Profilaxis antibiótica en Cirugía Oral y Maxilofacial
Antibiotic prophylaxis in Oral and Maxillofacial Surgery
Jose Ignacio Salmerón Escobar1, Alvaro del Amo Fernández de Velasco2
(1) Médico Adjunto
(2) Médico Residente. H.G.U. Gregorio Marañón de Madrid
Dirección para correspondencia
]]>
RESUMEN
La profilaxis antibiótica en cirugía oral y maxilofacial tiene como fin la prevención de la infección en la herida quirúrgica, ya sea por las características de la cirugía o por el estado general del paciente. Este riesgo se incrementa cuanto más se contamine el campo quirúrgico, siendo necesario realizar tratamiento profiláctico de la infección en cirugías limpias-contaminadas y contaminadas y tratamiento de la infección en cirugías sucias. Además, una adecuada técnica quirúrgica colabora con la reducción de la aparición de infección postquirúrgica. La antibioterapia de elección varía entre derivados de la penicilina con inhibidores de las betalactamasas (amoxicilina-clavulánico, ampicilina-sulbactam), cefalosporinas de segunda o tercera generación, quinolonas o clindamicina. La indicación de su uso variará en función del tipo de cirugía en cada ámbito de la cirugía oral y maxilofacial, según el grado de contaminación de la misma. De este modo en cirugía oral y en patología de glándulas salivares la literatura parece demostrar que no hay mejor pronóstico en cuanto al uso de antibioterapia profiláctica respecto a no usarla en pacientes sanos. En traumatología se justifica en fracturas compuestas o con comunicación con senos paranasales. En cirugía ortognática hay discrepancia en cuanto al criterio de empleo de profilaxis antibiótica, si bien se prefieren ciclos cortos de tratamiento. En cuanto a la cirugía oncológica, se ha demostrado la reducción de la incidencia de infección postquirúrgica con el uso de antibioterapia profiláctica peroperatoria, fundamentalmente en los casos en que se pone en contacto la mucosa oral con la región cervical.
Palabras clave: Infección, cavidad oral, Antibioticos, cirugía oral, cirugía maxilofacial, profilaxis.
ABSTRACT
Antibiotic prophylaxis in oral and maxillofacial surgery aims the prevention of the infection of the surgical wound, either due to the characteristics of the surgery or the general state of the patient. This risk increases with the contamination of the surgical operation area, making it necessary to imply a prophylactic treatment of the infection in clean-contaminated and contaminated surgeries and treatment of the infection in dirty surgeries. Moreover, a proper surgical technique helps to reduce the development of the postsurgical infection. The elective antibiotic chemotherapy ranges from penicillin-derivates with betalactamase inhibitors (amoxycillin-clavulanate, ampicilin-sulbactam) to second or third generation cephalosporins, quinolones or clindamycin. The indication for the use of these antibiotics depends on the type of surgery in oral and maxillofacial surgery, according to the degree of contamination. Thus in oral surgery and surgery of the salivary glands the literature demonstrates that there is not a better prognosis when using prophylactic antibiotherapy instead of not using it in healthy patients. In traumatology this prophylaxis is justified in compound fractures and those communicating with paranasal sinuses. In orthognatic surgery there is disagreement according to the criteria of using antibiotic prophylaxis, but short term treatment is preferred in case of using it. In oncological surgery it has been demonstrated the reduce in incidence of postsurgical infection using prophylactic peroperative antibiotherapy, mostly in those cases in which oral mucosa and cervical area contact.
Key words: Infection, oral cavity, antibiotic, maxillofacial surgery, prophylaxis.
]]> Introducción
La finalidad de la profilaxis antibiótica en cirugía es prevenir la posible aparición de infección a nivel de la herida quirúrgica, creando un estado de resistencia a los microorganismos mediante concentraciones antibióticas en sangre que eviten la proliferación y diseminación bacteriana a partir de la puerta de entrada que representa la herida quirúrgica.
La profilaxis está indicada siempre que exista un riesgo importante de infección, ya sea por las características mismas de la operación o por las condiciones locales o generales del paciente. Entre los factores que van a determinar la posibilidad de aparición de la misma destacan el tipo y tiempo de cirugía y el riesgo quirúrgico del paciente por su comorbilidad (riesgo ASA): diabetes, nefropatías, hepatopatías (cirrosis), cardiopatías, terapéuticas inmunosupresoras (corticoides, radioterapia, quimioterapia, infecciones previas con antibioticoterapia no bien conocida o racionalizada). Intervenciones menores en pacientes sanos no requieren profilaxis.
Al producirse el trauma quirúrgico con la aparición de una solución de continuidad en la piel, se produce la ruptura de la principal barrera que frena la entrada de microorganismos en el interior del cuerpo (1). De esta manera los gérmenes entran y pueden colonizar e infectar tejidos profundos (2). Esto hace que dependiendo del inóculo bacteriano aumente la posibilidad de infección, según sea una cirugía limpia, limpia-contaminada, contaminada o sucia. Cuanta mayor es la contaminación, mayor es el riesgo de infección postquirúrgica.
El riesgo de contaminación del campo quirúrgico se minimiza con una adecuada técnica quirúrgica, con el buen estado nutricional del paciente, etc (3,4), pero el que se ha demostrado como el factor más importante es la profilaxis antibiótica. El uso de antibióticos en cirugía debe realizarse únicamente en aquellos casos en los que esté indicado, el fármaco tiene que tener de vida media larga, poco tóxico y activo frente a los principales microorganismos que se pueden esperar de la contaminación del campo quirúrgico.
Medidas de control en la técnica quirúrgica para minimizar el riesgo de infección son: incisiones limpias; levantamiento mucoperióstico libre de desgarros; irrigaciones como método de enfriamiento y arrastre de partículas de los fresados del hueso alveolar; aspiración constante; hemostasia cuidadosa; en caso de utilizar anestesia local, evitar posibles desgarros de tejidos o capilares con la aguja; introducción lenta del anestésico; precaución esmerada en labios, colgajos y tejidos al utilizar los separadores, retractores, depresor lingual, etcétera; colocación de drenajes (si es preciso); apósitos y compresivos bien colocados. Debemos recordar que algunas de las suturas efectuadas son puntos de aproximación, por lo que existe un tránsito tanto del ambiente húmedo propio de la cavidad bucal, como de residuos alimenticios, por lo que se recomienda hacer enjuagues con suero fisiológico a partir de las 24 horas siguientes a la operación.
Para una profilaxis efectiva, se deben de conseguir concentraciones séricas efectivas desde la apertura hasta el cierre de la herida quirúrgica, por lo que es necesario administrar el antibiótico en un máximo de una hora antes de la incisión. El momento más propicio es durante la inducción anestésica y mediante la vía intravenosa. En caso de que se trate de una cirugía prolongada, puede ser necesario repetir la dosis del antibiótico para mantener unos niveles terapéuticos en sangre, dependiendo de la curva de biodisponibilidad y de la vida media de cada uno. No está demostrado que prolongar la antibioterapia más allá de 24 horas tras la cirugía reduzca el riesgo de infección, por lo que se considera mala práctica prolongar más allá de ese tiempo el tratamiento antimicrobiano (5).
Clasificación de las heridas quirúrgicas de acuerdo con el riesgo de contaminación-infección (6-10)
• Tipo I. Heridas limpias (no apertura de mucosas como la cavidad oral): tasa de infección de 1 a 4 %, no profilaxis antibiótica o profilaxis durante no más de 24 horas con amoxicilina-clavulánico puesto que se ha demostrado la ausencia de beneficio por el uso de antibioterapia postoperatoria.
]]> • Tipo II. Heridas limpias-contaminadas (apertura de mucosas como la cavidad oral o intervención de patología inflamatoria): tasa de infección de 5 a 15 %, profilaxis antibiótica con fármacos que cubran microorganimos gram + y anaerobios(11) (amoxicilina-clavulánico, cefazolina + anaerobicida (clindamicina o metronidazol) (12)).o Amoxicilina-clavulánico 2 g, repetir dosis 1 g/4h si se prolonga la cirugía (13).
o Alérgicos a betalactámicos: clindamicina 600 mg + gentamicina 120 mg, repetir dosis cada 4 horas si se prolonga la cirugía
• Tipo III. Heridas contaminadas (patología oncológica en la que se actúa sobre la cavidad oral y el cuello): tasa de infección de 16 a 25 %, debe efectuarse profilaxis antibiótica cubriendo gram – cuya cobertura es controvertida en cirugías limpias y limpias contaminadas, mediante el uso de fármacos como ampicilina-sulbactam o piperacilina-tazobactam.
o Amoxicilina-clavulánico 2 g, repetir dosis 1 g/4h si se prolonga la cirugía.
o Clindamicina 600 mg + cefazolina 2 g, repetir dosis cada 6 horas de clindamicina y 1 g de cefazolina cada 8 horas si se prolonga la cirugía
• Tipo IV. Heridas sucias e infectadas (tasa de infección de 25 %): tratamiento antibiótico siempre.
El uso de antisépticos tópicos en la cavidad oral reduce el inóculo bacteriano, pero no ha demostrado ser eficaz en la profilaxis de la colonización bacteriana.
]]>Clasificación de las intervenciones quirúrgicas
Se clasifican en 2 grupos, atendiendo a la presencia de gérmenes o no en la zona de la intervención; enumeramos una serie de operaciones tipo de la especialidad:
1. Intervenciones quirúrgicas sin presencia de gérmenes: Dientes retenidos; exostosis, torus; tumores odontogénicos, quistes (no infectados); épulis, cirugía preprotésica y preortodóntica; fracturas maxilares (cerradas); afección glandular; osteotomías; injertos, colgajos y otros.
2. Intervenciones quirúrgicas con presencia de gérmenes: Pericoronaritis del tercer molar, quistes inflamatorios, restos radiculares, granulomas, etcétera; sialolitiasis, fracturas abiertas, traumatismos, heridas contusas; sobreinfección añadida a la lesión tumoral, radionecrosis y otros.
Profilaxis antibiótica en distintas intervenciones quirúrgicas en cirugía oral y maxilofacial
Los datos de la literatura son contradictorios, si bien las series parecen indicar que la reducción de las complicaciones postoperatorias en cirugía oral y maxilofacial se debe fundamentalmente a la mejoría en la técnica quirúrgica y no a la profilaxis antibiótica. Se recomienda la antibioterapia per y postoperatoria en aquellos casos en que haya alto riesgo de infección o signos clínicos evidentes de infección.
Los antimicrobianos a elegir deben ser sensibles a la flora oral y cutánea cervicofacial, fundamentalmente Staphylococcus, Streptococcus, enterobacterias y anaerobios. Por ello es suficiente el uso de derivados de la penicilina combinados con inhibidores de las betalactamasas (amoxicilina-clavulánico, ampicilina-sulbactam), si bien se pueden usar otras pautas con cefalosporinas de segunda o tercera generación (cefazolina, cefoxitin, ceftriaxona) (14), quinolonas o clindamicina.
El uso de antisépticos preoperatorios en la cavidad oral (clorhexidina, povidona yodada) puede reducir las complicaciones derivadas del trauma en la mucosa, especialmente en pacientes con valvulopatías, implantes de material aloplástico, injertos óseos, inmunodeprimidos, ancianos y en pacientes con mala higiene oral (15).
]]> 1.- Cirugía oralLa tasa de infección es baja, por lo que en pacientes sanos la mayoría de procedimientos en cirugía oral no requieren antibioterapia. Se empleará tratamiento antibiótico profiláctico en casos de infección activa, pacientes con comorbilidad o inmunocomprometidos (16).
- Exodoncia de cordales: las distintas series parecen demostrar que el uso de antibioterapia postoperatoria no mejora el pronóstico frente a la posibilidad de infección postoperatoria. Sin embargo algunos estudios parecen indicar que en los procedimientos de extracción del tercer molar en los que se realiza osteotomía puede reducirse el índice de infecciones postoperatorias con el empleo de profilaxis con amoxicilina/clavulánico (17).
- Implantología: no hay mejoría demostrada por uso de antibioterapia postoperatoria prolongada frente a dosis única intraoperatoria, si bien en pacientes con radioterapia previa se emplean regímenes prolongados de antibioterapia para evitar la presencia de osteomielitis o pérdida de los dispositivos de implantes osteointegrados.
2.- Traumatología
Está aceptado ampliamente el uso de antibioterapia profiláctica en fracturas compuestas(18).
- Fracturas de mandíbula y dentoalveolares: los esquemas de tratamiento antibiótico son los clásicos del resto de la patología cervicofacial (penicilina y derivados, cefalosporinas de tercera generación). El tratamiento de fracturas no complicadas no parece aportar beneficios si bien muchos profesionales tratan estas fracturas para cubrir las posibles infecciones para reducir su incidencia (19-22). El tratamiento antibiótico en las primeras 72 horas no resulta necesario. El tratamiento antibiótico de las complicaciones infecciosas (abscesos, pseudoartrosis, osteomielitis...) es donde mayor consenso, si bien en este caso ya deja de ser antibioterapia profiláctica para convertirse en terapéutica (23-4).
- Fracturas orbitarias: no hay consenso en la literatura (algunos autores abogan por el tratamiento mientras que otros no) (26).
- Fracturas de tercio medio y superior: se emplean cefalosporinas de tercera, tratamiento en aquellos casos en que se presente licuorrea (26), si bien la gran mayoría de fracturas de esta región se consideran complejas de entrada y con comunicación de la mucosa oral con otras regiones como los senos paranasales por lo que, en nuestra experiencia, preferimos la cobertura antibiótica profiláctica de entrada en estas lesiones.
3.- Cirugía ortognática y cirugía preprotésica
]]> Se consideran cirugías limpias-contaminadas en las cuales algunas series han demostrado la efectividad de la profilaxis antibiótica postoperatoria (penicilina, cefalosporinas que no mejoran el pronóstico y suponen un mayor coste) (28-9), si bien otros autores parecen demostrar que no hay evidencias de mejor pronóstico frente a infección por el uso de antibioterapia postoperatoria, especialmente si se administra vía oral (30).Hay una mayor incidencia de infecciones en cirugía bimaxilar sin tratamiento antibiótico (31).
Algunos estudios han utilizado levofloxacino oral o cefazolina iv en osteotomías mandibulares, pero en el caso de éste último, es mejor utilizar amoxicilina-clavulánico por cepas resistentes a cefazolina (32).
El tiempo de tratamiento se había establecido en publicaciones previas en 5 días para cobertura antibiótica profiláctica, pero la incidencia de infección postoperatoria es igual en regímenes de 1 ó 5 días, si bien hay cierta mejoría en la morbilidad postoperatoria prolongando el tratamiento durante 5 días (33).
4.- Glándulas salivares
En cirugías como parotidectomía o submaxilectomía se ha demostrado la ausencia de efectividad del uso de profilaxis antibiótica (34).
5.- Cirugía oncológica, reconstructiva y cervical
Se ha demostrado que el uso de antibióticos perioperatorios reduce significativamente la incidencia de infecciones postoperatorias. Como en los casos anteriores, en patología cervical y, fundamentalmente, en cirugía oncológica, se pueden utilizar regímenes de antibioterapia profiláctica combinando clindamicina y cefazolina, cefalosporinas, aminoglucósidos, quinolonas o derivados de la penicilina con inhibidores de betalactamasas.
El riesgo de infección surge ante la posibilidad de poner en contacto áreas limpias con la mucosa oral, puesto que la principal fuente de contaminación en estos pacientes es la saliva que transporta un cantidad importante de bacterias. Otros factores contribuyentes son el mal estado general, los estados de inmunosupresión, radioterapia o quimioterapia preoperatoria, colgajos de reconstrucción o aquellos procedimientos que expongan a los tejidos a isquemia o necrosis tisular. Las fuentes de microorganismos en estas patologías son la saliva, la piel, las piezas dentarias y el propio tumor, por lo que el antibiótico a elegir debe cubrir no solamente a los gérmenes comunes de la saliva, como cocos gram + y anaerobios, sino también a gram – que se aíslan comúnmente en los tumores (35). Gran parte de las referencias en la literatura no consideran que haya que cubrir a los microorganismos gram – en cirugía oncológica de cabeza y cuello pero recientes publicaciones si parecen asociar un mejor pronóstico con cobertura de gram –.
Una pauta de antibioterapia puede ser gentamicina + clindamicina, que cubren bien gram +, gram – y anaerobios (no así la cefazolina que no cubre anaerobios). También amoxicilina-clavulánico y ampicilina-sulbactam tienen el mismo espectro, frente a clindamicina que no cubre suficientemente a los anaerobios.
]]> La duración del tratamiento no está estandarizada quedando en muchos casos a criterio del cirujano. La antibioterapia postoperatoria suele mantenerse hasta la retirada de los drenajes, si bien se prolonga en casos de infección de herida quirúrgica, dehiscencia o fístula.
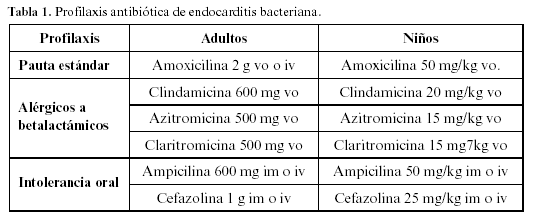
Profilaxis de endocarditis bacteriana
Se hará en todo paciente con cardiopatía predisponente que vaya a ser sometido a un procedimiento con riesgo de bacteriemia en cirugía oral y maxilofacial.
El antibiótico de elección es la amoxicilina-ácido clavulánico. En alérgicos, la alternativa es la clindamicina, claritromicina o azitromicina (tabla 1).
Pacientes con cardiopatías predisponentes:
1. De alto riesgo: prótesis endovascular, endocarditis previa, cardiopatía congénita cianógena compleja o fístulas sistémico-pulmonares realizadas quirúrgicamente
2. De riesgo moderado: otras cardiopatías congénitas, valvulopatías adquiridas, prolapso mitral con insuficiencia, miocardiopatía hipertrófica.
]]> 3. De bajo riesgo: CIA ostium secundum, CIA o CIV intervenidos, by-pass previo, prolapso mitral sin regurgitación, marcapasos.
Requieren profilaxis antibiótica los pacientes de alto riesgo y riesgo moderado que vayan a ser intervenidos en el ámbito maxilofacial usando como pautas antibióticas 1 hora antes vía oral o 30 minutos antes vía intravenosa.
Bibliografía
1. Schuit KE, Johnson JT. Infections of the head and neck. Pediatr Clin North Am 1981;28:965-71. [ Links ]
2. Takai S, Kuriyama T, Yanagisawa M, Nakagawa K, Karasawa T. Incidence and bacteriology of bacteremia associated with various oral and maxillofacial surgical procedures. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005;99:292-8. [ Links ]
3. Coskun H, Erisen L, Basut O. factors affecting wound infection rates in head and neck surgery., Otolaryngol Head Neck Surg 2000;123:328-33. [ Links ]
4. Girod DA, McCulloch TM, Tsue TT, Weymuller EA, Jr. Risk factors of complications in clean-contaminated head and neck surgical procedures. Head Neck 1995;17:7-13. [ Links ]
5. Hotz G, Novotny-Lenhard J, Kinzig M, Soergel F. Single-dose antibiotic prophylaxis in maxillofacial surgery. Chemotherapy 1994;40:65-9. [ Links ]
6. Grassi RF, Pappalardo S, De Benedittis M, Petruzzi M, Giannetti L, Cappello V, Baglio OA. Drugs in oral surgery. Brief guidelines for adult patients. Minerva Stomatol 2004;53:337-44. Review. [ Links ]
7. Mueller SC, Henkel KO, Neumann J, Hehl EM, Gundlach KK, Drewelow B. Perioperative antibiotic prophylaxis in maxillofacial surgery: penetration of clindamycin into various tissues. J Craniomaxillofac Surg 1999;27:172-6. [ Links ]
8. Peterson L. Antibiotic prophylaxis against wound infections in oral and maxillofacial surgery. J Oral Maxillofac Surg 1990;48:617-20. [ Links ]
9. Paterson JA, Cardo VA Jr, Stratigos GT. An examination of antibiotic prophylaxis in oral and maxillofacial surgery. J Oral Surg. 1970;28:753-9 [ Links ]
10. Weed HG. Antimicrobial prophylaxis in the surgical patient. Med Clin North Am 2003;87:59-75. [ Links ]
11. Finegold SM, Wexler HM. Present studies of therapy for anaerobic infections. Clin Infect Dis 1996;23:9-14. [ Links ]
12. Lazzarini L, Brunello M, Padula E, de Lalla F. Prophylaxis with cefazolin plus clindamycin in clean-contaminated maxillofacial surgery. J Oral Maxillofac Surg 2004;62:567-70. [ Links ]
13. Ball P, Geddes A, Rolinson G. Amoxycillin clavulanate: an assessment after 15 years of clinical application. J Chemother 1997;9:167-98. [ Links ]
14. Alfter G, Schwenzer N, Friess D, Mohrle E. Perioperative antibiotic prophylaxis with cefuroxime in oral-maxillofacial surgical procedures. J Craniomaxillofac Surg 1995;23:38-41. [ Links ]
15. Summers AN, Larson DL, Edmiston CE, Gosain AK, Denny AD, Radke L. Efficacy of preoperative decontamination of the oral cavity. Plast Reconstr Surg 2000;106:895-900. [ Links ]
16. Rikhotso E, Ferretti C. Prophylactic antibiotic use in oral surgery--a review of current concepts. SADJ 2002;57:408-13. Review. [ Links ]
17. Martínez lacasa J, Jímenez J, Ferràs V, García-Rey C, Bosom M, Solà-Morales Aguilar L, Garau1a J. Double Blind, Placebo-Controlled, Randomised, Comparative Phase III Clinical Trial o fPharmacokinetically Enhanced Amoxicillin/Clavulanate 2000/125, as Prophylaxis or as Treatment vs Placebo for Infectious and Inflammatory Morbidity after Third Mandibular MolarRemoval (TMR). Abstrac. 43rd Annual ICAAC Chicago. September 2003. [ Links ]
18. Maloney PL, Lincoln RE, Coyne CP. A protocol for the management of compound mandibular fractures based on the time from injury to treatment. J Oral Maxillofac Surg 2001;59:879-84. [ Links ]
19. Abubaker AO, Rollert MK. Postoperative antibiotic prophylaxis in mandibular fractures: A preliminary randomized, double-blind, and placebo-controlled clinical study. J Oral Maxillofac Surg 2001;59:1415-9. [ Links ]
20. Andreasen JO, Andreasen FM, Mejare I, Cvek M. Healing of 400 intra-alveolar root fractures. 2. Effect of treatment factors such as treatment delay, repositioning, splinting type and period and antibiotics. Dent Traumatol 2004;20:203-11. [ Links ]
21. Ghazal G, Jaquiery C, Hammer B. Non-surgical treatment of mandibular fractures--survey of 28 patients. Int J Oral Maxillofac Surg. 2004;33:141-5. [ Links ]
22. Heit JM, Stevens MR, Jeffords K. Comparison of ceftriaxone with penicillin for antibiotic prophylaxis for compound mandible fractures. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997;83:423-6. [ Links ]
23. Bruno JR, Kempers KG, Silverstein K. Treatment of traumatic mandibular nonunion. J Craniomaxillofac Trauma 1999;5:27-32. [ Links ]
24. Dhariwal DK, Gibbons AJ, Murphy M, Llewelyn J, Gregory MC. A two year review of the treatment and complications of mandibular angle fractures. J R Army Med Corps. 2002;148:115-7. [ Links ]
25. Teenier TJ, Smith BR. Management of complications associated with mandible fracture treatment. Atlas Oral Maxillofac Surg Clin North Am. 1997;5:181-209. [ Links ]
26. Courtney DJ, Thomas S, Whitfield PH. Isolated orbital blowout fractures: survey and review. Br J Oral Maxillofac Surg 2000;38:496-504. [ Links ]
27. Torrielli F, Camurati R, Cervar MF, Tel A. Fractures with loss of substance of the middle and upper third of the face: nosographic classification, surgical indications and the prevention of meningeal infections with the new antibiotic, cefuroxime. Minerva Stomatol 1980;29:163-82. [ Links ]
28. Baqain ZH, Hyde N, Patrikidou A, Harris M. Antibiotic prophylaxis for orthognathic surgery: a prospective, randomised clinical trial. Br J Oral Maxillofac Surg 2004;42:506-10. [ Links ]
29. Heit JM, Farhood VW, Edwards RC. Survey of antibiotic prophylaxis for intraoral orthognathic surgery. J Oral Maxillofac Surg 1991;49:340-2. [ Links ]
30. Zijderveld SA, Smeele LE, Kostense PJ, Tuinzing DB. Preoperative antibiotic prophylaxis in orthognathic surgery: a randomized, double-blind, and placebo-controlled clinical study. J Oral Maxillofac Surg 1999;57:1403-6 [ Links ]
31. Spaey YJ, Bettens RM, Mommaerts MY, Adriaens J, Van Landuyt HW, Abeloos JV, De Clercq CA, Lamoral PR, Neyt LF. A prospective study on infectious complications in orthognathic surgery. J Craniomaxillofac Surg 2005;33:24-9. [ Links ]
32. Yoda T, Sakai E, Harada K, Mori M, Sakamoto I, Enomoto S. A randomized prospective study of oral versus intravenous antibiotic prophylaxis against postoperative infection after sagittal split ramus osteotomy of the mandible. Chemotherapy 2000;46:438-44. [ Links ]
33. Bentley KC, Head TW, Aiello GA. Antibiotic prophylaxis in orthognathic surgery: a 1-day versus 5-day regimen. J Oral Maxillofac Surg 1999;57:226-30. [ Links ]
34. Johnson JT, Wagner RL. Infection following uncontaminated head and neck surgery. Arch Otolaryngol Head Neck Surg 1987;113:368-9. [ Links ]
35. Callender DL. Antibiotic prophylaxis in head and neck oncologic surgery: the role of gram-negative coverage. Int J Antimicrob Agents 1999;12:21-5;26-7. [ Links ]
]]>
![]() Dirección para correspondencia
Dirección para correspondencia
Dr. Jose Ignacio Salmerón
C/Rodríguez Marín 71
28016 Madrid
E-mail: jisalmeron@telefonica.net
Recibido: 17-12-2005
Aceptado: 5-04-2006