My SciELO
Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Cited by Google
Cited by Google -
 Similars in
SciELO
Similars in
SciELO -
 Similars in Google
Similars in Google
Share
Medicina Oral, Patología Oral y Cirugía Bucal (Internet)
On-line version ISSN 1698-6946
Med. oral patol. oral cir.bucal (Internet) vol.12 n.5 Sep. 2007
Lemierre Syndrome associated with dental infections. Report of one case and review of the literature
Inma Juárez Escalona1, Artur Díaz Carandell1, Samir Aboul-Hons Centenero1, Antonio Monner Diéguez3, Antonio Marí Roig2, Carlos Arranz Obispo2, Pedro Piulachs Clapera2, José Mª Lluch Salas2, Silvia Cuscó Albors1, Ramon Sieira Gil1
(1) Fifth year resident
(2) Staff Doctor
(3) Chief of Service. Oral and Maxilofacial Service. Bellvitge University Hospital. (HUB)
ABSTRACT
The first publication on Lemierre Syndrome appears in 1936 by Lemierre. It is defined as an "oropharynx bacterial infection characterized by the thrombophlebitis in the internal jugular vein, derived in a systemic septic embolism". In 81% of the cases, the Fusobacterium necrophorum is the most frequent etiologic agent. Fever is the most common symptom, but it can depending on the primary infection, tonsillitis, mastoiditis or odontogenic infection. According to the literature the mortality is very low, but with a significant morbidity, that is why the diagnosis and early treatment is very important. The diagnosis it´s clinical, even though the CT scan and other diagnosis methods (echography, MRI) help to determine the extent of the infection. Its necessary to administrate the antibiotics endovenous at high dose, (keeping in mind that the most frequent micro organism is anaerobic), and vital support measures if neccessary.
We present a case report of Lemierre Syndrome associated to an odonthogenic infection caused by the 4.8 molar.
Key words: Lemierre syndrome, infection, internal jugular venous thrombosis, septic pulmonary embolism.
RESUMEN
La primera publicación de Síndrome de Lemierre fue en 1936 por Lemierre. Se define como una "infección bacteriana orofaríngea que se caracteriza por la tromboflebitis de la vena yugular interna, complicándose con embolismos sépticos sistémicos". El 81% de los casos, el agente etiológico más frecuente es Fusobacterium necrophorum. La fiebre suele ser el síntoma más frecuente, pero dependiendo de la infección primaria, ya sea amigdalitis, mastoiditis o infección odontógena. La mortalidad es muy baja según la literatura, pero con una morbilidad significativa, por eso es muy importante el diagnóstico y tratamiento precoz. El diagnóstico es clínico, aunque la TC y otros métodos diagnósticos (ecografía, RM) ayudar a determinar la extensión de la infección. Es necesaria la administración de antibióticos por vía endovenosos a dosis máxima, recordando que el microorganismo más frecuente es anaeróbico, y unas medidas de soporte vital. Presentamos un caso clínico de Síndrome de Lemierre asociado a una infección odontógena por causa del molar 4.8.
Palabras clave: Síndrome Lemierre, infección, tromboflebitis vena yugular interna, embolismo pulmonar séptico.
Introduction
The Lemierre syndrome is caused by an oropharynx infection, which causes a septic thrombophlebitis of the internal jugular vein and therefore a metastatic infection. The first to describe it in 1936 was Lemierre with a publication of 20 cases, 18 of them died. It was a very common disease with a high mortality in the preantibiotic era. With the introduction of the antibiotics the incidence and the mortality decreased, that is why it is known as the "forgotten disease".
The most common etiologic agent is Fusobacterium necrophorum (1) (81.7% of the cases), is found in the oral cavity. In the 10,1% of the cases a mixed infection exists ( Fusobaterium necrophorum with Bacteroides fragilis, Staphylococcus epidermidis, Enterococcus sp ). The cultures are negatives in the 12,8% of the cases.
The tonsillitis is the most common primary infection (87, 1%), mastoiditis (2,7%) and the odontogenic infection in 1,8%.
The clinical symptoms depends on the primary infection, but mostly presented by fever in 82%, pain, odynophagia, trismus, vomit, nausea.
The period of time, since the oropharynx infection and invasion of the parapharyngeal space is approximately 7 days.
The second step is the dissemination of the infection through the lateral space of the pharynx, causing the thrombophlebitis of the internal jugular vein. Through hematogenous way septic embolus it gives off and metastasize more commonly in the lungs (79, 8%). The chest x-ray shows a pulmonary infiltrate in lack of cavitations. It is a disease with a high morbidity, and treatment plan should be agressive. The association of penicillin and metronidazol is considered a the first option treatment. When a gramnegative infection exists gentamicin is added (3). The therapy with antibiotics is extended from three to six weeks.
Finally, in the patients where the infection cannot be controlled, the ligation the internal jugular vein considered.
Clinical case
A 36 year old male patient, allergic to penicillin, is admitted to the Maxillofacial and Oral Surgery Service with a right mandibular swealling since five days and fever up to 38ºC.
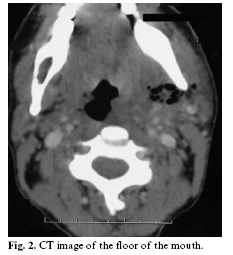
The physical exploration shows a septic mouth with important periodontal disease, great swealling at right submandibular level and edematous floor of the mouth. Blood test was showing 21.990 leukocytes in the blood test, the orthopantography reveal a periapical radiolucent image, important destructive of the 4.8 corone and a big ammount of caries (fig.1) and the cervical CT scan showed images of emphysema of the soft tissues of the neck and floor of the mouth (fig.2). We proceed to its surgical desbridement under general anesthesia and, a treatment was established with 600mg endovenous of clindamicin every 6 hours and 240mg endovenous of gentamicin every 24 hour. In the culture Streptococcus intermedius resistant to clindamicin grew, consequently the treatment was changed for 1gr. Endovenous of vancomicina every 12 hours and 500gr. metronidazol every 24 hours delivered by mouth.
Six days after the patient showed a maximum of fever over 38ºC with left pleuritic, we proced to perform a new chest x-ray that showed: occupation of the left costophrenic angle and nodular image in the left base. The blood cultures gave positive for Streptococcus intermedius (resistant to erythromicin, clindamicin and tetracyclin).
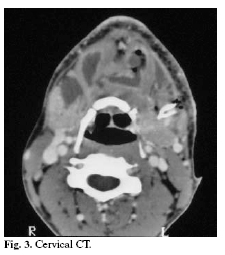
The control cervical CT showed a contra lateral extension of the abscess, localized garland in the rhino and oropharinx adipose tissue that descended to the tonsillar cells with presence of emphysema in contact with interfascial adipose tissue of the pterygoid muscles (fig.3), for this reason a new surgical debridement was performed with the extraction 4.8, with positive culture of Bacteroides fragilis (resistant to clindamicin and penicillin).
On the 11th day the possibility of Lemierre syndrome was considered changing the treatment for 500gr.endovenous of levofloxacin every 12 hours and 1gr. Endovenous of vancomicin every 12 hours during four weeks. A thoracic CT scan was performed where compatible images with septic pulmonary embolus were found, some of them abscessed in both hemithorax (fig.4). The patient presented good signs of evolution with a resolution of the respiratory siymptoms (cough and very purulent expectoration, left pleuritic pain and slight dyspneic feeling) and radiological resolution ( only a minimal occupation persist in the left costophrenic angle). At the moment of release, the blood test showed a normocytic anemia with an hemoglobyn of 10.2, probably related with the septic process, and thrombocytosis of 518.000 platelets. The patient remained without fever, hemodynamics where stable and was released from the hospital.
Discussion
The Lemierre Syndrome is a rare disease. In most of the cases (73%) happens in patients of ages between 16 and 25. In the literature, in an 81%, the etiologic agent is Fusobacterium necrophorum (1), being the blood culture negative in 12,3%. The first phase of the disease, is a pharyngeal infection (2), in 87,1% of cases, and only, in arise form an odontogenic infection. Clinically, it depends on the initial infection, but in most cases the patients complain of odynophagia and evidence of pharyngeal inflammation. The fever happens in an 82,5%, but it is not necessarily the first clinical symptom.
The second phase is the invasion of the pharyngeal lateral wall and the thrombophlebitis of the internal jugular vein. The symptoms are the results of the vital structures being affected. Trismus (9,1%) because of the affection of the pterygoid muscle, paralysis of the trapezius muscle by spinal accessory nerve affectation. Rarely you can touch the thrombosis of the internal jugular vein in the internal jugular vein.
Bacteriemia appears when the infection invades the internal jugular vein. The first sign of complication is fever. In the 78,8% of the cases, the metastatic complication is in the lung (3), 16,5% in the articulations and more rarely in abscesses and brain infarcts (4). The chest x-rays, show pulmonary infiltrates with absence of cavitations associated to pleural effusions (43.1%).
The diagnostic keypoints of Lemierre Syndrome are the symptoms and, secondarily, the image diagnostic methods. The detection of the thrombophlebitis of the internal jugular vein, includes CT, MRI, and ultrasounds (5). Some authors recommend thoracic CT scan as first diagnotic method, to demonstrate the pulmonary abscesses and to facilitate there drainage.
The initial treatment is done with endovenous antimicrobial agents, keeping in mind that the most common microorganism is anaerobic.
As a reminder, in the preantibiotic era the elected treatment was ligation the internal jugular vein. In the present it is the antibiotic treatment extended of 3 to 6 weeks. In the present literature, afortunately, the ligature of the internal jugular vein is not very frequent.
Conclusions
In the review of the literature, the chronic periodontitis (6) is the most common cause of odontogenic infection associated to septic pulmonary embolus.
The nine cases, reviewed in the literature, are young people, with no immunodeficiency but with serious periodontal disease.
In most cases, gingivitis is the initial sign, treated with antimicrobial agents and periodontal surgery.
Finally, the infection of odontogenic origins should be considered as a possible cause of septic embolus and the Lemierre syndrome, and be treated efficiently.
References
1. Ramirez S, Hild TG, Rudolph CN, Sty JR, Kehl SC, Havens P, et al. Increased diagnosis of Lemierre Syndrome and other Fusobacterium necrophorum infections at a children´s Hospital. Pediatrics 2003; 112:380-5. [ Links ]
2. Jiménez Y, Bagán JV, Murillo J, Poveda R. Odontogenic infections. Complications. Systemic manifestations. Med Oral Patol Oral Cir Bucal 2004; 9 Suppl:S139-47. [ Links ]
3. Steiner M, Grau MJ, Wilson DL, Snow Nj. Odontogenic infectation leading to cervical emphysema and fatal mediastinitis. J Oral Maxillofac Surg 1982; 40:600-4. [ Links ]
4. Chirinos J, Lichtstein D, Garcia J, Tamariz L. The evolution of Lemierre Syndrome. Report of 2 cases and review of the literature. Medicine 2002; 81:458-65. [ Links ]
5. Libeer C, Bockaert J, Van den Brande P, Zachee P, Van de Vyvere M, Geyskens W. The Lemierre syndrome: a complicated oropharyngeal infection. Acta Clinica Belgica 2005; 60:173-9. [ Links ]
6. Cook RJ, Ashton RW, Aughenbaugh GL, Ryu JH. Septic pulmonary embolism. Presenting features and clinical course of 14 patients. Chest 2005;128: 162-6 [ Links ]
7. Shibasaki Y, Yoshikawa H, Idezuka J, Yamazaki M, Onishi Y. Cerebral infarctions and brain abscess due to Lemierre Syndrome. Intern Medicine 2005; 44:653-6. [ Links ]
8. Screaton N, Ravenel J, Lehner PJ, Heitzman R, Flower C. Lemierre Syndrome: forgotten but not extinct-report of four cases. Radiology 1999; 213:369-74. [ Links ]
9. Shiota Y, Arikita H, Horita N, Hiyama J, Ono T, Ohkawa S, et al. Septic pulmonary embolism associated with periodontal disease. Report of two cases and rewiew of the literature. Chest 2002; 121:652-4. [ Links ]
![]() Correspondence:
Correspondence:
Dra Inma Juárez Escalona
Servicio cirugía oral y maxilofacial.
Hospital Universitari de Bellvitge.
C/ Feixa llarga s/n 08907
Hospitalet de Llobregat. Barcelona
E-mail: ijescalona@hotmail.com
Received: 17-06-2006
Accepted: 17-12-2006