 2009;15(4):407-11. [ Links ]
4. Tran T, Davila JA, El-Serag HB. The epidemiology of malignant gastrointestinal stromal tumors: an analysis of 1,458 cases from 1992 to 2000. Am J Gastroenterol 2005;100(1):162-8. [ Links ]
5. Miettinen M, Sarlomo-Rikala M, Sobin LH, Lasota J. Gastrointestinal stromal tumors and leiomyosarcomas in the colon: a clinicopathologic, immunohistochemical, and molecular genetic study of 44 cases. Am J Surg Pathol 2000;24(10):1339-52. [ Links ]
6. Cuffy M, Abir F, Longo WE. Management of less common tumors of the colon, rectum, and anus. Clin Colorectal Cancer 2006;5(5):327-37. [ Links ]
]]>