My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Revista Española de Enfermedades Digestivas
Print version ISSN 1130-0108
Rev. esp. enferm. dig. vol.105 n.5 Madrid May./Jun. 2013
https://dx.doi.org/10.4321/S1130-01082013000500007
PICTURES IN DIGESTIVE PATHOLOGY
Retinal thrombosis secondary to the combination therapy of pegylated interferon and ribavirin for chronic hepatitis C virus infection. A rare complication
Trombosis retiniana secundaria a terapia combinada con interferón pegilado y ribavirina por infección crónica por virus de hepatitis C. Una complicación poco frecuente
Felipe Sahidt Ortega-Ibarra1 and José María Remes-Troche1,2
1Faculty of Medicine, Miguel Alemán Valdés, Veracruz, Veracruz, México
2Department of Research. Laboratory of Digestive Physiology and Gastrointestinal Motility. Medical Biological Research Institute. Universidad Veracruzana. Veracruz, México
Introduction
Despite the fact that there are new therapies for treating chronic hepatitis C virus (HCV) infection (boceprevir, telaprevir), the combination of pegylated interferon and ribavirin continues to be the standard therapy. However, this treatment is not exempt from adverse effects (1-4).
Case report
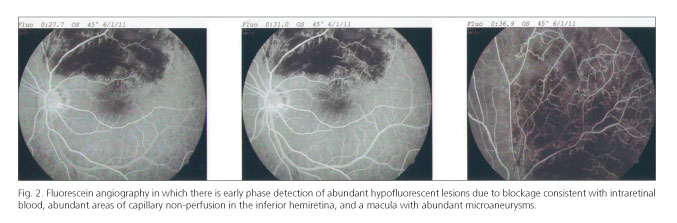
A 52-year-old man with chronic HCV genotype 2b infection was treated with 100 mg of pegylated interferon alpha-2b per week and 800 mg of ribavirin per day. He was asymptomatic before treatment. At 24 weeks, the patient was classified as a responder and 4 weeks after treatment he presented with left hemicranial headache and deteriorating vision on the left side. Fundus examination detected a generalized thinning of the arteriole and flame hemorrhages in the superior hemiretina with macular involvement (Fig. 1). Bilateral fluorescein angiography detected a delay in the inferior venous filling of the left eye. Abundant early phase hypofluorescent lesions due to blockage that were consistent with intraretinal blood, and microaneurysms in the macula were found (Fig. 2). Protein C and protein S levels were normal and the patient did not have Factor V Leiden. Ischemic occlusion of the superior venous branch of the central vein of the retina was diagnosed. Antiangiogenic therapy was prescribed (bevacizumab, a monoclonal antibody directed against vascular endothelial growth factor [VEGF]) every 6 weeks that resulted in a 70 % recovery of visual acuity.
There are fewer than 10 reports in the international literature on retinal thrombosis associated with interferon and ribavirin combination therapy (2-4). Previous studies suggest that interferon may cause immune complex deposition in the retinal vasculature that leads to retinal ischemia, congestion, and hemorrhage (4). The use of an anti-VEGF therapy is based on evidence of a relationship between the ophthalmologic vascular alterations during antiviral treatment and the circulating VEGF levels (5).
References
1. Fried MW. Side effects of therapy of hepatitis C and their management. Hepatology 2002;36:237-44. [ Links ]
2. Fragoso YD, Paggiaro MS, Mastromauro R, Jacondino Gda S, Wilson HM. Literature systematic review on the ophthalmological side effects of interferons. Arq Bras Oftalmol 2011;74:306-10. [ Links ]
3. Nadir A, Amin A, Chalisa N, van Thiel DH. Retinal vein thrombosis associated with chronic hepatitis C: a case series and review of the literature. J Viral Hepat 2000;7:466-70. [ Links ]
4. Guyer DR, Tiedeman J, Yannuzzi LA, Slakter JS, Parke D, Kelley J, et al. Interferon associated retinopathy. Arch Ophthalmol 1993;111:350-6. [ Links ]
5. Andrade RJ, González FJ, Vázquez L, Cilvetti A, Camargo R, García-Cortés M, et al. Vascular ophthalmologic side effects associated with antiviral therapy for chronic hepatitis C are related to circulating vascular endothelial growth factor levels. Antivir Ther 2006;11:491-8. [ Links ]











 text in
text in